Thalassemia is a serious genetic disorder that affects how red blood cells carry oxygen. It’s important to know if thalassemia is inherited, mainly for families with a history of it. We’ll look into the genetic roots of this condition and how it’s passed down.
This condition is an autosomal recessive disorder. This means both parents must carry the gene for a child to have the major form. The says over 200 mutations can cause thalassemias. This shows how complex its genetics are.
Key Takeaways
- Thalassemia is a genetic disorder affecting hemoglobin production.
- It is inherited in an autosomal recessive pattern.
- Both parents must be carriers to pass the major form to their child.
- The condition leads to anemia and other complications.
- Understanding its hereditary nature can guide prevention and treatment.
What Is Thalassemia?
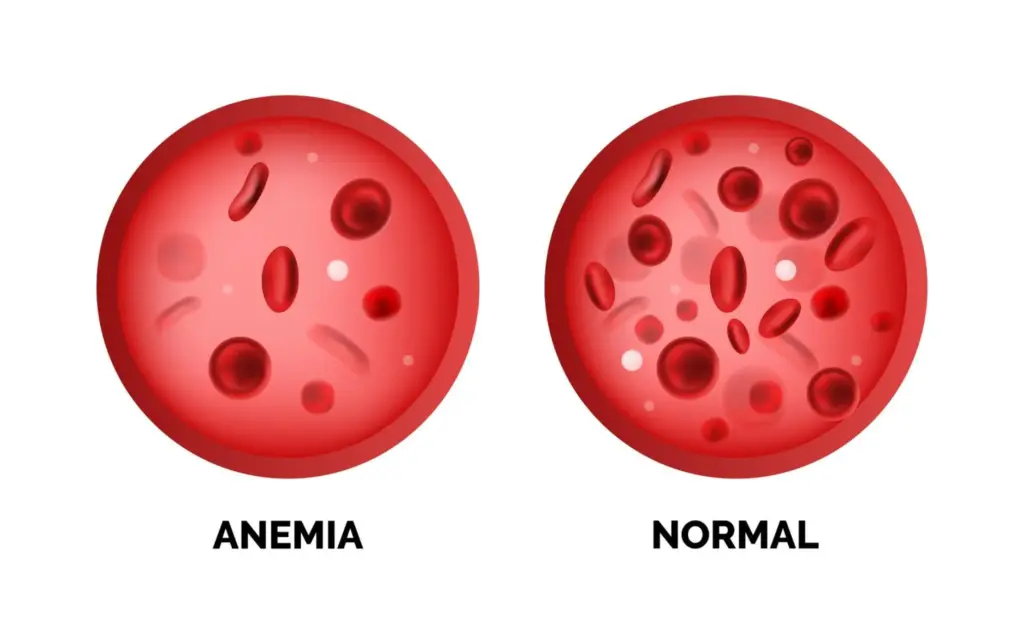
Thalassemia is a genetic disorder that affects the production of hemoglobin, the essential protein responsible for carrying oxygen in red blood cells. This disorder impacts the production of globin chains, leading to anemia and other health issues.
Definition and Classification
Thalassemia is a group of genetic disorders that affect hemoglobin production. It causes anemia and other complications. It’s mainly divided into alpha and beta thalassemia, based on the globin chain affected.
The severity of thalassemia depends on the genes affected and the genetic mutation. Alpha thalassemia happens with mutations in alpha-globin genes. Beta thalassemia results from mutations in beta-globin genes.
Key classification aspects include:
- Type of globin chain affected (alpha or beta)
- Number of genes affected
- Severity of the disorder
Historical Background
Thalassemia has been known for centuries, mainly in the Mediterranean. It was first described in the early 20th century. Progress has been made in understanding its genetics and symptoms.
Historically, thalassemia was often fatal. But, with better medical care, like blood transfusions and iron chelationtherapy, outcomes have improved.
Global Impact
Thalassemia is a big public health issue in many places, like the Mediterranean, Middle East, and Southeast Asia. It’s linked to malaria, as thalassemia carriers have an advantage against it.
Millions of people worldwide are carriers or have thalassemia. Efforts to manage it include screening, genetic counseling, and prenatal diagnosis to prevent severe cases.
Key global statistics include:
- Prevalence in specific regions: high in Mediterranean, Middle East, and Southeast Asia
- Number of carriers and affected individuals: millions worldwide
- Public health initiatives: screening, genetic counseling, prenatal diagnosis
The Genetic Foundation of Thalassemia

Thalassemia is a genetic disorder that affects how the body makes hemoglobin. Hemoglobin is a protein in red blood cells that carries oxygen. It’s vital for our bodies to function well.
