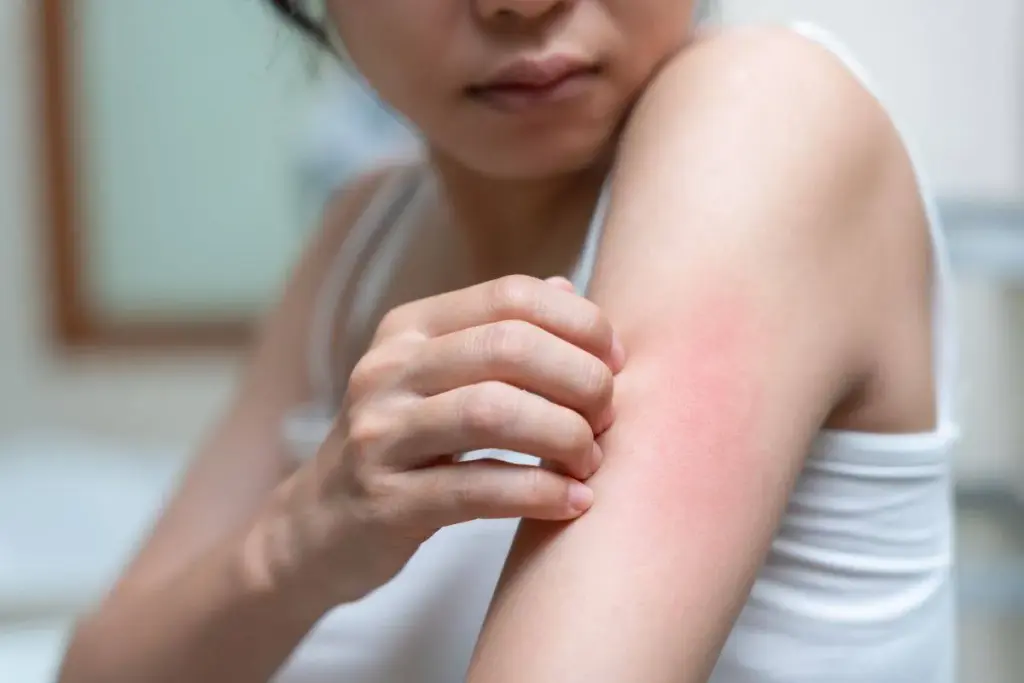
Autoimmune urticaria affects millions globally, causing discomfort and impacting daily life. We are here to help you understand this condition better. It is marked by itchy, raised welts on the skin, known as hives. Explaining the unique symptoms of autoimmune urticaria (hives) and how they differ from typical acute allergic reactions.
Symptoms of autoimmune urticaria vary by person. Common signs include itchy skin, rash, and swelling. Understanding these symptoms is key for effective management and treatment. We will look at the symptoms and discuss treatment options.
Key Takeaways
- Autoimmune urticaria is a condition characterized by itchy, raised welts on the skin.
- Common symptoms include itchy skin, rash, and swelling.
- Understanding the symptoms is critical for effective management.
- Various urticaria treatments are available to manage the condition.
- Autoimmune urticaria can significantly impact daily life.
Understanding Autoimmune Urticaria
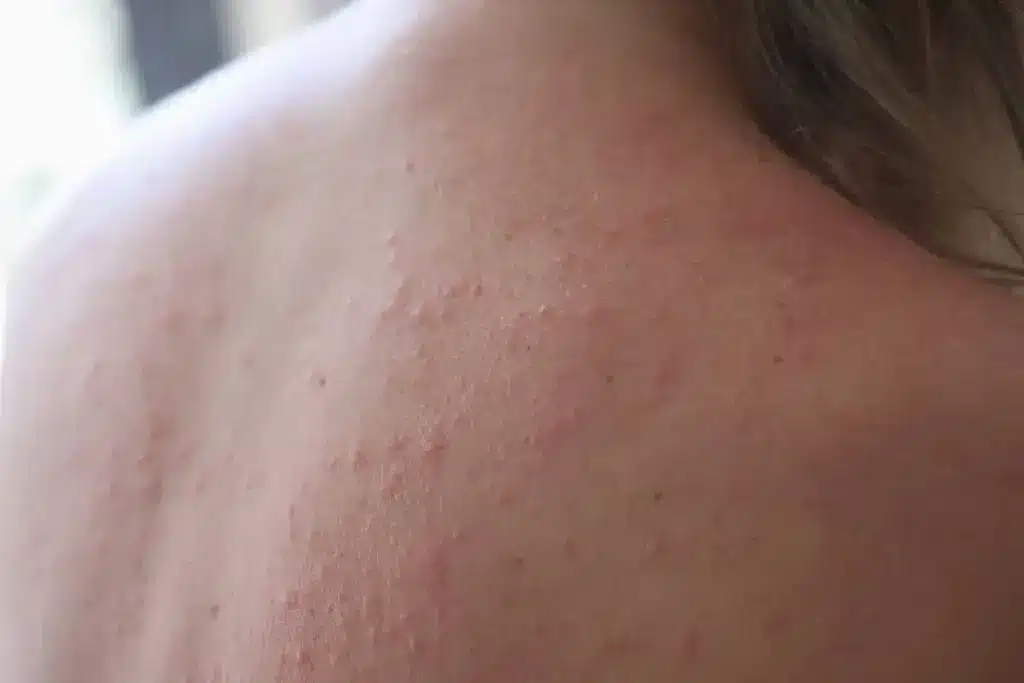
Autoimmune urticaria is when the immune system attacks the body’s own tissues. This leads to hives. It’s a complex issue.
