Neurology diagnoses and treats disorders of the nervous system, including the brain, spinal cord, and nerves, as well as thought and memory.
Send us all your questions or requests, and our expert team will assist you.
Overview and Definition
Chronic pain, when viewed through the lens of neurology, is often fundamentally different from the acute pain caused by a simple injury. While acute pain serves as a warning system for tissue damage, chronic neurological pain is a disease of the nervous system itself. It is defined as pain that persists or recurs for more than three months, long after the initial injury has healed, or pain that arises directly from a lesion or disease affecting the somatosensory system.
In neurology, this is often termed neuropathic pain. It occurs because the nerves themselves are damaged or malfunctioning, sending incorrect signals to the brain. This maladaptive plasticity means the brain learns to be in pain, rewiring neural pathways to amplify sensation, a phenomenon known as central sensitization.
The scope of chronic neurological pain includes conditions like trigeminal neuralgia, post-herpetic neuralgia, complex regional pain syndrome (CRPS), and central pain syndrome following a stroke or spinal cord injury. The mechanisms involve both the peripheral and central nervous systems. Peripheral sensitization occurs when nerve endings become hypersensitive to stimuli.
Central sensitization happens in the spinal cord and brain, where the threshold for pain is lowered, and non-painful stimuli (like a light touch) are perceived as painful (allodynia). Understanding these mechanisms is crucial because standard painkillers like ibuprofen or opioids are often ineffective for this type of pain, requiring medications that target nerve transmission instead.
Symptoms and Risk Factors
The symptoms of chronic neurological pain are distinct from the aching or throbbing of muscle or joint pain. Patients often describe the sensation as burning, shooting, electric shock-like, or stabbing. Pins and needles (paresthesia) or numbness in the affected area are common. Allodynia, where a bedsheet or a gentle breeze causes severe pain, is a hallmark sign of nerve sensitization.
Hyperalgesia is another common symptom, where a mildly painful stimulus feels excruciating. In conditions like CRPS, there may also be autonomic symptoms, such as changes in skin color, temperature, or sweating patterns in the affected limb, indicating involvement of the sympathetic nervous system.
The causes of chronic neurological pain are diverse. Diabetes is a leading cause, resulting in diabetic neuropathy where high blood sugar damages peripheral nerves. Shingles can lead to post-herpetic neuralgia, leaving patients with severe pain long after the rash clears. Traumatic injuries that sever or compress nerves, such as herniated discs or carpal tunnel syndrome, can transition into chronic pain states.
Chemotherapy and certain viral infections like HIV can also damage nerve fibers. Genetic factors may predispose some individuals to lower pain thresholds or greater susceptibility to central sensitization. Furthermore, psychological stress and depression can exacerbate the perception of pain through shared neurotransmitter pathways in the brain.
Diagnosis and Imaging
Diagnosis relies heavily on a precise history and neurological examination. The neurologist looks for sensory deficits, changes in reflexes, and signs of muscle wasting. Quantitative Sensory Testing (QST) may be used to measure the detection thresholds for vibration, temperature, and pain, helping to quantify the loss or gain of sensory function. Electromyography (EMG) and Nerve Conduction Studies (NCS) are critical for testing the health of the large nerve fibers, determining if the damage is axonal (affecting the nerve fiber) or demyelinating (affecting the protective coating).
While standard MRI scans are often normal in neuropathic pain (unless there is structural compression), advanced imaging techniques are revealing the brain’s role in chronic pain. Functional MRI (fMRI) can show altered activity in the “pain matrix” of the brain, including the anterior cingulate cortex and insula. High-resolution MRI neurography uses special sequences to visualize peripheral nerves directly, identifying areas of inflammation or entrapment that are invisible on regular scans. These tools help confirm that the pain is not “in the patient’s head” in a psychological sense, but is a physiological dysfunction of neural processing.
Treatment and Rehabilitation
Treating chronic neurological pain requires a different arsenal than nociceptive pain. First-line treatments often include anticonvulsants (like gabapentin or pregabalin) and antidepressants (like amitriptyline or duloxetine). These drugs work by calming overactive nerves or boosting the body’s natural pain-inhibiting pathways.
Topical treatments like lidocaine patches or capsaicin cream can help localize peripheral pain. Opioids are generally avoided due to the risk of dependence and low efficacy for nerve pain. For severe cases, nerve blocks or botulinum toxin injections may be used to interrupt pain signals temporarily.
When medications fail, neuromodulation offers hope. Spinal cord stimulation (SCS) involves implanting a device that sends electrical pulses to the spinal cord, masking pain signals before they reach the brain. Transcranial Magnetic Stimulation (TMS) is a non-invasive option that uses magnetic fields to stimulate nerve cells in the brain to control pain.