Hemoglobin Structure and Function
Hemoglobin is made of four chains: two alpha-globin and two beta-globin. Its structure is key to its job. It binds oxygen in the lungs and releases it to our tissues. The way these chains are arranged is vital for hemoglobin to work right.
Our DNA holds the blueprint for these chains. Any changes in these genes can cause problems with hemoglobin. This can lead to thalassemia.
How Genetic Mutations Affect Hemoglobin
Thalassemia is caused by mutations in the genes for globin chains. For example, beta-thalassemia comes from mutations in beta-globin genes. Alpha-thalassemia is caused by mutations in alpha-globin genes. The severity of thalassemia depends on how much the mutation affects globin chain production.
These mutations can be point mutations, deletions, or insertions. Where and what type of mutation it is determines how severe thalassemia will be.
The Role of Globin Chains
Globin chains are the foundation of hemoglobin. The right balance between alpha and beta chains is essential. In thalassemia, this balance is off because of mutations. This imbalance harms red blood cells, causing them to break down early and leading to thalassemia symptoms.
Knowing how globin chains work and how mutations affect them is important. Research into thalassemia’s genetics is ongoing. It may lead to new treatments and therapies.
Thalassemia as an Inherited Blood Disorder
Thalassemia is a blood disorder passed down through generations. It follows an autosomal recessive pattern. This means a person needs two defective genes, one from each parent, to have the condition.
Autosomal Recessive Inheritance Pattern
Thalassemia is inherited in an autosomal recessive manner. This means both parents must carry the thalassemia gene for their child to have thalassemia major. Carriers have a thalassemia trait, which is usually mild but can be passed on.
Carrier Status (Thalassemia Trait)
Being a carrier of thalassemia means having one normal and one mutated gene. Carriers are often asymptomatic or mildly symptomatic. It’s important for carriers to know their status for family planning.
Inheritance Probability and Risk Factors
If both parents are carriers, there’s a 25% chance their child will have thalassemia major. There’s a 50% chance the child will be a carrier like the parents. And a 25% chance the child won’t have thalassemia or be a carrier. Knowing these chances is key for families with thalassemia history.
|
Parental Carrier Status |
Child’s Chance of Thalassemia Major |
Child’s Chance of Being a Carrier |
Child’s Chance of Not Being Affected |
|---|---|---|---|
|
Both parents are carriers |
25% |
50% |
25% |
|
One parent is a carrier, the other is not |
0% |
50% |
50% |
Types of Thalassemia
It’s important to know the different types of thalassemia for proper diagnosis and treatment. Thalassemia is classified based on the affected globin chain.
Alpha Thalassemia Variants
Alpha thalassemia happens when there’s a mutation or deletion in the genes for alpha-globin. The severity depends on how many genes are affected. There are several types of alpha thalassemia, including:
- Silent carrier: One gene is affected, and symptoms are usually not seen.
- Alpha thalassemia trait: Two genes are affected, leading to mild anemia.
- Hemoglobin H disease: Three genes are affected, causing more severe anemia and complications.
- Alpha thalassemia major: All four genes are affected, leading to severe anemia and often fatal without prenatal diagnosis and intervention.
Beta Thalassemia Variants
Beta thalassemia is caused by mutations in the genes for beta-globin. The severity varies based on the mutation and how many genes are affected. The main types are:
- Beta thalassemia minor (trait): One gene is affected, leading to mild anemia.
- Beta thalassemia intermedia: Both genes are affected, but it’s less severe than thalassemia major.
- Beta thalassemia major: Both genes are severely affected, causing severe anemia, health issues, and the need for regular blood transfusions.
For more information on beta thalassemia, visit from the American Academy of Family Physicians.
Delta-Beta and Other Rare Forms
Delta-beta thalassemia is a rare form caused by a deletion of both delta and beta globin genes. It results in a mild form of thalassemia. Other rare forms include:
- Hemoglobin Lepore: A fusion gene from a deletion combining delta and beta globin genes.
