Psychiatry diagnoses and treats mental health conditions, including depression, anxiety, bipolar disorder, and schizophrenia.
Send us all your questions or requests, and our expert team will assist you.
The diagnosis of panic disorder is a rigorous clinical process that requires distinguishing the condition from a wide array of medical and psychiatric mimickers. Because the symptoms of panic are intensely physical, the evaluation pathway often begins in primary care or emergency medicine settings rather than psychiatry. A comprehensive evaluation serves two purposes: confirming the presence of panic disorder according to established nosological criteria and ensuring that no underlying organic pathology is driving the symptoms.
Effective diagnosis relies on a combination of structured clinical interviewing, patient history, physical examination, and the exclusion of other causes. There is no biological marker—no blood test or MRI scan—that positively identifies panic disorder. Instead, diagnosis is by exclusion and positive clinical correlation, requiring a skilled clinician to synthesize data from multiple domains of the patient’s health.

Modern psychiatry operates on the Biopsychosocial Model, which posits that mental health is influenced by three interconnected factors:
Effective psychiatric care addresses all three pillars. It is not simply about “fixing” a chemical imbalance; it is about treating the whole person within their life context.

While both professionals treat mental health conditions, there are distinct differences:
At Liv Hospital, psychiatrists and psychologists work together in a multidisciplinary team to provide comprehensive care.
The cornerstone of the diagnostic process is the clinical interview. This involves a detailed exploration of the nature of the attacks, the context in which they occur, and the patient’s response to them. Clinicians look for the hallmark feature: the unexpected nature of the initial attacks. The interview aims to uncover the “fear of fear” dynamic, assessing whether the patient worries about the implications of the attacks or has changed their behavior in response.
Establishing a timeline is critical. The clinician will inquire about the age of onset, the frequency of attacks, and the duration of the disorder. Panic disorder typically begins in late adolescence or early adulthood; onset after age 45 usually warrants a more aggressive search for medical causes. The chronology also tracks the evolution of symptoms. Often, patients describe a progression from isolated attacks to a state of chronic anticipatory anxiety and eventually avoidance. Understanding this trajectory helps stage the severity of the disorder and plan treatment.
Given the strong heritable component of panic disorder, a thorough family history is essential. Clinicians will investigate the presence of anxiety disorders, depressive disorders, or substance abuse issues in first-degree relatives. A positive family history does not confirm the diagnosis but significantly raises the index of suspicion. It also provides insight into the patient’s environmental upbringing—growing up with anxious parents can model anxious behavior and avoidance coping mechanisms, reinforcing the genetic vulnerability.
To ensure consistency and reliability, clinicians adhere to standardized criteria, typically those outlined in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) or the International Classification of Diseases (ICD). For a diagnosis of panic disorder, the patient must experience recurrent, unexpected panic attacks.
Crucially, at least one of the attacks must be followed by one month or more of one or both of the following:
The diagnosis also stipulates that the disturbance is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a medication) or another medical condition and is not better explained by another mental disorder.
Because panic symptoms are physically profound, a physical examination is mandatory to rule out organic disease. The sympathetic surge of panic mimics several severe medical conditions. Without excluding these, a psychiatric diagnosis is premature and potentially dangerous. The physical exam focuses on the cardiovascular, respiratory, and neurological systems.
Hyperthyroidism (an overactive thyroid) is a classic mimicker of panic disorder. Excess thyroid hormone increases metabolic rate, causing tachycardia, sweating, tremors, and anxiety—symptoms indistinguishable from a panic attack. A Thyroid Stimulating Hormone (TSH) and a reflex-free T4 test are standard evaluations. Other endocrine tumors, such as pheochromocytoma (an adrenal tumor releasing adrenaline), though rare, must be considered if the patient has episodic hypertension and palpitations.
Since chest pain and palpitations are primary symptoms, cardiac evaluation is standard, especially in older patients or those with risk factors. An electrocardiogram (ECG) is typically performed to rule out arrhythmias like supraventricular tachycardia (SVT) or atrial fibrillation, as well as ischemic heart disease. Mitral valve prolapse was once thought to be strongly linked to panic disorder; while the association is now considered weak, cardiac structural integrity is still worth verifying in specific cases.
To quantify the severity of the disorder and monitor treatment progress, clinicians utilize validated rating scales. These are not diagnostic in isolation but provide objective data on the subjective burden of the disease.
These tools allow clinicians to track the “baseline” of the patient’s distress and measure the efficacy of interventions over time.
Differential Diagnosis
The clinician must distinguish panic disorder from other psychiatric conditions where panic attacks occur as a secondary feature.
Correct differential diagnosis is vital because the treatment protocols for these conditions differ significantly from the protocol for primary panic disorder.
For complex cases, a multidisciplinary approach is often required. This may involve a primary care physician to manage general health, a psychiatrist for pharmacological management and diagnostic clarification, and a clinical psychologist for behavioral evaluation. In cases where vestibular symptoms (dizziness, vertigo) are prominent, referral to an otolaryngologist (ENT) or a neurologist may be necessary to rule out inner-ear disorders such as benign paroxysmal positional vertigo (BPPV) or vestibular migraine. This comprehensive approach ensures that the patient is viewed holistically, preventing the “siloing” of symptoms where physical and mental health are treated as unrelated entities.

