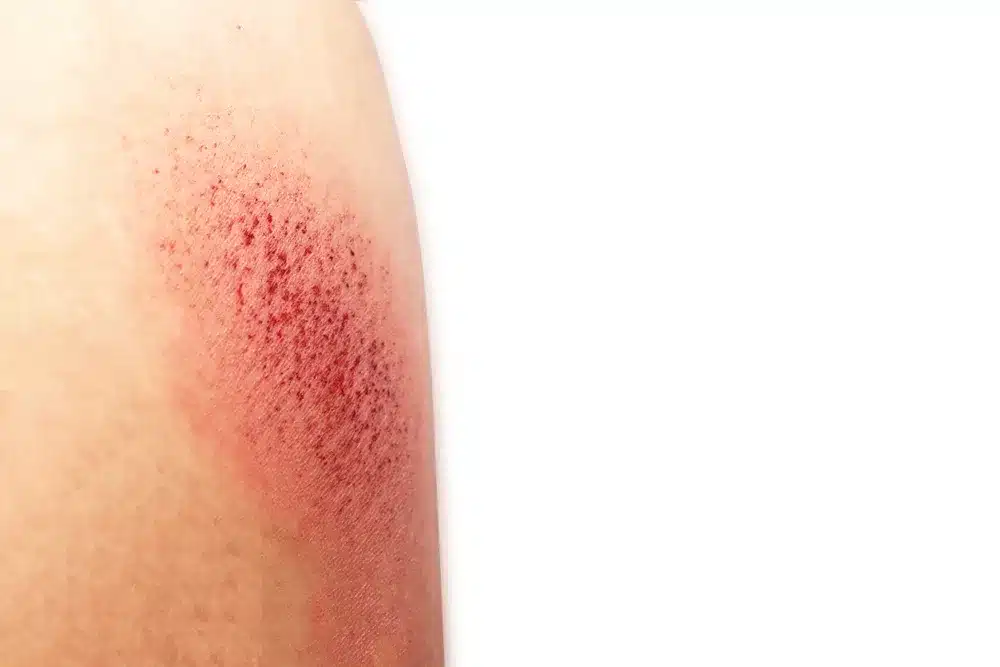
Red spots on the skin are called petechiae or purpura. They can show that you have a blood disorder. These spots can mean you have conditions like thrombocytopenia, immune thrombocytopenic purpura (ITP), leukemia, or hemophilia.
At Liv Hospital, we know how important it is to find and treat problems quickly. We use a team approach to care for our patients. Knowing what these spots mean is key to helping them get better.
Key Takeaways
- Blood disorders such as thrombocytopenia and leukemia can cause red spots on the skin.
- Purpura and petechiae are terms used to describe these red or purplish skin spots.
- Low platelet counts or defects in clotting mechanisms are often the underlying cause.
- A timely diagnosis is essential for effective treatment.
- Liv Hospital employs a multidisciplinary approach to diagnose and treat these conditions.
Understanding Red Spots on Skin: Types and Characteristics
Red spots on the skin can be different types. Each type looks and feels unique. Understanding these differences assists physicians in accurately diagnosing issues and determining appropriate treatment.
Petechiae: Tiny Red or Purple Spots
Petechiae are tiny, pinpoint spots that are often red or purple. They happen when small capillaries bleed. For more info on blood disorders, check out on blood.
“The presence of petechiae can be a sign of an underlying condition that requires medical attention.”
— Medical Expert
Purpura: Larger Red or Purple Patches
Purpura are larger red or purple patches on the skin. They can mean there’s a bigger bleeding problem. Purpura can come from many conditions, like blood clotting issues.
Ecchymoses: Bruise-like Discolorations
Ecchymoses are bruise-like spots that happen when blood bleeds into the skin or mucous membranes. They’re bigger than petechiae and purpura. They can be from trauma or bleeding disorders.
The Role of Blood Components in Skin Manifestations
The health of blood components, like platelets and blood vessels, is key to avoiding skin problems linked to bleeding disorders. We’ll look into how these parts help prevent conditions like petechiae and purpura.
Platelets and Blood Clotting
Platelets are tiny, colorless bits in our blood that help form clots to stop bleeding. A normal platelet count is between 150,000 and 450,000 per microliter of blood. If the platelet count drops, it can cause petechiae and other bleeding signs. Elrombopag is a drug that helps by boosting platelet production in the bone marrow.
