Stem cell transplants offer hope for patients with life-threatening diseases. But what happens if a transplant fails? A failed transplant can be devastating. It’s important to understand the risks and complications.
Graft failure is a big risk, happening in about 5–10% of hematopoietic stem cell transplants. This can cause severe and potentially life-threatening problems.
When a transplant fails, patients face big challenges. They need to manage symptoms and look for new treatment options. It’s key for patients and healthcare providers to know the causes and how to manage them.
Key Takeaways
- Graft failure occurs in about 5-10% of hematopoietic stem cell transplants.
- A failed transplant can lead to severe and potentially life-threatening complications.
- Understanding the causes and management strategies is vital for patients and healthcare providers.
- Patients facing a failed transplant need to explore new treatment options.
- Managing symptoms is a significant challenge for patients with a failed transplant.
Understanding Stem Cell Transplants and Failure Risks
Stem cell transplants are a complex treatment for serious diseases. They are used to treat life-threatening conditions like cancer and autoimmune disorders. It’s important for patients to understand this treatment.
Types of Stem Cell Transplants: Autologous vs. Allogeneic
There are two main types of stem cell transplants. Autologous transplants use the patient’s own stem cells. These cells are collected, stored, and then given back after treatment.
Allogeneic transplants use stem cells from a donor. This type can fight cancer better but has a higher risk of graft-versus-host disease (GVHD). The choice depends on the patient’s health and the disease being treated.
|
Transplant Type |
Source of Stem Cells |
Risk of GVHD |
Risk of Relapse |
|---|---|---|---|
|
Autologous |
Patient’s own cells |
Low |
Higher |
|
Allogeneic |
Donor cells |
Higher |
Lower |
The Transplantation Process: What Happens During the Procedure
The process starts with a conditioning regimen. This involves chemotherapy and/or radiation to clear the bone marrow. Then, the stem cells are infused into the patient’s bloodstream.
After infusion, the stem cells go to the bone marrow. There, they start making new blood cells. A leading hematologist says, “The success of a stem cell transplant depends on the type, the patient’s health, and the medical team’s expertise.”
“The success of a stem cell transplant depends not only on the type of transplant but also on the patient’s overall health and the expertise of the medical team.” – Hematologist
How Bone Marrow Transplants Work in the Body
Bone marrow transplants replace damaged bone marrow with healthy stem cells. These can be from the patient or a donor. Once in the bone marrow, the stem cells start making new blood cells.
The process of bone marrow regeneration is complex. It involves many cell types working together. Understanding this is key to managing expectations and spotting complications early.
Defining Transplant Failure: Primary vs. Secondary Graft Failure

Stem cell transplant failure can happen in two ways: primary and secondary graft failure. It’s important to understand these to manage patient hopes and results.
Primary Graft Failure: When Stem Cells Don’t Engraft
Primary graft failure happens when the stem cells don’t settle in the bone marrow. This means they can’t make new blood cells, causing a lack of blood production. Many things can cause this, like problems with the stem cells or the treatment plan.
Secondary Graft Failure: When Initial Success is Followed by Loss
Secondary graft failure is when the stem cells first work, then stop. This can be due to rejection, infections, or other issues. It’s a big worry because it shows the transplant’s early success is at risk.
Incidence Rates: The 5-10% Failure Risk
About 5-10% of people who get stem cell transplants face graft failure, whether it’s primary or secondary. This risk highlights the need for close monitoring and care after the transplant.
|
Type of Graft Failure |
Description |
Incidence Rate |
|---|---|---|
|
Primary Graft Failure |
Failure of stem cells to engraft |
5-10% |
|
Secondary Graft Failure |
Initial engraftment followed by graft loss |
Early Warning Signs of Stem Cell Transplant Failure
It’s important for patients and caregivers to know the early signs of stem cell transplant failure. Spotting these signs early can lead to better treatment results.