- Hemoglobin E/beta thalassemia: A compound heterozygous condition with a variable phenotype, from mild to severe.
|
Type of Thalassemia |
Genes Affected |
Severity |
|---|---|---|
|
Alpha Thalassemia Silent Carrier |
1 alpha-globin gene |
Mild/No symptoms |
|
Alpha Thalassemia Trait |
2 alpha-globin genes |
Mild anemia |
|
Hemoglobin H Disease |
3 alpha-globin genes |
Moderate to severe anemia |
|
Alpha Thalassemia Major |
4 alpha-globin genes |
Severe anemia, often fatal without intervention |
|
Beta Thalassemia Minor |
1 beta-globin gene |
Mild anemia |
|
Beta Thalassemia Intermedia |
Both beta-globin genes |
Moderate anemia |
|
Beta Thalassemia Major |
Both beta-globin genes severely affected |
Severe anemia, significant health issues |
Severity Spectrum: From Trait to Major
It’s important to know the severity spectrum of thalassemia for good management and treatment. This genetic blood disorder can range from mild to severe. Each level has its own degree of severity.
Thalassemia Minor (Trait)
Thalassemia minor, or the thalassemia trait, is a mild form. People with this usually have mild anemia or no symptoms. They can pass the disease to their children.
This condition is often found during routine blood tests.
Thalassemia Intermedia
Thalassemia intermedia is a moderate form, between minor and major in severity. Those with it may have anemia and other issues. But they usually don’t need blood transfusions often.
This condition can affect their quality of life, so it needs careful management.
Thalassemia Major
Thalassemia major, or Cooley’s anemia, is the most severe. It needs lifelong care, including blood transfusions and iron chelation. Without treatment, it can cause serious problems, like organ damage and growth issues in kids.
Research shows the severity of thalassemia can vary a lot. The table below highlights the main differences between minor, intermedia, and major forms.
|
Characteristics |
Thalassemia Minor |
Thalassemia Intermedia |
Thalassemia Major |
|---|---|---|---|
|
Symptoms |
Mild or no anemia |
Moderate anemia, possible complications |
Severe anemia, significant complications |
|
Transfusion Requirements |
None |
Occasional or none |
Regular |
|
Management |
Monitoring |
Occasional transfusions, monitoring |
Lifelong transfusions, iron chelation |
Understanding thalassemia’s severity spectrum is key for healthcare and patient management. By classifying it into minor, intermedia, and major, we can tailor treatments better. This helps meet each patient’s unique needs.
Genetic Mutations in Thalassemia
Thalassemia is caused by many genetic mutations that stop normal hemoglobin making. These changes can mess up the alpha or beta chains of hemoglobin. This leads to different types of thalassemia.
The Diversity of Thalassemia Mutations
Studies have found over 200 mutations that cause thalassemia. These changes affect the globin genes in different ways. Some stop the making of a globin chain, while others make it less or change it.
This variety makes thalassemia hard to diagnose. We’ll see how different mutations lead to different thalassemia types.
Common vs. Rare Mutations
Some thalassemia mutations are common in certain areas, while others are rare. For example, some are common in the Mediterranean, while others are found more in Southeast Asia. Knowing where these mutations are helps in making better screening plans.
Common mutations affect more people and are a big health issue. Rare ones are harder to find because they don’t happen often. We’ll talk about how tests are made to find both kinds of mutations.
Mutation Detection Methods
There are many ways to find thalassemia mutations. Methods like PCR, DNA sequencing, and gap-PCR help spot specific changes. These methods help doctors diagnose and screen for carriers, which is key for family planning.
Genetic testing has gotten better, making thalassemia diagnosis more accurate and accessible. We’ll look at how these methods help care for patients.
Global Prevalence and Distribution
Thalassemia is a genetic disorder found in many parts of the world. It’s more common in certain ethnic and geographical groups. Knowing where it’s most common helps us prevent and treat it better.
Mediterranean Basin
The Mediterranean region has a high rate of thalassemia. Countries like Greece, Italy, and Cyprus have many carriers and people with the disease. Research shows that up to 15% of people in these countries may carry the beta-thalassemia trait.
Middle East and India
In the Middle East, Iran, Saudi Arabia, and the United Arab Emirates have a lot of thalassemia. India also struggles with thalassemia, affecting certain communities. In these areas, up to 10% of people may carry the trait.
Southeast Asia and China
Southeast Asia, including Thailand, Indonesia, and Malaysia, has a lot of thalassemia cases. China, too, has a high rate, mainly in the south. The genetic diversity in these places makes thalassemia mutations more complex.
Africa and Other Regions
Africa, while less known for thalassemia, does have cases, mostly in North Africa. The Americas and Europe also have cases due to migration and genetic diversity.
