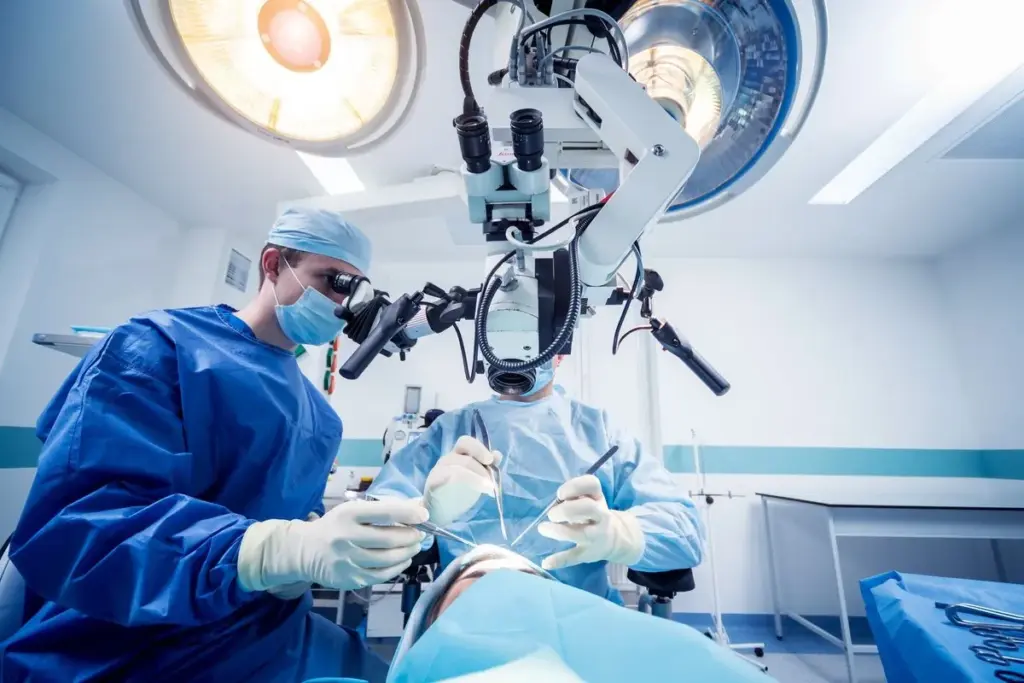
Neurosurgery is a critical field that saves lives but comes with big risks. Did you know that cardiac complications are a major concern in neurosurgical patients? The complex nature of these surgeries and the patient’s health can lead to heart problems.
Use the Rcri score to predict dangerous cardiac risks during surgery. Learn how this vital tool keeps patients safe during neurosurgery today.
It’s vital to check the heart risk in neurosurgery patients for the best results. The Revised Cardiac Risk Index (RCRI) helps with this. It’s a key tool for assessing heart risk in surgeries, including neurosurgery. By knowing the risks and using the RCRI, doctors can make better choices to avoid complications.
Key Takeaways
- Neurosurgery carries significant risks, including cardiac complications.
- The Revised Cardiac Risk Index (RCRI) is used to assess cardiac risk.
- Evaluating cardiac risk is critical for better patient outcomes.
- Healthcare providers use the RCRI to make informed decisions.
- Reducing heart risk is key in neurosurgical procedures.
