Infectious diseases specialists diagnose and treat infections from bacteria, viruses, fungi, and parasites, focusing on fevers, antibiotics, and vaccines.
Send us all your questions or requests, and our expert team will assist you.
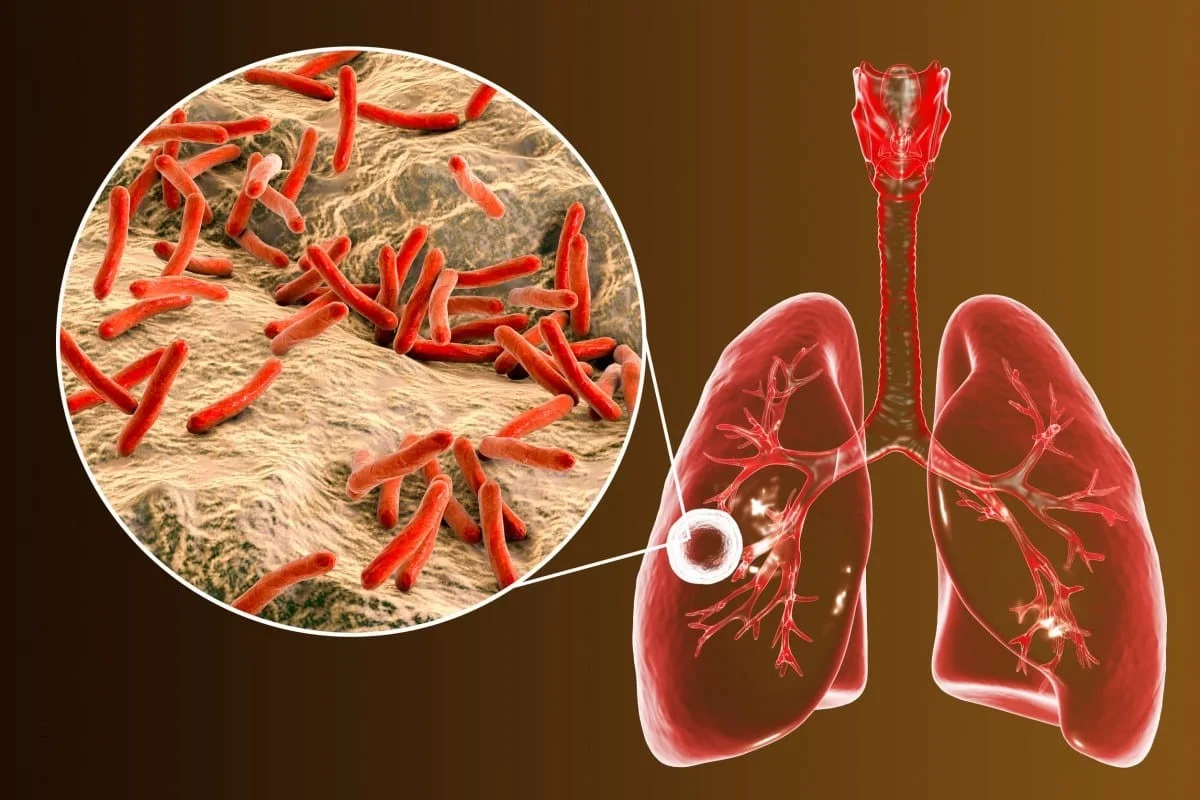
Tuberculosis, or TB, is still one of the most challenging bacterial diseases today. Many people think of it as a disease of the past, but it continues to be a major global health problem. TB is caused by Mycobacterium tuberculosis, a rod-shaped bacterium with a tough, waxy cell wall made of mycolic acids. This special coating protects the bacteria from many antibiotics, helps it survive in harsh environments, and allows it to avoid being destroyed by the immune system.
Tuberculosis is known as a granulomatous disease because of how the body tries to defend itself. When TB bacteria are inhaled and reach the lungs, immune cells called macrophages try to destroy them. Normally, these cells would break down the bacteria, but M. tuberculosis has ways to survive inside them. Since the immune system cannot get rid of the bacteria right away, it brings in more immune cells to surround the infected area, forming a structure called a granuloma.
The granuloma is the main sign of tuberculosis in the body. It shows a standoff between the bacteria and the immune system. Inside the granuloma, TB bacteria can stay inactive for many years, which is called Latent Tuberculosis Infection (LTBI). People with LTBI do not feel sick and cannot spread TB, but the bacteria can become active if the immune system weakens. When this happens, the bacteria break out of the granuloma and can cause active disease. Tuberculosis is more than just an infection; it is an ongoing battle between the body and the bacteria.
