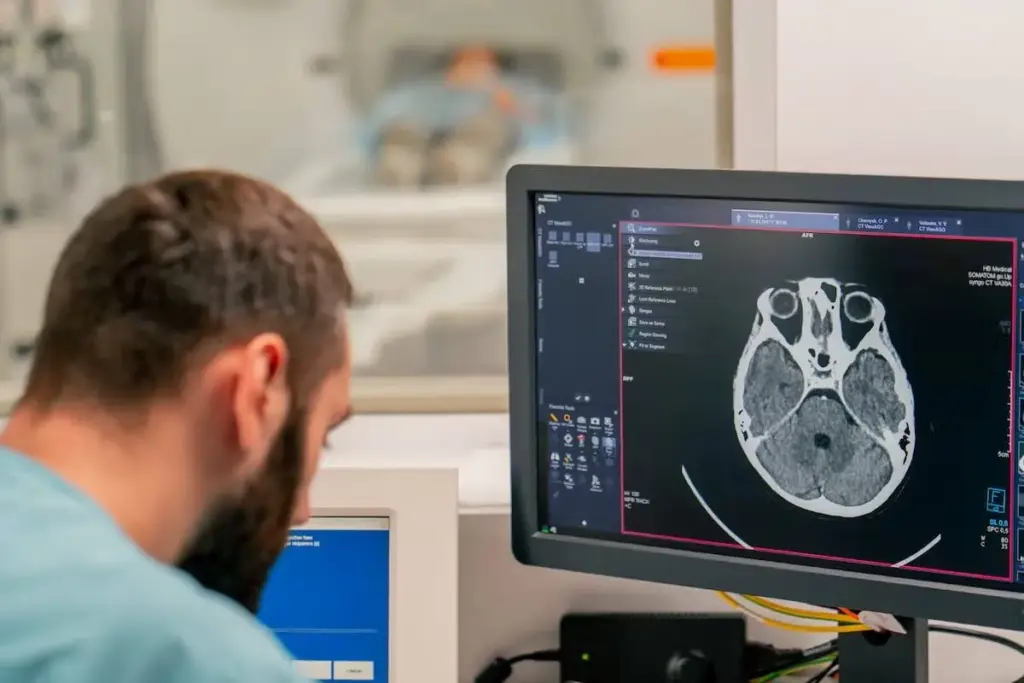
Interventional radiology has changed the medical world. It offers new ways to treat diseases without big surgeries. Thanks to image-guided therapy, we now treat many conditions differently.
Interventional radiology is key in cancer treatment. It uses targeted therapies that have fewer side effects. Tumor ablation is a big help in fighting some cancers.
Looking into interventional radiology, we see it’s making a big difference. It’s not just improving patient care. It’s also changing how we treat diseases in the future.
Key Takeaways
- Interventional radiology offers minimally invasive alternatives to traditional surgery.
- It plays a key role in cancer treatment with targeted therapies.
- Techniques like tumor ablation help manage some cancers.
- Image-guided therapy is a big part of interventional radiology.
- This field is improving patient care and changing medical treatments.
Understanding Interventional Radiology
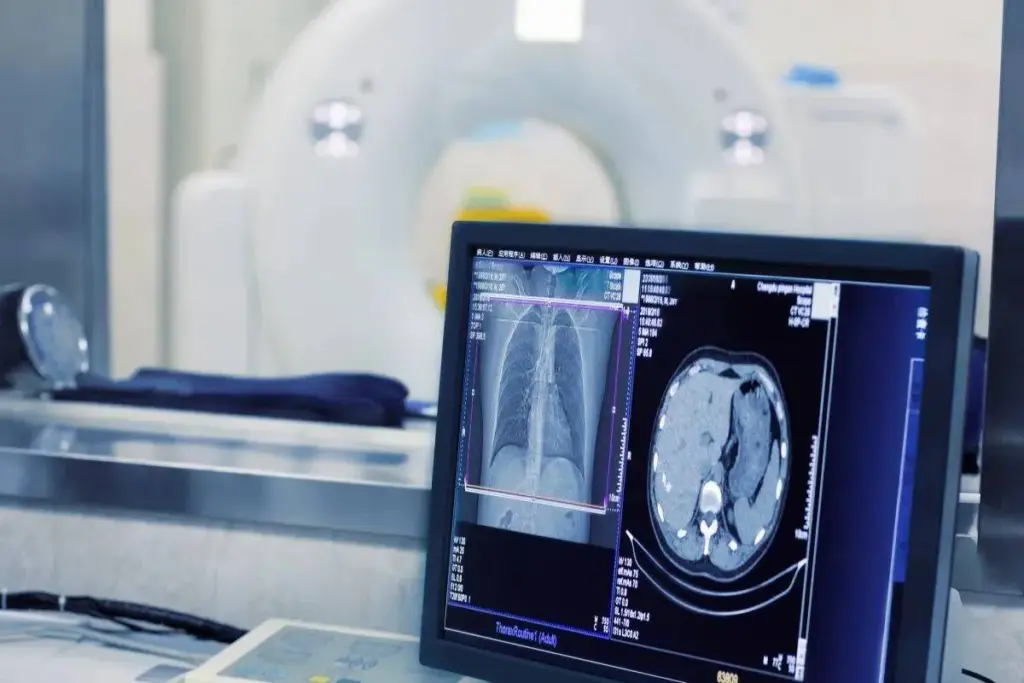
Interventional radiology is a key part of modern medicine. It has changed how we care for patients. Now, we use treatments that are less invasive. This means patients recover faster and face fewer risks.