The Landscape of Neurosurgical Procedures and Their Risk
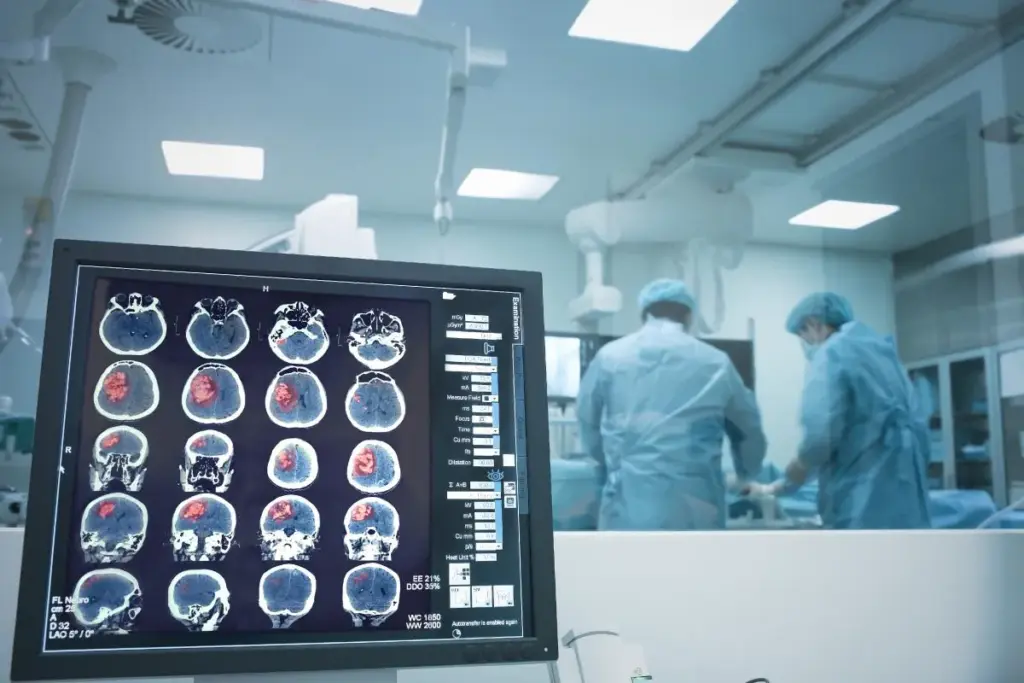
Neurosurgery is a complex field with many procedures. These treatments aim to fix problems in the brain, spine, and nervous system. While they can save lives, they also come with risks that must be weighed carefully.
Common Neurosurgical Interventions
Neurosurgery includes a wide range of procedures. Some common ones are:
- Cranial surgeries for tumors, aneurysms, or hemorrhages
- Spinal surgeries for herniated discs, spinal stenosis, or deformities
- Neuroendovascular procedures for vascular conditions
- Functional neurosurgery for movement disorders or chronic pain
Each procedure has its own risks and possible complications. For example, cranial surgeries might lead to neurological problems, infection, or swelling. Spinal surgeries could result in nerve damage, infection, or failure of implanted devices.
Inherent Risks in Neurosurgical Procedures
Neurosurgical procedures come with inherent risks, including:
|
Risk Category |
Description |
Examples |
|---|---|---|
|
Surgical Risks |
Risks directly related to the surgical intervention |
Bleeding, infection, nerve damage |
|
Anesthesiological Risks |
Risks associated with anesthesia administration |
Respiratory complications, allergic reactions |
|
Cardiac Risks |
Risks related to cardiac complications |
Myocardial infarction, cardiac arrest |
It’s key to understand these risks for better management. By spotting complications early, doctors can reduce them, helping patients recover better.
Comprehensive risk assessment is vital for neurosurgical procedures. It’s not just about the procedure but also the patient’s health. With careful planning and risk management, we can improve patient care and reduce risks.
