Bronchiolitis diagnosis at Liv Hospital combines clinical evaluation, oxygen monitoring, and expert pediatric assessment to ensure accurate and timely care.
Send us all your questions or requests, and our expert team will assist you.
Bronchiolitis Diagnosis and Evaluation
How Is Bronchiolitis Diagnosed?
Bronchiolitis diagnosis is mainly clinical, based on a child’s symptoms and physical exam.
There’s no single test; evaluation focuses on severity and ruling out other causes like pneumonia, foreign body, or early asthma.
Real Time Monitoring and Evaluation in Bronchiolitis at Liv Hospital
Because bronchiolitis can progress rapidly, the evaluation at Liv Hospital focuses on “real time” monitoring of the infant’s physiological stability.
This ensures that interventions are tailored to the child’s specific needs at that moment
Medical History and Physical Exam

The evaluation begins with a detailed history. The doctor will ask about the onset of cold symptoms, the child’s ability to feed, and whether there have been any pauses in breathing. During the physical exam, the clinician will check:
Pulse Oximetry (Oxygen Saturation)
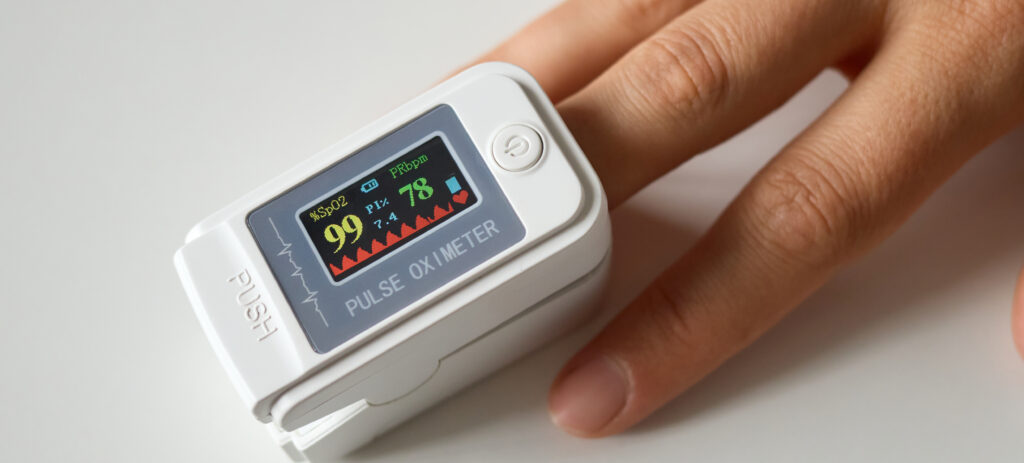
This is a vital, non-invasive test. A small sensor is placed on the infant’s foot or toe to measure the percentage of oxygen in the blood (SpO2).
Viral Testing (Nasopharyngeal Swab)
A doctor may use a soft swab to collect a sample of mucus from the back of the nose. This can be tested for RSV (Respiratory Syncytial Virus), influenza, or other common viruses.
While knowing the specific virus doesn’t usually change the treatment (since all are treated supportively), it helps in “cohorting” patients in the hospital to prevent the spread of the virus to others.
Chest X-ray

A chest X-ray is not routinely recommended for typical cases of bronchiolitis. However, a specialist may order one if:
Blood Tests
Routine blood work is rarely needed for bronchiolitis. However, in moderate to severe cases, a doctor might check:
Capillary Blood Gas (CBG)
In severe cases where a child is struggling significantly to breathe, a small prick on the heel can be used to check the levels of carbon dioxide and the pH of the blood.
This helps determine if the child’s lungs are effectively “venting” CO2 or if the infant is becoming too exhausted to continue breathing on their own.
Hydration Assessment
A key part of the evaluation is determining the child’s fluid status. The doctor will check:
Severity Scoring Systems
At Liv Hospital, we often use standardized scoring systems (like the Wang or RDAI score). These allow nurses and doctors to assign a number to the child’s distress based on respiratory rate, wheezing, and retractions.
This “common language” helps the team track whether a child is improving or needs more intensive care.
Differentiating Bronchiolitis from Asthma
Distinguishing the two can be tricky in older infants. While bronchiolitis is an infection, asthma is an allergic/inflammatory response.
Evaluating Risk for Complications
The evaluation includes identifying high-risk factors that make a child more likely to have a severe course:
How Does Liv Hospital Ensure Accurate and Timely Bronchiolitis Diagnosis?
At Liv Hospital, our pediatric team monitors infants closely, following the latest Level of Care protocols.
With 24/7 access to pediatric radiology and rapid viral testing, we provide fast, precise evaluation while focusing on the child’s overall well being.

Send us all your questions or requests, and our expert team will assist you.
Home oximeters are often inaccurate. Clinical diagnosis requires listening to the lungs and assessing breathing, which a device cannot do.
X-rays rarely change treatment and expose infants to radiation. They are used only if complications like pneumonia or a collapsed lung are suspected.
Symptoms usually worsen around days 3–5. Early diagnosis may require follow-up to ensure the child isn’t declining.
No. Most babies with RSV have mild symptoms; the test identifies the virus but doesn’t predict severity.
Not always. Wheezing can result from allergies, a swallowed object, or heart issues, making professional evaluation essential.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)