Definition and Core Concepts
Interventional radiology uses advanced imaging and small surgical techniques. This method allows for precise treatments with little harm to the body. Patients recover quickly and face less chance of infection.
“The beauty of interventional radiology lies in its ability to offer targeted treatments that are both effective and efficient,” says a leading expert in the field. “By leveraging cutting-edge imaging and radiation therapy, we can provide patients with life-changing outcomes.”
The Evolution of Minimally Invasive Procedures
The field of interventional radiology keeps getting better. New techniques and technologies are being developed. Minimally invasive treatments now tackle complex conditions that used to need open surgery.
- Advancements in advanced radiation oncology have enabled more precise targeting of diseased tissues.
- The development of new materials and devices has improved the safety and efficacy of interventional procedures.
- Increased use of real-time imaging has enhanced the accuracy of interventions.
We are always looking to improve in interventional radiology. We aim to give our patients the best care. By embracing new ideas and staying ahead in medical science, we ensure our patients get the best results.
The Science Behind Interventional Radiation
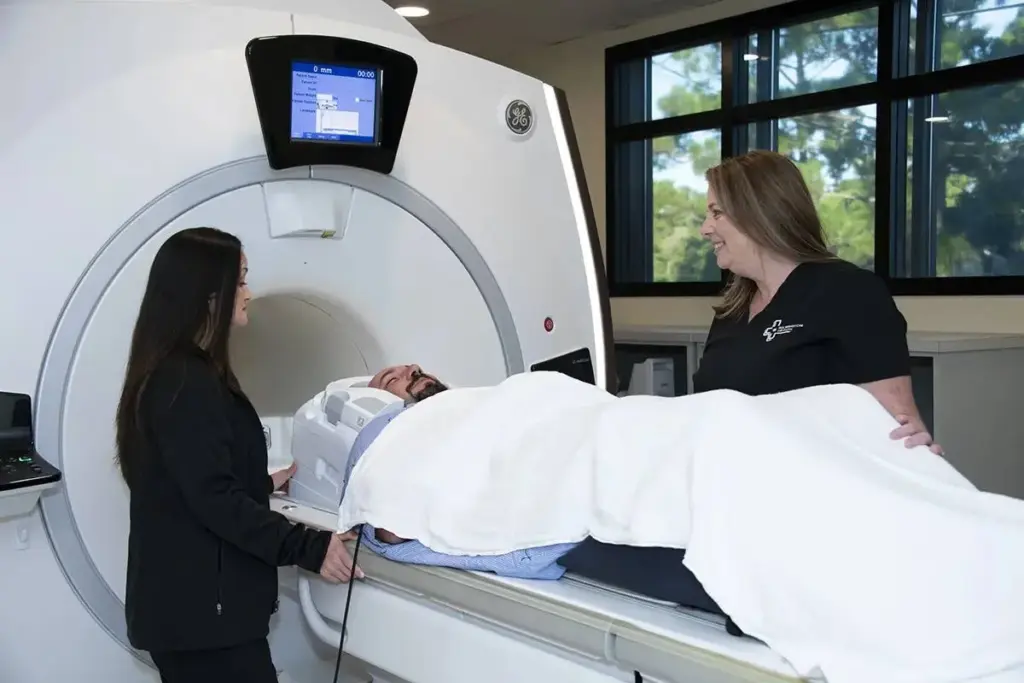
Interventional radiation works thanks to real-time images and targeted radiation. This mix of tech makes treatments for many health issues, like cancer, very effective.