Patient-Specific Risk Factors in Neurosurgery
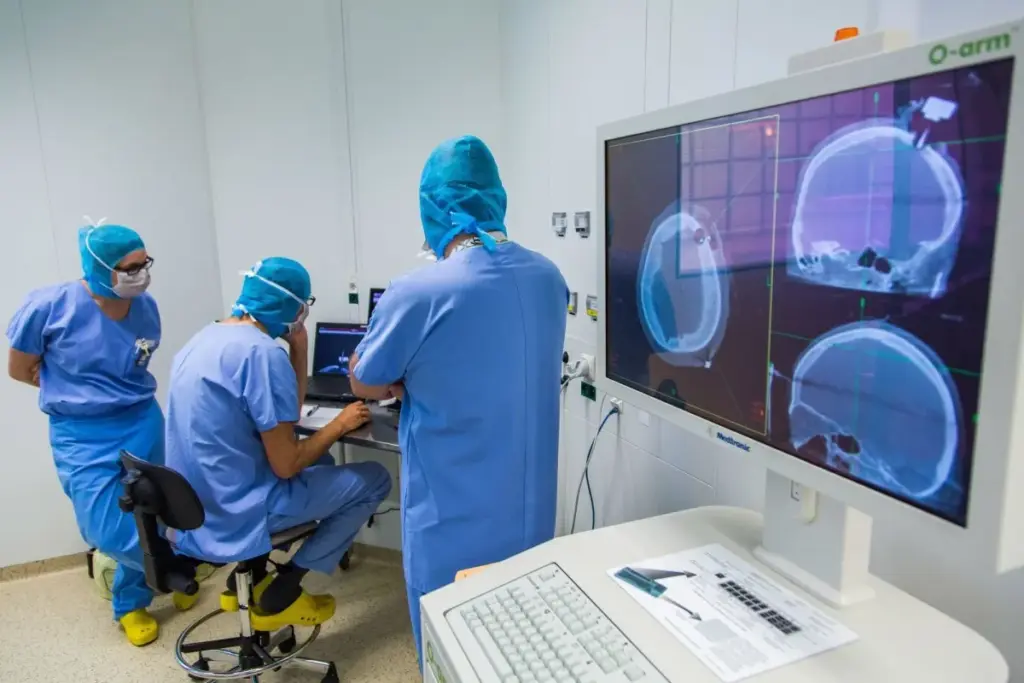
When it comes to neurosurgery, each patient’s unique factors are key. These factors help doctors decide the best course of action. This way, they can lower risks and get better results.
Every patient’s medical history, age, and health conditions affect their surgery risk. “The key to successful neurosurgery lies in understanding and managing patient-specific risk factors,” say top neurosurgeons.
Age-Related Considerations
Age is a big deal when it comes to surgery risks. Older patients often face more health issues and have less energy to recover. For example, older people might be more at risk for postoperative cognitive dysfunction because their brains are less resilient.
Younger patients, on the other hand, might have fewer health problems but could face long-term risks from surgery. We need to think carefully about these differences when planning surgeries.
Comorbidities Affecting Neurosurgical Outcomes
Having other health conditions can really change how well a surgery goes. Issues like diabetes, hypertension, and heart disease can make surgery harder and recovery slower. For instance, diabetes can slow down healing, raising the chance of infections.
It’s very important to manage these conditions well before, during, and after surgery. This means working together with different doctors and taking good care of the patient. By focusing on these specific factors, we can make surgeries safer and more successful.
“A thorough check-up before surgery is key to spotting and handling health issues that could affect surgery results,” say recent guidelines.
The RCRI Score: Evaluating Cardiac Risk in Neurosurgical Patients
The RCRI score is key for checking cardiac risk in neurosurgery patients. It comes from the Revised Cardiac Risk Index. This method is known for checking cardiac risk in surgeries not related to the heart.
Development and Validation of the Revised Cardiac Risk Index
The Revised Cardiac Risk Index was made to forecast heart problems in non-heart surgery patients. It found important risk factors for heart issues during surgery. Studies prove the RCRI score works well in predicting heart problems in surgeries, including neurosurgery.
The Six RCRI Criteria
The RCRI score uses six criteria:
- High-risk surgery
- History of ischemic heart disease
- History of congestive heart failure
- History of cerebrovascular disease
- Preoperative treatment with insulin
- Preoperative serum creatinine > 2.0 mg/dL
To understand the RCRI criteria for neurosurgical patients, let’s look at them in a table.
