Urology treats urinary tract diseases in all genders and male reproductive issues, covering the kidneys, bladder, prostate, urethra, from infections to complex cancers.
Send us all your questions or requests, and our expert team will assist you.
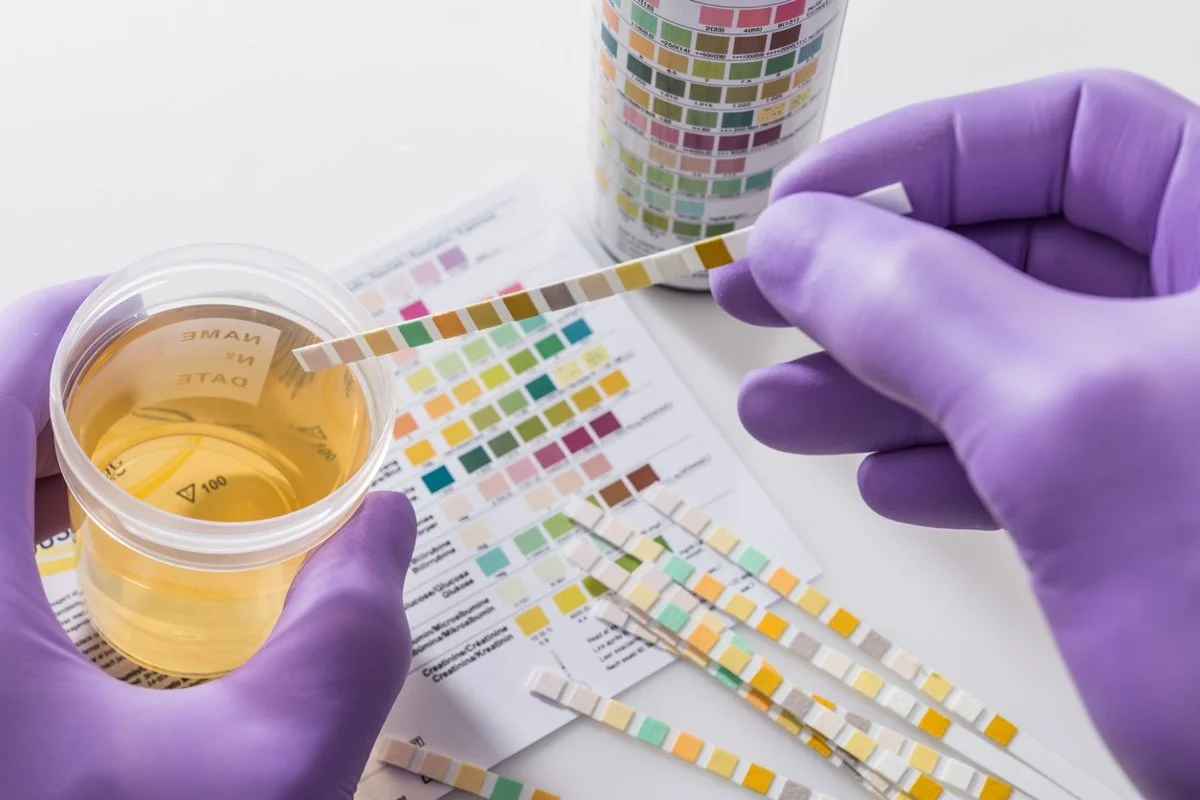
The Urine Flow Test, or uroflowmetry, is a key non-invasive test in urology. It measures how much urine is passed over time, but it also gives important information about the health of the bladder, prostate, and urethra. Today, doctors use uroflowmetry not just to check mechanics, but also as a sign of how healthy the bladder muscle and related structures are. The test helps doctors tell the difference between blockages, nerve problems, and weak bladder muscles.
Normal urine flow depends on how well the bladder muscle contracts and how open the urethra is. The bladder works like a pump, and the urethra is the tube that carries urine out. A healthy flow curve is usually bell-shaped, showing good coordination between the nerves that control the bladder and sphincter. If the curve is flat and lasts longer, it may mean there is a blockage, like an enlarged prostate or a urethral stricture, which makes it harder for urine to flow.
The urine flow test also looks at how the bladder turns stored energy into the force needed to push urine out. This process relies on healthy bladder muscle cells. If there is a blockage or poor blood flow, these cells can’t make enough energy, and the bladder gets weaker. Uroflowmetry helps doctors spot these problems early, so they can treat them before lasting damage happens.

