Understand the complexities of bone marrow failure. Learn what Myelodysplastic Syndrome is, how it affects blood production, and the hematologists who treat it at Liv Hospital.
Send us all your questions or requests, and our expert team will assist you.
Overview and Definition
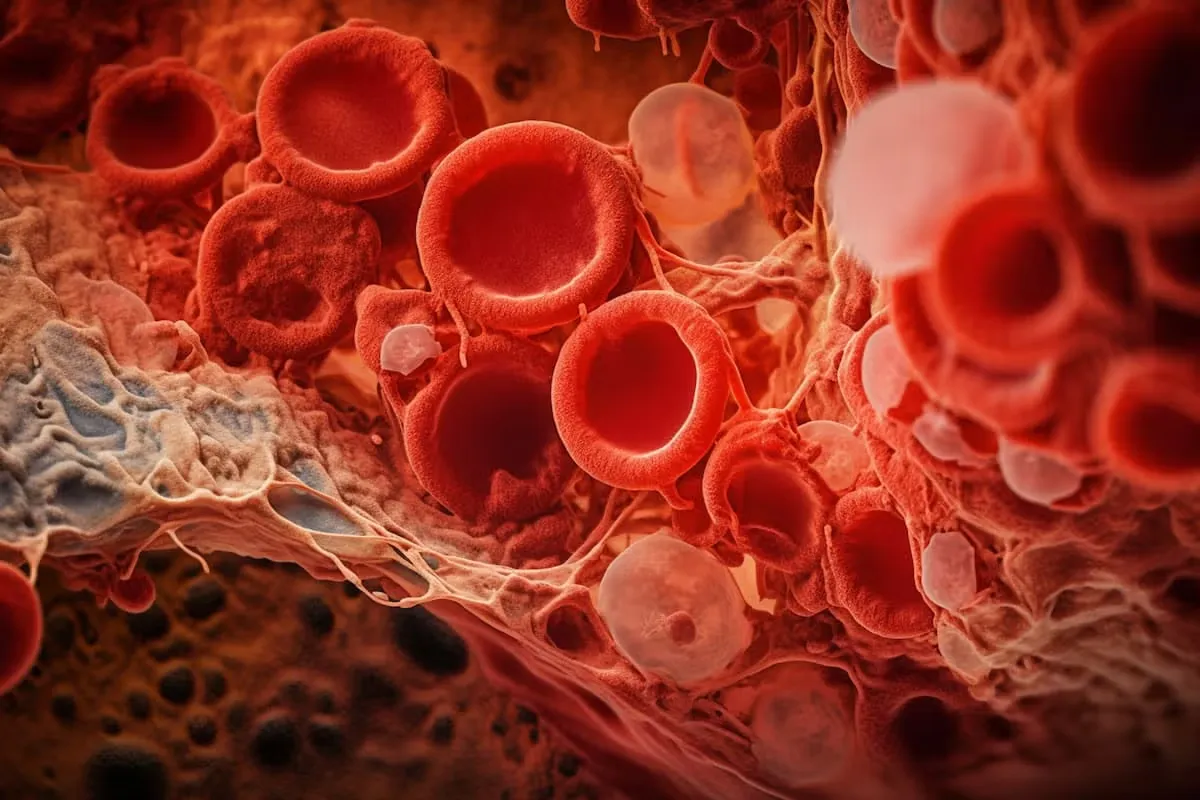
To understand Myelodysplastic Syndrome (MDS), it helps to understand how healthy bone marrow functions. The bone marrow is the soft, spongy tissue inside your bones that acts as a factory for blood cells. In a healthy person, stem cells in the marrow mature into three types of blood cells:
In MDS, this factory malfunctions. The stem cells become damaged (mutated) and begin producing “blasts” of immature blood cells that are misshapen or dysfunctional (dysplastic). Because these cells are defective, the body destroys many of them before they can leave the bone marrow. This results in “cytopenias,” or low blood counts, which is the hallmark of the disease.
