Neurology diagnoses and treats disorders of the nervous system, including the brain, spinal cord, and nerves, as well as thought and memory.
Send us all your questions or requests, and our expert team will assist you.
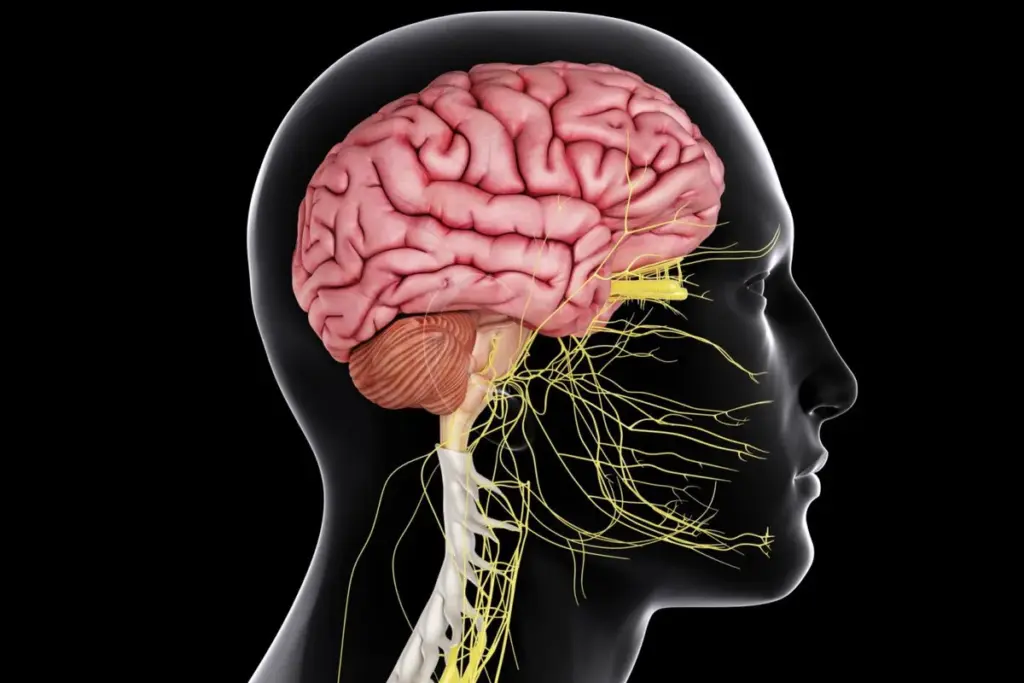
Psychoneuroimmunology, often abbreviated as PNI, is an integrative medical discipline that studies the complex, multidirectional communications between the central nervous system, the endocrine system, and the immune system. Historically, these systems were viewed as autonomous entities, functioning independently of one another. However, rigorous scientific inquiry over the last few decades has dismantled this isolationist view, revealing a unified network where psychological processes directly influence physiological function and vice versa.
The core premise of PNI is that the mind and body are biologically inseparable. Thoughts, emotions, and stress perceptions are not abstract concepts confined to the brain; they are transduced into chemical signals that circulate throughout the body, binding to receptors on immune cells. This dialogue determines the body’s ability to defend against infection, repair tissue damage, and distinguish self from non self.
This field operates on the understanding that the brain speaks to the immune system through two primary pathways: the autonomic nervous system and the neuroendocrine system. Conversely, the immune system speaks to the brain through chemical messengers called cytokines. This feedback loop explains phenomena such as “sickness behavior,” where the immune system manipulates the brain to induce lethargy and social withdrawal to conserve energy for healing.
