Recognize Myelofibrosis symptoms early: Splenomegaly (enlarged spleen), night sweats, bone pain, and fatigue. Learn the warning signs and when to see a doctor.
Send us all your questions or requests, and our expert team will assist you.
Conditions and Indications
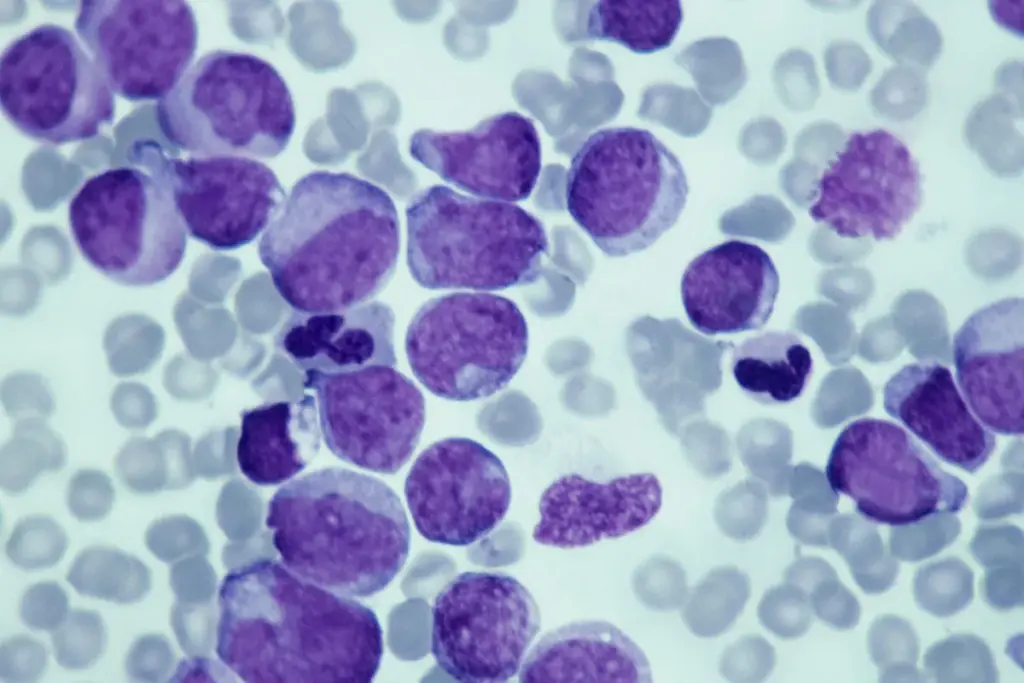
Recognizing the signs of Myelofibrosis can be challenging because the disease often begins silently. Many patients feel “off” for months or even years before a diagnosis is made, attributing their fatigue to aging or stress. However, as the bone marrow becomes increasingly scarred, the body sends specific distress signals. Understanding these conditions and indications is the critical first step toward getting the right help.
At Liv Hospital, we believe that an informed patient is an empowered patient. Whether you are noticing the first subtle changes in your energy levels or are managing profound physical symptoms like an enlarged spleen, recognizing these patterns is essential. Our Hematology and Bone Marrow Transplant Center specializes in interpreting these signals, using them not just to diagnose, but to stratify your risk and tailor a treatment plan that fits your specific needs.
As Myelofibrosis progresses, it creates a state of chronic inflammation in the body. This leads to a specific group of indications known as constitutional symptoms. These are systemic issues that affect your whole body, not just your blood.
Doctors often use the presence of these symptoms to grade the severity of the disease:
Myelofibrosis can lead to complications that require urgent medical attention. Being aware of these advanced indications can help you seek emergency care when needed.

