
Waking up from a coma can change your life. Knowing the stages of recovery is key for patients and their families. At Liv Hospital, we offer advanced care that truly helps those waking up from a coma.
The road to recovery varies greatly. It depends on the coma’s depth and length, your health, age, and why you were in a coma. We know every person’s recovery is different. Our team is here to offer personalized support and care.
Key Takeaways
- Post coma recovery is a highly individualized process.
- The depth and duration of the coma influence the recovery process.
- Underlying medical conditions and age play a significant role in recovery.
- Understanding the stages of recovery is key for patients and families.
- Liv Hospital provides advanced, patient-focused care for coma recovery.
Understanding Coma: The Starting Point of Recovery
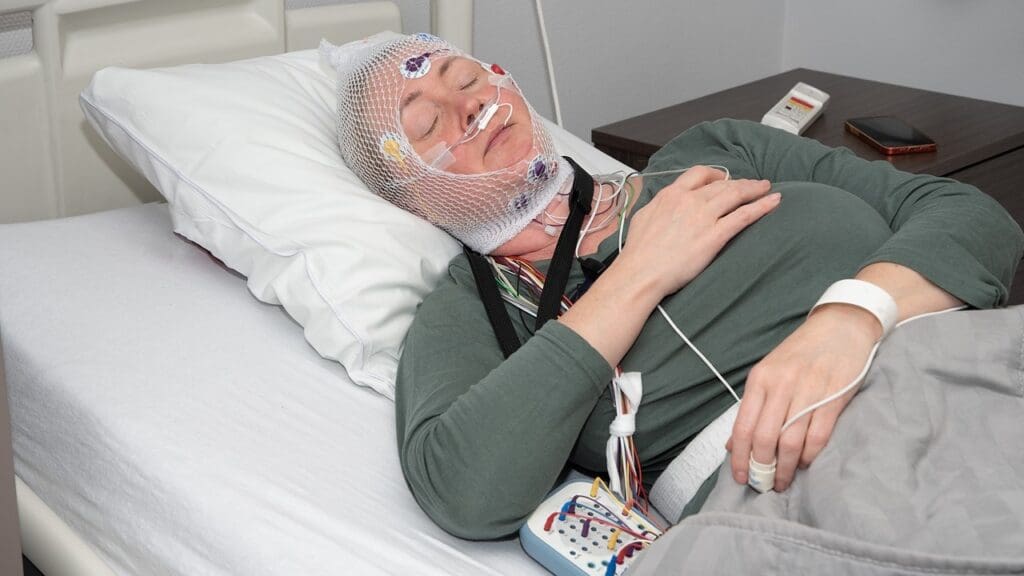
To start the recovery journey, it’s key to grasp what a coma is. A coma is a deep sleep-like state where a person can’t respond to their surroundings. This state can last for a long time.
What Defines a Coma
A coma means someone can’t wake up or react to anything. It’s not the same as being brain dead. People in a coma are alive but can’t respond to anything around them.
Common Causes of Coma
Comas can happen for many reasons. These include head injuries, strokes, infections, and metabolic issues. Knowing why someone is in a coma helps doctors figure out the best treatment.
| Cause | Description |
|---|---|
| Traumatic Brain Injury | Head injury leading to brain damage |
| Stroke | Interruption of blood supply to the brain |
| Infections | Bacterial or viral infections affecting the brain |
| Metabolic Disorders | Conditions like diabetes or liver disease affecting brain function |
Medical Assessment of Coma Depth
Doctors use scales like the Glasgow Coma Scale (GCS) to check coma depth. The GCS looks at eye opening, talking ability, and movement to see how awake someone is.
Knowing how deep and why someone is in a coma is important. It helps doctors create a good treatment plan and support the recovery process.
Factors That Influence Post Coma Recovery
Many factors affect how well someone recovers after a coma. Knowing these can help patients and their families understand the recovery journey.
Duration and Depth of Coma
The time spent in a coma and its depth are key to recovery. Shorter comas usually mean better chances of recovery.
