Infiltrative kidney diseases occur when abnormal cells or substances infiltrate the kidney tissue. This can lead to chronic conditions or cancer. At Liv Hospital, we offer detailed care for these conditions. We understand how important it is to know about their prevalence and impact.
These diseases include chronic kidney disease (CKD) and kidney cancers like renal cell carcinoma. They silently harm millions worldwide, affecting kidney function.
It’s key to grasp the infiltrative process and its effects on kidneys. New research and care models are coming up. We’re dedicated to top-notch healthcare and support for international patients.
Key Takeaways
- Infiltrative diseases of the kidneys involve the invasion of kidney tissue by abnormal cells or substances.
- Conditions such as CKD and renal cell carcinoma are classified as infiltrative kidney diseases.
- Liv Hospital offers detailed care for patients with infiltrative kidney diseases.
- Understanding the prevalence and impact of these conditions is vital for effective care.
- New research and patient-centered care models are emerging to tackle infiltrative kidney diseases.
Understanding Infiltrative Kidney Diseases

“Infiltrative kidney diseases” refers to many disorders where abnormal cells or substances invade the kidney. These issues can greatly affect how well the kidneys work.
Definition and Basic Pathophysiology
Infiltrative kidney diseases happen when foreign cells, proteins, or substances enter the kidney tissue. This can harm the kidney’s function, causing various symptoms. The disease process involves complex interactions between the invading substances and the kidney’s cells.
Key aspects of the pathophysiology include:
- Infiltration of abnormal cells or substances
- Inflammation and immune response
- Fibrosis and scarring
- Potential progression to chronic kidney disease
Impact on Kidney Structure and Function
Infiltrative kidney diseases can change the kidneys’ structure and function. Tools like ultrasound and CT scans are key in diagnosing these diseases. They give detailed images of the kidney’s anatomy.
|
Imaging Modality |
Typical Findings in Infiltrative Kidney Diseases |
|---|---|
|
Ultrasound |
Changes in kidney size, echogenicity, and presence of masses or lesions |
|
CT Scan |
Detailed assessment of kidney anatomy, detection of tumors or infiltrative lesions |
It’s vital to understand how infiltrative kidney diseases affect the kidneys. This knowledge helps in finding the best treatments.
The Infiltrative Process in Renal Pathology
The infiltrative process in renal pathology is complex. It involves changes in cells and molecules. These changes allow abnormal cells or substances to enter kidney tissue, altering its structure and function.
Mechanisms of Tissue Invasion
The ways tissue invasion happens in renal pathology are many. Abnormal cell growth and changes in how cells stick together are important. Also, changes in the area outside cells and the use of certain enzymes help cells invade.
This process often damages the normal structure of tissue. It lets abnormal cells spread and harm kidney function. Knowing how this works is key to finding better ways to diagnose and treat.
Cellular and Molecular Changes
Changes in cells and molecules are key in the infiltrative process. Molecular changes, like genetic mutations, push renal pathology forward. For example, some genetic changes can cause primary renal neoplasms, which can be either benign or cancerous.
Also, new imaging methods, like renal carcinoma ultrasound, help spot and understand renal lesions better. These tools help doctors find and treat patients who need it.
The infiltrative process in renal pathology is a complex mix of cell and molecular changes. Figuring out these changes is vital for better understanding kidney diseases and finding new treatments.
