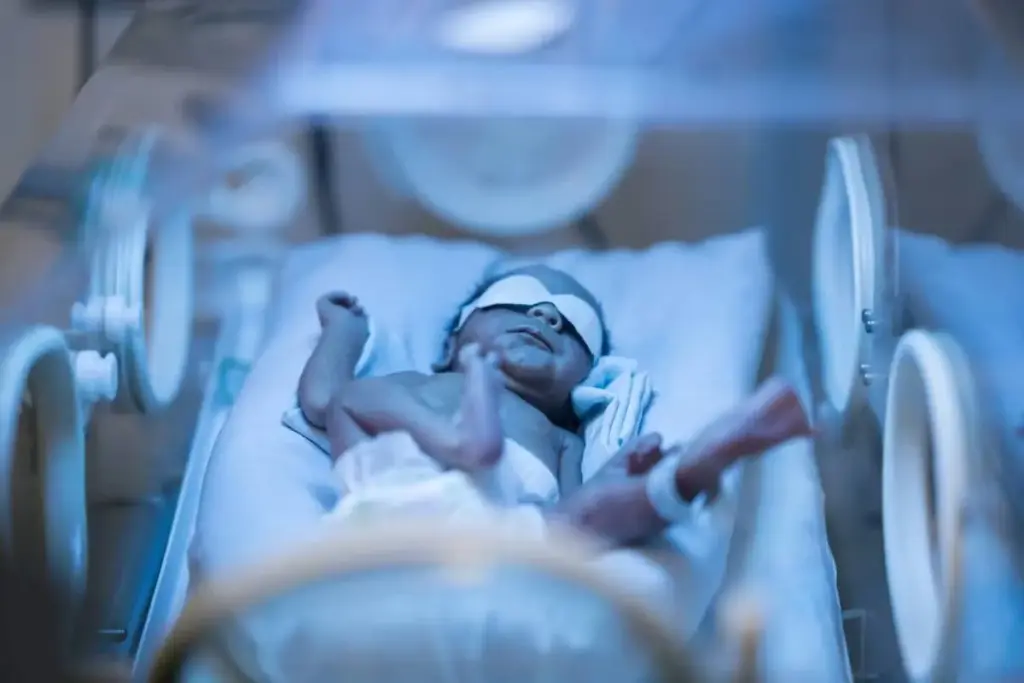
Nearly 60% of newborns get jaundice, a condition with high bilirubin levels. This makes phototherapy a common treatment. Listing the disadvantages and side effects of using a ultraviolet radiation lamp for phototherapy in newborns.
Phototherapy, or light therapy, helps treat neonatal jaundice by lowering bilirubin levels. It’s an effective way to treat neonatal hyperbilirubinemia. But, there are some disadvantages of phototherapy to think about.
As jaundice light treatment for newborns grows, knowing its downsides is key. This is important for healthcare providers and parents.
Key Takeaways
- Phototherapy is a common treatment for neonatal jaundice.
- It reduces bilirubin levels in the blood.
- Despite its effectiveness, phototherapy has several disadvantages.
- Understanding these downsides is key for healthcare providers.
- Parents should know the risks of phototherapy.
The Science Behind Neonatal Jaundice and Phototherapy
It’s important for healthcare providers to understand neonatal jaundice and phototherapy. Jaundice is when newborns have too much bilirubin in their blood. This can make their skin and eyes turn yellow.
If not treated, jaundice can cause serious health problems. So, knowing how to treat it is key.
How Bilirubin Accumulates in Newborns
Bilirubin builds up because of broken-down red blood cells. Newborns break down red blood cells faster. Their livers aren’t ready to handle all the bilirubin.
This leads to jaundice. Premature babies, blood group issues, and infections can make it worse.
The interleukin-1 family cytokines are involved in inflammation and the immune response. They play a role in neonatal jaundice. Knowing this helps in managing the condition better.