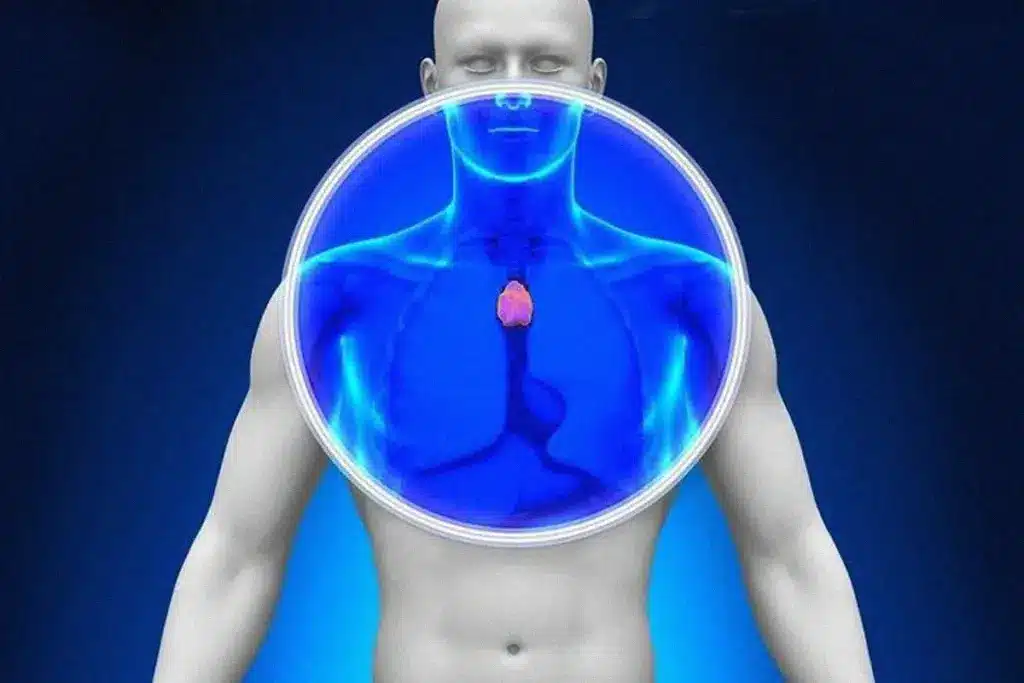
The HPA axis is the body’s primary stress management system and a central focus of psychoneuroimmunology research. When the brain perceives a threat, whether physical or psychological, the hypothalamus releases corticotropin releasing hormone (CRH). This triggers the pituitary gland to release adrenocorticotropic hormone (ACTH), which travels to the adrenal glands sitting atop the kidneys.
The end result of this cascade is the production of glucocorticoids, primarily cortisol in humans. Cortisol is a profound modulator of the immune system. In acute bursts, it prepares the body for action and prevents the immune system from overreacting to injury. It suppresses inflammation and redistributes white blood cells to the skin and lymph nodes, preparing the body for potential physical trauma.
However, when this system is chronically activated due to sustained psychological stress, the delicate balance collapses. The immune cells can become resistant to the signaling of cortisol, a phenomenon known as glucocorticoid resistance. This means that despite high levels of stress hormones, the immune system stops listening and produces runaway inflammation, contributing to chronic disease states.
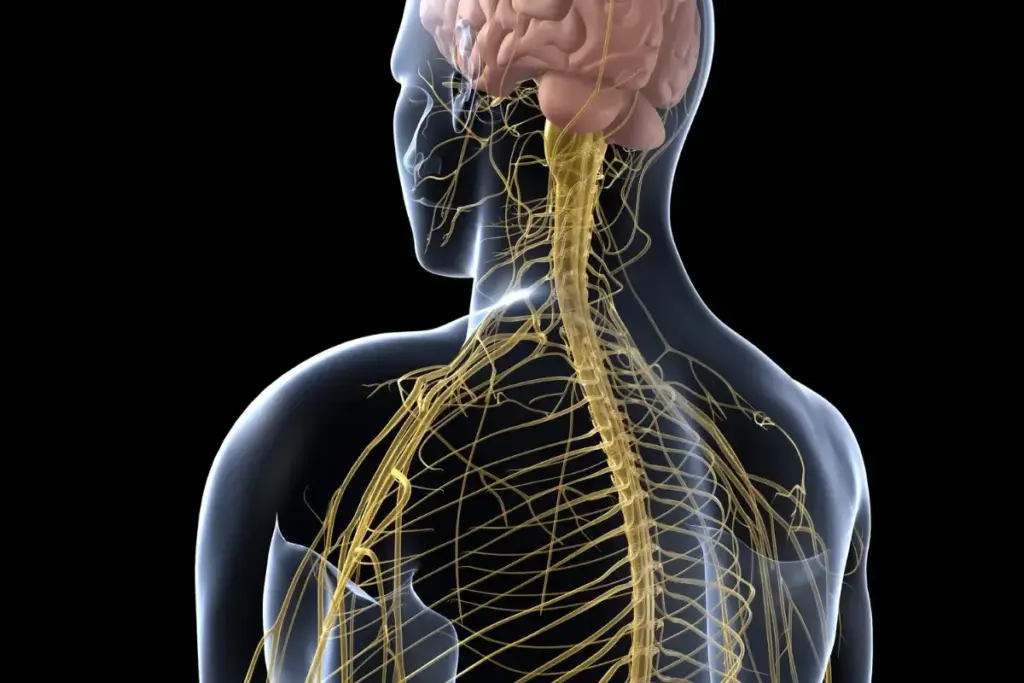
Parallel to the HPA axis is the Sympathetic-Adrenal-Medullary (SAM) axis, often referred to as the “fight or flight” system. This system utilizes the hardwired nerves of the autonomic nervous system to deliver messages instantly to immune organs. Nerves from the sympathetic system innervate the bone marrow, thymus, spleen, and lymph nodes, providing a direct physical connection between the brain and immunity.