Types of Renal Neoplasms and Their Characteristics
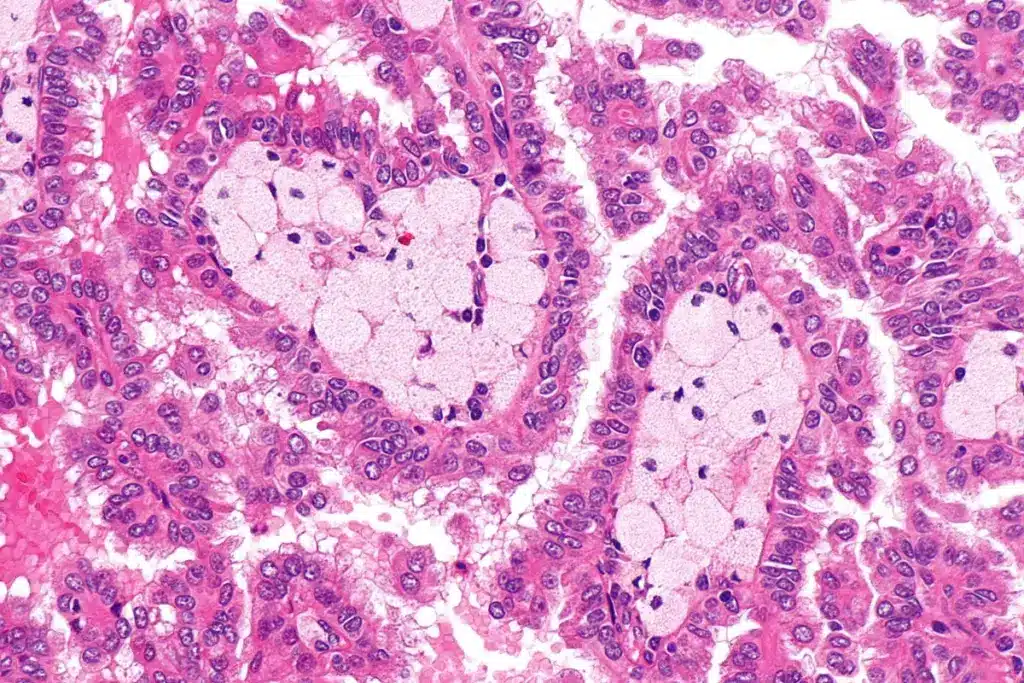
Kidney tumors, or renal neoplasms, are abnormal growths. They can be found through tests like kidney tumor ultrasound. These growths can be either benign or malignant, each with its own traits and effects on health.
Benign vs. Malignant Renal Masses
Renal masses are divided into benign and malignant types. Benign renal masses are non-cancerous and don’t spread. Examples include:
- Renal cysts
- Adenomas
- Angiomyolipomas
Malignant renal masses, by contrast, are cancerous. They can spread to other parts of the body. The most common type is renal cell carcinoma (RCC).
Classification Systems for Kidney Tumors
Kidney tumors are sorted based on their look, genetics, and how they behave. The World Health Organization (WHO) classification is widely used. It groups tumors by their appearance and genetic makeup.
This system helps in:
- Figuring out the prognosis
- Deciding on treatment
- Improving communication among doctors
Chronic Kidney Disease as an Infiltrative Condition
Chronic kidney disease (CKD) is a big health problem worldwide. It causes kidney damage over time. It’s linked to diabetes, high blood pressure, and genetics.
Progressive Nature of CKD
CKD gets worse over time if not treated. Inflammation and fibrosis in the kidneys cause permanent damage. The disease involves complex changes in cells and molecules that harm kidney function.
Knowing how CKD gets worse is key to managing it. Early treatment can slow the disease’s progress. For more info, check out studies on.
Global Prevalence and Impact
CKD affects about 13.4% of the world’s population. It lowers the quality of life and costs healthcare systems a lot.
|
Region |
Prevalence of CKD (%) |
Estimated Number of Cases |
|---|---|---|
|
North America |
14.8 |
Approximately 37 million |
|
Europe |
12.6 |
Around 61 million |
|
Asia |
13.1 |
Nearly 174 million |
The world needs better ways to fight CKD. Early detection and treatment can help a lot.
Renal Cell Carcinoma: Primary Renal Neoplasm
Renal cell carcinoma is a main type of kidney cancer in adults. It makes up about 90% of all cases. We will look into its subtypes, how it looks under a microscope, and its impact on people.
Subtypes and Histological Features
Renal cell carcinoma is not just one type of cancer. It’s a group of cancers with different looks and genetic makeup. The main types are:
- Clear cell renal cell carcinoma (ccRCC), which is the most common, making up 70-80% of cases. It has cells with clear cytoplasm because of glycogen and lipids.