To understand tuberculosis in the context of modern medical science, one must appreciate the mechanism of tissue damage. The destruction of lung tissue in active TB is not primarily caused by bacterial toxins, but rather by the host’s own immune response. This phenomenon, known as delayed-type hypersensitivity, involves a robust inflammatory response designed to deprive bacteria of resources. The center of the granuloma undergoes caseous necrosis—a form of cell death that transforms functional lung tissue into a soft, cheese-like substance. This necrotic debris destroys the delicate alveolar architecture required for gas exchange.
The lungs can repair themselves to some extent, but the long-term inflammation from TB often makes this difficult. Instead of growing new healthy lung tissue, the body forms scar tissue (fibrosis) to contain the damage. This scarring reduces lung function. Researchers are now studying how to help the lungs heal better after TB, aiming to control the immune response so that more healthy tissue is preserved and less scarring occurs.
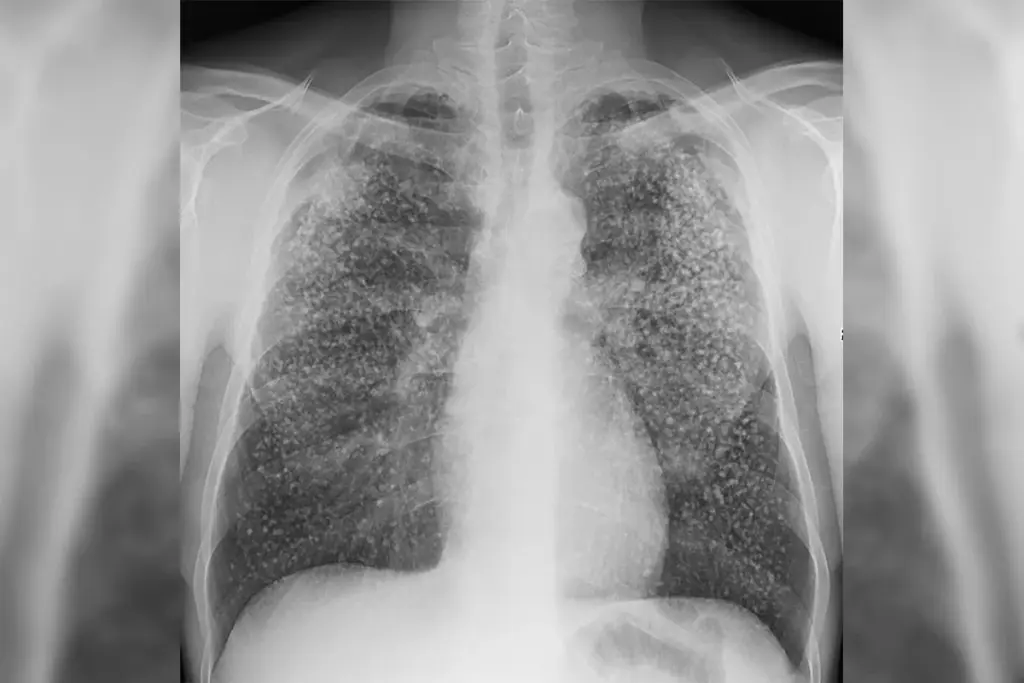
Although TB usually starts in the lungs, it can affect almost any part of the body. Because of this, TB is divided into two types: Pulmonary Tuberculosis (in the lungs) and Extrapulmonary Tuberculosis (outside the lungs).