Physical therapy is essential to prevent stiffness and muscle atrophy, often using desensitization techniques to help the brain re-adapt to touch. Cognitive Behavioral Therapy (CBT) is also a key component, helping patients manage the emotional toll of chronic pain and reducing the anxiety that amplifies pain perception.
Long-Term Care
Chronic pain management is typically a lifelong process rather than a cure. The goal is often to reduce pain to a manageable level rather than eliminate it entirely. Long-term care involves regular monitoring to adjust medications and manage side effects. Patients are encouraged to adopt “pacing” strategies—balancing activity with rest to avoid flare-ups. Sleep hygiene is critical, as poor sleep lowers the pain threshold. Engaging in low-impact exercise like swimming can help maintain mobility without stressing sensitized nerves.
The most effective long-term care comes from a multidisciplinary pain clinic. This team may include neurologists, pain specialists, physiotherapists, and psychologists working together. They address the biopsychosocial aspects of pain, recognizing that social isolation and job loss are real consequences of the condition.
Support groups provide a vital connection to others facing similar challenges. By addressing the physical, emotional, and social impacts of chronic neurological pain, patients can improve their quality of life and regain functional independence despite the persistence of symptoms.

Send us all your questions or requests, and our expert team will assist you.
Neurologically, chronic pain is a condition in which the nervous system continues to generate pain signals beyond normal healing. It reflects altered nerve and brain processing rather than ongoing injury alone.
Acute pain is short lived and protective, while chronic pain persists and becomes a disorder of pain processing pathways. The nervous system itself plays a central role in chronic pain.
Yes, chronic pain can occur even when imaging is normal. Functional changes in nerve signaling and brain processing can sustain pain without structural damage.
In many cases, yes. Chronic pain is increasingly recognized as a neurological disease involving maladaptive neural circuits.
It lasts because the nervous system undergoes lasting changes that maintain pain signaling. These changes do not automatically reverse when the original injury heals.

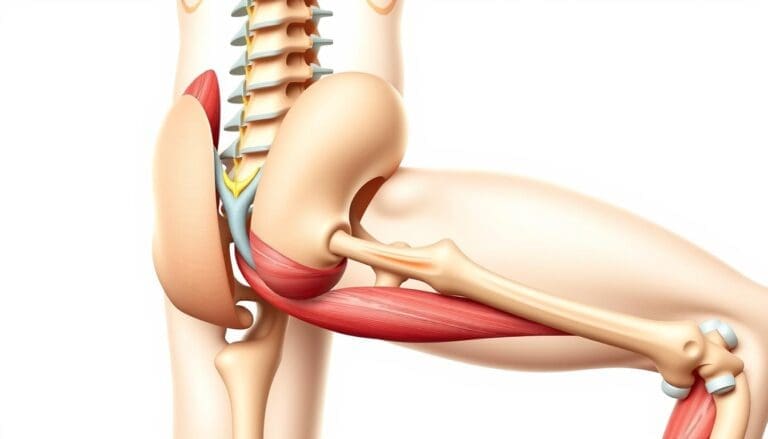 Chronic Pain
Chronic Pain Chronic Pain
Chronic Pain Chronic Pain
Chronic Pain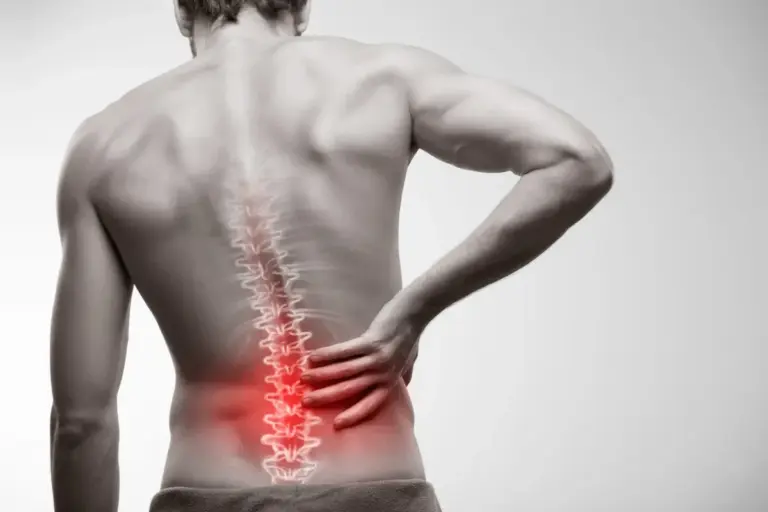 Chronic Pain
Chronic Pain Chronic Pain
Chronic Pain Chronic Pain
Chronic Pain
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)