Clinical Indicators of Potential Graft Failure
Signs of graft failure include persistent fever, fatigue, and shortness of breath. Watching for these symptoms can help catch problems early.
Bone Marrow Transplant Failure Symptoms
Symptoms of bone marrow transplant failure include infections, bleeding disorders, and anemia. These happen when the bone marrow doesn’t make enough blood cells. Knowing these symptoms is key to getting help fast.
Timeline: When Failure Typically Manifests
The time when stem cell transplant failure shows up can vary. The biggest risk is in the first few months. But, it’s important to keep watching for signs of failure even after that.
Staying alert to these early signs and knowing when failure might happen can help. It can lead to better treatment outcomes for patients and caregivers.
Major Causes of Stem Cell Transplant Failure
It’s important to know why stem cell transplants fail. This knowledge helps improve care for patients. There are many reasons why transplants might not work, and finding these reasons is key to better care.
Graft Rejection: When the Body Fights Back
Graft rejection happens when the body rejects the new stem cells. This can be due to genetic differences, not enough medicine to stop the immune system, or antibodies against the donor.
Disease Relapse: Signs of Relapse After Bone Marrow Transplant
Another big reason for transplant failure is disease relapse. This happens when cancer cells start growing again. It’s important to watch for signs of relapse to catch it early.
Infection Complications: A Major Risk Factor
Infections are a big risk for patients getting stem cell transplants. The treatment before the transplant weakens the immune system. Quick treatment of infections is key to avoiding transplant failure.
Graft-Versus-Host Disease (GVHD): When Donor Cells Attack
Graft-versus-host disease (GVHD) is when the donor’s immune cells attack the recipient’s body. GVHD can be acute or chronic and is a big problem after transplant. Managing GVHD is important to keep the patient safe.
|
Cause of Failure |
Description |
Management Strategies |
|---|---|---|
|
Graft Rejection |
Immune system rejects transplanted stem cells |
Immunosuppression, monitoring for donor-specific antibodies |
|
Disease Relapse |
Residual cancer cells begin to grow again |
Monitoring for signs of relapse, targeted therapies |
|
Infection Complications |
Weakened immune system increases infection risk |
Prompt diagnosis and treatment, antimicrobial prophylaxis |
|
GVHD |
Donor immune cells attack recipient tissues |
Immunosuppressive therapy, careful monitoring |
Knowing the main reasons for stem cell transplant failure is vital. It helps doctors find better ways to help patients. By understanding why transplants fail, doctors can give more personalized care.
Life Expectancy After Stem Cell Transplant: Success vs. Failure Scenarios
Life expectancy after a stem cell transplant can vary a lot. This depends on the disease being treated and how well the transplant goes.
Stem Cell Transplant Success Rates by Disease Type
Success rates for stem cell transplants change with each disease. For example, patients with multiple myeloma have a three-year survival rate of about 79% after a transplant.
Multiple Myeloma: 79% Three-Year Survival
Thanks to new treatments, survival rates for multiple myeloma patients have improved a lot.
Hodgkin Lymphoma: Up to 92% Success Rate
Hodgkin lymphoma patients have seen great success with stem cell transplants. Some studies show a 92% success rate.
Leukemia Stem Cell Transplant Outcomes
Leukemia patients face different outcomes with stem cell transplants. This depends on the type of leukemia and its stage at transplant time.
|
Disease Type |
Success Rate |
Three-Year Survival |
|---|---|---|
|
Multiple Myeloma |
75% |
79% |
|
Hodgkin Lymphoma |
92% |
85% |
|
Leukemia |
60-80% |
65-75% |
Stem Cell Transplant Death Rate Following Graft Failure
Graft failure is a serious issue that can affect life expectancy. It’s important to consider the death rate after graft failure for patients and doctors.
Life Span After Bone Marrow Transplant: Long-term Outlook
The long-term outlook after a bone marrow transplant depends on many things. These include the disease, the patient’s health, and any complications.
Knowing these factors helps manage expectations and make better treatment choices.