Send us all your questions or requests, and our expert team will assist you.
Doctors order heart tests (like an ECG) to prioritize safety. The symptoms of panic (chest pain, racing heart) overlap significantly with heart conditions. It is standard medical protocol to rule out the most immediately dangerous causes (cardiac issues) before diagnosing a psychiatric cause. This “rule out” process provides reassurance to both the doctor and the patient.
Yes, substance-induced anxiety is a specific diagnosis. Excessive caffeine intake, stimulant medications (like those for ADHD), corticosteroids, or asthma inhalers can induce physiological arousal that mimics panic. If the attacks stop when the substance is removed, the diagnosis is likely substance-induced anxiety disorder rather than panic disorder.
Panic disorder focuses on the attacks themselves and the fear of the symptoms. Agoraphobia focuses on the fear of the environment—specifically, situations where escape might be intricate or help unavailable if an attack occurs. While they often occur together, a person can have panic disorder without agoraphobia (they don’t avoid places) or agoraphobia without full panic disorder.
If the presentation is classic, a diagnosis can often be made in a single comprehensive session. However, if the medical history is complex or physical symptoms are atypical, the process may take weeks while medical tests (blood work, heart monitoring) are completed to rule out other causes.
Generally, no. MRI or CT scans are not standard for diagnosing panic disorder unless the patient has neurological signs (like seizures, confusion, or one-sided weakness) or a history of head trauma. For typical panic disorder, neuroimaging does not provide diagnostic value.


Vaginal cancer is a rare cancer that affects the vagina. It happens in fewer than 1 in 100,000 women each year. Knowing its symptoms is
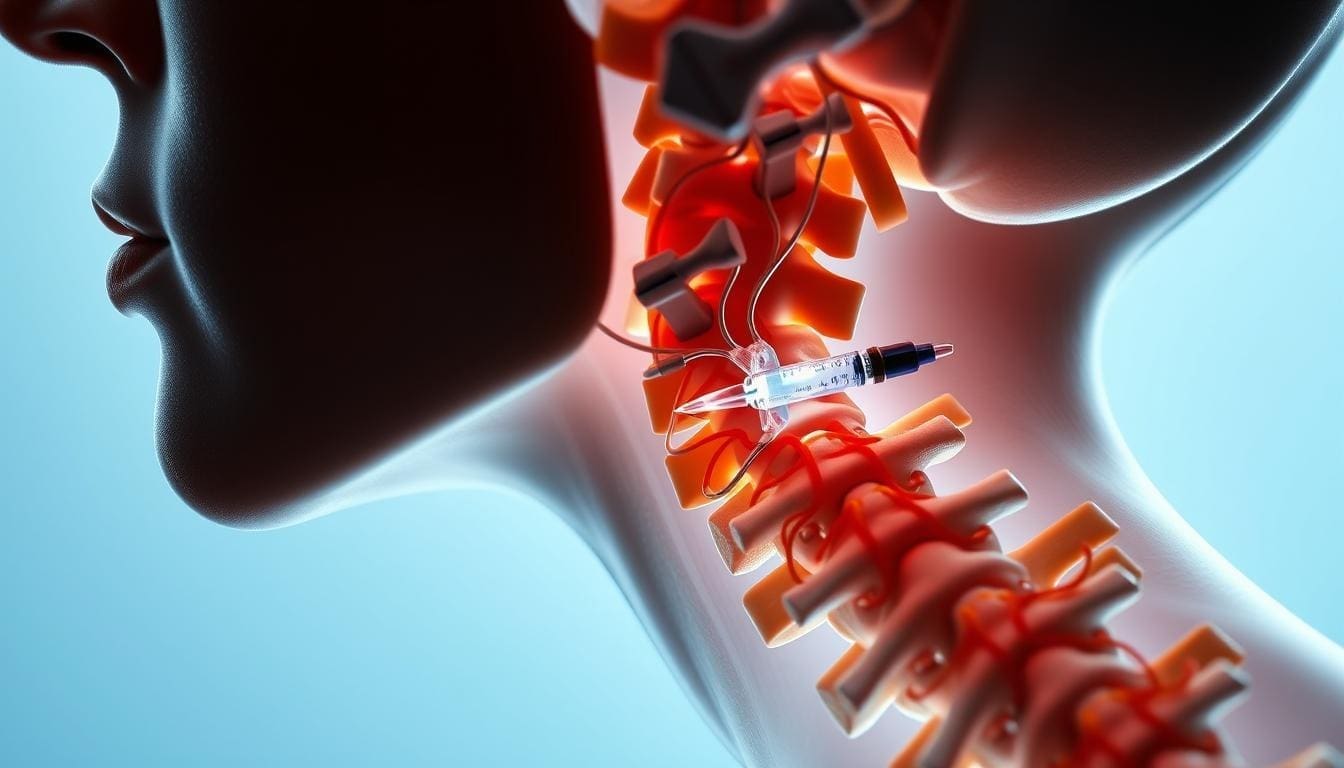
Facet joint injections are a common treatment for chronic neck and back pain. We inject a mix of anesthetic and anti-inflammatory medication into the facet
Carotid artery surgery, also known as carotid endarterectomy, removes plaque from the carotid arteries. It’s key for those at risk of stroke because of narrowed
Knowing about carotid endarterectomy (CEA) is key to avoiding strokes and improving blood flow.neck carotid surgery This surgery removes plaque from the carotid arteries. It
At Liv Hospital, we know how tough neck pain and arm pain can be. These issues often come from cervical spondylosis or disc herniation. That’s
If you’re dealing with neck pain from a herniated or slipped disc, you might have thought about epidural steroid shots. This option is a minimally

Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)