Thalassemia is a big public health problem worldwide. Its global spread shows we need to raise awareness and set up screening and management programs for each area.
|
Region |
Prevalence Rate |
Notable Countries |
|---|---|---|
|
Mediterranean Basin |
High |
Greece, Italy, Cyprus |
|
Middle East and India |
Moderate to High |
Iran, Saudi Arabia, India |
|
Southeast Asia and China |
Moderate to High |
Thailand, Indonesia, China |
|
Africa and Other Regions |
Low to Moderate |
North Africa, Americas, Europe |
Signs, Symptoms, and Complications
It’s important to know the signs and symptoms of thalassemia early. This helps in getting the right treatment. Thalassemia can lead to various health problems, from mild to severe.
Early Warning Signs
Pale skin, fatigue, and shortness of breath are early signs of thalassemia. These happen because thalassemia affects how red blood cells carry oxygen. This is due to a problem with hemoglobin, a key protein in red blood cells.
Chronic Anemia Manifestations
Chronic anemia is a big problem in thalassemia, like in thalassemia major. People with it often feel tired, weak, and dizzyall the time. This is because their bodies don’t make enough hemoglobin, which is needed to carry oxygen.
Iron Overload Complications
Iron overload is a big risk for people with thalassemia, mainly those who get many blood transfusions. Too much iron can harm organs like the heart, liver, and pancreas. This can cause heart issues, liver damage, and problems with the endocrine system. It’s key to keep iron levels in check to avoid these problems.
Growth and Development Issues
Thalassemia can also affect how children grow and develop. Delayed growth, poor weight gain, and developmental delays can happen because of chronic anemia and other issues. It’s important to watch and manage these problems closely.
Studies have found that thalassemia can lead to serious health issues if not treated well. It’s important for doctors and patients to know the signs, symptoms, and possible complications. This helps in getting the best care and improving life quality.
Diagnosing Thalassemia
To accurately diagnose thalassemia, we use several key tests. These tests help us identify thalassemia and ensure patients get the right care.
Complete Blood Count Analysis
A complete blood count (CBC) is often the first test for thalassemia. It checks the levels of different blood cells. In thalassemia, the CBC may show anemia, which is a low red blood cell count or hemoglobin level.
Anemia is a key symptom of thalassemia. The CBC helps us understand how severe it is.
Hemoglobin Electrophoresis
Hemoglobin electrophoresis is a key test for thalassemia. It separates and identifies different types of hemoglobin in the blood. This test can detect abnormal hemoglobin production in thalassemia.
“Hemoglobin electrophoresis is essential for diagnosing and characterizing thalassemia.” It helps us understand the genetic basis of the disorder.
Genetic Testing Approaches
Genetic testing is vital for diagnosing thalassemia. We analyze genes responsible for hemoglobin production to find mutations linked to thalassemia. This information is key for genetic counseling and family planning.
- DNA analysis to identify specific mutations
- Carrier screening for family members
- Prenatal diagnosis for pregnant individuals
Prenatal Diagnosis Options
Prenatal diagnosis is available for thalassemia. Techniques like chorionic villus sampling (CVS) or amniocentesis can diagnose thalassemia in the fetus. This is vital for expecting parents to make informed decisions.
“Prenatal diagnosis of thalassemia provides critical information for family planning and pregnancy management.”
Early diagnosis and treatment can greatly improve outcomes for thalassemia patients. By using these diagnostic methods, we can offer complete care for those with thalassemia.
Treatment Approaches for Thalassemia
Thalassemia treatment has grown, mixing new therapies with old ones like blood transfusions. A good treatment plan must fit each person’s needs.
Regular Blood Transfusions
For thalassemia major, blood transfusions are key. They keep hemoglobin levels up, easing anemia symptoms. This helps with growth and development.
“Regular blood transfusions have been a lifesaver for many thalassemia patients, significantly improving their quality of life,” a leading hematologist said.
Transfusions are given every 2-4 weeks. This depends on how severe the condition is and how well the patient responds. But, too many transfusions can cause iron overload, needing more treatment.
Iron Chelation Therapy
Iron chelation therapy is vital for iron overload from blood transfusions. It uses medicines to remove excess iron from the body. This helps avoid damage to the heart and liver.
There are many iron chelation agents, like deferoxamine, deferiprone, and deferasirox. Each has its own benefits and side effects. The right chelator depends on the patient’s needs and preferences.