Definition and Overview
Hives or wheals can show up anywhere on the body. They are itchy and can be different sizes.
If hives last more than six weeks, it’s called chronic. The causes are complex, mixing genetics and environment.
Causes and Triggers
Many things can set off or make autoimmune urticaria worse. These include:
- Genetic predisposition: If your family has autoimmune diseases, you’re at higher risk.
- Environmental factors like stress or infections.
- Certain medications that can make it worse.
Knowing what triggers it helps manage it better.
|
Cause/Trigger |
Description |
|---|---|
|
Genetic Predisposition |
People with a family history of autoimmune diseases are more likely to get it. |
|
Environmental Factors |
Stress, infections, and other things can trigger or make it worse. |
|
Certain Medications |
Some medicines can cause or make it worse. |
Common Symptoms of Hives

Hives can be very uncomfortable and disrupt our daily lives. When we have hives, we notice several symptoms. These symptoms affect our comfort and well-being.
Itchy Skin and Rash
One common symptom of hives is itchy skin, often with a rash. The itchiness can be mild or very severe. The rash can show up anywhere on the body and change shape or location.
- The itchiness can be intense, disrupting daily activities and sleep.
- The rash can manifest as raised, red patches or welts.
- Scratching the affected area can lead to further irritation.
Swelling and Redness
Along with itchy skin and rash, swelling and redness are common symptoms of hives. The skin may become inflamed, leading to swelling. This swelling can be uncomfortable and, in some cases, severe.
- Swelling can occur in the affected areas, sometimes causing the skin to become tender.
- Redness is a result of increased blood flow to the affected area, making the skin appear red or pink.
- In severe cases, swelling can affect the face, lips, tongue, or throat, potentially leading to more serious complications.
Understanding these symptoms is key to managing hives. By recognizing the signs of hives, we can take steps to alleviate discomfort. This helps prevent more serious complications.
Types of Autoimmune Urticaria
Autoimmune urticaria is divided into two main types. These are chronic spontaneous urticaria and chronic inducible urticaria. Each type has its own set of characteristics and treatment options.
Chronic Spontaneous Urticaria
Chronic spontaneous urticaria (CSU) causes wheals and angioedema without a known cause. It lasts more than six weeks. This condition is believed to be autoimmune.
CSU can really affect a person’s life. It’s hard to predict when symptoms will happen.
Key Features of CSU:
- Spontaneous onset of symptoms
- Duration of more than six weeks
- Involvement of autoimmune pathways
Chronic Inducible Urticaria
Chronic inducible urticaria (CIU) is caused by specific things like cold, heat, or pressure. Knowing what triggers it is key to managing it. We help patients find and avoid these triggers.
Triggers for CIU:
|
Trigger |
Description |
|---|---|
|
Cold |
Exposure to cold temperatures can induce urticaria symptoms. |
|
Heat |
Exposure to heat can trigger symptoms in some individuals. |
|
Pressure |
Physical pressure on the skin can lead to urticaria. |
By knowing the difference between CSU and CIU, we can treat each patient better. This helps improve their health outcomes.
Diagnosis of Autoimmune Urticaria
To diagnose autoimmune urticaria, doctors use a mix of medical history, physical check-ups, and special tests. This detailed method is key to understanding the condition and creating a good treatment plan.
Medical History and Physical Examination
Talking about your medical history is very important. We’ll ask about your symptoms, how long they’ve lasted, and what might make them better or worse. A physical examination will also be done to look at the hives and any other symptoms you have.
In the physical exam, we check the size, shape, and where the hives are. We also look for other skin signs. This helps us tell if it’s autoimmune urticaria or something else and guides us to more tests.
Skin Tests and Blood Tests
Skin tests and blood tests are key for diagnosing autoimmune urticaria. Skin tests find out what might be causing the hives. Blood tests look for autoantibodies that can cause hives.
An autologous serum skin test (ASST) might be done to find autoantibodies. Blood tests also check for other conditions that could cause similar symptoms. This ensures we get the right diagnosis.