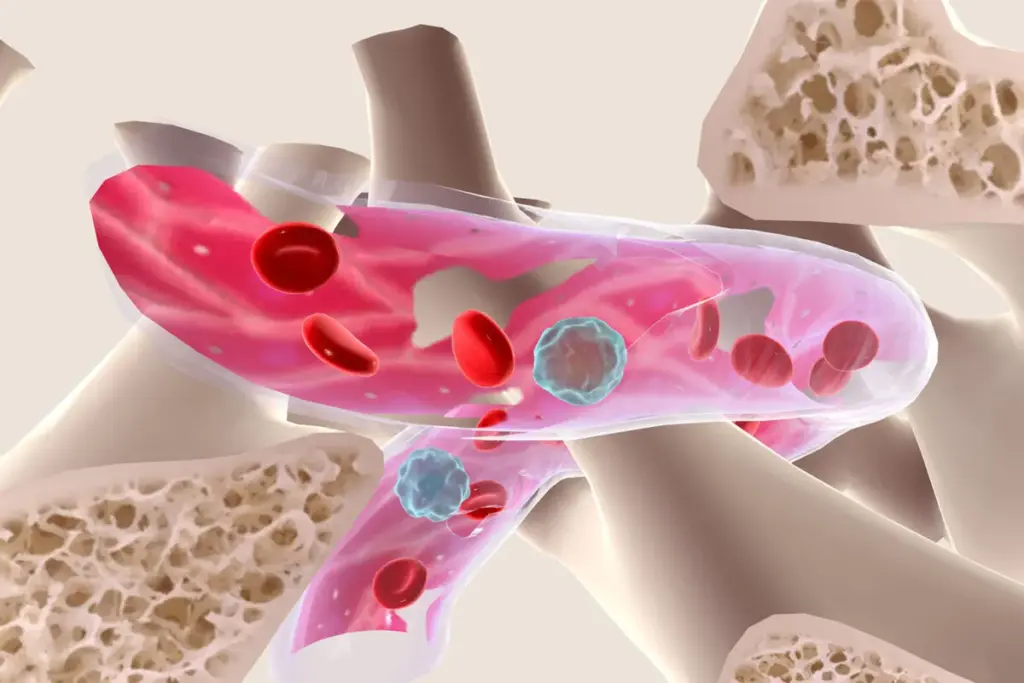
The impact of MDS on the body is directly related to which type of blood cell is lacking. The severity of symptoms often correlates with how low the blood counts have dropped.
As the disease progresses, the bone marrow may become overcrowded with these immature blasts, leaving no room for healthy cells to grow. This “crowding out” effect is what eventually leads to bone marrow failure.

In the past, Myelodysplastic Syndrome was frequently called “pre-leukemia” or “smoldering leukemia.” While these terms are less common today, they highlight a significant risk associated with the disease.
MDS has the potential to transform into Acute Myeloid Leukemia (AML), a rapid-growing cancer of the blood and bone marrow. This transformation occurs when the number of immature blast cells in the marrow rises above 20%.
However, it is important to note that not all MDS patients will develop leukemia. Approximately 30% of MDS cases progress to AML. For the majority of patients, the primary challenge is managing the complications of bone marrow failure (anemia and infection) rather than leukemia itself. Assessing this risk is a critical part of the initial evaluation at Liv Hospital.
Conditions and Indications
MDS often develops silently. In the early stages, many patients show no symptoms and are diagnosed only after routine blood tests reveal low cell counts. As bone marrow failure progresses, the lack of healthy cells leads to specific indications. Symptoms are directly related to which type of blood cell is low (red cells, white cells, or platelets).
Recognizing these signs early is crucial. If left untreated, conditions can lead to severe complications, such as heart strain from anemia or life-threatening infections due to a lack of white blood cells.
Red blood cells are the body’s oxygen carriers. They contain hemoglobin, which binds oxygen in the lungs and delivers it to tissues throughout the body. In the context of MDS, red blood cells are the most frequently affected cell line. When the marrow produces defective red cells, they are often destroyed before leaving the bone marrow or die prematurely in the bloodstream.
When red blood cell production fails, a person develops anemia. This leads to symptoms such as persistent fatigue, shortness of breath during mild exertion, pale skin, and heart palpitations. The heart must work harder to pump oxygen-poor blood, which can lead to heart strain over time. Managing this deficiency often requires regular blood transfusions or medications that stimulate the marrow to work harder.
White blood cells act as the body’s defense system. They are responsible for identifying and destroying bacteria, viruses, and fungi. Neutrophils are a specific type of white blood cell crucial for fighting bacterial infections. In MDS, the maturation of these cells is often blocked or disordered.
Dysfunction in white blood cell production leads to neutropenia. This is a critical condition because it removes the body’s primary barrier against infection. Patients may experience frequent fevers, recurrent sinus or lung infections, or skin infections that do not heal. Unlike anemia, which causes fatigue, neutropenia can be life-threatening if a severe infection develops rapidly. Protective measures and antibiotics are key parts of managing this aspect of the disease.
Diagnosis and Evaluation

Diagnosing MDS requires more than a standard blood test. While a Complete Blood Count (CBC) provides the first clue by revealing low blood counts, confirming the diagnosis requires looking directly at the source. The gold standard for evaluation is a bone marrow aspiration and biopsy.
During this evaluation, pathologists look for “dysplasia” abnormalities in the shape and size of the cells and count the percentage of immature “blast” cells. Genetic testing (cytogenetics) is also performed to look for chromosomal changes. This evaluation is critical for risk stratification, which helps doctors determine if the disease is low-risk (slow-growing) or high-risk (aggressive), ultimately guiding the treatment strategy.
MDS is not a single disease but a collection of related disorders. Doctors classify MDS based on how the cells look under a microscope and which genetic mutations are present. The World Health Organization (WHO) has updated these classifications to be more precise:
Treatment and Procedures
The treatment for Myelodysplastic Syndrome (MDS) varies from supportive care to curative interventions. For lower-risk patients, the focus is on active surveillance and symptom management, utilizing growth factor medications and blood transfusions. In contrast, higher-risk patients require more aggressive treatments.