Bone Marrow and Stem Cell Transplantation
Bone marrow transplantation (BMT) is the only cure for thalassemia major. It replaces the patient’s bone marrow with healthy marrow from a donor. Stem cell transplantation uses stem cells from the donor’s bone marrow or blood.
BMT can cure thalassemia but is risky. It’s mainly for those with severe thalassemia and a matched donor.
Gene Therapy and Emerging Treatments
Gene therapy is a new hope for thalassemia. It aims to fix the genetic problem causing the disorder. By adding a healthy gene, it could restore normal hemoglobin production.
Many gene therapy methods are being tested, with some showing promise. Though early, gene therapy could change thalassemia treatment, giving patients a lasting solution.
Living with Thalassemia
Managing thalassemia is more than just medical care. It’s about a whole-life approach. People with thalassemia need a plan that covers daily life, nutrition, exercise, and mental health support.
Daily Management Strategies
Managing thalassemia daily means several important steps. Regular blood transfusions keep hemoglobin levels healthy. Also, iron chelation therapy helps deal with iron buildup from transfusions.
|
Management Aspect |
Description |
Frequency |
|---|---|---|
|
Blood Transfusions |
Transfusions to maintain healthy hemoglobin levels |
Every 2-4 weeks |
|
Iron Chelation Therapy |
Treatment to remove excess iron from the body |
Daily, as prescribed |
|
Monitoring |
Regular check-ups and blood tests |
Ongoing, as advised by healthcare provider |
Nutritional Considerations
Eating a balanced diet is key for thalassemia patients. Nutritional supplements might be needed for essential nutrients. It’s also important to watch iron intake to avoid problems.
Physical Activity Guidelines
Staying active is good for health and managing thalassemia. Low-impact exercises like walking, swimming, or yoga are good choices. Always talk to a doctor before starting new exercises.
Psychological and Social Aspects
Thalassemia affects mental and social health. Counseling and support groups offer emotional support. Having a strong family and friend network is also important.
With a complete management plan, thalassemia patients can live full and happy lives. It’s about balancing medical care, lifestyle changes, and emotional well-being.
Genetic Counseling and Family Planning
Genetic counseling is key for families with thalassemia. It helps them understand genetic risks and explore reproductive choices.
When to Seek Genetic Counseling
If you have thalassemia or carry the trait, consider genetic counseling. Early counseling helps you grasp your risks and plan your family.
The Counseling Process
The process starts with a first meeting. A genetic counselor reviews your family’s health history and talks about thalassemia. Counselors use tools and techniques to teach about the condition and its genetic aspects.
|
Step |
Description |
|---|---|
|
Initial Consultation |
Assessment of family medical history and provision of information about thalassemia. |
|
Risk Assessment |
Evaluation of the risk of passing thalassemia to offspring. |
|
Discussion of Reproductive Options |
Exploration of various reproductive choices, including prenatal diagnosis and preimplantation genetic diagnosis. |
Reproductive Options for Carriers
Carriers of thalassemia have several options. These include prenatal diagnosis and preimplantation genetic diagnosis (PGD) during IVF.
Preimplantation Genetic Diagnosis
Preimplantation genetic diagnosis is used in IVF to check for genetic disorders. PGD can significantly reduce the chance of thalassemia major in a child.
Understanding your options and risks helps families make informed reproductive health decisions. Genetic counseling offers support and guidance throughout this journey.
Prevention and Screening Programs
Prevention and screening programs are key to fighting thalassemia globally. They help find carriers and those affected early. This way, we can act fast and make smart choices.
Population Screening Initiatives
Population screening is essential for finding thalassemia carriers in high-risk groups. It uses genetic tests to spot people with thalassemia genes.
Benefits of Population Screening:
- Early detection of carriers
- Informed family planning
- Reduction in the incidence of thalassemia major
Premarital Screening
Premarital screening tests couples for thalassemia before they get married. It’s common in areas where thalassemia is common.
|
Region |
Prevalence of Thalassemia Trait |
Premarital Screening Rate |
|---|---|---|
|
Mediterranean |
High |
80% |
|
Middle East |
Moderate to High |
70% |
|
Southeast Asia |
High |
60% |
Newborn Screening
Newborn screening tests babies for thalassemia right after birth. It helps start the right care early.
Newborn screening programs have been instrumental in improving outcomes for children with thalassemia.
Public Health Strategies
Good public health strategies are vital for thalassemia prevention and screening. They include awareness campaigns, education for doctors, and genetic testing access.