Principles of Light Therapy for Hyperbilirubinemia

Phototherapy uses light to change bilirubin into a form that’s easier to get rid of. UV light therapy, or blue light, is often used. It’s absorbed by bilirubin, starting a reaction that makes bilirubin easier to excrete.
The success of phototherapy depends on several things. These include the light’s intensity and wavelength, how much skin is exposed, and how long the treatment lasts. Healthcare providers must adjust these factors to get the best results.
Types of Phototherapy Devices Used in Neonatal Care
Neonatal jaundice treatment uses various phototherapy devices. Each has its own features and uses in caring for newborns.
Conventional Phototherapy Units
Conventional phototherapy units are common in treating jaundice in newborns. They have fluorescent lamps that give off blue light. This light breaks down bilirubin effectively.
Key Features: They can adjust intensity and have timers. Some can also change the light spectrum.
Fiber-Optic Blankets and Pads
Fiber-optic blankets and pads are a newer phototherapy option. They use fiber-optic cables to send light directly to the baby’s skin. This makes treatment more flexible and comfortable.
Advantages: Babies can move more freely. They can be used during feeding or when being held. This might also lower the risk of eye damage from light.
LED-Based Systems
LED-based phototherapy systems are becoming more popular. They use LEDs that emit light at a wavelength best for breaking down bilirubin. They also produce less heat than traditional lamps.
Benefits: They are energy-efficient and last longer. They also give off less heat. This makes babies more comfortable and safe during treatment.
|
Device Type |
Key Characteristics |
Advantages |
|---|---|---|
|
Conventional Phototherapy Units |
Fluorescent lamps, blue spectrum light |
Effective bilirubin breakdown, adjustable intensity |
|
Fiber-Optic Blankets and Pads |
Fiber-optic cables, localized light delivery |
Increased infant mobility, comfort during treatment |
|
LED-Based Systems |
Specific wavelength LEDs, energy-efficient |
Optimal bilirubin breakdown, reduced heat output |
Understanding Ultraviolet Radiation Lamps in Phototherapy
Edit
Full screen
Delete
ultraviolet radiation lamp
It’s key to know about ultraviolet radiation lamps for phototherapy. UV light is vital in treating neonatal jaundice. The type of UV lamp used affects treatment success and safety.
UVA vs. UVB vs. UVC Properties
Ultraviolet radiation is split into three types: UVA, UVB, and UVC. UVA has the longest wavelength (320-400 nm) and is used in phototherapy. It goes deeper into the skin. UVB (290-320 nm) is used too, but it’s absorbed by the skin’s outer layers. UVC, with a wavelength of 100-290 nm, is not used for phototherapy. It can cause skin damage and doesn’t penetrate much.
Safety Concerns with UV Light Sources
The use of UV light sources in phototherapy has safety issues. Skin damage and skin cancer risk are big concerns. UV radiation can also harm the eyes, so eye protection is essential. It’s important to watch how long and how intense the UV exposure is.
Differences Between Medical and Germicidal UV Lamps
It’s important to know the difference between medical UV lamps and germicidal UV lamps. Medical lamps are made for treating neonatal jaundice. Germicidal lamps kill bacteria and viruses with UVC light. Using the wrong lamp can cause ineffective treatment or harm.
In conclusion, ultraviolet radiation lamps are important in phototherapy. But, their use needs careful thought about the UV type, safety, and monitoring. This ensures treatment is both effective and safe.
Short-Term Physical Side Effects of Phototherapy
Phototherapy helps newborns but can cause short-term issues. These problems are important for doctors to watch. They can affect a baby’s comfort and health.
Dehydration and Electrolyte Imbalances
Phototherapy can lead to dehydration and electrolyte imbalances. Newborns might lose more fluids. This is because they have more bowel movements and lose water through their skin.
It’s key to keep an eye on how much fluid and electrolytes they have. This helps avoid serious problems.
Temperature Regulation Problems
Phototherapy can make it hard for newborns to keep their body temperature right. The lights might make them too hot or too cold. It’s important to keep the room at a stable temperature.