- Papillary renal cell carcinoma (pRCC), which is about 10-15% of cases. It’s split into two types based on its look and genetics.
- Chromophobe renal cell carcinoma, a less common type. It has a better outlook than clear cell and papillary types.
Each type has its own look and genetic changes. These are key for diagnosing and predicting how the cancer will behave.
Incidence and Mortality Statistics
Renal cell carcinoma is a big health problem worldwide. In the U.S., it’s about 4% of all new cancer cases, as seen in 2025 data. The number of cases has gone up because more tumors are found by chance.
Renal cell carcinoma affects many people, with a lot of new cases each year. It has a high death rate, showing the need for early detection and treatment.
Knowing about renal cell carcinoma’s types, how it looks, and its statistics is key. We aim to raise awareness and improve treatment for those with this disease.
Other Infiltrative Kidney Diseases
Infiltrative kidney diseases include lymphomas and amyloidosis. These conditions harm the kidneys’ function.
They are different from diseases that start in the kidneys. They can greatly affect the kidneys’ structure and how they work.
Lymphomas and Metastatic Tumors
Lymphomas are cancers of the lymphatic system. They can spread to the kidneys, either as a main site or as part of a wider disease.
Metastatic tumors in the kidney are also common. The most usual places these tumors come from are the lung, breast, and colon.
|
Disease |
Characteristics |
Clinical Implications |
|---|---|---|
|
Lymphoma |
Cancer of the lymphatic system |
Renal infiltration, possible acute kidney injury |
|
Metastatic Tumors |
Cancer spread from other primary sites |
Renal dysfunction, possible hematuria |
Amyloidosis and Depositional Diseases
Amyloidosis is when abnormal proteins (amyloid) build up in tissues, including the kidneys. This leads to progressive renal failure.
Other diseases like light chain deposition disease also harm the kidneys. They do this by building up abnormal proteins.
Risk Factors for Infiltrative Kidney Diseases
Several key risk factors have been identified for infiltrative kidney diseases. These include hypertension, diabetes, and environmental exposures.
Hypertension and Diabetes: Major Contributors
Hypertension and diabetes are major risk factors for kidney diseases. Hypertension damages the blood vessels in the kidneys, making them less effective. Diabetes can cause diabetic nephropathy, a common cause of chronic kidney disease.
Managing these conditions is key to preventing kidney disease. Studies show that controlling blood pressure and blood sugar can lower the risk of kidney problems.
Environmental and Genetic Factors
Exposure to certain chemicals and heavy metals increases the risk of kidney disease. Genetic predisposition also plays a role, with some genetic mutations making people more susceptible to kidney diseases.
|
Risk Factor |
Description |
Impact |
|---|---|---|
|
Hypertension |
High blood pressure damaging kidney blood vessels |
Increased risk of kidney disease progression |
|
Diabetes |
Diabetic nephropathy leading to chronic kidney disease |
Significant cause of kidney failure |
|
Environmental Exposures |
Exposure to chemicals and heavy metals |
Increased risk of kidney damage |
|
Genetic Predisposition |
Genetic mutations affecting kidney function |
Increased susceptibility to kidney diseases |
Understanding and managing risk factors for infiltrative kidney diseases is vital. By addressing hypertension, diabetes, environmental exposures, and genetic predisposition, we can reduce disease incidence and improve outcomes.
Clinical Presentation and Symptoms
It’s important to know the signs of infiltrative kidney diseases early. This helps in getting the right treatment quickly. These diseases can show up in different ways, based on the cause and how much the kidneys are affected.
Early Warning Signs
The first signs of infiltrative kidney diseases can be hard to spot. They might include:
- Fatigue and general malaise
- Weight loss
- Loss of appetite
- Mild flank pain or discomfort
These symptoms can point to a kidney problem. But they don’t only mean kidney disease. It’s key to be careful, mainly if you have risk factors like high blood pressure, diabetes, or a family history of kidney issues.
