Pediatrics provides specialized medical care for infants, children, and adolescents. Learn about routine screenings, vaccinations, and treatments.
Send us all your questions or requests, and our expert team will assist you.
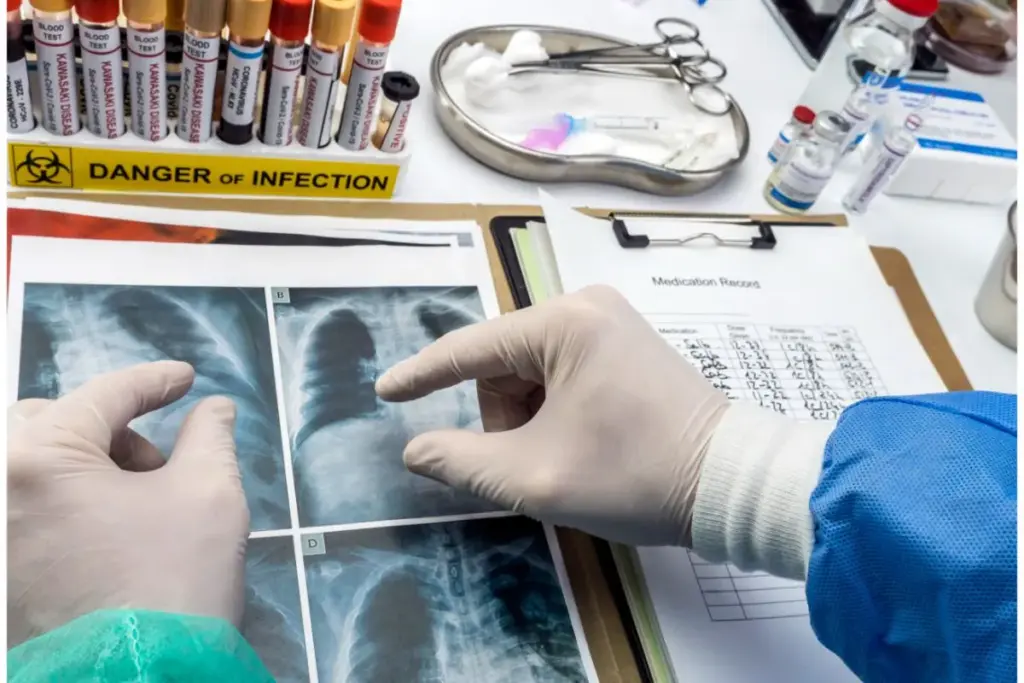
Diagnosing Kawasaki disease presents a unique challenge to clinicians because there is no single pathognomonic laboratory test or “gold standard” diagnostic tool. The diagnosis is primarily clinical, based on a specific set of criteria that identify the constellation of symptoms associated with vasculitis. The challenge is magnified in “incomplete” cases, where children do not manifest the full spectrum of classic symptoms yet face the same risk of coronary artery aneurysms. The evaluation process is designed to be rigorous and redundant, employing exclusionary criteria and the astute interpretation of supportive laboratory and imaging data. At Liv Hospital, this involves a multidisciplinary approach that integrates pediatricians, infectious disease specialists, and pediatric cardiologists to provide a comprehensive evaluation.

The classic diagnosis is based on the criteria developed by Dr. Tomisaku Kawasaki. A patient must exhibit a fever for at least five days (or fewer if treated) plus four of the five principal clinical features: extremity changes, polymorphous exanthem, bilateral non-exudative conjunctivitis, oral mucosal changes, and cervical lymphadenopathy. However, strict adherence to these criteria can result in missed diagnoses in atypical cases. Therefore, modern evaluation algorithms incorporate “incomplete” Kawasaki disease protocols. These protocols mandate that any infant with unexplained fever for seven days or more should undergo evaluation for Kawasaki disease, regardless of clinical signs. This lowers the threshold for testing and treatment, prioritizing cardiac safety over rigid diagnostic purity.
Supplemental Laboratory Criteria: In the absence of full clinical signs, markers like anemia, low albumin, and elevated liver enzymes serve as diagnostic proxies.