Blood clotting is a complex process involving platelets, clotting factors, and blood vessels. Knowing how it works is important for diagnosing and treating bleeding disorders that show up on the skin, like petechiae.
Blood Vessels and Their Function
Blood vessels, including capillaries, arterioles, and venules, are vital for skin health. They help keep blood flowing smoothly and prevent leaks or ruptures, which can cause petechiae and purpura. Problems with blood vessel health, like vasculitis or fragility, can also lead to these skin issues.
Understanding blood vessels helps us figure out why petechiae and other bleeding disorders happen. It also guides how to treat them, possibly by fixing the vascular issue.
Petechiae: Clinical Significance and Evaluation
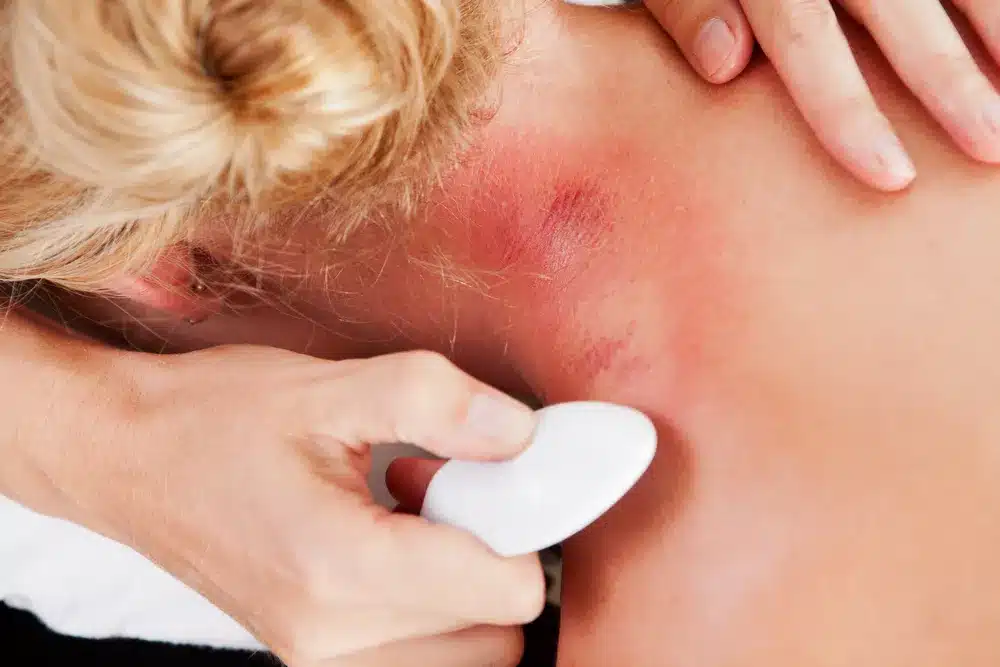
Petechiae are small red or purple spots on the skin. They can be a sign of many health issues, from minor to severe. These spots come from bleeding in small blood vessels and can show up anywhere on the body. It’s important to understand what petechiae mean and how to check them to know what to do next.
Common Causes of Petechiae
Petechiae can be caused by many things, like infections, autoimmune disorders, and bleeding problems. In kids, viral infections often cause petechiae in children. For adults, serious conditions like leukemia or severe infections might be the reason. Also, some medicines and vitamin shortages can lead to petechiae.
Distinguishing Benign from Serious Causes
Telling if petechiae are just minor or serious is key. Minor causes might be a viral infection or strain from coughing or vomiting. But, petechiae can also mean serious issues like meningitis or leukemia. A full medical history and physical check-up are needed to figure out the cause and when to worry about petechiae.
Diagnostic Approach to Unexplained Petechiae
If petechiae show up without a clear reason, a careful petechiae diagnosis is needed. This includes a detailed medical history, physical exam, and lab tests like blood counts and coagulation studies. Sometimes, a bone marrow biopsy might be needed to find the cause of petechiae in adults or kids.
As doctors, we must carefully check petechiae. We need to think about all possible causes and act quickly and correctly.