Age and Overall Health
A person’s age and health before the coma matter a lot. Younger, healthier people often recover better.
Underlying Cause of Coma
The reason for the coma also plays a big role. Causes like trauma or infection can affect recovery differently.
Quality of Medical Care
The care received during and after the coma is very important. Good medical care can greatly improve recovery chances.
Here’s a table showing how these factors impact recovery:
| Factor | Influence on Recovery | Example |
|---|---|---|
| Duration of Coma | Shorter comas generally have better outcomes | A patient in a coma for 1 week may have a better prognosis than one in a coma for 1 month |
| Age | Younger patients tend to recover better | A 30-year-old patient may have a better recovery than an 80-year-old |
| Underlying Cause | Traumatic causes may have different outcomes than medical causes | A coma due to head trauma may have a different prognosis than one caused by infection |
| Quality of Care | High-quality care improves outcomes | Access to specialized rehabilitation services can enhance recovery |
Understanding these factors helps healthcare teams and families support patients better. They can tailor care to meet each person’s needs.
Typical Recovery Timelines After Coma
Recovering from a coma is different for everyone. Yet, most people follow similar timelines. Knowing these can help patients and their families better understand the recovery journey.
Initial Consciousness (2-4 Weeks)
The first step is waking up, which usually happens in two to four weeks. Patients might start to show they’re awake by opening their eyes or responding to voices.
Early Recovery Phase (1-3 Months)
Once patients wake up, they start to get back some of their lost abilities. This stage can last from one to three months. It’s when they start to improve their thinking and moving skills.
Extended Recovery Period (6-12+ Months)
The next stage is the extended recovery, lasting six months to over a year. Here, patients keep getting better, becoming more independent and functional.
| Recovery Phase | Timeline | Characteristics |
|---|---|---|
| Initial Consciousness | 2-4 Weeks | Regaining wakefulness, responding to commands |
| Early Recovery | 1-3 Months | Improving cognitive and motor skills |
| Extended Recovery | 6-12+ Months | Regaining independence, continued progress |
Every coma recovery is unique, and timelines can vary a lot. But knowing these general guidelines can help manage hopes and provide support during the recovery.
The 8 Stages of Post Coma Recovery: An Overview
Recovering from a coma is a complex journey with many stages. Each stage has its own unique traits. The path through these stages can differ greatly from person to person. This depends on the brain injury’s severity and the patient’s health.
The Rancho Los Amigos Scale
The Rancho Los Amigos Scale is a key tool for tracking brain injury recovery. It was created by the Rancho Los Amigos National Rehabilitation Center. This scale breaks down recovery into eight stages, helping to understand a patient’s progress.
Progression Through Recovery Stages
As patients move through the eight stages, their awareness, responsiveness, and thinking skills improve. Early stages show little response, while later stages see big gains in thinking and moving skills.
Knowing these stages is key for setting realistic hopes and giving the right care. Healthcare teams can adjust their plans based on the patient’s current stage. This ensures care is tailored to meet their unique needs.
Stage 1-2: From Unresponsiveness to Generalized Response
The first steps towards recovery involve moving from being unresponsive to showing generalized responses. In these early stages, patients often show minimal consciousness and start to react physically. These signs are key to tracking their progress.
Signs of Minimal Consciousness
Minimal consciousness shows itself through small responses to stimuli, like slight movements or facial changes. These signs are hopeful for caregivers, showing the patient is starting to come back to life.
Early Physical Reactions
Early physical reactions include reflexive movements, like pulling away a limb when touched or in pain. These reactions mark important steps in the recovery journey, showing the patient is slowly becoming more aware.
What Caregivers Can Expect
Caregivers are key during this time, providing vital support and watching the patient’s progress. They should see slow but steady improvements. But, the speed of recovery can differ greatly from person to person.
| Stage | Characteristics | Caregiver Actions |
|---|---|---|
| Stage 1 | No response to stimuli | Monitor patient’s condition, provide basic care |
| Stage 2 | Generalized responses, such as reflexive movements | Encourage interaction, note any changes in responsiveness |
Knowing about these early recovery stages helps caregivers and family members support their loved ones better. It’s a tough journey, but with the right support, they can make progress.