Echocardiography is the primary imaging modality for evaluating the cardiovascular impact of Kawasaki disease. It enables real-time visualization of the coronary arteries, myocardium, and valves. In the past, coronary arteries were classified simply as “normal” or “aneurysmal.” Today, the evaluation is much more precise, utilizing Z-scores. A Z-score standardizes the coronary artery diameter relative to the child’s body surface area. A Z-score of greater than 2.5 indicates dilation, while scores greater than 10 or absolute dimensions greater than 8mm indicate giant aneurysms. This quantitative approach detects subtle dilations that would be missed by visual inspection alone, thereby enabling earlier escalation of therapy. The echocardiogram also assesses for pericardial effusion and mitral regurgitation, which are indicators of active carditis.
Laboratory evaluation plays a critical supportive role. In the acute phase, acute-phase reactants such as C-Reactive Protein (CRP) and Erythrocyte Sedimentation Rate (ESR) are almost universally elevated. A CRP level greater than 3.0 mg/dL and an ESR greater than 40 mm/hr are standard cutoffs used in diagnostic algorithms. The Complete Blood Count (CBC) typically reveals leukocytosis (high white blood cell count) with a neutrophilic predominance and a “left shift,” indicating immature white cells responding to severe stress. Normocytic, normochromic anemia is common due to inflammation-suppressed bone marrow. Importantly, the platelet count is usually normal in the first week but rises dramatically in the second week (thrombocytosis), providing retrospective confirmation of the diagnosis and a risk factor for thrombosis.
Systemic inflammation in Kawasaki disease often affects the liver and kidneys, providing additional diagnostic clues. Mild to moderate elevations in serum transaminases (ALT and AST) and gamma-glutamyl transferase (GGT) are frequently observed. Hypoalbuminemia is a marker of increased vascular permeability (capillary leak) and is associated with more severe disease and a higher risk of IVIG resistance. Urinalysis is a critical part of the workup; sterile pyuria (white blood cells in the urine with no bacteria) is found in a significant percentage of patients. This is caused by sterile urethritis and helps distinguish Kawasaki disease from a bacterial urinary tract infection, which would present with bacteria and a positive culture.
A vital component of the evaluation is distinguishing Kawasaki disease from its “mimics.” Adenovirus infection can cause fever, conjunctivitis, and swollen lymph nodes, but usually presents with exudative conjunctivitis and upper respiratory symptoms. Scarlet fever presents with a rash and strawberry tongue, responds rapidly to penicillin, and has a positive strep test. Systemic Juvenile Idiopathic Arthritis (sJIA) can present with fever and rash, but typically has a distinct fever pattern and a more chronic course. Multi-System Inflammatory Syndrome in Children (MIS-C), associated with COVID-19, shares many features with Kawasaki disease but often affects older children and has more prominent gastrointestinal and cardiac dysfunction. Serological testing for COVID-19 antibodies and detailed history taking are now standard parts of the evaluation to differentiate these entities.
Part of the advanced evaluation involves predicting which patients are likely to be resistant to the standard IVIG therapy. Various scoring systems (such as the Kobayashi score) use baseline laboratory values, such as sodium levels, AST, CRP, platelet count, and neutrophil count, to stratify risk. Patients identified as high-risk for IVIG resistance may be evaluated for intensified initial therapy, such as the addition of corticosteroids to the primary IVIG infusion. This predictive evaluation is a key step in personalized medicine for Kawasaki disease, allowing clinicians to be proactive rather than reactive in managing the most vulnerable patients.

Send us all your questions or requests, and our expert team will assist you.
A Z-score is a number that compares the size of your child’s heart arteries to what is normal for a child of the same size. A higher number means the vessel is larger or dilated.
No single blood test is proof, but high levels of inflammation markers (CRP and ESR) combined with physical symptoms strongly support the diagnosis.
Doctors test for viruses to make sure the symptoms aren’t caused by a common infection like Adenovirus or Measles, which can look very similar to Kawasaki disease.
It means there are white blood cells in the urine (indicating inflammation) but no bacteria (no infection). This is a helpful clue pointing towards Kawasaki disease.
Typically, an echocardiogram is done at diagnosis, then again at 2 weeks, and at 6-8 weeks. If everything is normal, checks may stop; otherwise, they continue long-term.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)