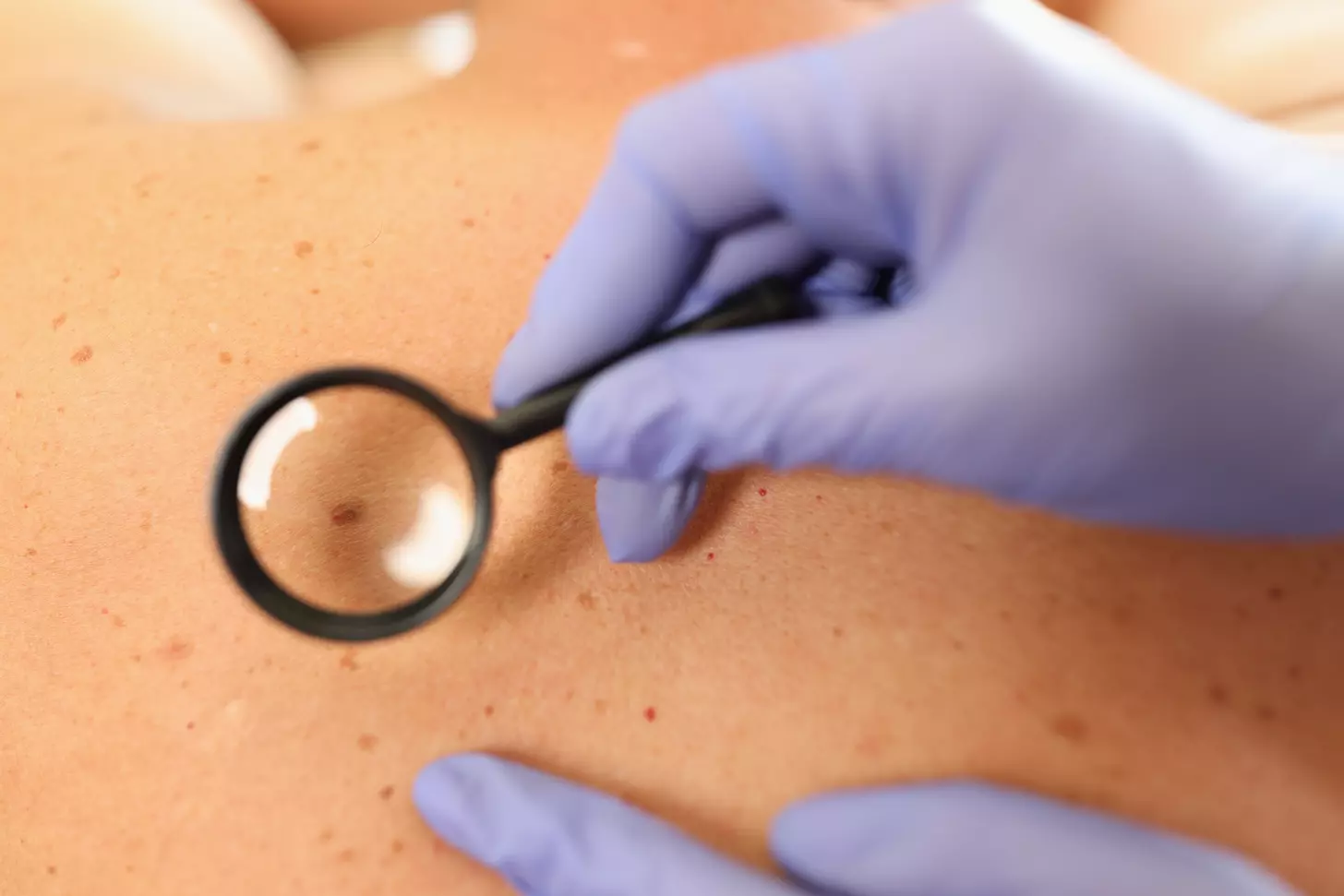
Stem cells can develop into many cell types and act as the body’s repair system. They replace or restore damaged tissues, offering new possibilities for treating diseases.
Send us all your questions or requests, and our expert team will assist you.
Bone Marrow Failure is a serious and complex condition in blood medicine. It is not just one disease, but a group of problems where the bone marrow stops or greatly reduces making blood cells. To understand how serious this is, it helps to know how healthy bone marrow works. Found inside the bones, bone marrow is a busy organ, as important as the liver or kidneys. It is the main place where the body makes cells for the immune system and for carrying oxygen.