Bone Marrow Regeneration After Transplant
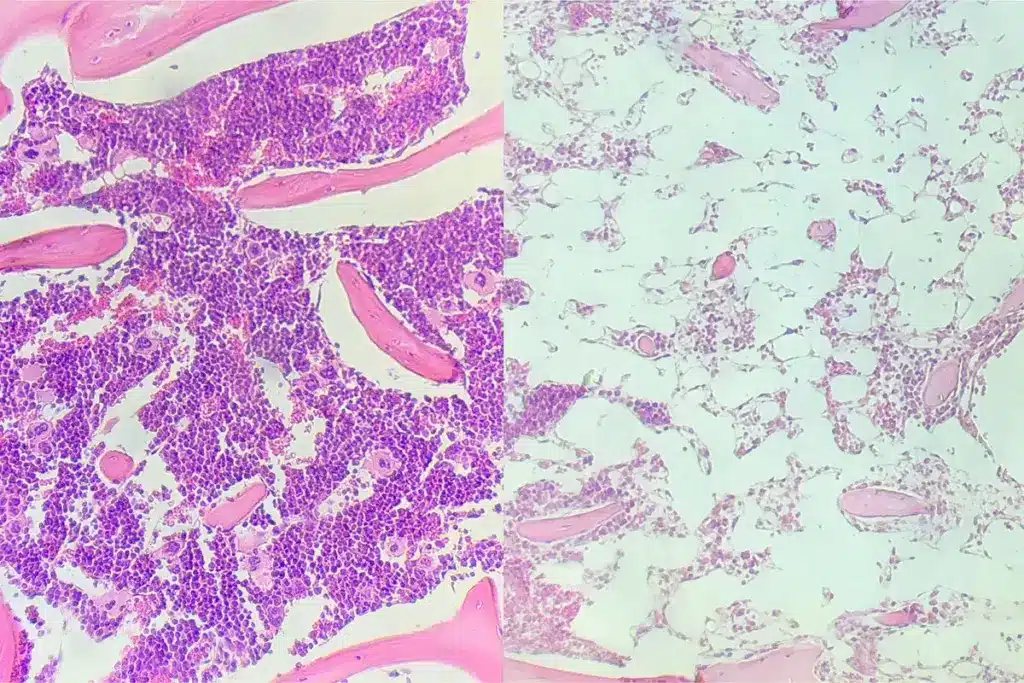
The process of bone marrow regeneration after a stem cell transplant is complex. The body starts to rebuild its bone marrow. This is key for making healthy blood cells.
Does Bone Marrow Grow Back After Transplantation?
Bone marrow can grow back after a transplant. This growth is helped by the stem cells used in the transplant. Successful engraftment of these stem cells is vital for bone marrow regeneration.
Can You Live Without Bone Marrow: Understanding the Risks
Living without bone marrow is risky. It can lead to severe infections and anemia because the body can’t make enough blood cells. The dangers of bone marrow failure highlight the need for successful regeneration after a transplant.
Timeline for Bone Marrow Recovery
The time it takes for bone marrow to recover varies. It usually takes weeks to months for it to produce blood cells normally. It’s important to have close monitoring by healthcare professionals during this time to handle any issues.
Immediate Interventions When a Transplant Fails
When a stem cell transplant fails, quick medical action is key. This is to manage complications and help patients get better. A failed transplant can cause serious health problems, so fast and effective care is needed.
Emergency Medical Management
Emergency care for graft failure is all about tackling health risks fast. Doctors give medicines to help bone marrow recover. They also fight infections and handle graft-versus-host disease (GVHD) issues. Quick treatment is vital to stop things from getting worse.
Supportive Care Measures
Supportive care is important for patients after a transplant fails. It includes helping with nutrition, counseling, and managing long-term problems. Good supportive care can really help patients feel better.