Thrombocytopenia: A Primary Cause of Red Spots

Thrombocytopenia is when you have too few platelets in your blood. This can cause red spots on your skin. It happens for many reasons, like problems with your bone marrow or an immune system issue.
Definition and Classification
Having less than 150,000 platelets per microliter of blood is thrombocytopenia. It’s split into types based on why it happens. For example, if your bone marrow isn’t working right, or if your immune system is attacking your platelets.
Knowing the type helps doctors figure out how to treat it. For instance, if your bone marrow isn’t making enough platelets, that’s one thing. But if your immune system is destroying them, that’s another.
Mechanisms of Low Platelet Count
There are many reasons why you might have low platelets. Here are a few:
- Decreased Production: This can happen if your bone marrow is failing or if it’s filled with disease, like leukemia.
- Increased Destruction: In immune thrombocytopenia (ITP), your body’s immune system attacks and destroys platelets.
- Sequestration: If your spleen is too active, it can hold onto platelets, making them hard to find in your blood.
Incidence and Epidemiology
Thrombocytopenia can affect anyone, at any age. The patterns of who gets it vary based on the cause. For example, ITP can hit both kids and adults, while chemotherapy-related thrombocytopenia is more common in cancer patients.
|
Cause |
Incidence |
Common Population |
|---|---|---|
|
Immune Thrombocytopenia (ITP) |
1-2 per 100,000 adults/year |
Adults and children |
|
Chemotherapy-induced |
Variable, depending on regimen |
Cancer patients |
|
Hypersplenism |
Dependent on underlying cause |
Patients with liver disease or splenic disorders |
Treating thrombocytopenia depends on why you have it and how bad it is. Doctors might use drugs like eltrombopag to help your body make more platelets. They also try to fix the underlying problem.
We’ll look closer at how eltrombopag and other treatments help manage thrombocytopenia.
Immune Thrombocytopenic Purpura (ITP)
ITP is an autoimmune disease where the body attacks its own platelets. This leads to low platelet counts, causing bleeding and bruising.
Pathophysiology and Autoimmune Mechanisms
ITP happens when the immune system makes antibodies against platelets. This marks them for destruction. It’s a complex process involving many immune cells and cytokines.
The spleen is key in this process. It’s where platelets are destroyed. Autoantibodies make platelets easier for splenic macrophages to remove.
Clinical Presentation and Diagnosis
People with ITP often have symptoms like petechiae, purpura, and ecchymoses. These are due to low platelet counts. The severity can vary.
To diagnose ITP, doctors use clinical evaluation, lab tests, and sometimes bone marrow exams. These help rule out other causes of low platelets.
Treatment Options and Management
Treatment for ITP depends on how severe it is. Corticosteroids are often used first to reduce platelet destruction.
If initial treatments don’t work, other options are considered. These include immunosuppressive therapy, thrombopoietin receptor agonists, and splenectomy. The choice depends on the patient’s health and ITP severity.
Managing ITP also means watching platelet counts. Treatments are adjusted as needed to prevent bleeding and manage side effects.
Leukemia and Red Spots: Understanding the Connection
It’s important to know how leukemia and skin spots like petechiae and purpura are linked. Leukemia, a blood cancer, affects the body’s blood cell production. This can cause various skin symptoms.
Types of Leukemia
There are many types of leukemia, but some are more likely to cause skin symptoms. These include:
- Acute Lymphoblastic Leukemia (ALL)
- Acute Myeloid Leukemia (AML)
- Chronic Lymphocytic Leukemia (CLL)
- Chronic Myeloid Leukemia (CML)
AML and ALL are often linked with skin symptoms because they progress quickly and affect blood cell production.
Mechanisms Behind Petechiae
Petechiae in leukemia happen because of the disease’s impact on platelets. Leukemia can cause thrombocytopenia, a low platelet count. This makes it hard for blood to clot, leading to petechiae, small, red or purple spots on the skin.
Prevalence and Prognosis
The frequency of skin symptoms like petechiae and purpura in leukemia patients varies. For example, a study found many AML patients had skin symptoms. These symptoms can also show if the disease is getting worse or coming back.
|
Type of Leukemia |
Common Skin Manifestations |
Prevalence |
|---|---|---|
|
Acute Myeloid Leukemia (AML) |
Petechiae, Purpura |
High |
|
Acute Lymphoblastic Leukemia (ALL) |
Petechiae, Ecchymoses |
Moderate to High |
|
Chronic Lymphocytic Leukemia (CLL) |
Purpura, Skin Infections |
Low to Moderate |
|
Chronic Myeloid Leukemia (CML) |
Petechiae, Purpura |
Low |
For more on petechiae as a leukemia symptom, check out.