By using your medical history, physical exam, and test results, we can accurately diagnose autoimmune urticaria. Then, we can create a treatment plan that works for you.
Treatment Options for Hives
For those with hives, knowing the treatment options is vital. The aim is to ease symptoms, cut down on outbreaks, and enhance life quality.
Antihistamines
Antihistamines are often the first choice for hives. They block histamine, a chemical that makes blood vessels swell. This leads to itching and redness. Here are some antihistamines to consider:
- Non-drowsy antihistamines such as loratadine or cetirizine, great for daytime use.
- Drowsy antihistamines like diphenhydramine, useful at night because they help you sleep.
Talking to a healthcare provider is key to finding the right antihistamine and dosage for you.
Corticosteroids
Corticosteroids are strong anti-inflammatory drugs for severe hives. They’re used when antihistamines don’t work. Here’s what you need to know about corticosteroids:
- Short-term use: They’re usually prescribed for a short time to avoid long-term side effects.
- Tapering off: It’s important to slowly stop taking corticosteroids to avoid side effects, with a doctor’s help.
Corticosteroids can offer a lot of relief, but it’s important to weigh the benefits against the risks. Always follow your doctor’s advice.
Lifestyle Changes to Manage Symptoms
To manage symptoms of autoimmune urticaria, we suggest several lifestyle changes. These changes can greatly reduce the discomfort of hives.
Dietary Adjustments
Diet is key in managing autoimmune urticaria. Some foods can trigger or worsen symptoms, while others can help. Keeping a food diary to track symptoms after eating certain foods is helpful.
Avoiding known allergens and foods high in histamine is a good start. This includes fermented foods, fish, and some cheeses. Eating a balanced diet with fruits, vegetables, and whole grains is also beneficial.
Stress Management Techniques
Stress can trigger autoimmune urticaria flare-ups. So, using stress management techniques is important. Meditation, yoga, and deep breathing exercises can lower stress levels.
Also, regular sleep, exercise, and relaxation techniques help manage stress. This, in turn, helps control hives symptoms.
By making these lifestyle changes, people with autoimmune urticaria can better manage their symptoms. This improves their overall quality of life.
When to Seek Medical Attention
People with autoimmune urticaria should know when to get medical help. This condition can sometimes get serious and need quick action from doctors.
Serious Symptoms to Watch For
Some symptoms mean you need to see a doctor right away. These include:
- Increasing severity of hives: If your hives get worse or don’t get better, you should see a doctor.
- Difficulty breathing: Though rare, it can happen if swelling blocks your airways.
- Abdominal cramps and diarrhea: Sometimes, it can cause stomach problems.
If you have these symptoms, talk to your doctor right away. They can help figure out what to do next.
Emergency Situations
Autoimmune urticaria can sometimes cause anaphylaxis, a very serious allergic reaction. You need to get help fast if you have symptoms like:
- Swelling of the face, lips, tongue, or throat: This can make it hard to breathe.
- Rapid heartbeat: A fast heart rate is a sign of a bad allergic reaction.
- Dizziness or fainting: Feeling dizzy or faint can mean your blood pressure is dropping.
|
Symptom |
Description |
Action Required |
|---|---|---|
|
Difficulty Breathing |
Swelling affecting the airways |
Seek immediate medical attention |
|
Abdominal Cramps and Diarrhea |
Gastrointestinal symptoms associated with autoimmune urticaria |
Consult a healthcare provider |
|
Anaphylaxis |
Life-threatening allergic reaction |
Call emergency services immediately |
If you’re in an emergency, don’t wait. Getting help fast can make a big difference.
Impact of Autoimmune Urticaria on Daily Life
Autoimmune urticaria is more than a skin issue; it deeply affects daily life and well-being. It’s tough to live with, impacting physical health, emotions, and mind. We see how it can change a person’s life.
Emotional and Psychological Effects
The unpredictable nature of autoimmune urticaria can cause emotional distress. Hives coming and going can lead to anxiety and stress. This affects mental health a lot.
People with chronic urticaria often face depression and anxiety. It’s key to tackle these emotional and psychological impacts. Healthcare support, family, and friends are vital. Counseling and stress management help a lot in dealing with these feelings.
|
Emotional Challenges |
Coping Strategies |
|---|---|
|
Anxiety and Stress |
Mindfulness and Meditation |
|
Depression |
Cognitive Behavioral Therapy (CBT) |
|
Social Isolation |
Support Groups |
Work and Social Life Challenges
Autoimmune urticaria affects work and social life a lot. Visible symptoms can make people feel embarrassed and self-conscious. They might avoid social events. At work, it can lower productivity due to discomfort or the need for medical visits.
Talking openly with employers and colleagues can help at work. Flexible hours or a private space can make a big difference. Teaching friends and family about the condition can also help. It creates a supportive environment and reduces feelings of isolation.