|
RCRI Criterion |
Description |
Relevance to Neurosurgery |
|---|---|---|
|
High-risk surgery |
Surgical procedures that are considered high-risk for cardiac complications |
Many neurosurgical procedures are considered high-risk due to their complexity and impact on vital functions. |
|
History of ischemic heart disease |
Previous myocardial infarction or angina |
Patients with a history of ischemic heart disease are at higher risk of cardiac complications during neurosurgery. |
|
History of congestive heart failure |
Previous diagnosis of congestive heart failure |
Congestive heart failure can complicate neurosurgical procedures due to limited cardiac reserve. |
|
History of cerebrovascular disease |
Previous stroke or transient ischemic attack |
Relevant for neurosurgical patients as it indicates vascular pathology. |
|
Preoperative treatment with insulin |
Diabetes requiring insulin therapy |
Indicates metabolic issues that could affect surgical outcomes. |
|
Preoperative serum creatinine > 2.0 mg/dL |
Renal insufficiency indicated by elevated serum creatinine |
Renal dysfunction can impact the clearance of anesthetic and other drugs used in neurosurgery. |
By using the RCRI score, doctors can better check cardiac risk in neurosurgical patients. This helps in making better decisions and might lower the risk of heart problems.
Applying the RCRI Calculator in Neurosurgical Risk Assessment
Healthcare providers use the RCRI calculator to assess cardiac risks before surgery. The Revised Cardiac Risk Index (RCRI) is key for checking cardiac risk in surgeries, like neurosurgery.
Step-by-Step Guide to RCRI Calculation
To find the RCRI score, we look at six criteria. Let’s go through these steps to see how to use the RCRI calculator.
- High-risk surgery
- History of ischemic heart disease
- History of congestive heart failure
- History of cerebrovascular disease
- Diabetes requiring insulin
- Preoperative serum creatinine > 2.0 mg/dL
Each criterion gets one point. The total score helps us understand the patient’s cardiac risk.
|
RCRI Score |
Cardiac Risk |
Recommended Action |
|---|---|---|
|
0 |
Low |
Proceed with surgery |
|
1-2 |
Moderate |
Consider further evaluation |
|
3 or more |
High |
Optimize cardiac condition before surgery |
Clinical Decision-Making Based on RCRI Scores
The RCRI score plays a big role in making decisions in neurosurgery. A higher score might mean more tests or better heart health before surgery. We adjust our plans based on each patient’s risk.
Clinical Decision-Making Example: If a patient scores 3 or more, we might wait to improve their heart health. This could lower the risk of heart problems during and after surgery.
Using the RCRI calculator helps us make better choices. This improves patient results in neurosurgery.
Alternative Risk Assessment Tools in Neurosurgery
There are new tools for assessing risks in neurosurgery. These tools help tailor care to each patient. This approach improves outcomes.
ASA Physical Status Classification System
It ranges from ASA I (healthy) to ASA VI (brain-dead with organs for donation). For example, ASA III means severe systemic disease. This helps doctors plan better.
Neurosurgery-Specific Risk Calculators
These calculators predict complications after neurosurgery. They look at patient details, health issues, and surgery type. They help neurosurgeons understand risks better.
For instance, they might consider age, diabetes, and surgery type. This helps in planning care and getting consent.
Every patient is different. These tools give a deeper look at neurosurgery risks. With these and clinical knowledge, doctors can manage risks better.
Comprehensive Risk Stratification in Neurosurgical Procedures
Risk stratification is key in neurosurgery to keep patients safe and ensure the best results. Neurosurgery is complex and carries risks. So, a detailed approach to risk stratification is vital to spot and reduce complications.
Preoperative Risk Evaluation Process
The preoperative risk evaluation is a major part of risk stratification in neurosurgery. It checks the patient’s medical history, current health, and the risks of the surgery. We use tools like the Revised Cardiac Risk Index (RCRI) to predict cardiac risks.
It also looks at the patient’s function, comorbidities, and lab and imaging results. This helps us understand the patient’s risk better.
Multidisciplinary Approach to Risk Assessment
In neurosurgery, a team effort is essential due to the high risks. Neurosurgeons, anesthesiologists, cardiologists, and others work together. This ensures all risks are considered and strategies are made to reduce them.
The team reviews the patient’s case and plans for managing risks. This teamwork improves safety and leads to better care and decisions.
Major Adverse Cardiac Events (MACE) in Neurosurgery
Major adverse cardiac events (MACE) are a big worry for patients having neurosurgery. These events can greatly affect how well a patient does after surgery. It’s very important for doctors to know how often MACE happen, how common they are, and how to stop them.