Decision-Making Timeline for Secondary Interventions
Deciding on next steps after a transplant fails is important. Doctors look at the patient’s health, figure out why the transplant failed, and choose the best course. This team effort might include thinking about a second transplant or other treatments.
|
Intervention Type |
Timeline |
Key Considerations |
|---|---|---|
|
Emergency Medical Management |
Immediate |
Addressing acute complications, stabilizing the patient |
|
Supportive Care Measures |
Ongoing |
Managing symptoms, improving quality of life |
|
Secondary Interventions |
Within weeks to months |
Evaluating the need for a second transplant or alternative treatments |
Understanding the quick steps needed when a transplant fails helps doctors care for patients better. This can lead to better health outcomes.
Second Transplant Considerations: Benefits and Risks
When a stem cell transplant fails, deciding on a second transplant is tough. It’s about weighing the good and bad sides. You need to look at the patient’s health, why the first transplant didn’t work, and what might happen with the second one.
Candidacy for a Second Transplant
To see if a patient can get a second transplant, doctors check their health and any other health issues. Those who are healthy and can handle another transplant are usually better candidates.
Finding a New Donor: Challenges and Solutions
Finding a donor for a second transplant can be hard. New ways to match donors and using different types of donors have helped. But, it takes time and more tests to make sure it’s safe.
Success Rates of Second Transplants
The success of a second transplant depends on many things. Like the disease, how long ago the first transplant was, and the patient’s health now. While some patients do well, the success rate is often lower than the first time.
Non-Relapse Mortality: The 48% Two-Year Risk
One big risk with second transplants is death from causes other than the disease. A study found a 48% risk of death from other causes within two years. This shows how important it is to choose carefully and take good care after the transplant.
|
Factor |
Consideration |
Impact on Outcome |
|---|---|---|
|
Patient Health |
Overall condition and comorbidities |
Significant impact on survival and success |
|
Donor Match |
Quality of the donor match |
Influences graft-versus-host disease and survival |
|
Disease Status |
Remission status at second transplant |
Affects relapse risk and overall survival |
Alternative Treatment Options When Transplantation Fails
For patients facing stem cell transplant failure, there are several alternative treatments. These options can offer new hope. It’s important to look into other treatments that might improve outcomes.
Immunotherapy Approaches
Immunotherapy is a promising option for those who have failed transplant. It uses the body’s immune system to fight diseases. Immunotherapies can be tailored to the individual patient’s needs, making treatment more personal.
What Happens If CAR T-Cell Therapy Fails
CAR T-cell therapy modifies T cells to attack cancer. Though promising, it may not work for everyone. In such cases, novel therapies and clinical trials are key for further treatment.
Novel Medications and Clinical Trials
Novel medications and clinical trials are alternatives for transplant failure. These treatments are at the forefront of research. They offer innovative solutions not found in standard treatments.
International Treatment Protocols and Innovations
International collaborations bring new therapies to patients worldwide.
Exploring these alternatives, patients and healthcare providers can find effective next steps. Even after transplant failure, there’s hope for treatment.
Long-Term Monitoring After Transplant Failure
Long-term monitoring is key for patients who have failed a stem cell transplant. This care is vital for managing chronic issues and keeping quality of life high.
Follow-Up Schedule and Important Assessments
After a transplant fails, we suggest a regular check-up schedule. This includes regular blood tests, bone marrow assessments, and imaging studies. These help catch problems early.
These steps help us tackle complications quickly. This improves the patient’s overall health.
Managing Chronic Complications
Chronic issues can pop up after a transplant fails. These include graft-versus-host disease (GVHD), infections, and organ damage. We help manage these with medication, lifestyle adjustments, and other support.
Quality of Life Considerations
Keeping quality of life in check is a big part of long-term care. We aim to help patients manage symptoms, stay physically active, and deal with emotional and psychological challenges.
Emotional and Psychological Impact of Transplant Failure
When a stem cell transplant fails, it affects more than just the body. It touches on deep emotional and psychological challenges. Patients and their families face a tough journey, filled with emotions and uncertainty.
