Infectious diseases specialists diagnose and treat infections from bacteria, viruses, fungi, and parasites, focusing on fevers, antibiotics, and vaccines.
Send us all your questions or requests, and our expert team will assist you.

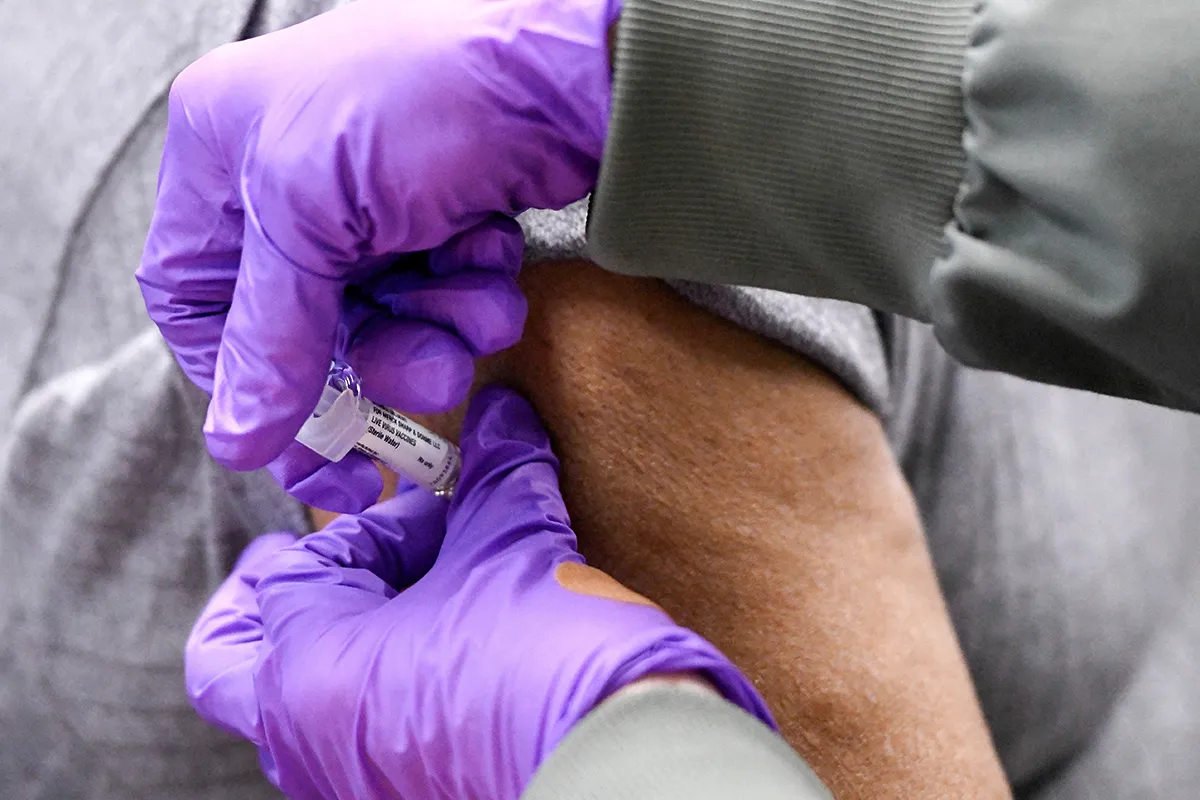
Vaccination is the cornerstone of pertussis prevention. The history of this vaccine involves a significant technological shift from Whole-Cell (wP) to Acellular (aP) formulations.
The standard prevention protocol involves a multi-dose series starting in infancy.
The most vulnerable demographic for pertussis mortality is infants under two months of age—those too young to be vaccinated themselves. To bridge this immunity gap, public health authorities universally recommend Maternal Immunization.
Pregnant women are advised to receive the Tdap vaccine during every pregnancy, ideally between 27 and 36 weeks of gestation. The maternal immune system produces high levels of IgG antibodies in response to the vaccine. These antibodies are actively transported across the placenta to the fetus. When the baby is born, they possess a high concentration of maternal antibodies that provide passive protection against pertussis during the critical first months of life, until the infant’s own vaccination series can begin. This strategy has been proven to be the most effective method for preventing neonatal pertussis deaths.