Stage 3-4: Localized Response and Confused-Agitated State
Patients move into stages 3 and 4 as they recover. They show a localized response and a confused-agitated state. This means they start to notice their surroundings more.
Emerging Awareness
In stage 3, patients react more to certain things. This is a big step because it shows they’re starting to interact with their world in a meaningful way. They might start to listen to commands or notice things they see.
Managing Agitation and Confusion
Stage 4 is when patients might get agitated, confused, or even aggressive. It’s important to manage this to keep them safe and comfortable. Caregivers and doctors work hard to make a calm space. They use gentle words and actions to help.
Communication Breakthroughs
Even with challenges, stages 3 and 4 can be times of big communication wins. Patients might say their first words or answer simple questions. Being consistent and patient is vital in supporting them.
Knowing what stages 3 and 4 are about helps caregivers and doctors help patients more. With the right care, patients can get through these tough times and keep moving forward.
Stage 5-6: Progressing Through Confusion to Appropriate Responses
Stages 5 and 6 of post-coma recovery bring big improvements. Patients get better at knowing where they are and remembering things. They start to answer in ways that make sense, showing they’re getting better.
Improving Orientation
Patients start to know their surroundings better in stages 5 and 6. They recognize people they know, understand time and date, and notice their surroundings more. They also start to help with simple tasks and talk more with their caregivers.
Memory Formation Challenges
Even with better orientation, stages 5 and 6 patients face memory issues. They might forget recent things or have trouble learning new stuff. We help them with memory aids and repeating information to improve their memory.
Developing Consistent Responses
In stages 5 and 6, patients also get better at responding consistently. They react more predictably and in a way that makes sense. We help them through therapy and positive feedback.
Stage 7-8: Achieving Automatic and Purposeful Responses
Reaching automatic and purposeful responses is a big step for coma survivors. It happens in stages 7 and 8. At this time, patients show big improvements in thinking and moving.
Regaining Independence
Stages 7 and 8 bring a big win: getting back independence. Patients start doing things like dressing, eating, and taking care of themselves. This not only helps their body but also their mind.
Cognitive Processing Improvements
These stages also see big leaps in thinking. Patients remember better, solve problems more easily, and react to their surroundings in a smarter way. These skills are key to getting back into daily life.
Potential for Full Recovery
The chance of fully recovering varies, but stages 7 and 8 are hopeful signs. With the right therapy and support, many can make a big comeback. They regain not just physical strength but also their mental sharpness.
| Recovery Stage | Characteristics | Expected Outcomes |
|---|---|---|
| Stage 7 | Automatic responses, improved cognitive function | Increased independence, better problem-solving |
| Stage 8 | Purposeful responses, enhanced memory | Near-normal functioning, possible full recovery |
Common Experiences When Coming Out of a Coma
Coming out of a coma is a tough journey. Patients face many physical, emotional, and mental challenges. They start to wake up and find it hard to adjust.
Amnesia and Memory Gaps
Amnesia or memory loss is common. People may forget what happened before or during their coma. But, in many cases, their memory gets better with time.
Disorientation and Confusion
Feeling lost and confused is also common. Patients might not know where they are or who they are. We try to make their environment calm and familiar to help them.
Sensory Sensitivity
Some people become very sensitive to light, sound, or other things around them. This is called sensory sensitivity. We help manage this by making their environment more comfortable.
Emotional and Behavioral Changes
Changes in mood and behavior are also seen. Patients might get upset, agitated, or act differently. We support them and their families during these tough times.
| Common Experiences | Description |
|---|---|
| Amnesia and Memory Gaps | Difficulty recalling past events or forming new memories |
| Disorientation and Confusion | Feeling uncertain about surroundings, time, or identity |
| Sensory Sensitivity | Overly sensitive to environmental stimuli like light or sound |
| Emotional and Behavioral Changes | Mood swings, agitation, or changes in behavior |
Knowing about these common experiences helps patients and their families. It makes the recovery journey easier. With the right support, we can help those coming out of a coma get better.
