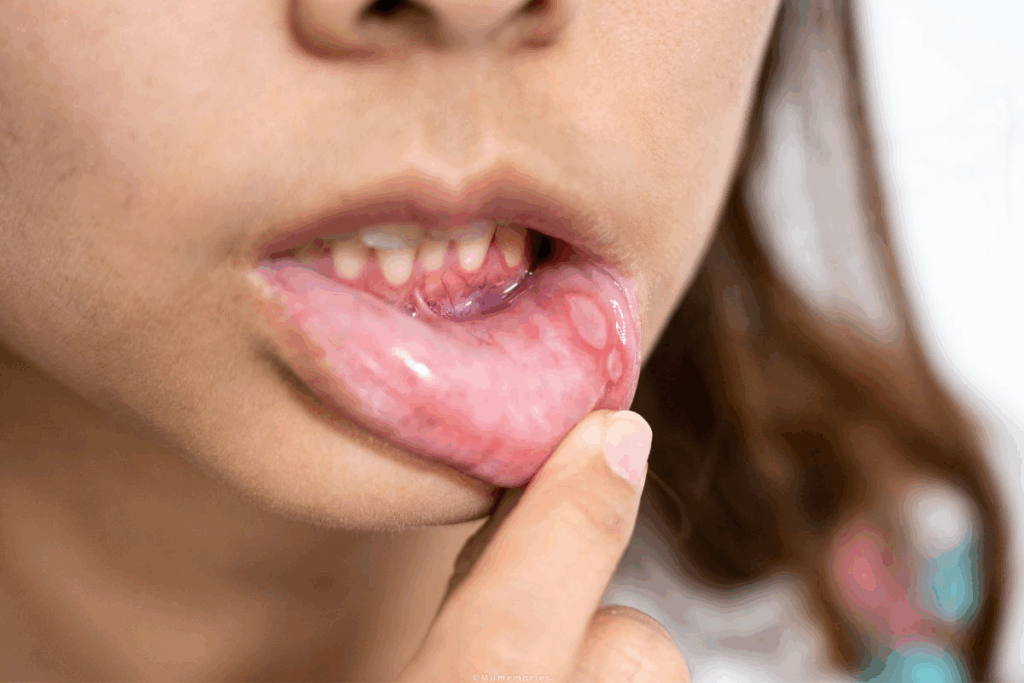
Oral leukoplakia is a condition with white spots in the mouth. It’s important to understand this because it can turn into oral cancer. It affects about 3.41% of people worldwide. This is your ultimate oral leukoplakia definition guide. Learn what this precancerous white patch is and why it’s so critical to treat.
Early detection and treatment of this condition are key. At Liv Hospital, we focus on your health. We aim to diagnose and treat you thoroughly.
Key Takeaways
- Oral leukoplakia is a potentially malignant disorder.
- It is characterized by white lesions in the mouth.
- Early detection is key for effective management.
- The global prevalence is about 3.41%.
- Liv Hospital offers complete care for diagnosis and treatment.
Oral Leukoplakia Definition: A Comprehensive Overview
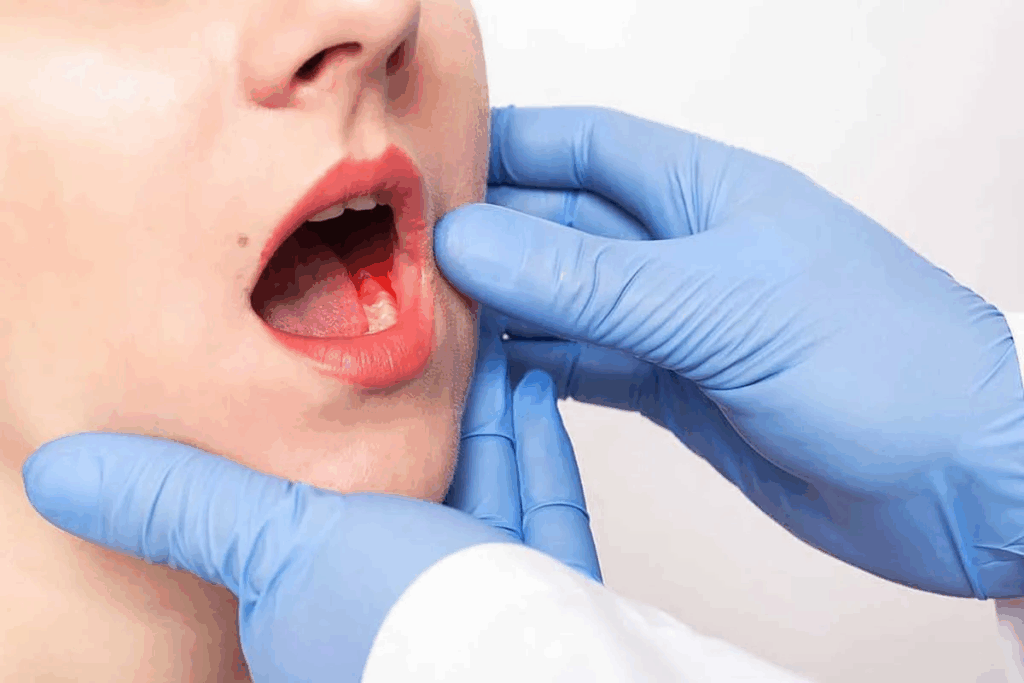
Understanding oral leukoplakia is key for diagnosis and treatment. It shows up as white or gray patches on the mouth’s lining. This includes the tongue, gums, and inner cheeks.
