Nephrology focuses on diagnosing and treating kidney diseases. The kidneys filter waste, balance fluids, regulate blood pressure, and manage acute and chronic conditions.
Send us all your questions or requests, and our expert team will assist you.
Overview and Definition
Renal osteodystrophy is a medical term that describes the changes in bone structure and health that occur as a direct result of chronic kidney disease. Most people think of the kidneys as organs that filter waste and make urine, but they are actually the body’s main chemists. They are responsible for maintaining the precise balance of minerals, electrolytes, and hormones that keep our skeleton strong and durable. When the kidneys begin to fail, this delicate balance is disrupted, leading to significant changes in how bone is built and maintained. This condition is part of a broader systemic issue often referred to by doctors as Chronic Kidney Disease-Mineral and Bone Disorder, or CKD-MBD.
For patients and their families, understanding renal osteodystrophy is a crucial part of managing kidney disease. It helps explain why a condition affecting an organ in the lower back can eventually lead to pain in the hips, legs, or joints. It is not simply a matter of weak bones like osteoporosis, although the two conditions share some similarities. Instead, it is a complex metabolic disorder where the body struggles to regulate calcium and phosphorus, leading to bones that may be too weak, too brittle, or even too soft. Recognizing the connection between kidney function and bone health empowers patients to take proactive steps in their diet and medication routine to protect their mobility and quality of life.
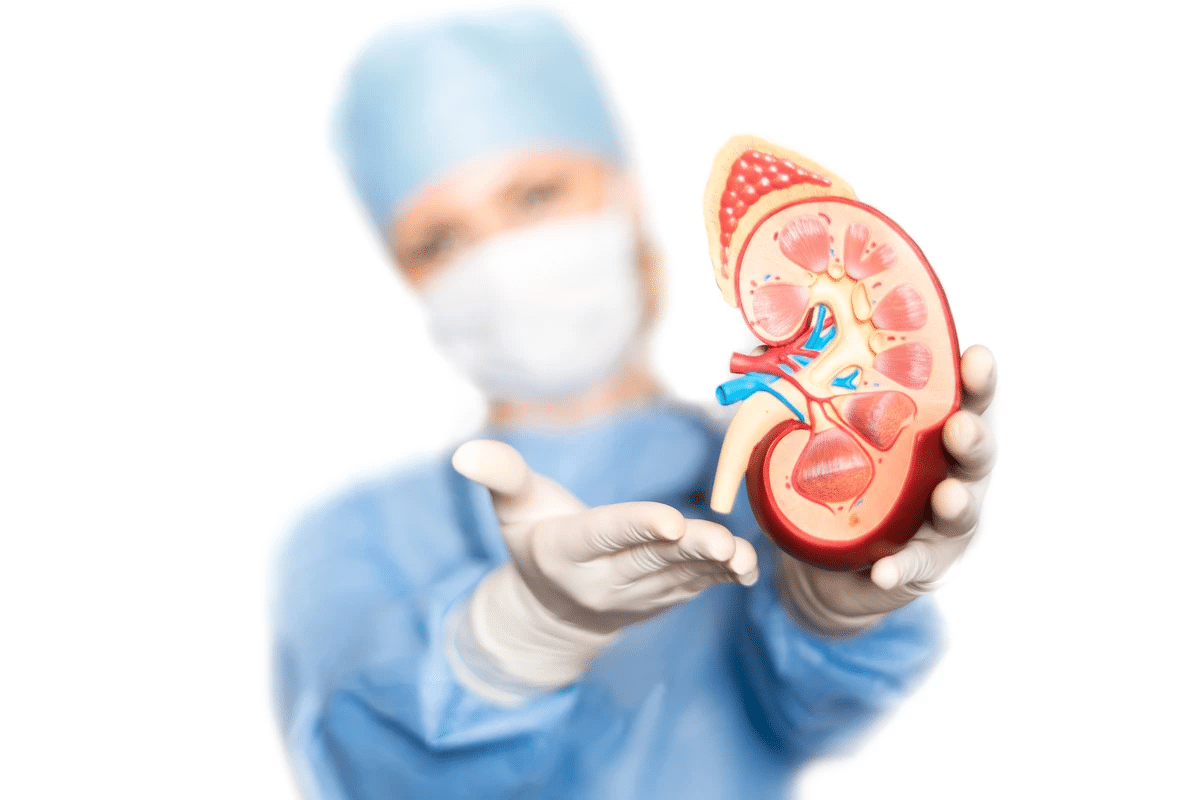
To understand why bone disease happens in kidney patients, we must first look at the vital relationship between the kidneys and the skeleton. Healthy kidneys perform two essential jobs for bone health. First, they balance phosphorus and calcium in the bloodstream. Phosphorus is a mineral found in many foods, and we need it for energy and cell repair. However, too much phosphorus pulls calcium out of the bones, making them weak. Healthy kidneys flush out excess phosphorus in the urine. When kidneys are damaged, phosphorus builds up in the blood, acting like a magnet that strips calcium from the skeleton.
Second, the kidneys are responsible for activating vitamin D. We absorb vitamin D from the sun and food, but it is inactive until it passes through the kidneys. Once activated, this vitamin acts like a key that unlocks the door for calcium to be absorbed from our food into our bodies. Without healthy kidneys, the body cannot use vitamin D efficiently. This process leads to a drop in blood calcium levels. The body, desperate for calcium to keep the heart and nerves working, steals it from the largest calcium bank in the body: the bones. This continuous theft of calcium weakens the bone structure over time.
Renal osteodystrophy specifically refers to the physical changes in the bone tissue itself. It is the skeletal component of the broader mineral and bone disorder. Doctors assess this condition by measuring bone turnover, mineralization, and volume. In a healthy body, bone is constantly being broken down and rebuilt in a balanced cycle. This process is called remodeling. In renal osteodystrophy, this cycle is broken.
Depending on the specific chemical imbalances in the blood, the bone turnover might become dangerously high or dangerously low. High turnover means the bone is being broken down faster than it can be built properly, often due to high levels of parathyroid hormone. Low turnover means the bone The bone has become lazy and is not renewing itself, which makes it old and brittle. Both states lead to bones that are prone to fracture and unable to repair themselves effectively.
The parathyroid glands are four tiny glands located in the neck, just behind the thyroid. They act as the thermostat for calcium in the body. Their job is to produce parathyroid hormone (PTH). When the glands sense that calcium levels in the blood are low—a common occurrence in kidney disease—they release more PTH. This hormone travels to the bones and commands them to release calcium into the bloodstream to compensate for the deficit.
In the early stages of kidney disease, this system works to keep blood calcium normal. However, as kidney disease progresses and phosphorus levels rise while vitamin D levels fall, the parathyroid glands work overtime. They eventually grow larger and become stuck in the “on” position, pumping out massive amounts of PTH constantly. This condition is called secondary hyperparathyroidism. The excess hormone causes the bone cells to go into overdrive, aggressively breaking down bone tissue to release minerals, leaving the skeleton weak and fibrous.
This specific diagnosis frequently coexists with renal osteodystrophy. “Secondary” means the parathyroid glands are actually healthy, but they are reacting to a problem elsewhere (the failing kidneys). “Hyper” means overactive. Treating this condition is often the primary way doctors try to correct the bone disease. By controlling the hormone levels, they can slow down the destruction of bone tissue.
Normally, when calcium levels rise back to normal, the parathyroid glands shut off. In kidney patients, because the kidneys cannot activate vitamin D (which helps shut off the glands) and because phosphorus remains high (which stimulates the glands), the feedback loop fails. The glands never receive the signal to stop, leading to a relentless attack on the bones unless medical intervention occurs.