Skin Rashes and Bronze Baby Syndrome
Phototherapy can also cause skin problems. Some babies get skin rashes or Bronze Baby Syndrome. This makes their skin look grayish-brown. These issues usually go away but can worry parents.
In summary, phototherapy is a lifesaver for many newborns with jaundice. But, it has short-term side effects. Doctors need to watch closely to help their patients the best they can.
Eye-Related Complications and Risks
Phototherapy is a common treatment for neonatal jaundice. But, it comes with eye-related risks. Newborns are exposed to strong light, which can harm their eyes.
Potential for Retinal Damage
The light used in phototherapy can damage the retina in newborns. The retina is very sensitive to light. Prolonged exposure to certain wavelengths can cause cell damage.
Key factors influencing retinal damage risk include:
- Intensity and duration of phototherapy
- Wavelength of light used (UVA, UVB, or blue light)
- Adequacy of eye protection measures
Challenges with Eye Protection Compliance
It’s vital to protect eyes during phototherapy to avoid damage. But, making sure eye protection is used correctly can be hard.
Common issues include:
- Eye patches or masks may not fit properly, leaving areas exposed
- Frequent removal of eye protection for feeding or care can compromise protection
- Monitoring and maintaining eye protection can be labor-intensive
Long-Term Vision Concerns
Phototherapy is usually safe, but there are worries about long-term vision effects. Scientists are studying these risks.
Some long-term vision concerns include:
- Increased risk of cataracts or other lens opacities
- Potential for retinal abnormalities or scarring
- Impact on visual development in premature infants
Healthcare providers must consider the benefits and risks of phototherapy. They should also use strong eye protection to reduce risks.
Disruption of Parent-Infant Bonding During Treatment
Edit
Full screen
Delete
parent-infant bonding
Phototherapy can disrupt the early bonding between parents and their newborns. This period is key for a lifelong connection.
Limited Physical Contact and Holding
Phototherapy requires newborns to be under special lights. This limits their physical contact with parents. It makes it hard for parents to hold their babies close.
Physical touch is vital for bonding. It releases hormones that foster love and attachment. With less touch, bonding can be delayed or harder.
Impact on Breastfeeding Establishment
Phototherapy can also hurt breastfeeding. Mothers might struggle to get a good latch or keep up milk supply. This is because they can’t feed their baby as often.
Frequent breastfeeding is key for the baby’s nutrition and bonding. Phototherapy’s impact on breastfeeding is a double blow.
Psychological Effects on Parents
Seeing their newborn under phototherapy lights can stress parents. They often feel guilty, worried, and helpless.
Healthcare support is key to easing these feelings. Knowing the challenges of phototherapy helps parents prepare for its emotional toll.
Potential Long-Term Complications of Phototherapy
Phototherapy is used to treat neonatal jaundice but raises concerns about its long-term effects. It uses light to break down bilirubin in the skin. But, we don’t fully understand how it affects a newborn’s body.
DNA Damage and Cellular Changes
UV radiation in phototherapy can damage DNA. This is because UV light can change DNA, leading to mutations. Studies have shown these mutations can cause long-term changes in cells, affecting health later in life.
It’s important to note that not all phototherapy uses UV radiation. Many devices use LED lights that don’t have UV. But, UV light’s risk of DNA damage is a concern.
|
Type of Light Therapy |
Risk of DNA Damage |
Clinical Implications |
|---|---|---|
|
UV Light Therapy |
High |
Potential long-term cellular changes |
|
LED Light Therapy (without UV) |
Low |
Minimal risk of DNA damage |
Research on Cancer Risk
Some studies look at phototherapy’s link to cancer. UV radiation can cause DNA damage and possibly lead to skin cancer. But, it’s essential to note the evidence is not clear, and more research is needed.
A study found no big increase in cancer risk for those who got phototherapy as newborns. Yet, continued monitoring and research are key to ensure its safety.
Neurodevelopmental Concerns
Phototherapy’s impact on brain development is also being studied. Some research suggests a link to neurodevelopmental issues. But, the evidence is not yet solid. Further investigation is needed to fully understand this.