Medical Definition and Terminology
The word “leukoplakia” comes from Greek. “Leuko” means white, and “plakia” means patch. This matches its look. Studies say leukoplakia might lead to cancer, so it needs careful attention.
Doctors see leukoplakia as a white or gray patch that won’t come off. It’s a sign of higher cancer risk. They spot it by looking, but might need more tests to be sure.
Distinguishing Features from Other Oral Lesions
It’s important to tell leukoplakia apart from other mouth issues. Here’s how:
- Appearance: It looks like white or gray patches.
- Location: You often find it on the tongue, gums, and inner cheeks.
- Texture: The patches can feel smooth or rough.
- Persistence: Unlike other patches, leukoplakia can’t be rubbed off.
Knowing these signs helps doctors diagnose it right. A big study showed leukoplakia is common worldwide. It’s found in 0.33% to 11.74% of people. This shows we need to know about it and how to spot it.
The Clinical Appearance of Leukoplakia
It’s key to know how leukoplakia looks to spot it early. This condition shows up as white or gray patches in the mouth. These patches can look different from one person to another.
Visual Characteristics and Texture
Leukoplakia spots are usually painless at first. They can be white or gray and vary in size and shape. The texture can be smooth or rough, sometimes even cracked.
Things like tobacco use and irritation can change how leukoplakia looks. For example, smokers might see patches that are rougher.
Common Presentations and Variations
Leukoplakia can show up in different ways. Some spots are all white, while others have white and red parts or are irregular.
It’s more common in men than women, and in people over 60, smokers, and drinkers. Knowing these patterns helps doctors diagnose it right and figure out the risk.
Regular dental visits are important for catching leukoplakia early, mainly for those at high risk. Understanding its look helps doctors act fast to help patients.
Global Prevalence and Epidemiology
It’s key for healthcare pros to grasp the epidemiology of oral leukoplakia. This knowledge helps us see how common it is worldwide and where it’s more common. Oral leukoplakia is a big worry because it can turn into cancer.
Worldwide Statistics and Regional Differences
Oral leukoplakia is found in about 3.41% of people globally. But, the numbers change a lot in different places. This is because of things like smoking and chewing betel nut.
In some Asian countries, where betel nut is a big habit, oral leukoplakia is much more common. This shows why knowing about each area’s numbers is important.
Age, Gender, and Demographic Patterns
Men get oral leukoplakia more than women, and it gets more common with age. People over 60 see a big jump in cases.
Who gets it also matters. Some groups, like those who smoke or drink a lot, face a higher risk.
Key demographic factors include:
- Age: Increased prevalence in individuals over 60 years
- Gender: Higher prevalence in males
- Ethnicity: Variations among different ethnic groups
- Risk factors: Tobacco use, alcohol consumption, betel nut chewing
The chance of oral leukoplakia turning into cancer varies a lot. It can range from 0.1% to 17.5% worldwide. Knowing these numbers helps us find better ways to prevent and treat it.
Major Risk Factors for Oral Leukoplakia
Knowing the risk factors for oral leukoplakia is key to preventing it. Several factors can lead to this condition. By identifying them, we can manage and possibly prevent oral leukoplakia.
Tobacco Use and Its Mechanisms
Tobacco use is a big risk for oral leukoplakia. The mouth’s mucous membrane gets irritated and cells grow too much from tobacco’s harmful chemicals. Research shows tobacco users face a higher risk than non-users.