Hematopoietic stem cells are at the heart of blood cell production. These rare cells can make copies of themselves to keep their numbers up and can also turn into different types of mature blood cells. These include red blood cells for carrying oxygen, white blood cells for fighting infection, and platelets for blood clotting. When bone marrow fails, this whole process breaks down. The marrow, which is usually full of developing cells, becomes empty. A biopsy shows that the active tissue is replaced by fat cells and support tissue.
The clinical manifestation of this cellular void is pancytopenia, a dangerous scarcity of all three major blood cell types. The physiological consequences are systemic and severe. The lack of red blood cells leads to profound anemia, manifesting as exhaustion, dyspnea, and cardiac strain. The absence of white blood cells, particularly neutrophils, strips the body of its primary defense against bacteria and fungi, turning mundane environmental exposures into lethal threats. The deficiency of platelets results in a hemorrhagic state, ranging from cutaneous bruising to catastrophic intracranial bleeding.

Bone marrow failure usually happens in two main ways: it can be acquired during life or inherited from birth. Knowing which type a patient has is key to choosing the right treatment.

The medical history of Bone Marrow Failure is a narrative of evolving understanding, moving from fatalism to curative intervention. The condition was first vividly described in the late 19th century by Paul Ehrlich, who noted a rapidly fatal condition in a young woman characterized by anemia and bleeding. For decades, the diagnosis was synonymous with a terminal prognosis, with treatment limited to palliative blood transfusions that could only prolong life briefly.
In the mid-1900s, doctors realized that bone marrow could regenerate. This led E. Donnall Thomas and others to develop bone marrow transplants. They showed that giving healthy marrow from a donor could fill the patient’s empty marrow and restore blood cell production. This was the first time stem cell therapy worked in people.
At the same time, doctors found that some patients got better after taking medicines that suppress the immune system. This proved that acquired aplastic anemia is often caused by the immune system attacking the marrow. Now, treatments focus on either stopping this attack or replacing the marrow. New research in gene therapy and molecular biology is bringing hope for even more cures in the future.
Bone marrow failure happens more often in some parts of the world. For example, aplastic anemia is two to three times more common in Asian countries like Thailand and China than in Western countries. While genes matter, researchers have also looked at environmental causes. In the past, many cases were seen in workers exposed to benzene, a chemical used in factories, showing that certain toxins can damage stem cells.
Today, scientists are still studying other possible causes, such as pesticides, certain viruses like hepatitis, and rare drug reactions. Knowing what triggered the disease can help doctors plan treatment and prevent future cases. Because bone marrow failure affects people worldwide, doctors work together internationally to improve treatments and survival rates.

Cancer develops through the interaction of multiple factors including genetics, lifestyle, age and environmental exposures. Because every person has a unique risk profile, our specialists at Liv Hospital take time to evaluate these elements individually. We guide patients toward healthier lifestyle choices, early screening methods and practical preventive strategies. By transforming knowledge into action, we help you take meaningful steps toward protecting your long term health and well being.
At Liv Hospital, we believe that empowerment begins with understanding. While cancer is a complex disease with no single cause, our knowledge of contributing risk factors is constantly growing. We recognize that a combination of factors from genetic predispositions to lifestyle choices and environmental influences plays a role in its development. Our approach is proactive and personalized. The dedicated experts at Liv Hospital work with you to assess your individual risk profile and provide compassionate, practical guidance on lifestyle modifications. We partner with you to transform awareness into action, helping you take meaningful steps to safeguard your long-term health and well-being.
Send us all your questions or requests, and our expert team will assist you.
Pancytopenia is a medical term for a condition in which a patient has low counts of all three major blood cell types: red blood cells, white blood cells, and platelets. It is the hallmark finding in bone marrow failure, indicating that the production line for all blood elements has shut down.
Bone marrow failure itself, such as aplastic anemia, is not cancer. It is a deficiency disorder where cells are missing. However, because the remaining stem cells are under stress, there is a risk that they will mutate over time and evolve into blood cancers such as Myelodysplastic Syndrome (MDS) or Acute Myeloid Leukemia (AML).