In conclusion, phototherapy is a lifesaving treatment for jaundice in newborns. But, we must keep watching its long-term effects. Research into DNA damage, cancer risk, and brain development will help us understand its complications better.
Special Risks for Premature and Low Birth Weight Infants
Premature babies getting phototherapy face special challenges. Their bodies are not fully developed. This makes them more likely to face both the good and bad sides of light therapy.
Increased Sensitivity to Light Exposure
Premature babies are more sensitive to light. Their eyes are not fully grown. This means they can get hurt by the strong light used in phototherapy.
Eye protection is key to prevent eye damage. Doctors use eye patches or shields. But keeping them on can be hard, like when the baby moves or is handled.
Compromised Skin Barrier Function
Premature babies have thinner, more fragile skin. This makes them more at risk for dehydration, electrolyte imbalances, and skin problems during phototherapy.
It’s important to watch the baby’s skin closely. If there’s any sign of irritation or other problems, tell the doctor right away.
|
Risk Factor |
Description |
Mitigation Strategy |
|---|---|---|
|
Increased Light Sensitivity |
Premature infants are more sensitive to light therapy due to immature retinal development. |
Use appropriate eye protection and adjust light intensity. |
|
Compromised Skin Barrier |
Thinner skin increases the risk of dehydration and skin irritation. |
Monitor skin condition closely and adjust treatment as needed. |
|
Modified Treatment Protocols |
Premature infants may require adjusted treatment schedules and intensities. |
Tailor phototherapy protocols to the individual infant’s needs. |
Modified Treatment Protocols
Because of their special needs, phototherapy plans for premature and low birth weight babies may need to change. This could mean adjusting the light’s strength, how long it’s on, or how often it’s checked.
Doctors have to find the right balance. They need to treat jaundice well but also protect these babies from phototherapy’s risks.
Equipment-Related Hazards and Technical Failures
Phototherapy equipment is key for treating jaundice in newborns. It’s effective, but it comes with risks. These risks can harm newborns.
Overheating and Burns
One big risk is overheating, which can cause burns. Newborns, and premature ones in particular, can’t control their body heat well. Overheating happens if the equipment isn’t set right or if the baby is too close to the light.
- Inadequate monitoring of the infant’s temperature
- Incorrect settings on the phototherapy device
- Proximity of the infant to the light source
Inconsistent Light Delivery
Inconsistent light delivery is another problem. If the light isn’t steady, jaundice treatment might not work. This could mean more intense treatment or other steps are needed.
- Irregular maintenance of phototherapy equipment
- Technical malfunctions
- Improper use of the device
Electrical Safety Concerns
Electrical safety is a big deal with medical gear, like phototherapy devices. Electrical safety concerns come from bad wiring, wrong grounding, or damaged cords.
- Regular inspection of equipment for damage
- Adherence to manufacturer guidelines for maintenance
- Training for healthcare staff on electrical safety
In summary, phototherapy is vital for jaundice treatment in newborns. But, we must know the risks. Healthcare providers can make treatment safer and more effective by understanding these risks.
Limitations of Phototherapy Patches and Portable Devices
Phototherapy patches and portable devices are new and exciting. But, they have some big limitations that affect how well they work.
Efficacy Issues with Smaller Light Sources
The small lights in these devices can cause efficacy issues. They might not shine as brightly as older phototherapy units. This could mean treatments take longer or don’t work as well.
A study showed that patch-based therapy needed longer times to lower bilirubin levels as much as traditional therapy.
Coverage Problems and Uneven Treatment
Getting the patches or devices to cover the baby’s skin evenly is hard. If the device moves or is placed wrong, some spots might not get enough light.
This can cause some areas to not get enough light. This might mean bilirubin levels don’t drop enough.
Monitoring Challenges
It’s harder to check if phototherapy patches and portable devices are working right.