- Communicate openly with your employer about your needs.
- Utilize stress management techniques to improve well-being.
- Seek support from family, friends, and support groups.
Understanding the full impact of autoimmune urticaria helps us support those affected. It’s important to address physical symptoms and emotional, psychological, and social challenges. This way, we can help improve their lives.
Understanding Flare-Up Patterns
It’s important to know what causes flare-ups for those with autoimmune urticaria. By spotting patterns and triggers, we can find ways to control it better.
Seasonal and Environmental Influences
Seasonal changes and the environment play big roles in flare-ups. For example, hot weather or high humidity can make symptoms worse. Knowing these environmental factors is key to managing the condition.
Some people get more flare-ups in certain seasons. Spring and summer can bring pollen and heat, which might cause hives. On the other hand, cold weather in winter can also be a trigger for some. Being aware of these seasonal patterns helps prepare for flare-ups.
Identifying Personal Triggers
What triggers flare-ups can vary a lot among people with autoimmune urticaria. Common ones include certain foods, stress, and infections. Keeping a symptom diary helps find personal triggers. It lets people track when flare-ups happen and what might have caused them.
- Foods that can trigger hives include shellfish, nuts, and eggs.
- Stress management techniques, such as meditation or yoga, can help reduce flare-ups.
- Staying away from personal triggers can greatly improve life for those with autoimmune urticaria.
Understanding and managing flare-up patterns helps those with autoimmune urticaria live more predictable lives. We suggest working with healthcare providers to create a personalized plan for managing the condition.
Research and Future Directions
Studies and clinical trials are making progress in autoimmune urticaria treatment. Researchers are working hard to find better ways to help people with this condition.
Latest Findings in Autoimmune Urticaria
New studies have shed new light on how autoimmune urticaria works. They show how autoantibodies play a big role and how we might target them for treatment.
Thanks to advanced diagnostic tools, doctors can now diagnose autoimmune urticaria more accurately. This means they can create better treatment plans for their patients.
Potential New Treatments
There are promising new treatments on the horizon. These include biologics that aim to fix the immune system problems in autoimmune urticaria.
Also, scientists are studying the genetic underpinnings of the condition. This could lead to treatments that are tailored to each person’s genetic makeup.
Support and Resources
Living with autoimmune urticaria can be tough, but you’re not alone. We offer many support and resources to help you manage it.
Connecting with Others
Support groups and online communities are great places to share your story. You can ask questions and get support from people who get it. These groups offer both emotional support and practical advice.
Educational Resources and Advocacy
There are many educational resources like articles, videos, and webinars. They help you understand your condition better. Advocacy groups also work hard to raise awareness and fund research for new treatments.
By using these resources, you can take charge of your condition. This can greatly improve your life. We encourage you to explore these options and connect with others who face similar challenges.
FAQ
What is autoimmune urticaria?
Autoimmune urticaria is when your body attacks itself, causing hives. We’ll dive deeper into this condition in our article.
What are the common symptoms of hives?
Symptoms include itchy skin, rash, swelling, and redness. These can affect your daily life.
What causes autoimmune urticaria?
It’s caused by a mix of genetics, environment, and immune system factors. The exact reasons are not fully known.
How is autoimmune urticaria diagnosed?
Doctors use your medical history, physical exam, and tests like skin and blood tests. We’ll cover the details later.
What are the treatment options for hives?
Treatments include antihistamines and corticosteroids. These can help ease symptoms. We’ll look at these options closely.
Can lifestyle changes help manage symptoms of autoimmune urticaria?
Yes, changes like diet and stress management can help. We’ll offer tips on making these changes.
When should I seek medical attention for hives?
See a doctor for serious symptoms like breathing trouble or worsening symptoms. We’ll talk about when to act fast.
How does autoimmune urticaria impact daily life?
It can affect your mood, work, and social life. We’ll discuss these impacts in more detail.
What are the latest research findings in autoimmune urticaria?
New research is uncovering treatments and future directions. We’ll share the latest findings.
Where can I find support and resources for autoimmune urticaria?
There are support groups, online communities, and resources for help. We’ll provide information on where to find them.
How long do hives last?
Hives can last from a few hours to years. We’ll discuss the different types and their characteristics.
What is chronic spontaneous urticaria?
It’s a type of autoimmune urticaria with recurring hives without a clear cause. We’ll explore this condition further.
What is the role of antihistamines in treating hives?
Antihistamines are a common treatment for hives. They help with itching and swelling. We’ll discuss their use in more detail.
References
New England Journal of Medicine. Evidence-Based Medical Insight. Retrieved from https://www.nejm.org/doi/full/10.1056/NEJMra022319


































