Nephrology focuses on diagnosing and treating kidney diseases. The kidneys filter waste, balance fluids, regulate blood pressure, and manage acute and chronic conditions.
Send us all your questions or requests, and our expert team will assist you.
Nephrology is the medical specialty focused on the diagnosis and treatment of kidney diseases. The kidneys are vital organs responsible for filtering waste from the blood, regulating fluid balance, and managing blood pressure. This field addresses everything from sudden kidney injury to long-term chronic kidney disease. Nephrology aims to preserve kidney function and manage the systemic complications that arise when kidneys fail.
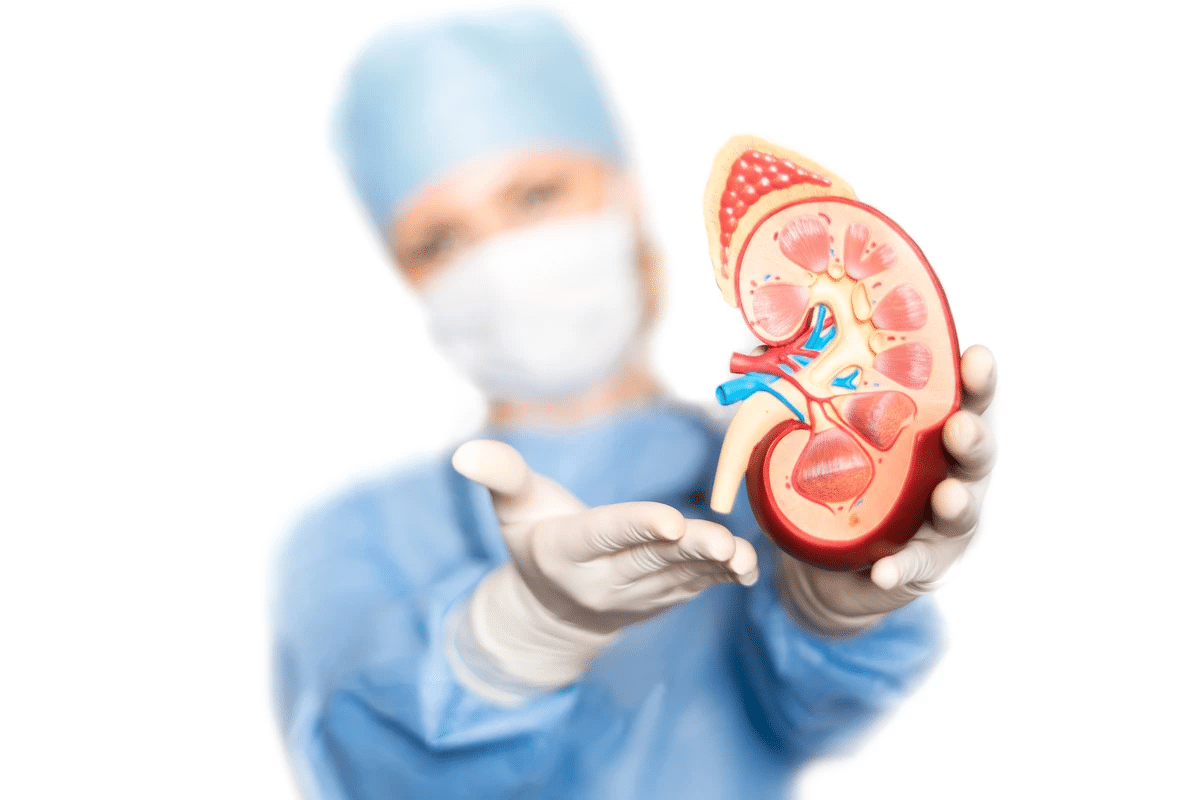
The kidneys are two bean-shaped organs, each about the size of a fist. Their primary role is to act as a sophisticated filtration system. They remove waste products, toxins, and excess fluid from the body, which are then excreted as urine. In addition, the kidneys produce hormones that help control blood pressure, stimulate red blood cell production, and maintain bone health by activating Vitamin D.
A nephrologist is a medical doctor who specializes in kidney care. They have advanced training in kidney diseases, kidney failure, and the systemic effects of kidney dysfunction, such as hypertension. Patients are often referred to a nephrologist when they show signs of decreased kidney function, significant protein or blood in the urine, or have complex conditions like kidney stones or uncontrolled high blood pressure.
Nephrologists manage a broad spectrum of kidney-related issues. These include:

Kidney disease is often referred to as a “silent” condition because symptoms may not become apparent until significant function has been lost. Understanding the subtle signs and primary causes is essential for early detection and intervention.
In the early stages, many people have no symptoms. As the disease progresses, individuals may experience:
The two leading causes of chronic kidney disease are diabetes (Type 1 or Type 2) and high blood pressure (hypertension). These conditions damage the small blood vessels in the kidneys over time. Other risk factors include:
Send us all your questions or requests, and our expert team will assist you.

You should see a doctor if you experience any persistent symptoms of kidney disease. Your primary care physician may refer you to a nephrologist if routine blood or urine tests reveal potential problems, such as high creatinine levels or protein in the urine. Individuals with high-risk conditions, such as diabetes or uncontrolled hypertension, should have their kidney function monitored regularly.
A precise diagnosis is the foundation of an effective kidney care plan. Nephrologists use a series of tests to understand the complete picture of your kidney health. This process is not just about identifying a problem; it is about determining its severity and underlying cause. By evaluating blood, urine, and imaging, the medical team can assess the glomerular filtration rate (GFR), which measures how well the kidneys are filtering. This data is essential for staging chronic kidney disease (CKD) and guiding subsequent treatment decisions.
The diagnostic process typically begins with simple, non-invasive tests:
Chronic Kidney Disease is classified into five stages based on the eGFR. Staging helps doctors create an appropriate treatment plan to slow the progression of the disease.
To determine the underlying cause of kidney damage, a nephrologist may order imaging tests like an ultrasound or a CT scan. These tests can reveal abnormalities in kidney size or structure, or identify blockages such as kidney stones or tumors. In some cases, a kidney biopsy may be performed. This involves taking a tiny sample of kidney tissue with a needle for examination under a microscope, which can provide a definitive diagnosis of conditions such as glomerulonephritis.


Treatment in nephrology is highly personalized, aiming to slow disease progression, manage symptoms, and maintain quality of life. The approach depends on the specific condition and its stage. For early-stage disease, this often involves lifestyle changes and medications. For advanced kidney failure, renal replacement therapies are necessary. These sophisticated treatments require specialized medical oversight to manage the patient’s complex needs effectively.
For early to moderate CKD, the primary goal is to slow its progression and manage underlying causes. This includes:
When the kidneys fail (Stage 5 CKD), renal replacement therapy is required to perform the kidneys’ functions. There are two main types of dialysis:
A kidney transplant is the preferred treatment for end-stage renal disease for medically eligible patients. This surgical procedure involves placing a healthy kidney from a living or deceased donor into the patient’s body. A successful transplant offers the best chance for a longer, higher-quality life, freeing the patient from dialysis. After transplantation, patients must take lifelong immunosuppressive medications to prevent organ rejection.

Choosing the right center for kidney care is crucial, as many conditions require long-term, specialized management. A successful nephrology department combines advanced diagnostic technology with a compassionate, multidisciplinary team. This integrated approach ensures that patients receive comprehensive care, from early detection and risk management to the most advanced treatments for kidney failure. Our focus is on providing a supportive environment led by expert physicians dedicated to preserving kidney function.
Kidney disease affects the entire body. Our nephrologists work closely with other specialists, including cardiologists, endocrinologists, and vascular surgeons, to manage the complex needs of our patients. This collaborative “kidney care team” also includes specialized dietitians to provide nutritional counseling and social workers to support patients through the challenges of chronic illness.
We provide a full spectrum of advanced treatments for kidney failure. Our medical center is equipped with state-of-the-art hemodialysis units, offering safe and comfortable treatment. We also provide comprehensive training and support for patients who choose home dialysis, including peritoneal dialysis, empowering them to manage their care in their own environment. Our team is also highly experienced in managing the complex care required before and after kidney transplantation.
We believe in a partnership with our patients. Managing a chronic condition like kidney disease is a lifelong journey. Our team is dedicated to patient education, helping individuals understand their condition and actively participate in their treatment plan. We prioritize clear communication and accessible care, ensuring that every patient feels heard, supported, and confident in their medical team.