Advanced Disease Manifestations
As these diseases get worse, symptoms get more serious. Signs of advanced disease might include:
- Severe flank pain
- Hematuria (blood in the urine)
- Proteinuria (excess protein in the urine)
- Renal failure symptoms, such as edema, electrolyte imbalances, and uremia
The exact symptoms can depend on the type of disease. For example, kidney cancer might show up as a mass in the belly. Lymphoma could cause swollen lymph nodes and other widespread symptoms.
|
Symptom |
Early Disease |
Advanced Disease |
|---|---|---|
|
Flank Pain |
Mild discomfort |
Severe pain |
|
Hematuria |
Microscopic |
Gross hematuria |
|
Proteinuria |
Mild |
Nephrotic range |
|
Renal Function |
Normal or mildly impaired |
Significantly impaired |
Spotting these symptoms early is key. It helps in starting treatment right away for infiltrative kidney diseases.
Diagnostic Imaging of Renal Masses
Diagnostic imaging is key in checking and treating kidney tumors. We use different imaging methods to find and understand kidney tumors. This is vital for picking the right treatment.
Ultrasound Findings in Kidney Tumors
Ultrasound is often the first tool used to look at kidney tumors. It’s easy and gives important info about the tumor’s size, where it is, and what it looks like. Ultrasound can tell if a mass is cystic or solid, but it’s not always clear.
A study in the Journal of Ultrasound in Medicine shows ultrasound’s role in finding kidney cancer. It says ultrasound is good at spotting kidney tumors but not always sure.
“Ultrasound is a valuable initial imaging modality for renal masses, but further characterization with CT or MRI is often necessary.”
– Journal of Ultrasound in Medicine
CT and MRI Evaluation
CT and MRI are key for looking closer at kidney tumors found by ultrasound. CT scans give detailed pictures that show the tumor’s size, where it is, and if it’s touching other parts.
|
Imaging Modality |
Key Features |
Clinical Utility |
|---|---|---|
|
Ultrasound |
Initial assessment, differentiation between cystic and solid masses |
First-line imaging for renal masses |
|
CT Scan |
Detailed cross-sectional images, assessment of tumor size and invasion |
Staging and preoperative planning |
|
MRI |
High-resolution images, characterization of tumor composition |
Problem-solving, specially for complex cases |
MRI is great for figuring out what a kidney tumor is made of and how it relates to nearby areas. It’s used when CT scans are not clear or when there’s worry about too much radiation or allergy to contrast.
In summary, using ultrasound, CT, and MRI together gives a full view of kidney tumors. This helps doctors make the best choices for their patients.
Laboratory Tests and Kidney Biopsy
Diagnosing kidney diseases often involves lab tests and a kidney biopsy. These methods help doctors see how much damage there is and what might be causing it.
Blood and Urine Biomarkers
Laboratory tests are key in spotting kidney diseases. Blood tests check for waste products like creatinine and urea, showing how well the kidneys are working. Urine tests look for things like too much protein or blood, signs of kidney trouble.
Some biomarkers in blood and urine can tell us more about what’s going on. For example, certain proteins or enzymes in the blood might show kidney damage or disease.
- Serum creatinine levels help assess kidney function.
- Urine protein-to-creatinine ratio can indicate kidney damage.
- Blood urea nitrogen (BUN) levels can also reflect kidney function.
Biopsy Procedure and Interpretation
A kidney biopsy takes a small piece of kidney tissue for a closer look. This can give doctors clear answers about the disease.
The biopsy process includes:
- Preparation: Patients are told to stop certain medicines beforehand.
- Procedure: The biopsy is done under local anesthesia, guided by imaging to get the right sample.
- Post-procedure care: Patients are watched for any issues and given care instructions.
Looking at the biopsy results means checking the tissue for disease signs like inflammation or scarring. Pathologists use a microscope to examine the tissue. What they find helps decide how to treat the disease.
“Kidney biopsy remains the gold standard for diagnosing various kidney diseases, providing critical information that guides treatment strategies.”