Advanced Imaging Technologies
For interventional radiation to succeed, advanced imaging is key. These include:
- High-resolution fluoroscopy: Shows the treatment area in real-time.
- Ultrasound guidance: Helps target tumors and tissues precisely.
- CT and MRI imaging: Gives detailed images for planning and delivering radiation.
These tools help aim radiation exactly where it’s needed, making treatments more effective.
Principles of Targeted Radiation Delivery
Targeted radiation focuses on the tumor, not healthy tissues. This is key in radiation oncology services. It helps keep treatments effective while protecting the body.
The main principles are:
- Precision: Radiation goes exactly where it’s needed.
- Minimally invasive: Fewer surgeries are needed.
- Personalized treatment: Treatments are tailored for each patient.
Real-time Image Guidance
Real-time images let doctors adjust treatments as they go. This is vital for precision radiation treatment. It allows for quick changes to keep the treatment on track.
The benefits are:
- Improved accuracy: Treatments work better.
- Reduced risk: Fewer complications and side effects.
- Enhanced patient safety: Treatments are safer and more effective.
Key Differences Between Interventional Radiology and Traditional Surgery
Interventional radiology is a new way to treat medical conditions. It’s different from traditional surgery. With new technology, this difference is becoming more important.
Benefits of Minimally Invasive Approaches
Interventional radiology uses small cuts and imaging to do procedures. This means less damage to the body and fewer risks of infection.
It’s great because it can treat many conditions without open surgery. For example, embolization and ablation can be done with local anesthesia. This avoids the dangers of general anesthesia.
Recovery Time and Hospital Stay Comparison
People who get interventional radiology treatments usually recover faster. This is because it’s less invasive, causing less pain and trauma.
|
Procedure Type |
Average Recovery Time |
Typical Hospital Stay |
|---|---|---|
|
Interventional Radiology |
1-3 days |
0-1 day |
|
Traditional Surgery |
Several weeks |
3-7 days or more |
Cost Effectiveness and Insurance Coverage
Interventional radiology is often cheaper than surgery. It needs less hospital time and care, leading to lower costs.
Many insurances cover it because it saves money and improves health. But, what’s covered can change based on the procedure and plan.
In summary, interventional radiology is a good choice instead of surgery. It’s less invasive, leads to quicker recovery, and is more affordable. As medicine keeps getting better, interventional radiology will likely play a bigger role, giving patients more options and better results.
Common Vascular Interventions
Vascular interventions are key in interventional radiology. They offer effective treatments for many vascular diseases. These methods have changed how we treat vascular conditions, making them less invasive than traditional surgery.
Angiography and Angioplasty Procedures
Angiography lets doctors see inside blood vessels. It helps find blockages and other problems. Angioplasty uses a balloon to open narrowed vessels, improving blood flow.
Often, a stent is placed to keep the artery open. These methods are used for diseases like PAD and CAD. They offer quick recovery and lower risks compared to surgery.
Embolization for Bleeding Control
Embolization stops bleeding by blocking blood flow. It uses materials like coils or particles. This method is good for acute bleeding, tumors, and vascular malformations.
We use it for bleeding in the gut, trauma, and some tumors. The procedure is guided by images for accuracy.
Vascular Stenting Applications
Vascular stenting places a stent in narrowed or blocked vessels. This restores blood flow. Stents can be bare metal or drug-eluting, releasing medication to prevent re-narrowing.
Stenting treats conditions like carotid artery disease, PAD, and CAD. It’s often done with angioplasty.
|
Procedure |
Application |
Benefits |
|---|---|---|
|
Angiography |
Diagnostic imaging of blood vessels |
Identifies blockages and abnormalities |
|
Angioplasty |
Treatment of narrowed blood vessels |
Restores blood flow, minimally invasive |
|
Embolization |
Control of bleeding and tumor management |
Effective in managing acute bleeding and tumors |
|
Vascular Stenting |
Treatment of narrowed or blocked vessels |
Restores blood flow, prevents re-narrowing |
Interventional Oncology Applications
Interventional oncology has changed cancer treatment by introducing new, less invasive methods. It uses advanced imaging and new treatments to fight cancer more effectively.