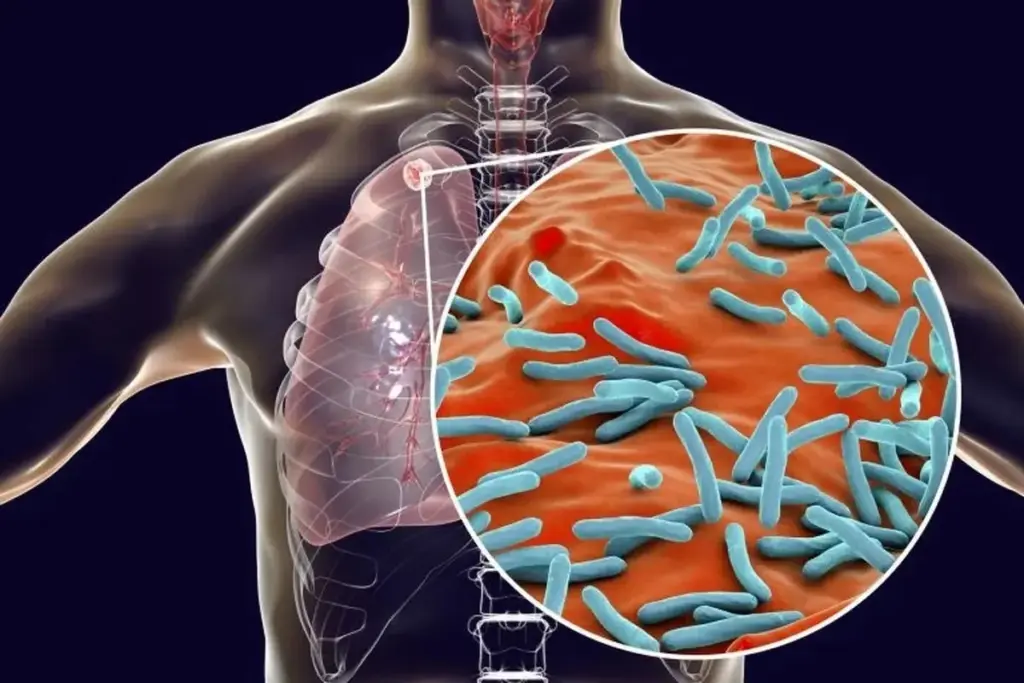
Tuberculosis is a worldwide disease, but it affects some regions more than others. It spreads through the air when someone with active TB coughs, talks, or sneezes, releasing tiny droplets. These droplets can stay in the air for hours, so good ventilation and avoiding crowded spaces are important to prevent its spread.
Today, TB is one of the top causes of death from infection. The problem is worse when someone also has HIV, because HIV weakens the immune system and makes it easier for TB to become active. There are also new strains of TB that do not respond to standard antibiotics, called MDR-TB and XDR-TB. Because of this, doctors are exploring new treatments that help the body’s own defenses fight the disease.
Contemporary medicine views tuberculosis through the lens of cellular biology. Research has moved beyond simple bacteriology to investigating the complex “omics”—genomics, proteomics, and metabolomics—of the interaction between M. tuberculosis and the human host. Scientists are mapping bacterial genetic diversity to understand virulence factors and drug resistance mechanisms. Simultaneously, they are studying the genetic polymorphisms in humans that confer susceptibility or resistance to the disease.
This cellular perspective is crucial for developing new diagnostic tools and vaccines. Current research aims to identify biomarkers—specific proteins or genetic signals in the blood—that can predict which individuals with latent infection are at highest risk of progressing to active disease. This predictive capability would enable targeted preventive therapy, a core concept of precision medicine. Furthermore, understanding the cellular mechanisms of dormancy is vital for eradicating the “persister” bacteria that survive antibiotic treatment and cause relapse. The integration of advanced immunology and cellular research is transforming TB from a disease of simple infection control to a complex challenge of immune engineering and tissue preservation.


Send us all your questions or requests, and our expert team will assist you.
Latent TB Infection (LTBI) occurs when a person has the TB bacteria in their body, but their immune system has successfully contained it within granulomas. These individuals have no symptoms, do not feel sick, cannot spread the bacteria to others, and usually have a normal chest X-ray. Active TB disease occurs when the immune system fails to contain the bacteria, allowing them to multiply, cause symptoms, damage tissues, and become transmissible.
No, while the lungs are the most common site of infection due to airborne transmission, TB can affect almost any part of the body. Common extrapulmonary sites include the lymph nodes, the pleura (lining of the lungs), the kidneys, the bones and joints (primarily the spine), and the brain and spinal cord (meningitis).
The cell wall of Mycobacterium tuberculosis is exceptionally thick and rich in lipids called mycolic acids. This waxy coating acts as a shield, protecting the bacteria from dehydration, chemical disinfectants, and the immune system’s digestive enzymes. It also makes the bacteria naturally resistant to many common antibiotics, requiring specialized drugs for treatment.
A granuloma is a tiny, organized collection of immune cells that forms when the immune system attempts to wall off substances it cannot eliminate, such as TB bacteria. In TB, it serves as a prison for the bacteria, preventing them from spreading. However, the bacteria can survive in a dormant state inside the granuloma for years.
The lungs have some regenerative capacity, but severe TB often causes a type of tissue death called necrosis, which the body heals by forming scar tissue (fibrosis) rather than regenerating functional lung tissue. This scarring is permanent. Modern treatments aim to stop the infection early, minimizing scarring and preserving as much lung function as possible.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)