Incidence and Prevalence in Neurosurgical Patients
The chance of MACE happening in neurosurgery patients can change a lot. This depends on the surgery type, the patient’s health before surgery, and their heart risk. Research shows that neurosurgery patients face a higher risk of heart problems. This is because surgery can be stressful, there might be blood loss, and fluid levels can change.
“The risk of heart problems in neurosurgery patients is a big worry,” say experts. “It means we need to check their heart health before surgery and watch them closely.”
“Heart problems are a major reason for sickness and death in neurosurgery patients. This highlights the necessity of implementing effective prevention strategies.”
Prevention Strategies for MACE in Neurosurgery
To stop MACE in neurosurgery, we need to use many different methods. This includes checking the patient’s heart risk before surgery, making sure the heart is working well, and managing the surgery carefully. Using tools like the Revised Cardiac Risk Index (RCRI) can help find patients at higher risk for MACE.
- Pre-surgery, make sure the heart medicines are right and the heart is in good shape.
- During surgery, keep an eye on blood flow and heart rate.
- After surgery, watch closely over patients who are at high risk.
By using these methods, doctors can lower the chance of MACE and help patients do better after neurosurgery. As we learn more about heart risks in neurosurgery, we can make our care even better to protect our patients’ hearts.
Anesthesiological Risks and Considerations in Neurosurgery
Neurosurgery is a complex field that requires careful planning from anesthesiologists. They must understand both the surgery and anesthesia to keep patients safe. This ensures the best possible results for patients.
Unique Challenges in Neuroanesthesia
Neuroanesthesia is a specialized area that comes with its own set of challenges. Anesthesiologists must keep the brain’s blood flow right while making sure the patient is asleep enough. Managing the pressure inside the skull is key to avoiding problems during surgery.
Another big challenge is getting the patient to wake up quickly after surgery. This is so doctors can check the brain right away. It’s a fine line between keeping the patient asleep during surgery and waking them up fast and safely.
The ASA Score in Anesthetic Risk Assessment
- ASA I: Normal healthy patient
- ASA II: Patients with mild systemic disease
- ASA III: Patients with severe systemic disease
- ASA IV: Patients with severe systemic disease that is a constant threat to life
- ASA V: Moribund patients who are not expected to survive without the operation
Using the ASA score helps anesthesiologists plan better. It’s a simple but powerful tool in getting ready for surgery. It helps doctors make safer choices for their patients.
Cardiac Clearance Protocols for Neurosurgical Patients
Neurosurgery needs careful planning before the operation. This includes checking the heart to lower surgery risks. It’s key to make sure patients are ready for surgery to avoid heart problems.
Preoperative Cardiac Evaluation Guidelines
Checking the heart before surgery is very important. Guidelines say to look at the patient’s heart history, like past heart attacks, artery disease, and heart failure. The Revised Cardiac Risk Index (RCRI) helps guess the chance of heart problems during and after surgery.
The heart check-up includes talking about the patient’s health, a physical exam, and tests like ECGs and echocardiograms. Those with big heart risks might need more tests, like stress tests or imaging.
Medical Optimization Before Neurosurgery
Getting the patient’s health ready for surgery is key to lower heart risks. This means controlling high blood pressure, diabetes, and high cholesterol. Patients with artery disease might need to adjust their blood thinners and might need to have their arteries fixed.
We work on improving the patient’s health with lifestyle changes and medicine tweaks. This could mean quitting smoking, losing weight, and starting or changing medicines like beta-blockers and statins. Making the patient ready for surgery takes teamwork from neurosurgeons, cardiologists, anesthesiologists, and more.
Surgical vs. Procedural Risk in Neurosurgical Interventions
The world of neurosurgery is complex. Different procedures have different surgical and procedural risk levels. Knowing these risks helps in choosing the best surgical method.
Neurosurgery includes minimally invasive and open procedures. Each type has its own risk level. Let’s dive into these to understand their risks better.