Tumor Ablation Techniques
Tumor ablation kills cancer cells with heat, cold, or chemicals. Radiofrequency ablation (RFA) and cryoablation are popular for treating tumors in the liver, kidney, and lung. These methods are guided by images to target tumors accurately and protect healthy tissue.
Benefits of tumor ablation include shorter recovery times, less pain, and treating patients who can’t have surgery. These procedures have brought new hope to many patients.
Transarterial Chemoembolization (TACE)
TACE delivers chemotherapy directly to tumors through the blood, then blocks the tumor’s blood supply. This method boosts chemotherapy’s effectiveness and starves the tumor of nutrients and oxygen.
TACE is very effective for liver cancer and has improved survival rates for patients with tumors that can’t be removed. The procedure is done under local anesthesia, and most patients can go home the same day.
Radioembolization with Y-90 Microspheres
Radioembolization uses tiny Yttrium-90 (Y-90) microspheres infused with radiation. These microspheres are delivered to the tumor through the blood, killing cancer cells. This method is precise, reducing harm to healthy tissue.
Radioembolization with Y-90 microspheres treats various cancers, including liver cancer and metastatic disease. Most patients find the procedure tolerable, with mild side effects.
Gastrointestinal and Hepatobiliary Procedures
Interventional radiology has changed how we treat the digestive system and liver. It uses new imaging to find and fix many problems. This makes treatment easier and less invasive.
Biliary Drainage and Stenting
Biliary drainage and stenting help with blocked bile ducts and other liver issues. We use stents or catheters to open up the bile flow. This helps patients feel better and live longer.
We do this by going through the skin and using imaging to guide us. It’s a small procedure that avoids big surgery. This means patients heal faster and face fewer risks.
Feeding Tube Placement Techniques
Feeding tubes help patients who can’t eat normally. This includes those with cancer, brain problems, or injuries. We use special methods to place these tubes safely.
With imaging, we guide the tube to the right spot in the stomach or small intestine. This method is less painful and safer than old surgery ways.
Transjugular Intrahepatic Portosystemic Shunt (TIPS)
TIPS helps with high blood pressure in the liver. It stops bleeding and swelling. We make a new path in the liver to lower pressure.
To do TIPS, we go through the jugular vein to the liver. Then, we make a connection to the portal vein. This is done under X-ray and needs careful planning and watching.
In summary, these procedures are key in interventional radiology. They offer new ways to treat complex problems. With modern imaging and techniques, we can make patients’ lives better and shorter recovery times.
Genitourinary Interventions
Genitourinary interventions are key in interventional radiology. They offer non-invasive solutions for many urological issues. These methods have changed how we treat genitourinary problems, giving patients better options than surgery.
Nephrostomy and Ureteral Stenting
Nephrostomy and ureteral stenting help with urinary tract blockages. A nephrostomy creates a direct path to the kidney to clear blockages. Ureteral stenting puts a stent in the ureter to keep urine flowing. These treatments can save lives and greatly improve patients’ quality of life.
Prostate Artery Embolization for BPH
Prostate artery embolization (PAE) is a new way to treat BPH. It blocks blood to the prostate, shrinking it and easing symptoms. This method is less invasive than surgery, with fewer side effects and quicker recovery.
Uterine Fibroid Embolization
Uterine fibroid embolization (UFE) is a top choice for treating uterine fibroids. It cuts off blood to the fibroids, causing them to shrink and die. UFE is great for women who want to avoid major surgeries, with a shorter recovery time.
Varicocele Embolization
Varicocele embolization treats varicoceles, enlarged veins in the scrotum. It blocks abnormal blood flow, easing pain and improving fertility. This procedure is done as an outpatient, under local anesthesia, allowing quick return to daily activities.
Musculoskeletal Applications
Interventional radiology has changed how we treat musculoskeletal issues. It offers less invasive treatments for patients around the world. These treatments are key in managing bone and soft tissue problems.
Vertebroplasty and Kyphoplasty for Spinal Fractures
Vertebroplasty and kyphoplasty help with spinal fractures. Vertebroplasty fills the fractured vertebra with bone cement. Kyphoplasty first inflates a balloon to make space, then adds cement.