When activated, these nerves release catecholamines—norepinephrine and epinephrine (adrenaline). Immune cells, including macrophages and lymphocytes, possess receptors for these chemicals on their surface. When norepinephrine binds to these receptors, it triggers intracellular pathways that can alter the transcription of genes within the immune cell.
This pathway explains why acute stress can temporarily boost specific immune functions, such as the number of Natural Killer cells in the blood. However, chronic sympathetic overactivity leads to a pro inflammatory gene expression profile. The immune system shifts towards producing inflammatory chemicals while simultaneously suppressing the antiviral response, leaving the host vulnerable to viral infections and cancer progression.
Communication in PNI is not a one way street from brain to body; the immune system also talks back to the brain. This occurs primarily through cytokines, which are small protein signaling molecules used by immune cells. Pro inflammatory cytokines, such as Interleukin 1 (IL 1), Interleukin 6 (IL 6), and Tumor Necrosis Factor alpha (TNF alpha), can signal the central nervous system.
While cytokines are too large to cross the blood brain barrier freely, they utilize active transport channels or bind to the vagus nerve to send signals to the brainstem. Once the brain receives the message that inflammation is present in the body, it initiates a distinct behavioral program known as “sickness behavior.”
Sickness behavior is characterized by fatigue, loss of appetite, loss of interest in social interaction (anhedonia), and increased sleepiness. In an acute infection, this is adaptive; it forces the organism to rest and conserve energy for the fever response. However, in chronic inflammation, these cytokines can lead to persistent depressive symptoms, brain fog, and fatigue syndromes, illustrating the immune basis of many psychiatric conditions.
Modern psychoneuroimmunology has expanded to include the critical role of the gut microbiome. The intestines house the largest collection of immune cells in the body (GALT – Gut Associated Lymphoid Tissue) and trillions of bacteria. These bacteria communicate with the host’s nervous and immune systems, forming a triad of regulation.
Stress can alter the composition of the gut bacteria, reducing diversity and promoting the growth of opportunistic pathogens. This state, known as dysbiosis, can compromise the intestinal lining, allowing bacterial products to leak into the bloodstream (“leaky gut”). This leakage triggers a systemic immune response, which in turn affects the brain, creating a vicious cycle of stress and inflammation.
Conversely, a healthy microbiome produces short chain fatty acids like butyrate, which have potent anti inflammatory and neuroprotective effects. Research suggests that targeting the microbiome via diet or probiotics can influence the brain’s stress response and the immune system’s reactivity, offering new avenues for PNI based treatments.


With patients from across the globe, we bring over three decades of medical

Response within 2 hours during business hours
By clicking "Send Request", you agree to our terms and to share your contact info with the clinic.
Was this article
helpful?
Send us all your questions or requests, and our expert team will assist you.
The main goal is to scientifically understand the biological mechanisms by which the brain and the immune system communicate, explaining how mental states affect physical health and how physical illness affects mental health.
While related, PNI provides the molecular and cellular evidence for the connections that psychosomatic medicine describes clinically, moving beyond theory to measurable biomarkers like cytokines and hormones.
Positive thinking alone is not a cure, but PNI research shows that reducing stress and maintaining a positive affect can lower inflammation and improve immune function, which supports conventional medical treatments.
The immune system talks to the brain by releasing chemical messengers called cytokines into the blood, which signal the brain directly or stimulate the vagus nerve to send “sickness signals” to the brainstem.

 Neurology
Neurology
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)