It’s key to keep an eye on bilirubin levels and the baby’s skin. This helps make sure the device is doing its job and makes any needed changes.
|
Device Type |
Efficacy |
Coverage |
Monitoring Ease |
|---|---|---|---|
|
Traditional Phototherapy |
High |
Excellent |
Easy |
|
Phototherapy Patches |
Variable |
Good |
Moderate |
|
Portable Devices |
Variable |
Good |
Moderate |
Home Phototherapy: Unique Disadvantages and Concerns
Phototherapy at home is becoming more common. It’s important to know the risks and challenges it brings. Treating newborns at home is convenient but comes with its own set of problems.
Inadequate Supervision and Monitoring
One big worry is inadequate supervision and monitoring. Hospitals have medical staff watching over treatment. But at home, parents have to follow instructions and watch for problems.
- Lack of continuous monitoring of bilirubin levels
- Inadequate observation for signs of dehydration or other side effects
- Potential for incorrect usage of the phototherapy device
Equipment Misuse Risks
Equipment misuse is another big concern. Parents might not know how to use the phototherapy equipment right. This can make treatment not work or even cause harm.
- Incorrect positioning of the light source
- Inadequate maintenance or cleaning of the device
- Misunderstanding the recommended treatment duration and intensity
Delayed Recognition of Complications
Delayed recognition of complications is a big issue with home phototherapy. Without doctors around, parents might not see serious problems like severe jaundice or dehydration right away.
To deal with these risks, we need to:
- Teach parents well about using phototherapy devices at home
- Make sure they see doctors regularly
- Get them to report any worries or side effects quickly
Intensive Phototherapy: Increased Risks and Side Effects
Intensive phototherapy is used when regular phototherapy doesn’t work for high bilirubin levels in newborns. It uses many light sources to get better results.
When Multiple Light Sources Are Required
For newborns with very high bilirubin, one light source might not be enough. Multiple light sources are used to cover more area. This is key for those at risk of severe bilirubin problems.
Studies show using many light sources can greatly help phototherapy (PMC10605061). But, it makes treatment more complex and requires careful watching.
Heightened Risk of Adverse Effects
Intensive phototherapy with many lights can lead to more problems. These include dehydration, electrolyte imbalances, and skin and eye damage. Careful monitoring is key to avoid these issues.
- Dehydration risk from more water loss.
- Electrolyte imbalances if not managed right.
- Skin rashes and other skin problems.
Monitoring Requirements
Newborns on intensive phototherapy need close monitoring. This includes checking bilirubin levels, hydration, and overall health. It’s vital to adjust treatment and avoid side effects.
Using UV sterilization lamps in phototherapy units also needs careful watching. It’s important to use them safely and effectively.
Pharmacological Side Effects of Adjunct Treatments
Adjunct treatments used with phototherapy can cause extra side effects. These treatments help make phototherapy work better or manage other conditions.
Medications Used Alongside Phototherapy
Many medications are used with phototherapy. They help make it more effective or manage side effects. Some examples include:
- Phenobarbital: Helps get rid of bilirubin faster.
- Intravenous immunoglobulin (IVIG): Lowers bilirubin levels in certain cases.
- Antibiotics: Used if there’s a chance of infection.
Each of these drugs can have its own side effects and how they interact with other drugs.
Drug Interactions and Complications
Drug interactions are a big worry with adjunct treatments and phototherapy. Some drugs can affect how bilirubin works in the body. This can increase the risk of serious problems like kernicterus.
|
Medication |
Potential Interaction |
Complication |
|---|---|---|
|
Phenobarbital |
Induces hepatic enzymes |
Alters metabolism of other drugs |
|
IVIG |
Aseptic meningitis |
Rare but serious complication |
|
Antibiotics |
Variable interactions with bilirubin |
Potential displacement of bilirubin from albumin |
Risk-Benefit Assessment
It’s very important to do a careful risk-benefit check when using adjunct treatments with phototherapy. Doctors need to think about the good things these treatments do against the possible bad side effects.
Choosing to use these treatments should be based on what each patient needs. They should be watched closely for any bad effects.