These methods greatly reduce pain and improve life quality. They’re great for those who haven’t gotten better with other treatments.
|
Procedure |
Description |
Benefits |
|---|---|---|
|
Vertebroplasty |
Injection of bone cement into the fractured vertebra |
Pain relief, stabilization of the vertebra |
|
Kyphoplasty |
Inflation of a balloon to create space, followed by bone cement injection |
Restoration of vertebral height, pain relief |
Pain Management Interventions
Pain management is vital in musculoskeletal care. Interventional radiology offers many pain relief options. This includes nerve blocks and joint injections.
Bone Biopsy and Tumor Ablation
Bone biopsy and tumor ablation are key for diagnosing and treating musculoskeletal tumors. Bone biopsy gets a tissue sample for diagnosis. Tumor ablation uses methods like radiofrequency or cryoablation to kill tumor cells.
These methods are essential for treating musculoskeletal tumors. They offer a less invasive way to treat different types of tumors.
Neurological Interventions
Interventional radiology is key in managing neurological disorders. It uses minimally invasive procedures. These methods are safer than traditional surgery for the brain and spine.
Acute Stroke Treatment
Acute stroke treatment is a big part of interventional radiology. Mechanical thrombectomy has changed how we treat ischemic strokes. It removes blood clots and brings blood back to the brain.
This procedure is done quickly after a stroke. It shows how important fast medical help is.
Brain Aneurysm Coiling and Flow Diversion
Brain aneurysm coiling and flow diversion treat brain aneurysms. Coiling fills the aneurysm with platinum coils to stop bleeding. Flow diversion uses a stent to redirect blood flow.
Both methods are very effective. They help prevent rupture and lower the risk of complications.
Spinal Interventions for Pain Management
Spinal interventions, like vertebroplasty and kyphoplasty, help with spinal fracture pain. They inject bone cement into the vertebra to stabilize it and lessen pain. Other methods include nerve blocks and spinal cord stimulation for chronic pain.
|
Procedure |
Description |
Benefits |
|---|---|---|
|
Mechanical Thrombectomy |
Removal of blood clot in ischemic stroke |
Restores blood flow, reduces damage |
|
Brain Aneurysm Coiling |
Filling aneurysm with platinum coils |
Prevents rupture, reduces bleeding risk |
|
Vertebroplasty/Kyphoplasty |
Injecting bone cement into fractured vertebra |
Stabilizes vertebra, reduces pain |
The Patient Experience in Interventional Radiology
We focus on the patient experience in interventional radiology. We aim to support patients fully throughout their treatment.
Pre-procedure Evaluation and Preparation
Before a procedure, patients get a detailed check-up. This includes looking at their medical history, doing lab tests, and talking about the procedure’s risks and benefits. We also give them instructions on what to do before the procedure, like fasting or changing medications.
What to Expect During Treatment
During the procedure, we keep a close eye on patients and make sure they’re comfortable. We use the latest imaging tech to guide our work, making sure it’s precise and safe. Our team explains each step clearly and answers any questions patients have.
Post-Procedure Care and Recovery Timeline
After the procedure, patients go to a recovery area where they’re watched for any immediate issues. We give them detailed instructions on how to care for themselves, including wound care and medication. The recovery time varies, but most patients can get back to normal in a few days to a week.
Follow-up and Long-term Monitoring
Follow-up care is key in interventional radiology. We schedule check-ups to see how the procedure is working and to address any concerns. Sometimes, we also need to keep an eye on patients over the long term to make sure the treatment is lasting and to manage any ongoing conditions.
|
Stage |
Description |
Timeline |
|---|---|---|
|
Pre-procedure |
Evaluation, preparation, and education |
1-2 weeks before procedure |
|
Procedure |
Interventional radiology treatment |
On the day of the procedure |
|
Post-procedure |
Recovery and initial healing |
1-7 days after procedure |
|
Follow-up |
Monitoring and long-term care |
After recovery, as needed |
Risks, Complications, and Considerations
Interventional radiology has many benefits, but it also comes with risks and complications. It’s important to know these factors to understand how they might affect treatment success and patient outcomes.