— Expert in Nephrology
Treatment Approaches for Infiltrative Renal Neoplasms
Infiltrative renal neoplasms need a treatment plan that uses the latest in renal oncology. We will look at the different treatments available. We will see how they work and their benefits.
Surgical Management Options
Surgery is key in treating infiltrative renal neoplasms.
- Partial Nephrectomy: This method tries to keep the kidney working. It removes the tumor and a bit of tissue around it.
- Radical Nephrectomy: This involves taking out the whole kidney. It’s often used for bigger tumors or when the disease is more spread out.
Medical Therapies and Targeted Treatments
Medical treatments have improved a lot. They now target the specific traits of the tumor.
- Targeted Therapy: These drugs attack specific ways tumors grow and spread, like VEGF inhibitors.
- Immunotherapy: This uses the body’s immune system to fight cancer, including checkpoint inhibitors.
Emerging Therapies and Clinical Trials
The field of treating renal neoplasms is always changing. New treatments and clinical trials are being tested.
- CAR-T Cell Therapy: A type of immunotherapy that makes T cells attack cancer cells.
- Ongoing Research: Clinical trials are looking into new targets and treatments. They offer hope for the future.
Treating infiltrative renal neoplasms needs a detailed and personal approach. Knowing the treatments, like surgery, medical therapies, and new options, helps doctors give the best care to their patients.
End-Stage Kidney Disease Management
Managing end-stage kidney disease needs a detailed plan. This plan includes different treatments. A mix of treatments is key to better patient care.
Dialysis Modalities
Dialysis is a main treatment for end-stage kidney disease. There are two main dialysis modalities: hemodialysis and peritoneal dialysis.
Hemodialysis uses a machine to clean the blood outside the body. Patients often go to a dialysis center several times a week. This method works well but changes a lot of things in a patient’s life.
Peritoneal dialysis uses the lining of the abdomen to filter waste from the blood. It can be done by hand during the day or with a machine at night.
- Continuous Ambulatory Peritoneal Dialysis (CAPD): This involves manual exchanges throughout the day.
- Automated Peritoneal Dialysis (APD): This uses a machine to perform exchanges at night.
Kidney Transplantation Considerations
Kidney transplantation is another important treatment for end-stage kidney disease. It can lead to a more normal life, with fewer food limits and more freedom.
The kidney transplant process involves several steps. These include:
- Evaluating if a patient is a good candidate for a transplant. This looks at the patient’s health and if they match with a donor kidney.
- Finding a suitable donor, whether alive or deceased.
- Post-transplant care, which is very important for the transplant’s success.
Kidney transplantation has many benefits. But, it also comes with risks, like needing to take medicine for life to stop the body from rejecting the new kidney.
Managing end-stage kidney disease is complex. It requires looking at all treatment options carefully. By knowing about dialysis modalities and kidney transplantation considerations, patients and doctors can make better choices. This helps improve patient care.
Patient Monitoring and Follow-up Care
Keeping an eye on patients and following up is key for managing kidney diseases. We’ll talk about the need for surveillance and how to handle complications in kidney care.
Surveillance Protocols
Regular checks are vital to catch any disease changes or come-backs. Here are some key checks we suggest:
- Regular imaging studies (e.g., ultrasound, CT scans)
- Watching kidney function with serum creatinine and eGFR
- Urine tests for protein and blood
Managing Complications
Handling complications is a big part of caring for patients. Some common issues include:
- Chronic kidney disease getting worse
- Hypertension
- Electrolyte imbalances
We stress the need for quick action to lessen these problems. Acting fast can greatly help patients.
With a detailed plan for monitoring and follow-up, we can improve life for those with kidney diseases.
“Regular follow-up and monitoring are key to managing kidney disease and preventing complications.”
— Expert Opinion
Conclusion
We’ve looked into the details of infiltrative kidney diseases. This includes what they are, their types, and how they affect the kidneys. At Liv Hospital, we know how vital it is to offer complete care for these conditions.
Our team works together to make sure patients get the right diagnosis and treatment. We use the newest medical and surgical methods. We also focus on keeping an eye on patients and following up to handle any issues and improve their health.