Before maternal immunization became the standard, the “Cocooning” strategy was the primary way to protect infants. This approach involves vaccinating everyone who will be in close contact with the newborn—parents, siblings, grandparents, and caregivers—at least two weeks before meeting the baby. The theory is to create a protective “cocoon” of immune individuals around the vulnerable infant, preventing the bacteria from entering the household. While still recommended as a supplementary measure, it has proven logistically difficult to implement perfectly, making maternal immunization the priority intervention.
When a case of pertussis is identified, preventing secondary spread is critical. Post-Exposure Prophylaxis (PEP) involves administering a course of antibiotics (usually Azithromycin) to close contacts of the infected person, regardless of their vaccination status.
PEP is recommended for:

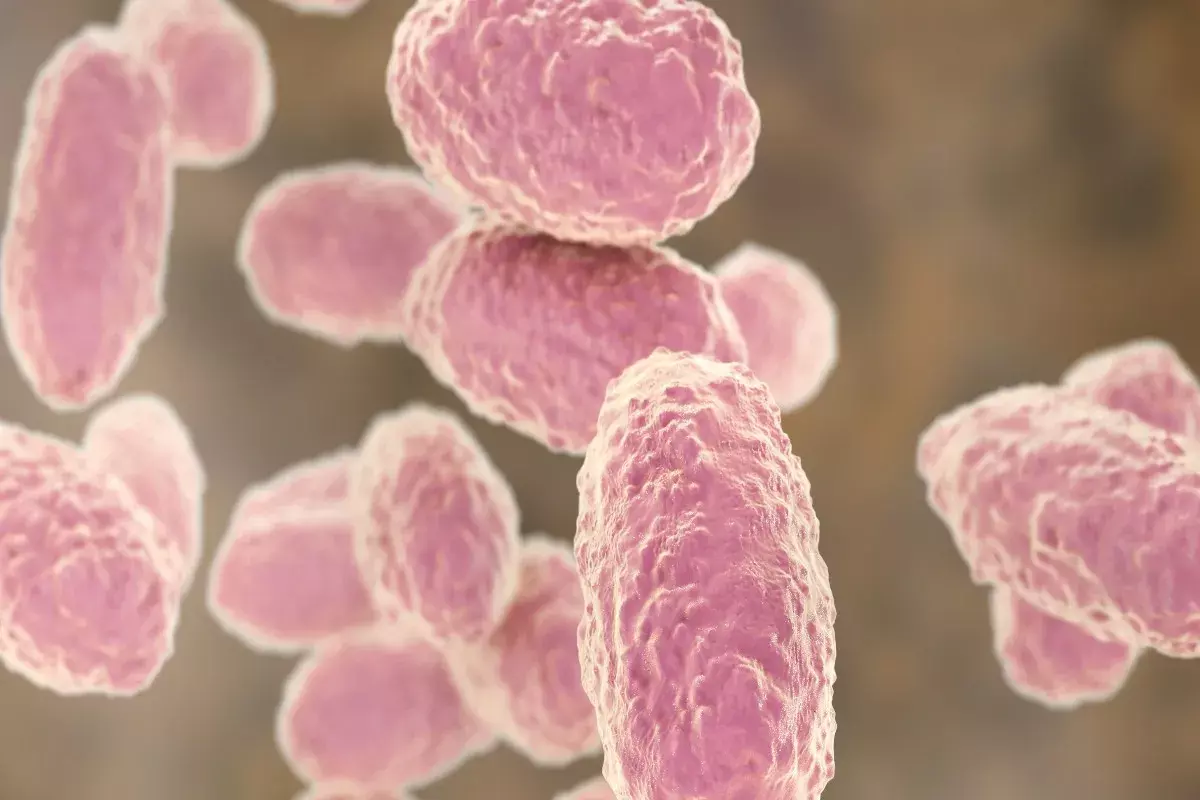
Pertussis is unique because even with high vaccination coverage, “herd immunity” is challenging to sustain. The extremely high transmissibility (R0) of the virus and the waning immunity of acellular vaccines mean that the bacteria continue to circulate in the population, often causing asymptomatic or mild infections in adults. This reality underscores the necessity of targeted protection for the vulnerable (infants) rather than relying solely on the community to stop transmission. Prevention strategies must therefore remain dynamic, focusing on keeping boosters up to date and rigorously protecting the youngest members of society.

Send us all your questions or requests, and our expert team will assist you.
The antibody levels in the mother peak a few weeks after vaccination and then decline. To ensure the baby receives the highest possible amount of antibodies through the placenta, the mother needs a fresh “boost” of antibodies during the third trimester of each pregnancy, even if the pregnancies are close together.
Acellular vaccines are excellent at preventing severe disease (symptoms), but they are less effective at preventing colonization. This means a vaccinated person might still carry the bacteria in their nose and throat for a short time without feeling sick, potentially spreading it. This is why hygiene and avoiding vulnerable infants when you have a cough are still important.
No. DTaP contains higher doses of the antigens and is designed for the developing immune systems of infants and young children (under 7 years). Tdap contains lower doses (indicated by the lower case letters) and is used as a booster for older children, adolescents, and adults whose immune systems need a reminder.
No. The current acellular vaccines (DTaP and Tdap) contain only purified parts of the bacteria (proteins), not the whole bacteria. Because there is no whole, live, or even dead bacterium in the shot, it is biologically impossible for the vaccine to cause the disease.
Consult your doctor immediately. Even if you are vaccinated, you may be prescribed a course of antibiotics (Post-Exposure Prophylaxis) to prevent you from getting sick or spreading the bacteria, especially if you live with infants, pregnant women, or people with weak immune systems.






Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)