Yes, viral infections are known triggers of acquired bone marrow failure. Viruses such as Epstein-Barr Virus (EBV), Cytomegalovirus (CMV), HIV, and certain hepatitis viruses can trigger the immune system to attack the bone marrow. Parvovirus B19 specifically attacks red blood cell precursors, causing a temporary failure known as pure red cell aplasia.
When hematopoietic stem cells die or are destroyed, the space in the bone marrow cavity is filled by adipocytes, or fat cells. This is the body’s way of filling the vacuum. On a biopsy, a yellow, fatty marrow is the classic visual sign of aplastic anemia, distinguishing it from a red, cellular marrow.
Quantitative failure, like aplastic anemia, means there are not enough stem cells; the factory is empty. Qualitative failure, like Myelodysplastic Syndrome, means the marrow is full of cells that are defective, misshapen, and do not function properly, often dying before they reach the bloodstream.

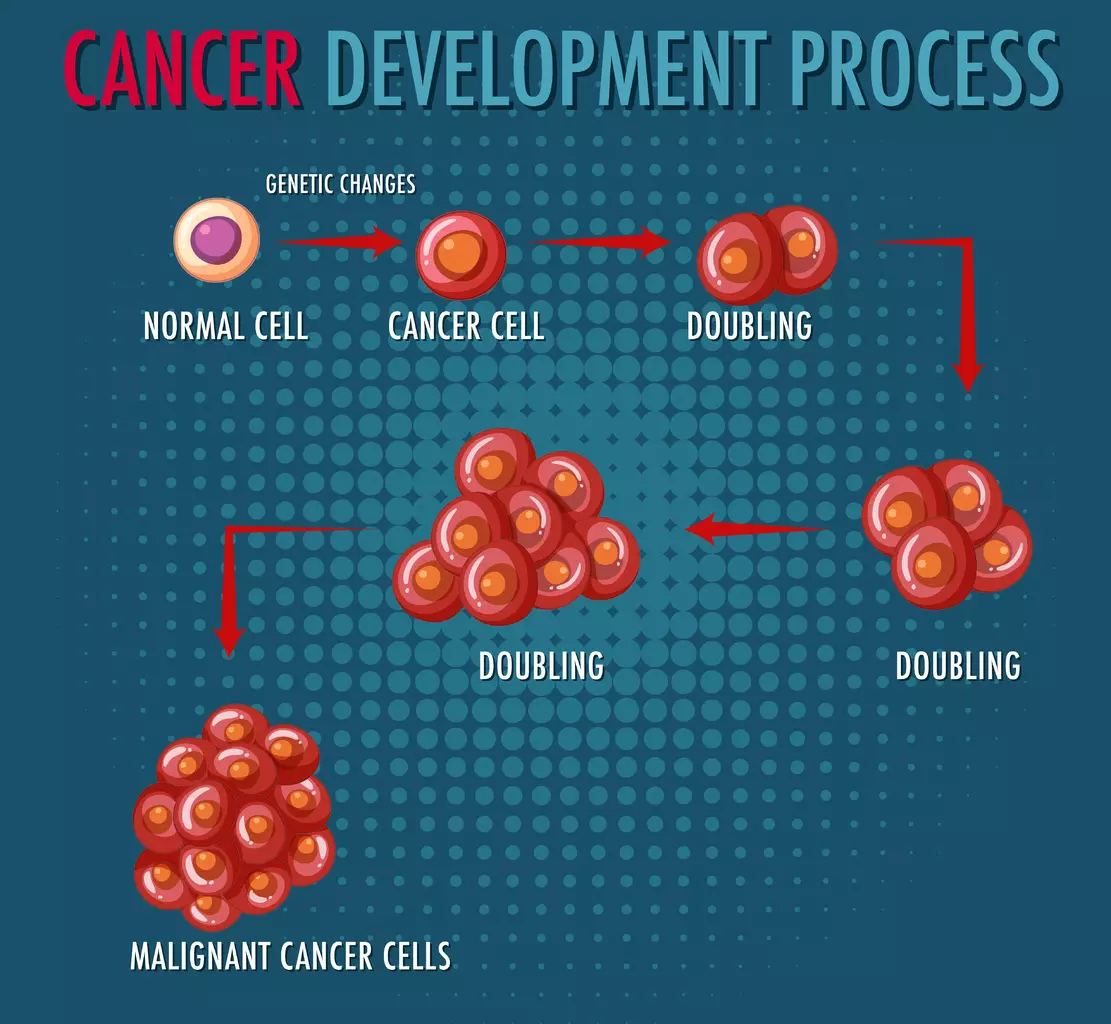

PET scan necessity seriousness is highlighted by the fact that nearly 1.9 million new cancer cases are expected in the United States this year, underscoring
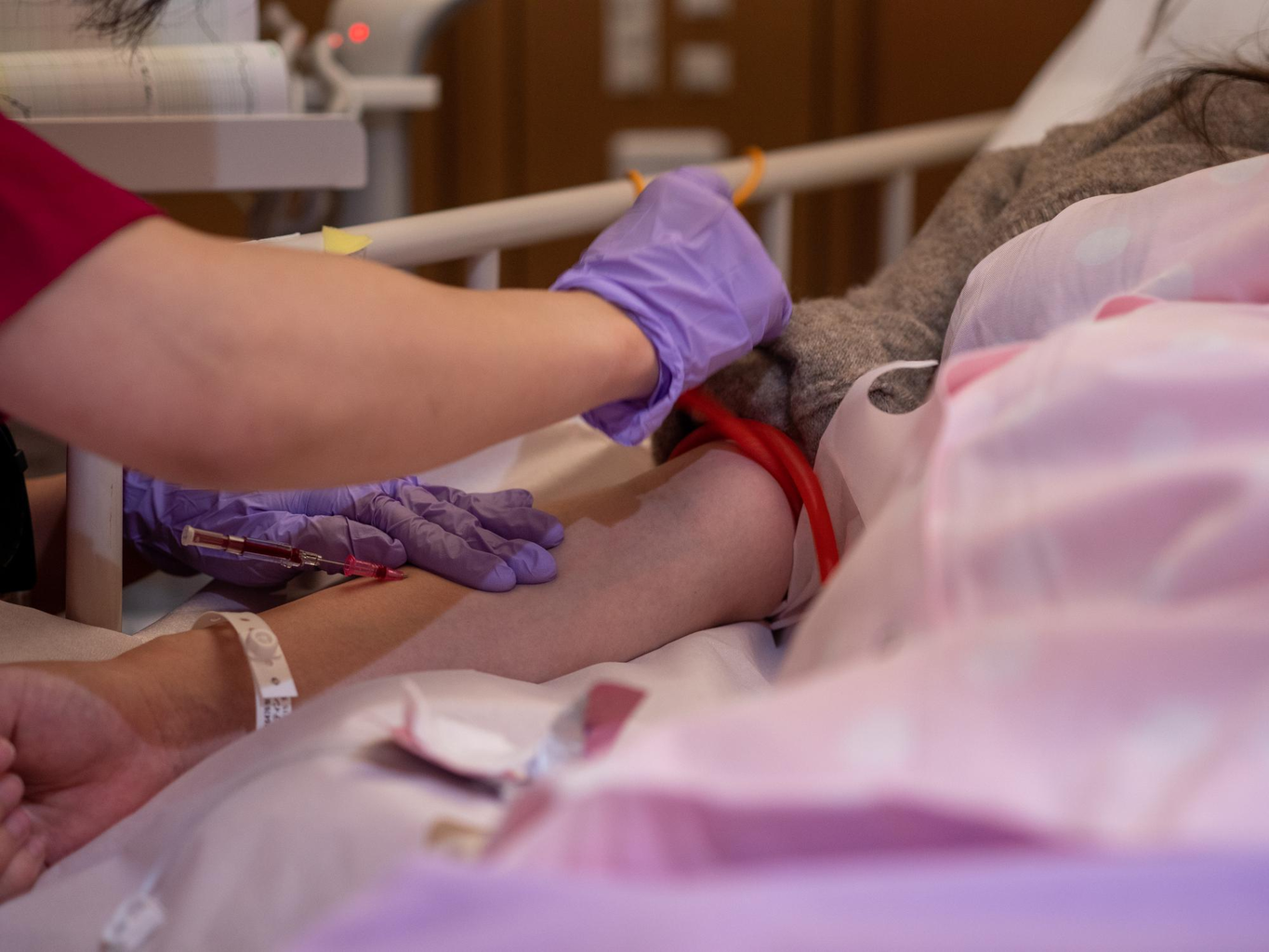

Bone marrow disease affects thousands worldwide by impairing the body’s ability to produce healthy blood cells. Studies show that genetic mutations, environmental exposures, and infections