Key ways tobacco use leads to oral leukoplakia include:
- Chemical irritation from tobacco products
- Genetic changes in oral mucosal cells
- Weak immune response
Alcohol Consumption Patterns
Alcohol is also a major risk for oral leukoplakia. How often and how much alcohol is drunk can raise the risk. Alcohol irritates the mucosa and makes it more open to harmful substances, increasing leukoplakia risk.
“Alcohol consumption has been consistently associated with an increased risk of oral leukoplakia, particular when combined with tobacco use.”
Chronic Irritation and Other Contributing Factors
Chronic irritation, whether from mechanical, chemical, or thermal sources, can lead to oral leukoplakia. Issues like candidiasis and vitamin deficiencies also play a part. Good oral hygiene and addressing these can lower the risk.
Other factors include:
- Candidiasis or other infections
- Vitamin deficiencies, like vitamin A and B
- Mechanical irritation from dental appliances or rough teeth
Understanding these risk factors helps us manage and prevent oral leukoplakia. It’s vital to take preventive steps and get regular dental check-ups to keep an eye on oral health.
Classification Systems for Leukoplakia Lesions
Understanding leukoplakia types is key to managing this condition. Knowing the type helps doctors assess the risk of cancer and choose the right treatment.
Homogeneous vs. Non-homogeneous Types
Leukoplakia is divided into two main types: homogeneous and non-homogeneous. Homogeneous leukoplakia looks like uniform white patches. These are usually flat and thin, and are less likely to turn cancerous.
Non-homogeneous leukoplakia has a mixed look, with white and red spots, or thick and nodular surfaces. This type is more likely to develop into cancer.
Specialized Forms and Their Significance
Some leukoplakia types need extra attention. For example, proliferative verrucous leukoplakia (PVL) is rare but aggressive. It looks like a wart and can easily turn into cancer. PVL is hard to treat and must be closely watched.
“The classification of leukoplakia into different types is not just a matter of academic interest; it has significant implications for patient management and prognosis.” – Medical Expert, Oral Pathologist
Speckled leukoplakia has white patches with red spots. This type also has a higher risk of turning into cancer.
It’s important for doctors to know these types. It helps them give the best care. And it helps patients understand their risks and how to manage them.
Anatomical Distribution and High-Risk Locations
The place where oral leukoplakia lesions appear is key to knowing the risk of turning cancerous. Some spots in the mouth are more likely to become cancer than others.
Floor of the Mouth and Tongue Involvement
Lesions on the floor of the mouth and the ventral surface of the tongue are at high risk. This is because they can easily turn into cancer. The floor of the mouth is thin and has lots of blood vessels, making it a perfect place for cancer to spread.
The tongue, mainly its back and sides, is also a high-risk area. Lesions here can grow fast and have a higher chance of becoming oral cancer.
Retromolar Areas and Other Critical Sites
Other risky spots include the retromolar trigone and the soft palate. The retromolar trigone is often under a lot of stress, making it more likely for leukoplakia to turn into cancer.
Location | Risk Level | Reason |
Floor of the Mouth | High | Thin mucosa, rich vascular supply |
Tongue (Posterior and Lateral) | High | Aggressive nature, high risk of oral cancer |
Retromolar Trigone | High | High mucosal stress |
Soft Palate | Moderate | Less common but can get leukoplakia |
Knowing these high-risk spots is vital for catching oral leukoplakia early. Regular checks and quick action can greatly help patients.
Malignant Transformation: Understanding the Danger
Oral leukoplakia can turn into cancer, which is why knowing the risks is key. Both patients and doctors need to be aware of this danger.
Global Conversion Rates and Statistics
The chance of oral leukoplakia turning into cancer varies. Studies show rates from 0.1% to 17.5%. The yearly change rates are between 0.3% and 6.9%.
This big range comes from different study groups, follow-up times, and how they diagnose.
To grasp the global rates better, let’s look at some important numbers:
Region | Conversion Rate (%) | Annual Transformation Rate (%) |
Asia | 0.5-12.0 | 0.5-4.0 |
Europe | 0.1-17.5 | 0.3-6.9 |
North America | 1.0-10.0 | 0.5-3.0 |
Predictive Factors for Cancerous Changes
Knowing what can lead to cancer in oral leukoplakia is vital. This helps in early treatment and better management. Key factors include:
- Lesion characteristics: Non-homogeneous, large, and dysplastic lesions are at higher risk.