The Complete Neurorehabilitation Process
Neurorehabilitation is a detailed process to help people regain their abilities after a coma. It’s a mix of therapies aimed at improving their independence and quality of life.
Physical Therapy Approaches
Physical therapy is key in neurorehabilitation. It focuses on improving movement, strength, and flexibility. Physical therapists create special exercise plans to help patients regain motor skills.
These exercises can include moving joints, walking training, and balance activities. They help patients do everyday tasks better.
Occupational Therapy Interventions
Occupational therapy helps patients do things they enjoy, like taking care of themselves, working, and having fun. Occupational therapists figure out what patients need and find ways to help them.
They use tools and methods to make patients more independent. This includes using special equipment and techniques.
Speech and Language Therapy
Speech and language therapy helps with communication and swallowing problems after a coma. Speech-language pathologists work to improve how patients speak, understand, and express themselves.
They also help with swallowing issues. This therapy is important for patients to talk and connect with others.
Cognitive Rehabilitation
Cognitive rehabilitation focuses on improving thinking skills lost after a coma. This includes memory, attention, and solving problems. Specialists create plans to help patients regain these skills.
They use tools like memory aids and attention training. This helps patients think better and recover faster.
By combining these therapies, neurorehabilitation offers a full support system for coma survivors. Our team works together to make personalized plans for each patient. This helps them achieve the best results.
Medical Complications During Post Coma Recovery
The time after waking up from a coma is filled with possible health problems. As people start to wake up, they might face many health issues. These can affect how well they recover.
Neurological Complications
Neurological problems are a big worry during this time. Issues like seizures, hydrocephalus, and high brain pressure can happen. Seizures often need medicine to control them. Hydrocephalus, where fluid builds up in the brain, might need a shunt to help.
Physical Complications
Physical problems can also occur, like muscle loss, stiff joints, and infections. Being in bed for too long can cause muscles to waste and joints to stiffen. Physical therapy is key to getting back on your feet. Infections, like pneumonia and urinary tract infections, are common because of weak immune systems and medical devices.
Psychological Complications
Psychological issues, like depression, anxiety, and PTSD, can also affect recovery. These might need counseling and medicine to handle. Therapy to improve memory and focus is also important.
Knowing about these possible problems helps doctors give better care. This way, coma survivors can have a better recovery and a better life.
Supporting a Loved One Through Recovery
Helping a loved one recover from a coma needs careful strategies. Your support is key to their recovery. It’s a big role to play.
Communication Techniques
Talking clearly and patiently is important. Use simple words and keep eye contact. This helps them focus. Be patient with their responses, as they might take longer.
Tips for Effective Communication:
- Speak clearly and at a moderate pace
- Use non-verbal cues like touch and gestures
- Encourage them to express their needs and feelings
Creating a Stimulating Environment
A good environment helps a lot. Make their space comfy and familiar. Play their favorite music and show family photos. Having familiar objects around is also good.
Managing Caregiver Stress
Caring for someone can be tough. Watch for signs of stress like feeling tired or anxious. Getting help from others is important.
“Caregivers need to take care of themselves to effectively care for their loved ones.” – Healthcare Professional
Working With the Medical Team
Working with doctors is key. Keep a log of progress and ask questions. This helps ensure your loved one gets the right care.
| Aspect of Care | Role of Caregiver | Role of Medical Team |
|---|---|---|
| Communication | Use effective communication techniques | Provide guidance on communication strategies |
| Environment | Create a stimulating environment | Advise on environmental adjustments |
| Stress Management | Recognize and manage caregiver stress | Offer support and resources for stress management |
Working with doctors and using good communication helps a lot. A good environment and managing stress also play big roles. Together, you can help your loved one recover well.
Long-Term Outcomes for Coma Survivors
Looking at the long-term outcomes for coma survivors is complex. It involves many factors that affect their recovery. The path to health and independence is filled with stages and challenges.
Potential for Independence
Many coma survivors aim to regain their independence. With the right rehabilitation, some make big strides. Rehabilitation programs are key in helping them learn again and adapt.