Advanced therapies include hypomethylating agents that help restore bone marrow function. However, Allogeneic Stem Cell Transplantation remains the only potential cure for eligible patients, involving the replacement of defective bone marrow with healthy stem cells from a donor. At Liv Hospital, our multidisciplinary team assesses each patient to identify the most effective treatment plan.
Stem cells are the foundational cells of the bone marrow, capable of self-renewal and differentiation into various blood cells. In MDS, mutations in stem cells give them a survival advantage but hinder their ability to produce healthy cells. This leads to a predominance of defective stem cells in the marrow. Consequently, blood transfusions alone are insufficient; the only potential cure involves replacing these defective stem cells through Allogeneic Stem Cell Transplantation.
Recovery and Follow-up
MDS is typically a chronic condition that requires lifelong monitoring. Recovery looks different for every patient. For those undergoing stem cell transplantation, recovery is a gradual process involving immune system reconstitution and close monitoring for graft-versus-host disease. For those on maintenance therapy, it involves regular clinic visits to monitor blood counts and adjust medications.
Follow-up care focuses on maintaining quality of life, managing side effects of treatment, and preventing complications like iron overload from frequent transfusions. Regular bone marrow assessments are also standard to ensure the disease has not progressed to acute leukemia. A comprehensive follow-up plan ensures that patients remain stable and supported throughout their journey.
MDS can affect people of all backgrounds, but it is predominantly a disease of older adults. The median age of diagnosis is around 70 years old, and it is rare in people under 50. Men are slightly more likely to develop the condition than women.
Genetic factors and environmental history play a role. While most cases are not inherited, people with certain genetic syndromes (like Fanconi anemia) are at higher risk. Additionally, those who have worked in industries with heavy chemical exposure or who are cancer survivors are specific demographics that monitor for this condition. The burden of MDS is significant because symptoms like fatigue are often dismissed as “just getting older,” leading to delayed diagnosis.
It is important to distinguish between primary and secondary Myelodysplastic Syndromes. Primary MDS, also known as de novo MDS, occurs without a known cause. It is generally associated with aging and the random genetic mutations that accumulate in stem cells over time. This is the most common form of the disease.
Secondary MDS, or treatment-related MDS, occurs as a result of previous exposure to chemotherapy or radiation therapy used to treat a different cancer. It can also be caused by long-term exposure to toxic chemicals like benzene. Secondary MDS is generally more aggressive and harder to treat than primary MDS. Understanding the origin of the disease is vital for the medical team at Liv Hospital to formulate a realistic and effective treatment plan.
It is important to distinguish between primary and secondary Myelodysplastic Syndromes. Primary MDS, also known as de novo MDS, occurs without a known cause. It is generally associated with aging and the random genetic mutations that accumulate in stem cells over time. This is the most common form of the disease.
Secondary MDS, or treatment-related MDS, occurs as a result of previous exposure to chemotherapy or radiation therapy used to treat a different cancer. It can also be caused by long-term exposure to toxic chemicals like benzene. Secondary MDS is generally more aggressive and harder to treat than primary MDS. Understanding the origin of the disease is vital for the medical team at Liv Hospital to formulate a realistic and effective treatment plan.
Because MDS is a complex cancer that affects the entire blood system, management requires high-level expertise. A general practitioner may not have access to the advanced genetic testing required for accurate risk stratification. A patient might receive transfusions for anemia without addressing the underlying progression of the disease.
A center dedicated to hematologic malignancies, like Liv Hospital, utilizes a multidisciplinary tumor board. This includes hematologists, pathologists, and transplant specialists who review the case together. They understand the timing of when to watch and wait versus when to proceed to transplant. Specialized care ensures that the treatment plan balances the aggressiveness of the disease with the patient’s overall health and quality of life.

Send us all your questions or requests, and our expert team will assist you.
The exact cause is often unknown but it results from acquired genetic mutations in bone marrow stem cells that accumulate with age or exposure to toxins.
Yes the World Health Organization classifies MDS as a form of blood cancer because it involves the uncontrolled growth of abnormal cells.
The only potential cure is a stem cell transplant from a healthy donor but this is an intensive procedure not suitable for every patient.
No MDS is not a contagious disease it is caused by internal genetic changes and cannot be passed to others.
MDS is characterized by fewer than 20% blast cells in the marrow while acute leukemia is defined by having 20% or more blast cells.

 Myelodysplastic Syndrome
Myelodysplastic Syndrome Myelodysplastic Syndrome
Myelodysplastic Syndrome Myelodysplastic Syndrome
Myelodysplastic Syndrome Myelodysplastic Syndrome
Myelodysplastic Syndrome Myelodysplastic Syndrome
Myelodysplastic Syndrome
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)