Minimally Invasive Neurosurgical Procedures
Minimally invasive neurosurgery aims to cause less damage and speed up recovery. It uses smaller cuts and less tissue disruption than traditional surgery.
The perks of these procedures are:
- Lower risk of infection
- Less pain after surgery
- Shorter hospital stays
- Quicker return to daily activities
But, minimally invasive procedures also have risks. These include limited view of the surgical area and possible incomplete procedure due to technical issues.
Open Neurosurgical Procedures
Open neurosurgery uses a bigger incision for better access to the brain or spine. It’s more invasive but gives the surgeon a clear view of the area.
The benefits of open neurosurgery are:
- Clearer view of complex anatomy
- Handling of big or complex lesions
- More control over bleeding and complications
But, open neurosurgical procedures also come with higher risks. These include higher infection risk, longer recovery, and possible tissue damage.
In summary, both minimally invasive and open neurosurgical methods are important in neurosurgery. Each has its own risks and benefits. Knowing these differences is key to improving patient care and outcomes.
Risk Mitigation Strategies in High-Risk Neurosurgical Cases
Effective risk mitigation in neurosurgery needs a full plan. This plan covers before, during, and after surgery. We focus on making patients better before surgery and keeping an eye on them during surgery.
Preoperative Optimization Techniques
Getting patients ready for surgery is key. We check their health history and current status. We also look at any risks they might have.
We work on managing conditions like high blood pressure and diabetes. These can affect how well a patient does during surgery.
- Medical Optimization: Making sure chronic conditions are under control.
- Nutritional Support: Helping patients eat better to improve their health.
- Smoking Cessation: Helping patients stop smoking to lower risks.
|
Preoperative Optimization Technique |
Description |
Benefit |
|---|---|---|
|
Medical Optimization |
Managing chronic conditions |
Reduces surgical risks |
|
Nutritional Support |
Improving nutritional status |
Enhances recovery |
|
Smoking Cessation |
Quitting smoking before surgery |
Decreases pulmonary and cardiac complications |
Intraoperative Monitoring and Management
Watching patients closely during surgery is very important. We use advanced tools to keep an eye on their health. This lets us act fast if something goes wrong.
- Advanced Neuromonitoring: Techniques like EEG and SSEP help check brain function.
- Hemodynamic Monitoring: We watch blood pressure and heart function closely.
- Anesthetic Management: We adjust anesthesia to fit the patient’s needs and the surgery.
By getting patients ready before surgery and watching them closely during, we can lower risks. This leads to better results for our patients.
Comparing Neurosurgical Risk Across Different Procedures
It’s important to compare the risks of different neurosurgical procedures. These procedures vary in complexity and risk. Understanding these differences helps doctors make better decisions for their patients.
Highest Risk Neurosurgical Interventions
Some neurosurgical procedures are considered high-risk. This is because of their complexity or the critical areas they involve. For example, surgeries near the brainstem are high-risk due to the risk of serious brain damage.
Examples of high-risk procedures include craniectomies for traumatic brain injury and resection of brain tumors in eloquent areas. These surgeries need careful planning and management to reduce risks.
- Craniectomies for traumatic brain injury
- Resection of brain tumors in eloquent areas
- Surgery involving the brainstem
Lower Risk Neurosurgical Procedures
On the other hand, some neurosurgical procedures are considered lower risk. These include minimally invasive surgeries like endoscopic discectomies or certain shunt placements. These procedures generally have fewer complications than more invasive surgeries.
The risk of neurosurgical procedures also depends on the patient. Factors like age, health conditions, and the type of problem being treated are important. Knowing these factors helps doctors provide better care and improve outcomes.
|
Procedure Type |
Risk Level |
Common Complications |
|---|---|---|
|
Craniectomy for TBI |
High |
Infection, cerebral edema |
|
Endoscopic Discectomy |
Low |
Nerve damage, infection |
Patient Communication and Informed Consent in High-Risk Neurosurgery
High-risk neurosurgery needs a detailed approach to talking with patients and getting their consent. It’s important to tell patients about the risks, benefits, and other options. This is both a legal and ethical must in neurosurgery.