Our goal is to make our patients’ lives better. We’re committed to top-notch healthcare. Our modern facilities and skilled team show our dedication to excellence.
In summary, treating infiltrative kidney diseases needs a detailed and tailored approach. At Liv Hospital, we’re all in on giving this kind of care. We aim to give our patients the best results possible.
FAQ
What is an infiltrative disease of the kidneys?
An infiltrative disease of the kidneys happens when abnormal cells or substances invade the kidney tissue. This invasion can harm the kidney’s structure and function. It can cause problems like chronic kidney disease and kidney cancer.
How do infiltrative kidney diseases affect kidney function?
These diseases can damage kidney tissue. This damage makes it hard for the kidneys to filter waste and excess fluids from the blood. As a result, toxins and electrolyte imbalances can build up, leading to complications.
What are the common types of renal neoplasms?
Renal neoplasms can be benign or malignant. The most common malignant type is renal cell carcinoma, with several subtypes. Benign types include cysts and adenomas.
What is the role of imaging techniques in diagnosing infiltrative kidney diseases?
Imaging techniques like ultrasound, CT scans, and MRI are key in diagnosing these diseases. They help spot renal masses, check for kidney damage, and guide biopsies.
What are the risk factors for developing infiltrative kidney diseases?
Risk factors include hypertension, diabetes, environmental exposures, and genetic predisposition. Lifestyle factors and certain medical conditions also play a role.
How is renal cell carcinoma diagnosed and treated?
Diagnosing renal cell carcinoma involves imaging, lab tests, and biopsies. Treatment options include surgery, medical therapies, targeted treatments, and emerging therapies like clinical trials.
What is the significance of chronic kidney disease as an infiltrative condition?
Chronic kidney disease is a progressive condition that can lead to end-stage kidney disease. It requires dialysis or a kidney transplant. It affects millions worldwide.
How are infiltrative kidney diseases monitored and managed?
Monitoring and follow-up care are key in managing these diseases. Surveillance and strategies for managing complications help prevent disease progression and improve outcomes.
What are the treatment options for end-stage kidney disease?
Treatment options include dialysis and kidney transplantation. The choice depends on the patient’s needs and medical considerations.
How can I find a doctor for infiltrative kidney diseases?
Liv Hospital offers advanced care for infiltrative kidney diseases. Our team of experts creates personalized treatment plans to improve patient outcomes.
References
- National Cancer Institute. (n.d.). Kidney & renal pelvis cancer (SEER Stat Facts). Retrieved from https://seer.cancer.gov/statfacts/html/kidrp.html
- Yirga, G. K., Aytenew, T. M., Kassaw, A., Hiruy, E. G., Shiferaw, K., Baye, A. A., Kerebeh, G., Mekonnen, G. B., Ewunetu, M., Amare, A. T., Birlie, T. A., Wassie, F. D., Diress, T., Abeje, G., Eshetie, Y., Abere, Y., & Bantie, B. (2025). Chronic kidney disease among patients with hypertension in sub-Saharan Africa: A systematic review and meta-analysis. BMC Public Health, 25(1), 1603. https://doi.org/10.1186/s12889-025-22828-8 (PMCID: PMC12044763) PMC+1
- U.S. Department of Defense. (n.d.). Kidney Cancer Research Program (KCRP) – Congressionally Directed Medical Research Programs. Retrieved from https://cdmrp.health.mil/kcrp/default
- (Authors). (2023). Title of article associated with PMC9646516. PMC. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9646516/
- Kidney Research UK. (2023). World Kidney Day 2023: Kidney disease statistics & facts. Retrieved from https://www.kidney.org.uk/news/wkd-2023-kidney-disease-statistics-and-facts
- Gill, D. (2023). The citrate transporter SLC13A5 as a therapeutic target for kidney disease: Evidence from Mendelian randomization to inform drug development. Cells, 12(6), Article 10729503. https://doi.org/10.3390/cells12069503 (PMCID: PMC10729503) PMC


