Myelofibrosis is a progressive disease, meaning it worsens over time. In the earliest phase, often called the pre-fibrotic stage, the bone marrow changes are microscopic, and you may not feel sick at all.
In fact, nearly 30% of patients are asymptomatic at the time of diagnosis. For these individuals, the condition is usually discovered accidentally during a routine annual physical or a blood test for another issue.
Common incidental findings that trigger a referral to a hematologist include:
If your blood work shows these irregularities without an infection or clear cause, it is a primary indication to investigate further.
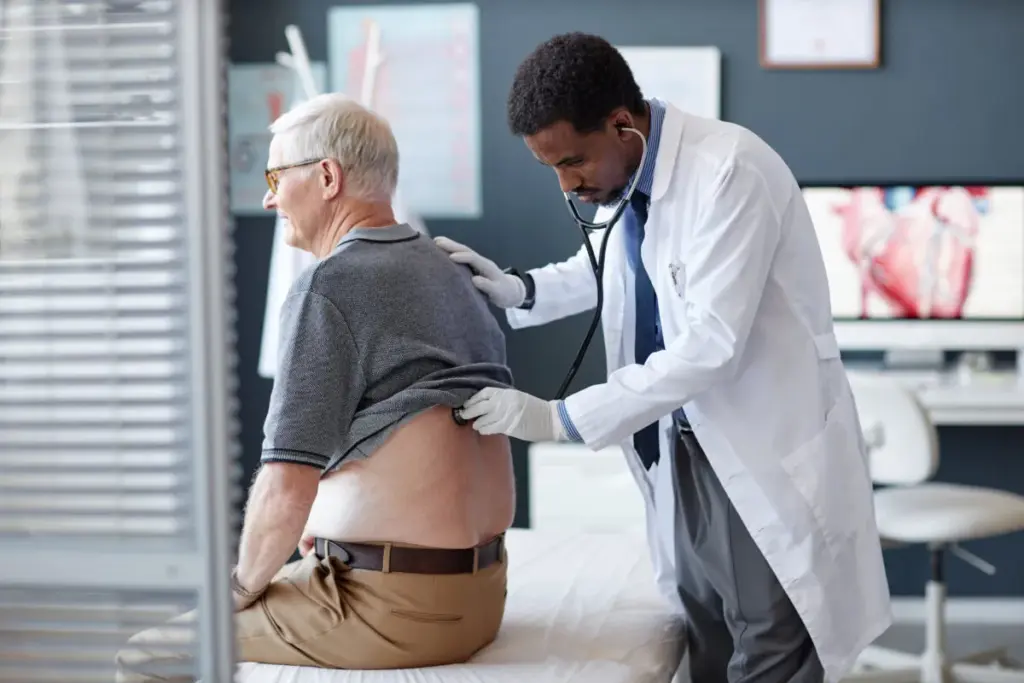
The most distinct and often the most uncomfortable indication of Myelofibrosis is splenomegaly (an enlarged spleen). Because the scarred bone marrow cannot produce enough blood cells, the spleen attempts to take over this job (extramedullary hematopoiesis).
A healthy spleen is about the size of a fist and is tucked safely inside the rib cage. In Myelofibrosis, it can grow to the size of a football or larger, extending down into the pelvis.
Symptoms of an enlarged spleen include:
Managing spleen size is a primary goal of treatment at Liv Hospital, as it directly impacts your daily comfort and nutrition.

Send us all your questions or requests, and our expert team will assist you.
While the disease is caused by genetic mutations, certain factors increase the likelihood of developing these mutations. Understanding your risk profile is essential for early screening.
Key Risk Factors:
At Liv Hospital, we don’t just ask “Do you have Myelofibrosis?”; we ask “Which risk category are you in?” We use the DIPSS Plus (Dynamic International Prognostic Scoring System) to categorize patients.
Your risk score is calculated based on:
Why does this matter?
Knowing your score is the single most important factor in deciding whether to travel for treatment.
If you have been diagnosed with an MPN (like PV or ET) and notice a change in your symptoms such as new fatigue or an enlarging spleen it is time for a re-evaluation.
Liv Hospital offers a comprehensive “Myelofibrosis Risk Assessment” package for international patients. This includes verifying your diagnosis with our advanced pathology review and providing a second opinion on your transplant eligibility.
You should consult a specialist if:
It is often described as a deep, dull ache or throbbing sensation in the long bones of the legs, the ribs, or the back. It differs from arthritis pain because it is not located specifically in the joints but rather in the bone itself.
This is called “aquagenic pruritus.” It is caused by the release of histamines and other chemicals from abnormal blood cells (mast cells/basophils) triggered by the change in temperature. It is a classic sign of MPNs.
Yes. It can be mistaken for other autoimmune disorders, metastatic cancer, or other blood diseases. A bone marrow biopsy with specific staining for fibrosis is required to confirm the diagnosis and rule out mimics.
During a bone marrow aspiration, the doctor inserts a needle to pull out liquid marrow. Because Myelofibrosis causes scarring, the marrow becomes solid and no liquid comes out. This “dry tap” is a strong indication of fibrosis.
No. In modern medicine, we rarely remove the spleen (splenectomy) as a first option because of the risks. We prefer to use medications (JAK inhibitors) or radiation to shrink it first. Splenectomy is reserved for severe cases where drugs fail.

 Orthopedics
Orthopedics Geriatrics
Geriatrics Ear Nose Throat
Ear Nose Throat Interventional Radiology
Interventional Radiology Ear Nose Throat
Ear Nose Throat Rheumatology
Rheumatology
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)