To understand how the urine flow test works, it helps to know how the body controls urination. Many chemical signals and cell receptors are involved. For example, acetylcholine from nerves makes the bladder muscle contract by letting calcium into the cells. At the same time, nitric oxide helps relax the muscles at the bladder outlet.
Abnormalities in the urine flow rate often reflect a disruption in this signaling cascade. In conditions of bladder outlet obstruction, the detrusor muscle undergoes hypertrophy, and the density of nerve terminals may decrease, a phenomenon known as partial denervation. This leads to altered sensitivity to neurotransmitters and the development of pathological spontaneous activity. The flow rate thus becomes a functional mirror of these microscopic changes. In the context of regenerative medicine, tracking improvements in flow rate following therapies can indicate the restoration of normal cellular signaling and neuromuscular connectivity.
The lining of the bladder, called the urothelium, senses when the bladder is stretched and releases signals like ATP and prostaglandins. These help control urination. If the lining is damaged by inflammation or stress, it can’t sense properly, leading to problems with urination. The urine flow test can show these issues, helping doctors choose treatments to repair the bladder lining and its function.

Lower urinary tract symptoms are common worldwide, especially in older adults. The urine flow test is an important tool to help doctors find problems early. By catching blockages soon, doctors can treat them before they harm the kidneys or lower quality of life.
In developing healthcare infrastructures, the portability and non-invasive nature of uroflowmetry make it an invaluable asset. It allows for the widespread screening of populations at risk for obstructive uropathy without the need for expensive, invasive urodynamic suites. This accessibility aligns with the preventative philosophy of modern medicine, which seeks to address pathology at the functional stage before it progresses to anatomical failure.
Moreover, integrating uroflowmetry data into global health registries enables the identification of epidemiological trends. Variations in flow parameters across different populations can shed light on the influence of environmental factors, diet, and lifestyle on urological health. This data drives the development of public health initiatives focused on metabolic health and preventative care, reducing the long-term incidence of catheter dependence and renal replacement therapies.
For tissue engineering and regenerative treatments, the urine flow test shows if the therapy is working. Whether doctors rebuild the urethra or use stem cells to fix the sphincter, the main goal is to restore normal urine flow. Any new tissue must be strong enough to handle the force of urination.
The urine flow test checks how well new or repaired tissues in the urinary tract work under real conditions. A normal flow curve after surgery means the new tissue is working well with the body. Researchers are also testing biodegradable materials with a patient’s own cells to replace damaged urethra, and they use the flow test over time to see if these treatments succeed.

The future of urine flow testing lies in integrating digital health and artificial intelligence. Smart toilets and home monitoring devices are being developed to provide continuous, longitudinal data on voiding patterns. These devices use acoustic sensors, optical flow cytometry, and artificial intelligence algorithms to analyze flow characteristics in the patient’s natural environment, thereby eliminating the white-coat effect often seen in clinical testing.
This continuous stream of data allows for the detection of subtle changes in voiding dynamics that may precede symptomatic progression. Machine learning models can analyze these patterns to predict the risk of acute urinary retention or the failure of medical therapy. This shift towards remote, continuous monitoring aligns with the personalized medicine approach, enabling timely interventions tailored to each individual’s unique physiological rhythm.

Send us all your questions or requests, and our expert team will assist you.
A standard urine flow rate depends on age and gender. Generally, a maximum flow rate (Qmax) greater than 15 milliliters per second is considered nonobstructive in adult men, provided the voided volume is adequate, typically greater than 150 milliliters. In women, normal flow rates are usually higher, often exceeding 20 to 25 milliliters per second. A flow rate consistently below 10 milliliters per second suggests a high probability of obstruction or detrusor muscle weakness.
Uroflowmetry alone cannot definitively distinguish between a blockage, such as an enlarged prostate, and a weak bladder muscle (detrusor underactivity). Both conditions can produce a low flow rate. To differentiate them, further testing, such as pressure flow urodynamics, is required. This invasive test measures the pressure inside the bladder while voiding. High pressure with low flow indicates blockage, while low pressure with low flow indicates a weak muscle.
The urine flow test is completely non-invasive and painless. It simply involves urinating into a specialized funnel or toilet that contains a sensor to measure the speed and volume of the stream. No catheters, needles, or instruments are inserted into the body. The primary requirement is that the patient must arrive with a comfortably full bladder to ensure a representative void.
Yes, anxiety can significantly affect the results. The phenomenon known as shy bladder or paruresis is common in clinical settings. Sympathetic nervous system activation from stress can tighten the bladder neck and inhibit bladder muscle contraction, leading to a falsely low flow rate or an interrupted stream. Clinicians often allow patients to void in private and may repeat the test to ensure accuracy.
The shape of the flow curve provides diagnostic clues beyond the numbers alone. A standard curve is bell-shaped and continuous. A flattened, plateau-like curve often indicates a stricture or rigid obstruction. An intermittent or staccato curve, where the flow stops and starts, suggests that the patient is straining with the abdominal muscles to void or has sphincter dyssynergia, in which the sphincter does not relax properly.


Did you know trouble peeing can signal a health problem? Proper urinary function is key for our health. When we can’t pee easily, it’s uncomfortable

Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)