Doctors classify renal osteodystrophy into different types based on what is happening at the cellular level. Knowing the type helps determine the treatment, as the wrong medication could make the problem worse. The most common form is characterized by high bone turnover, often called osteitis fibrosa cystica. In this type, the high levels of PTH cause the bone to become soft and deformed, with fibrous tissue replacing solid bone.
On the other end of the spectrum is adynamic bone disease. This is a condition of low bone turnover. Here, the bone cells have essentially gone dormant. The bone is not being broken down, but it is also not being rebuilt or repaired. This often happens if PTH levels are suppressed too much by medication or if there is a history of diabetes. These bones are very brittle and can break because microscopic cracks are not repaired. Another form is osteomalacia, where the bone forms but fails to harden because of a lack of vitamin D or mineral buildup, leading to soft, bendable bones.
Renal osteodystrophy is a risk for almost anyone with chronic kidney disease, but the severity usually correlates with the stage of kidney failure. It is rarely seen in Stage 1 or 2 CKD. Changes in blood chemistry typically begin in Stage 3, often silently. By the time a patient reaches Stage 4 or Stage 5 (kidney failure requiring dialysis), nearly all patients have some degree of bone pathology, even if they do not yet feel pain.
Children with kidney disease are at particularly high risk because their bones are still growing. Renal osteodystrophy can lead to skeletal deformities, stunted growth, and bowed legs in pediatric patients. Adults on dialysis are also a major risk group. The dialysis process itself does not perfectly mimic the kidney’s ability to balance minerals, requiring patients to be extremely vigilant with their diet and medications to protect their bones.
The disorder does not just stay in the bones. When calcium and phosphorus levels in the blood are too high, they can combine to form dense crystals. The crystals settle in soft tissues as a result of the bones’ resistance to absorbing these minerals. This is called extraskeletal calcification. These gritty deposits can form in the heart valves, lungs, eyes, and most dangerously, in the blood vessels.
When blood vessels calcify, they turn from flexible tubes into stiff, hard pipes. This makes the heart work much harder to pump blood, leading to high blood pressure and an increased risk of heart attack and stroke. This phenomenon explains why doctors are so aggressive about treating mineral bone disorders. It’s not just about avoiding broken hips; it’s also about protecting the heart and preventing artery hardening.


With patients from across the globe, we bring over three decades of medical

Response within 2 hours during business hours
By clicking "Send Request", you agree to our terms and to share your contact info with the clinic.
Was this article
helpful?
Send us all your questions or requests, and our expert team will assist you.
Osteoporosis is a general thinning of bones due to aging or hormonal changes. Renal osteodystrophy is caused specifically by the chemical imbalances of kidney failure and involves complex changes in bone turnover, not just thinning.
Usually, you cannot feel the early stages of the disease. It is often a silent condition until it progresses to a point where it causes deep bone pain or a fracture occurs.
Not necessarily. While milk has calcium, it is also very high in phosphorus, which is dangerous for kidney patients. You should follow your renal dietitian’s advice regarding dairy products.
A transplant restores kidney function and can resolve many chemical imbalances, allowing bones to heal over time. However, some bone damage may be permanent, and monitoring is still needed.
Medication and diet can reverse many of the chemical imbalances. While severe bone deformities may not fully resolve, treating the condition can strengthen bones and prevent future fractures.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)