In summary, knowing the link between leukemia and skin spots is key for early detection and treatment. By understanding which leukemia types cause skin symptoms and why, doctors can provide better care.
Hemophilia and Other Clotting Disorders
Hemophilia is a genetic disorder that makes it hard for the body to form blood clots. This is important because blood clots help stop bleeding. We will look at the different types of hemophilia, their signs, and how to manage them.
Types and Characteristics
Hemophilia is mainly split into two types: Hemophilia A and Hemophilia B. Hemophilia A is caused by a lack of factor VIII, while Hemophilia B is due to a lack of factor IX. The severity of hemophilia depends on how much clotting factor is in the blood.
- Mild Hemophilia: Patients have 5-40% of normal clotting factor levels. Bleeding usually happens after trauma or surgery.
- Moderate Hemophilia: This has 1-5% of normal clotting factor levels. Bleeding can happen after minor injuries.
- Severe Hemophilia: Less than 1% of normal clotting factor levels. Patients often have spontaneous bleeding into joints and muscles.
Skin Manifestations and Bleeding Patterns
Skin signs in hemophilia include bruising and bleeding into the skin, known as ecchymoses and purpura. The pattern and severity of bleeding can vary a lot among people with hemophilia.
|
Type of Hemophilia |
Clotting Factor Deficiency |
Common Bleeding Sites |
|---|---|---|
|
Hemophilia A |
Factor VIII |
Joints, muscles, and skin |
|
Hemophilia B |
Factor IX |
Joints, muscles, and skin |
Management and Preventive Strategies
Managing hemophilia involves replacing the missing clotting factor through replacement therapy. This can be done when needed to treat bleeding or regularly to prevent it.
- Prophylactic Treatment: Regular infusion of clotting factor concentrates to keep levels up and prevent bleeding.
- On-Demand Treatment: Infusion of clotting factor concentrates at the time of bleeding to stop it.
- Gene Therapy: A new approach that aims to fix the genetic defect causing hemophilia.
Understanding hemophilia’s types, characteristics, and management options helps us better support those affected by it.
Henoch-Schönlein Purpura: A Focus on Children
Henoch-Schönlein purpura (HSP) mainly affects kids, causing symptoms like purpura and joint pain. It’s a type of vasculitis that inflames blood vessels. This can lead to many different symptoms.
Pathogenesis and Immunological Factors
The exact cause of HSP is not fully understood. It’s thought to start with an abnormal immune response, often from a cold. Immunoglobulin A (IgA) is key, as it’s found in the blood vessels. This leads to inflammation and damage.
Many factors contribute to HSP, including genetics, environment, and immune system issues. These all work together in complex ways.
Clinical Features and Systemic Involvement
HSP is known for a set of symptoms: purpura, arthritis, abdominal pain, and renal involvement. The purpura, seen on legs and buttocks, is the main sign. It often leads parents to seek help.
Systemic involvement can vary. Some kids have mild symptoms, while others face serious issues like kidney problems. Joint pain and swelling are common, affecting knees and ankles. Abdominal pain can be severe and may come before purpura, leading to wrong diagnoses.
Treatment Approaches and Outcomes
Managing HSP focuses on relieving symptoms and watching for complications. Rest and hydration are key, along with pain relief medicines. In severe cases, stronger treatments like corticosteroids may be needed.
For serious kidney or stomach problems, more aggressive treatment is used. Regular check-ups are vital to catch any long-term issues, like kidney disease.
Most kids with HSP get better, but some may have ongoing problems or kidney issues. Knowing the prognosis helps manage expectations and guide treatment.
Other Blood Disorders Causing Red Spots
<SEP-16279_image_4>
Several blood disorders can cause red spots on the skin. These include DIC and Von Willebrand disease. They affect blood clotting.
Disseminated Intravascular Coagulation (DIC)
DIC is a serious condition. It causes blood clots in small blood vessels all over the body. This uses up platelets and clotting factors, leading to bleeding and red spots.