Alternative Approaches to Managing Neonatal Jaundice
Managing neonatal jaundice goes beyond just phototherapy. Other strategies are used based on the jaundice’s severity, cause, and the baby’s health. Phototherapy is a key treatment, but other methods are also important.
Exchange Transfusion: Indications and Risks
Exchange transfusion is a serious option for severe jaundice. It replaces the baby’s blood with donor blood to lower bilirubin quickly. This is needed when bilirubin levels are too high and could cause kernicterus, a serious brain damage risk.
Exchange transfusion is used when phototherapy doesn’t work, in hemolytic disease, and when bilirubin encephalopathy signs appear. But, it has risks like infections, blood clotting problems, and vascular access issues.
Intravenous Immunoglobulin Therapy
Intravenous immunoglobulin (IVIG) therapy is another option for neonatal jaundice, mainly for HDN. IVIG helps reduce the need for exchange transfusions and can lessen hemolysis severity.
IVIG can lessen jaundice by reducing red blood cell breakdown. But, it comes with risks like adverse reactions and the need for careful monitoring.
Enhanced Feeding Strategies
Enhanced feeding is a gentle yet effective way to manage neonatal jaundice. It involves making sure the baby drinks enough and eats often to help get rid of bilirubin. Breastfeeding is recommended because it helps with gut health and passing bilirubin.
Feeding often keeps the baby hydrated, which is key for bilirubin removal. Also, breastfeeding support is vital in neonatal care, providing many benefits beyond just treating jaundice.
Clinical Decision-Making: When Phototherapy’s Risks Outweigh Benefits
Clinicians must decide when phototherapy’s risks are too high for newborns. This is a big challenge in neonatal care. The newborn’s condition can change quickly.
Good decision-making means checking how severe neonatal jaundice is. It’s also about knowing when phototherapy is needed.
Severity Thresholds for Treatment
Guidelines say to start phototherapy based on bilirubin levels, age, and risk factors. Getting it right is key to treat just enough.
The American Academy of Pediatrics says to start phototherapy based on risk, age, and bilirubin levels. This way, treatment fits each newborn’s needs.
Risk Stratification Approaches
Risk stratification helps find out who’s at higher risk from jaundice or phototherapy. Premature birth, low weight, and hemolysis are important factors.
- Premature babies might need different treatment because they’re more vulnerable.
- Babies with hemolytic disease might need closer watch and treatment.
This helps doctors make better choices about phototherapy’s intensity and length.
Individualized Treatment Planning
Every newborn is different, so treatment must be tailored. The cause of jaundice, other health issues, and how well treatment works are all important.
“The goal of treatment is not just to reduce bilirubin levels but to do so in a way that minimizes risk and supports the overall health of the newborn.” –
Expert in Neonatal Care
By weighing these factors, doctors can create safe and effective treatment plans.
Conclusion: Balancing Necessity Against Disadvantages
Phototherapy is key in treating neonatal jaundice. Yet, it has downsides that must be thoughtfully weighed. Knowing about phototherapy and its use in treating high bilirubin levels is vital for doctors.
The downsides of phototherapy include short-term side effects, eye problems, and long-term risks. These must be balanced against its benefits. In some cases, other treatments like exchange transfusion or intravenous immunoglobulin therapy might be needed.
Understanding the risks and benefits of phototherapy is important. By recognizing its drawbacks and taking steps to lessen them, doctors can improve care for jaundiced newborns.
FAQ
What is phototherapy, and how is it used to treat neonatal jaundice?
Phototherapy uses light to lower bilirubin levels in the blood. This helps treat neonatal jaundice. It changes bilirubin into a form that’s easier to remove from the body.
What are the different types of phototherapy devices used in neonatal care?
There are several types of phototherapy devices. These include conventional units, fiber-optic blankets, and LED systems. Each type has its own use in treating jaundice in newborns.
References
New England Journal of Medicine. Evidence-Based Medical Insight. Retrieved from https://www.nejm.org/doi/full/10.1056/NEJMct0708377


