- Location: Lesions on the floor of the mouth, tongue, and retromolar areas are more dangerous.
- Patient habits: Using tobacco and alcohol greatly increases the risk.
Understanding these factors helps doctors plan better care and surveillance.
By knowing the risks and factors for cancer, we can improve care for oral leukoplakia patients.
Diagnostic Approaches and Procedures
To diagnose oral leukoplakia, we use a detailed method. This includes a clinical exam, looking at the patient’s history, and sometimes a biopsy. We will look at the different ways to identify and treat oral leukoplakia.
Clinical Examination Techniques
First, we do a thorough clinical exam. We look and feel the lesion to see its size, texture, and where it is. This helps us spot signs of dysplasia or early cancer.
- Visual inspection to assess the lesion’s appearance and color
- Palpation to evaluate the texture and consistency of the lesion
- Examination of the surrounding tissues for any signs of abnormality
Biopsy Methods and Importance
A biopsy is key to confirm oral leukoplakia and check for dysplasia or cancer. We use different biopsy methods to get tissue samples for lab tests.
The biopsy’s role is huge. It gives a clear diagnosis and helps decide treatment.
Advanced Diagnostic Technologies
Along with exams and biopsies, we use new tech to help diagnose oral leukoplakia. These include:
- Toluidine blue staining to highlight areas of dysplasia or cancer
- Autofluorescence imaging to detect abnormal tissue fluorescence
- Molecular diagnostic tests to identify genetic alterations associated with oral leukoplakia
These tools help us spot risky lesions and keep an eye on patients better.
By using exams, biopsies, and new tech, we can accurately diagnose and treat oral leukoplakia. This improves patient results.
Histopathological Assessment and Staging
Getting a precise histopathological evaluation is key to figuring out how serious oral leukoplakia is. This step involves looking closely at tissue samples. It helps spot the tiny details and cell changes linked to the condition.
Microscopic Features and Cellular Changes
When checking oral leukoplakia, experts look for certain signs under the microscope. These include hyperkeratosis, acanthosis, and dysplasia. Finding these signs helps figure out how bad the lesion is and if it might turn cancerous.
- Hyperkeratosis: This is when the keratin layer gets thicker, often due to long-term irritation.
- Acanthosis: The epithelial layer gets thicker, which can be a reaction or a sign of dysplasia.
- Dysplasia: This means the cells are not maturing right and the tissue looks abnormal, showing a risk of turning cancerous.
Dysplasia Grading and Prognostic Implications
Grading dysplasia is a big part of the histopathological check-up. It tells us a lot about what the future might hold for oral leukoplakia. The grading system puts dysplasia into three levels: mild, moderate, and severe. Each level shows how bad the cell and tissue changes are.
- Mild Dysplasia: This has only a little cell and tissue change, with a low chance of turning cancerous.
- Moderate Dysplasia: There’s more cell and tissue change, showing a moderate risk of turning into cancer.
- Severe Dysplasia/Carcinoma in Situ: This has big cell and tissue changes, with a high risk of turning into cancer.
The grade of dysplasia is very important for planning treatment. It helps doctors decide how closely to watch the patient or if they need to take action. So, getting the histopathological assessment right is very important for good care and better patient results.
Treatment Strategies and Management Options
There are many ways to treat oral leukoplakia, from old methods to new ones. The right treatment depends on several things. These include the size, location, and cause of the patches, and the patient’s health and wishes.
Conservative Approaches and Monitoring
For many, the first step is to try conservative methods. This means regular monitoring to watch for changes in the lesions. It also includes lifestyle changes, like quitting tobacco and drinking less alcohol. These habits can help prevent and slow down oral leukoplakia.
Other conservative treatments might include medicines or supplements. Some research shows that antioxidants and retinoids could help manage oral leukoplakia.
Surgical Interventions and Techniques
When conservative methods don’t work or if the lesions show signs of dysplasia, surgery might be needed. The surgery can be simple or complex, like laser surgery or cryotherapy. The choice depends on the size and location of the leukoplakia and the patient’s health.
After surgery, it’s important to keep a close eye on the patient. This is to catch any signs of new lesions or if the old ones come back. Teaching patients about the importance of follow-up visits and self-exams is key.
Emerging Therapies and Clinical Trials
New treatments for oral leukoplakia are being developed all the time. These include new medicines, photodynamic therapy, and other innovative methods. They are being tested in clinical trials.