Key aspects of DIC include:
- Complex pathophysiology involving both clotting and bleeding
- Association with severe underlying conditions such as sepsis or malignancy
- Clinical presentation that can range from mild to severe
Von Willebrand Disease
Von Willebrand disease is the most common inherited bleeding disorder. It’s caused by a lack or problem with von Willebrand factor (VWF). VWF is key for platelet adhesion and blood clotting.
Characteristics of Von Willebrand disease include:
- Mucocutaneous bleeding symptoms
- Variable severity depending on the type and level of VWF deficiency
- Potential for significant bleeding after trauma or surgery
Vitamin K Deficiency and Coagulation Disorders
Vitamin K is vital for clotting factor production in the liver. A lack of vitamin K can cause coagulopathy. This leads to an increased tendency to bleed, showing as red spots on the skin.
Causes and consequences of vitamin K deficiency include:
- Nutritional deficiencies or malabsorption
- Use of certain medications such as anticoagulants
- Increased risk of bleeding complications
In conclusion, DIC, Von Willebrand disease, and vitamin K deficiency are significant blood disorders. They can cause red spots on the skin. Understanding these conditions is key for proper diagnosis and management.
Diagnostic Approach to Blood Disorders with Skin Manifestations
Diagnosing blood disorders with skin symptoms is complex. It involves both clinical evaluation and lab tests. We use a detailed approach to find the right diagnosis, considering all important factors.
Initial Assessment and Clinical Evaluation
The first step is key in finding the cause of skin symptoms. We start by taking a detailed medical history. This includes when the symptoms started, how long they last, and what they look like.
Then, we do a physical exam to see how bad the skin lesions are. We look for signs of blood disorders like petechiae, purpura, or ecchymoses. We also check other parts of the body, as some blood disorders can affect more than just the skin.
Laboratory Testing and Interpretation
Lab tests are essential in diagnosing these conditions. We often use:
- Complete Blood Count (CBC) to check platelet, white blood cell, and red blood cell counts.
- Blood smear to look at blood cell shapes.
- Coagulation studies to check for bleeding and clotting problems.
- Bone marrow biopsy to diagnose bone marrow issues.
Understanding these tests is important. The results must match the symptoms to make a correct diagnosis.
|
Laboratory Test |
Purpose |
Relevance to Blood Disorders |
|---|---|---|
|
Complete Blood Count (CBC) |
Assess platelet count, white blood cell count, and red blood cell count. |
Helps diagnose thrombocytopenia, leukemia, and other blood cell disorders. |
|
Blood Smear |
Examine the morphology of blood cells. |
Aids in identifying abnormal cell morphology indicative of specific blood disorders. |
|
Coagulation Studies |
Evaluate bleeding and clotting disorders. |
Essential for diagnosing hemophilia, von Willebrand disease, and other clotting disorders. |
Imaging and Other Diagnostic Modalities
We also use imaging and other tests to help diagnose. For example, ultrasound or CT scans can show internal bleeding or organ problems.
Skin biopsies can also be used. They help us understand the skin lesions better.
By combining clinical evaluation, lab tests, and imaging, we can accurately diagnose and treat blood disorders with skin symptoms. This way, we provide our patients with the best care possible.
Multidisciplinary Treatment Strategies
<SEP-16279_image_5>
Treating blood disorders with skin symptoms needs teamwork from different doctors. A good plan combines hematological interventions, dermatological management, and integrated care strategies.
Hematological Interventions
Hematologists play a key role in treating the blood issues that lead to red spots. They might use:
- Medicines for problems like low platelets or leukemia.
- Blood transfusions to replace missing cells.
- Chemotherapy or other treatments for the root cause.
Our hematologists team up with others to make a treatment plan that fits each patient. This shows how integrated care is key to the best results.
Dermatological Management
Dermatologists focus on the skin problems linked to blood disorders. They might use:
- Topical treatments to reduce inflammation or help healing.
- Steps to protect the skin from injury.
- Watching for changes in skin symptoms that might mean a treatment change is needed.
By mixing dermatological management with hematological treatments, we offer a full care plan for red spots from blood disorders.