Common Persistent Deficits
Even with progress, some survivors face lasting challenges. These can be cognitive, physical, or emotional. These deficits can change daily life, needing ongoing support.
Quality of Life Considerations
The quality of life for coma survivors depends on many things. It’s about regaining independence, managing health, and fitting back into communities. Support from family, caregivers, and healthcare professionals is essential.
Stories of Long Coma Survivors
Inspiring stories of coma survivors show the power of hope and care. These stories show that recovery paths and outcomes vary.
Understanding what affects long-term outcomes helps us support coma survivors better. This way, we can help them on their recovery journey.
Conclusion: The Journey of Recovery
Recovering from a coma is a long and unique journey. It needs patience, understanding, and lots of support. We’ve looked at the different stages of getting better, from not being able to respond to being able to do things on purpose.
Many things can affect how well someone recovers. These include how long and deep the coma was, the person’s age, health, and the quality of their medical care. Knowing these things helps family and caregivers support them better.
The path to recovery isn’t always straightforward. Patients might face challenges like memory loss, feeling lost, and mood changes. But, with the right therapy, like physical and speech therapy, many can get their independence back and improve their life quality a lot.
In wrapping up, we stress the importance of a caring and supportive environment. Understanding the complexities of coma recovery and giving the right care and support helps patients on their tough journey. This way, they can reach the best possible outcomes.
What is post coma recovery, and how long does it typically take?
Post coma recovery is different for everyone. It can take weeks to over a year. This depends on the coma’s depth, cause, and medical care.
What are the 8 stages of post coma recovery as outlined by the Rancho Los Amigos Scale?
The Rancho Los Amigos Scale breaks down recovery into 8 stages. These stages show how a person moves from not responding to responding well. They help doctors and caregivers support the recovery process.
What are the common experiences of patients coming out of a coma?
Patients often forget things, feel disoriented, and are sensitive to sounds and lights. They may also act differently or feel new emotions. It’s important to support them through these changes.
What is the comprehensive neurorehabilitation process, and what types of therapies are involved?
Neurorehabilitation includes physical, occupational, speech, and cognitive therapies. These help patients regain independence and improve their thinking. The goal is to achieve the best possible results.
What are the medical complications that can arise during post coma recovery?
Complications can include neurological, physical, and mental issues. Proper care and attention can manage these risks. Working closely with doctors is key.
How can I support a loved one through the recovery process?
Support involves good communication, a stimulating environment, and managing stress. Working with the medical team is also important. This approach helps your loved one recover well.
What are the long-term outcomes for coma survivors, and what can they expect?
Outcomes vary, but many regain independence and live well. Some may face ongoing challenges. It’s important to work with doctors to address these issues.
How long does a coma feel like, and what do people experience during this time?
Coma duration varies, and time perception is different. People may not be aware of their surroundings. The coma period can feel unknown.
Can you talk after waking up from a coma, and what are the communication challenges?
Talking ability varies based on brain injury. Communication challenges are common. Speech therapy can help address these issues.
Is there a cure for coma, and how can medical professionals help?
There’s no cure for coma, but quality care is essential. Doctors manage complications and support recovery. Their help is vital for the patient and their family.
References
- Flint Rehab (TBI Recovery Timeline) : https://www.flintrehab.com/tbi-recovery-timeline
- NeuLife Rehabilitation (10 Recovery Stages After a Brain Injury) : https://neuliferehab.com/what-are-the-10-recovery-stages-after-a-brain-injury
- Matrix Neurological (Brain Injury Stages of Recovery – Ranchos Scale) : https://www.matrixneurological.org/information/fact-sheets/brain-injury-stages-of-recovery-ranchos-scale
- Harvard Medical School (Recovery May Take Time) : https://hms.harvard.edu/news/recovery-may-take-time
- Brain Injury Law Center (Brain Injury Recovery Stages) : https://www.brain-injury-law-center.com/blog/brain-injury-recovery-stages



