Coping Strategies for Patients
Dealing with a failed stem cell transplant is complex. Professional counseling can help patients manage their emotions. Support groups, online or in-person, offer a sense of community and understanding.
It’s important for patients to talk openly with their healthcare team. This helps identify the need for more support or help.
Support Resources for Families
Families are key in supporting patients through stem cell transplants. When a transplant fails, families feel the emotional pain too. Family therapy can help them cope together and support each other.
Educational resources help families understand the medical and emotional sides of transplant failure. This knowledge empowers them to support their loved ones better.
Working Through Uncertainty and Fear
Uncertainty and fear are big challenges after a transplant fails. Patients and families must face these emotions head-on. Mindfulness practices and relaxation techniques can help manage anxiety and fear.
“The greatest glory in living lies not in never falling, but in rising every time we fall.” –
This quote shows the strength needed to overcome transplant failure. The journey is tough, but there are ways to cope and move forward.
|
Coping Mechanisms |
Benefits |
|---|---|
|
Professional Counseling |
Addresses emotional turmoil, provides guidance |
|
Support Groups |
Fosters community, reduces feelings of isolation |
|
Mindfulness Practices |
Reduces anxiety, promotes relaxation |
Conclusion: Navigating the Journey After Transplant Failure
Understanding stem cell transplant failure is key. We’ve looked at its causes, complications, and how to manage them. This includes early signs and other treatment choices.
Knowing the stem cell transplant journey is vital. It helps patients, caregivers, and doctors give the best care. If a transplant fails, it’s important to look at new treatment plans. This might include immunotherapy or new medicines.
Transplant failure is tough, but we’re here to help. By knowing the risks and challenges, we can improve care. This makes a big difference for patients.
FAQ
What happens if a stem cell transplant fails?
If a stem cell transplant fails, patients face serious risks. These include graft failure, disease relapse, infections, and GVHD. It’s important to understand the causes and how to manage them to improve outcomes.
What are the types of stem cell transplants?
There are two main types of stem cell transplants. Autologous transplants use the patient’s own stem cells. Allogeneic transplants use stem cells from a donor.
How does bone marrow regenerate after a transplant?
Bone marrow can grow back after a transplant. The time it takes varies. Usually, it takes a few weeks to months for bone marrow to regenerate.
Can you live without bone marrow?
Living without bone marrow is risky. It can lead to severe infections and anemia. Bone marrow is key for making blood cells, and without it, life is at risk.
What are the early warning signs of stem cell transplant failure?
Signs of graft failure include persistent cytopenias, recurrent infections, and disease relapse. Spotting these signs early is vital for timely medical action.
What causes stem cell transplant failure?
Failure can be due to graft rejection, disease relapse, infections, and GVHD. Knowing these causes helps in finding effective ways to manage them.
What is the life expectancy after a stem cell transplant?
Life expectancy after a transplant varies. It depends on the disease type and transplant success. Success rates and long-term outlook differ by disease.
What are the success rates of second transplants?
Second transplant success rates vary. Factors include the disease and donor availability. Non-relapse mortality is a big risk, with a 48% two-year risk.
What are the alternative treatment options when transplantation fails?
When transplantation fails, options include immunotherapy, CAR T-cell therapy, and new treatments. These may offer hope when transplants don’t work.
How do you manage chronic complications after transplant failure?
Managing chronic complications requires ongoing monitoring. Regular follow-ups and strategies to reduce late effects are key. Quality of life is also important.
What are the emotional and psychological impacts of transplant failure?
Transplant failure can be tough emotionally and psychologically. Patients and families need support. Coping strategies and resources are vital for dealing with uncertainty and fear.
What happens if CAR T-cell therapy fails?
If CAR T-cell therapy fails, patients may see disease progression or relapse. Other treatments, like new medications and clinical trials, might be considered.
References


