Integrated Care Approaches
Integrated care approaches are vital for complex conditions like blood disorders with skin symptoms. This means:
- Working together between hematologists, dermatologists, and other healthcare teams.
- Creating treatment plans that cover the patient’s whole health and specific needs.
- Teaching and supporting patients and their families to manage the condition well.
Using an integrated care method helps improve patient results and their life quality.
When to Seek Medical Attention for Red Spots
<SEP-16279_image_6>
Knowing when to see a doctor for red spots is key. These spots can be from simple issues or serious health problems. It’s important to watch for signs that mean you need to get help right away.
Warning Signs Requiring Immediate Care
Some red spots need quick medical help. Look out for these signs:
- Rapid spread: If the red spots are growing fast on your skin.
- Severe symptoms: Feeling feverish, having joint pain, or other big symptoms with the red spots.
- Changes in appearance: If the spots change color, size, or shape over time.
Follow-up Care and Monitoring
After seeing a doctor, you’ll need to keep an eye on things. This means:
- Regular check-ups with your doctor to watch the spots and your health.
- Laboratory tests to find out what might be causing the red spots.
Conclusion
Red spots on the skin can show many underlying blood disorders. These include conditions that cause petechiae and purpura. It’s important to understand these conditions, how to diagnose them, and the treatment options.
At Liv Hospital, we aim to give top-notch healthcare. We use a team approach to ensure the best results for our patients. Our experts work together to handle blood disorders, giving each patient personalized care and support.
Knowing the causes of red spots on the skin is key. It helps patients get the right treatment quickly. This improves their life quality. We work hard to give the best care to those with blood disorders, including petechiae and purpura. We make sure they get the support they need.
FAQ
What are petechiae and purpura?
Petechiae are small, pinpoint spots on the skin that are often red or purple. Purpura refers to larger patches. Both are signs of blood disorders.
What causes red spots on the skin?
Red spots can come from many blood disorders. These include thrombocytopenia, immune thrombocytopenic purpura (ITP), leukemia, hemophilia, and Henoch-Schönlein purpura (HSP).
What is thrombocytopenia?
Thrombocytopenia is when you have too few platelets. This can cause bleeding and skin issues like petechiae and purpura.
How is thrombocytopenia treated?
To treat thrombocytopenia, doctors might use medications like eltrombopag. These help manage low platelet counts.
What is immune thrombocytopenic purpura (ITP)?
ITP is when your immune system attacks platelets. This leads to low platelet counts, or thrombocytopenia.
How is ITP diagnosed and treated?
Doctors diagnose ITP through tests and exams. Treatment includes medicines to stop the immune system from attacking platelets.
Can leukemia cause red spots on the skin?
Yes, leukemia can cause skin symptoms like petechiae and purpura.
What is hemophilia?
Hemophilia is a bleeding disorder. It makes it hard for blood to clot, leading to long bleeding.
How is hemophilia managed?
Managing hemophilia includes replacement therapy and taking steps to prevent bleeding.
What is Henoch-Schönlein purpura (HSP)?
HSP is a type of vasculitis that mainly affects kids. It causes purpura, joint pain, and stomach problems.
When should I seek medical attention for red spots on the skin?
See a doctor right away if you have severe bleeding, trouble breathing, or other serious symptoms.
What diagnostic approaches are used to evaluate blood disorders with skin manifestations?
Doctors use tests, exams, and imaging to diagnose blood disorders with skin symptoms.
How are blood disorders with skin manifestations treated?
Treatment involves a team effort. It includes medicines, skin care, and overall care plans.
What is the role of platelets in blood clotting?
Platelets are key for blood clotting. Without enough or functioning platelets, bleeding disorders can occur.
What is disseminated intravascular coagulation (DIC)?
DIC is when blood clots form in small blood vessels all over the body. It can cause bleeding problems.
What is von Willebrand disease?
Von Willebrand disease is a bleeding disorder. It’s caused by a lack or problem with von Willebrand factor, a clotting protein.
How does vitamin K deficiency affect coagulation?
Vitamin K deficiency can cause coagulation problems. Vitamin K is needed for making clotting factors.
References
Fred Hutch Cancer Center: https://www.fredhutch.org/en/diseases/blood-disorders/facts-resources.html





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