Effective Risk Communication Strategies
In neurosurgery, where risks are high and mistakes can be fatal, clear communication is key. We must use methods that help patients understand and build trust with their doctors.
- Clear explanation of the procedure and its associated risks
- Discussion of possible complications and how likely they are
- Presentation of other treatment choices
- Encouragement of patient questions and concerns
“Clear and empathetic communication is essential in building trust between neurosurgeons and their patients, especially in high-stakes decision-making scenarios.”
Shared Decision-Making Process
The shared decision-making process is key to patient-centered care in neurosurgery. It’s about working together with patients to make choices that respect their wishes and values.
|
Components of Shared Decision-Making |
Description |
|---|---|
|
Patient Education |
Providing patients with all the info about their condition and treatment options. |
|
Risk Assessment |
Looking at the risks of different treatments. |
|
Patient Preferences |
Understanding and respecting the patient’s values and preferences in making decisions. |
By involving patients in decisions, we can make sure the treatment fits their goals and hopes. This leads to better results for them.
Conclusion: Navigating the Risk Landscape in Modern Neurosurgery
Understanding and managing risks in modern neurosurgery is key for the best patient results. The Revised Cardiac Risk Index (RCRI) guidelines help doctors assess heart risks in neurosurgery patients. This helps them make better decisions for their patients.
We’ve looked at different tools and strategies for risk assessment. These include the RCRI score, ASA Physical Status Classification System, and neurosurgery-specific risk calculators. These tools help doctors understand and manage risks better.
Using these tools and strategies can help reduce complications and improve care in neurosurgery. It’s important to understand the risks and work together to care for patients.
FAQ
What is the Revised Cardiac Risk Index (RCRI) score, and how is it used in neurosurgery?
The RCRI score helps doctors check the heart risk of patients going for non-heart surgery, like neurosurgery. It looks at six things to guess the chance of big heart problems.
How do patient-specific factors impact neurosurgical outcomes?
Things like age, health problems, and overall health really affect how well a patient does after neurosurgery. Older people or those with big health issues might face more risks.
What are the risks associated with neurosurgical procedures?
Neurosurgery can lead to heart problems, brain issues, and infections. It’s key to figure out the risks to make sure patients do well.
How is the RCRI score calculated, and what does it signify?
The RCRI score looks at six things: risky surgery, heart disease history, heart failure history, brain disease history, insulin use, and kidney function. A higher score means a bigger heart risk.
What alternative risk assessment tools are used in neurosurgery?
Other tools used in neurosurgery include the ASA Physical Status Classification System and special neurosurgery risk calculators. They give more info on patient risk and help plan care.
How is cardiac clearance done for neurosurgical patients?
Cardiac clearance for neurosurgery patients means checking their heart before surgery. Making sure patients are healthy before surgery is key to lower heart risks.
What are the differences in risks between minimally invasive and open neurosurgical procedures?
Minimally invasive surgeries usually have less risk than open surgeries. But, the risks depend on the surgery, the patient, and other things.
How can risks be mitigated in high-risk neurosurgical cases?
To lower risks in high-risk surgeries, doctors use special techniques before and during surgery. A team effort is important for better patient results.
Why is effective risk communication important in high-risk neurosurgery?
Good risk talk is key in high-risk neurosurgery. It makes sure patients know what’s going on and can make choices. It’s about caring for patients and doing the right thing.
What is the role of a multidisciplinary approach in risk assessment for neurosurgery?
A team of doctors, including neurosurgeons and anesthesiologists, is vital for checking and managing risks in neurosurgery. They work together for the best care.
How does the ASA score assess anesthetic risk in neurosurgery?
The ASA score helps doctors understand the risk of anesthesia by classifying patients. It helps spot who might need extra care during anesthesia.
What are Major Adverse Cardiac Events (MACE) in neurosurgery, and how can they be prevented?
MACE in neurosurgery are serious heart problems that can happen during or after surgery. To stop them, doctors check the heart before surgery, make patients healthy, and watch them closely during surgery.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC9568714/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