We suggest talking to your doctor about these new options. Joining clinical trials can give you access to treatments that are not yet widely available.
In summary, treating oral leukoplakia needs a mix of old and new methods. By using conservative treatments, surgery, and new therapies, we can give patients the best care possible.
Prevention and Risk Reduction Methods
To prevent oral leukoplakia, it’s important to tackle risk factors and adopt healthy habits. Knowing and reducing the main causes can lower the risk of getting oral leukoplakia.
Tobacco and Alcohol Cessation Programs
Tobacco and alcohol use are big risks for oral leukoplakia. Cessation programs are key to stop these habits. There are many resources, like counseling and medicine, to help quit.
Studies show quitting tobacco and drinking less alcohol can make leukoplakia lesions smaller. It also lowers the chance of these lesions turning cancerous.
Dietary Modifications and Nutritional Support
Eating right is also key in preventing oral leukoplakia. Eating more fruits, vegetables, and antioxidants can help. Nutritional support and healthy eating advice are great for those at high risk.
Dietary Component | Benefit |
Fruits and Vegetables | Rich in antioxidants, vitamins, and minerals that help protect against cellular damage. |
Antioxidants | Help in reducing oxidative stress and potentially lowering the risk of oral leukoplakia. |
Whole Grains | Provide fiber, vitamins, and minerals that contribute to overall health. |
Regular Dental Check-ups and Self-examination
Going to the dentist regularly is vital for catching oral leukoplakia early. Dentists can spot lesions and offer oral health tips. Also, self-examination helps people keep an eye on their mouth health between dentist visits.
Combining quitting tobacco and alcohol, eating better, and regular dental visits can greatly lower the risk of oral leukoplakia. These steps are essential for good oral health and preventing serious problems.
Conclusion: Living with and Managing Oral Leukoplakia
Living with oral leukoplakia means you need to manage it well. This includes regular checks, making lifestyle changes, and getting treatment when needed. It’s important to be proactive to lower the risks.
Managing oral leukoplakia well means using both medical help and taking care of yourself. Going to the dentist regularly and checking yourself is key. This helps catch any changes early.
Knowing the risks and taking steps to avoid them can help prevent oral leukoplakia. We suggest working with your doctor to create a plan that’s right for you.
Good management of oral leukoplakia can stop it from getting worse. We aim to give top-notch care and support to patients from around the world.
FAQ
What is oral leukoplakia?
Oral leukoplakia is a condition where white patches or lesions appear in the mouth. It often happens due to chronic irritation or other factors. It’s seen as a potentially malignant disorder, which means it can turn into cancer.
What does leukoplakia mean?
Leukoplakia is a condition with white patches or lesions on mucous membranes, often in the mouth. The term comes from Greek words “leuko,” meaning white, and “plakia,” meaning patch.
What are the risk factors for developing oral leukoplakia?
Major risk factors include tobacco use, alcohol consumption, and chronic irritation. Poor oral hygiene and certain infections can also play a role.
How is oral leukoplakia diagnosed?
It’s diagnosed through clinical examination, biopsy, and histopathological assessment. Advanced diagnostic technologies like toluidine blue staining may also be used.
What are the treatment options for oral leukoplakia?
Treatment options include conservative approaches like monitoring and lifestyle changes. Surgical interventions like laser surgery or excision are also available. Emerging therapies, including chemoprevention, are being explored.
Can oral leukoplakia be prevented?
Yes, it can be prevented or its risk reduced. Methods include tobacco and alcohol cessation programs, dietary modifications, and regular dental check-ups.
What is the risk of malignant transformation in oral leukoplakia?
Oral leukoplakia is a potentially malignant disorder. The risk of turning into cancer varies based on the lesion’s location and characteristics. Regular monitoring and follow-up are key to detect any changes.
How is the severity of oral leukoplakia assessed?
Severity is assessed through histopathological evaluation. This involves examining cellular changes and dysplasia grading. This information helps determine the prognosis and guides treatment.
What are the common locations for oral leukoplakia lesions?
Lesions can occur in various locations in the mouth, including the floor of the mouth, tongue, and retromolar areas. These are high-risk sites that need close monitoring.
References
National Center for Biotechnology Information. Oral Hairy Leukoplakia: EBV Reactivation and Treatment. Retrieved from https://pubmed.ncbi.nlm.nih.gov/27601641/


