With strong prevention and screening efforts, we can lessen thalassemia’s impact on people, families, and communities worldwide.
Thalassemia and Comorbidities
People with thalassemia face many health issues. This is why they need full care. Thalassemia affects how the body makes hemoglobin, leading to other health problems. It’s important to know about these issues to help patients the best way.
Thalassemia and Cancer Risk
Studies show thalassemia patients are more likely to get some cancers. The reasons are not clear, but anemia and iron buildup from transfusions might play a part. suggests watching patients closely and taking steps to prevent cancer is key.
Cardiovascular Complications
Heart problems are big worries for thalassemia major patients. Too much iron from transfusions can harm the heart. It’s important to check the heart often and use iron chelation therapy to keep risks low.
Endocrine Disorders
Thalassemia patients often face endocrine issues because of iron buildup. Problems like thyroid issues, diabetes, and low sex hormones can happen. Finding and treating these early is critical to avoid serious problems later.
Infection Susceptibility
Thalassemia patients, and those who have had their spleen removed, are more likely to get sick. The spleen helps fight off infections, and iron overload can weaken the immune system. Vaccines and antibiotics might be suggested to keep infections away.
Dealing with thalassemia means more than just treating the main condition. It’s about handling all related health issues too. A team of doctors, including hematologists, cardiologists, and endocrinologists, is essential for the best care.
Conclusion
Thalassemia is a complex genetic disorder that needs a full management plan. Understanding its genetic roots, how it’s passed down, and treatment options is key for top-notch care.
Studies show early detection, treatment, and ongoing care can greatly help those with thalassemia. Our hospital network aims to offer top healthcare and support for international patients. We make sure they get the best care for thalassemia.
By recognizing thalassemia’s complexities and the need for personalized treatment, we can enhance the lives of those with this disorder.
FAQ
What is thalassemia?
Thalassemia is a serious genetic disorder. It affects how the body makes hemoglobin. This leads to anemia and other health issues.
Is thalassemia inherited?
Yes, thalassemia is passed down through genes. Both parents must carry the gene for a child to have thalassemia major.
What are the different types of thalassemia?
Thalassemia is divided into types based on the affected globin chain. This includes alpha and beta thalassemia.
What are the symptoms of thalassemia?
Symptoms of thalassemia include anemia and iron overload. It can also affect growth and development.
How is thalassemia diagnosed?
Doctors use several methods to diagnose thalassemia. These include blood tests, hemoglobin electrophoresis, and genetic testing.
What are the treatment options for thalassemia?
Treatments for thalassemia include regular blood transfusions and iron chelation therapy. Bone marrow transplantationis also an option.
Can thalassemia be prevented?
Thalassemia can’t be prevented, but screening and genetic counseling can help. They identify carriers and reduce transmission risk.
What is the role of genetic counseling in thalassemia?
Genetic counseling is key for families with thalassemia history. It offers information on reproductive choices and genetic diagnosis before implantation.
How does thalassemia affect quality of life?
Thalassemia can greatly affect one’s life. It requires ongoing management to maintain physical and emotional health.
Are there any comorbidities associated with thalassemia?
Yes, thalassemia increases the risk of cancer, heart problems, and endocrine disorders.
What is the global prevalence of thalassemia?
Thalassemia is a major health concern in many areas. This includes the Mediterranean, Middle East, India, Southeast Asia, and Africa.
How can thalassemia be managed on a daily basis?
Daily management includes regular transfusions, iron chelation, and following nutritional and physical activityguidelines.
References:
- Bajwa, H., & Basit, H. Thalassemia. In StatPearls. National Center for Biotechnology Information. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK545151/ NCBI
- Advanced molecular approaches to thalassemia disorder and the selection of molecular‑level diagnostic testing in resource‑limited settings. PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC12206028/ PMC
- Thalassemias: An Overview. PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC7510249/ PMC
- A combined approach for β‑thalassemia based on gene therapy‑mediated adult hemoglobin (HbA) production and fetal hemoglobin (HbF) induction. PMC. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3389244/ NCBI
- Kliegman, R. M., Stanton, B. F., St Geme, J. W., & Schor, N. F. (2009). Thalassemia. American Family Physician, 80(4), 339–346. Retrieved from https://www.aafp.org/pubs/afp/issues/2009/0815/p339.html
- PMC article (Year). Title. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3677479/



