Common Side Effects and Management
Most people who have interventional radiology procedures don’t have many side effects. But, some common ones include:
- Pain or discomfort at the procedure site
- Bruising or swelling
- Nausea or vomiting
- Fatigue
These side effects can be managed with medicine or other care. Managing them well is key to keeping patients comfortable and helping them recover faster.
Potential Serious Complications
Even though they are rare, serious complications can happen. These might include:
- Infection at the procedure site
- Bleeding or hematoma
- Allergic reactions to contrast agents
- Vascular injury
It’s important for patients to know about these risks and for doctors to take steps to prevent them. If serious complications do happen, the medical team will act quickly to lessen their effects.
Patient Selection Criteria
Not every patient is right for interventional radiology. Doctors look at several things to decide if it’s a good fit, like the patient’s health and the condition being treated. A detailed check-up is needed to find the best treatment.
When Traditional Surgery May Be Preferred
Sometimes, traditional surgery is better. This choice depends on the condition’s complexity, the patient’s health history, and other factors. Doctors and patients work together to choose the best treatment, whether it’s interventional radiology or surgery.
Knowing about the risks and considerations of interventional radiology helps patients make better choices. It’s important to talk to a healthcare provider about any worries or questions to get the best care.
Finding Qualified Interventional Radiology Providers
Finding the right interventional radiology provider is key. The provider’s expertise greatly affects treatment success. It’s important to know what to look for in qualifications and characteristics.
Board Certification and Specialized Training
When looking for a provider, board certification is essential. It shows the radiologist has passed tough training and tests. They also have specialized skills in certain procedures.
To check if a provider is certified, look up the American Board of Radiology (ABR). The ABR certifies radiologists who meet education, training, and exam standards in radiology, including interventional.
Hospital and Facility Considerations
The quality of the hospital or facility is also key. Accreditation by groups like The Joint Commission is important. It means the facility meets high standards for patient care and safety.
|
Accreditation Criteria |
Description |
Importance |
|---|---|---|
|
Facility Accreditation |
Ensures compliance with safety and care standards |
High |
|
Equipment Quality |
State-of-the-art technology for accurate diagnoses and treatments |
High |
|
Staff Qualifications |
Trained and experienced staff in interventional radiology |
High |
Insurance Coverage and Cost Factors in the US
It’s important to understand insurance coverage and costs for interventional radiology services. Most plans cover these services when they’re medically necessary. But, coverage can vary.
Patients should check their insurance and talk about costs with their provider. Costs depend on the procedure’s complexity, the facility’s fees, and the radiologist’s charges.
Conclusion
Interventional radiology keeps getting better, bringing new treatments for many health issues. This includes cancer treatment through small, precise methods and radiation oncology.
Image-guided therapy is key in finding and treating diseases. It offers targeted solutions that work well.
The advantages of interventional radiology are obvious. It helps patients recover faster, reduces complications, and improves health outcomes. This makes it a vital part of today’s medicine.
As technology improves, interventional radiology will grow. It will offer even better treatments for tough health problems.
FAQ
What is interventional radiology?
Interventional radiology is a medical field that uses small procedures guided by images. It helps diagnose and treat many conditions. This method is less invasive than traditional surgery.
What conditions can be treated with interventional radiology?
It treats many conditions like vascular diseases and cancer. It also helps with gastrointestinal and genitourinary issues. Our team works with patients to find the best treatment.
What are the benefits of interventional radiology compared to traditional surgery?
It has smaller incisions and less pain. Recovery times are shorter, and risks are lower. We often use local anesthesia for safety.
How is targeted radiation delivery achieved in interventional radiation therapy?
Advanced imaging guides the placement of radiation. This ensures the radiation goes directly to the target. It protects healthy tissues.
What is the role of advanced imaging technologies in interventional radiology?
Imaging technologies help us see the area in real-time. They guide our tools and check the procedure’s accuracy. This leads to precise treatment.
Are interventional radiology procedures painful?
We aim to reduce discomfort. Many procedures use local anesthesia. Some patients get sedation to relax. Pain after the procedure is managed with medication.
How do I find a qualified interventional radiology provider?
Look for board certification and specialized training. Check the hospital’s reputation and technology. Also, verify insurance and costs.
What are the possible risks and complications of interventional radiology?
Risks include bleeding and infection. We carefully choose patients and take steps to reduce risks.
How long does it take to recover from an interventional radiology procedure?
Recovery times vary. Some can return to normal in days, while others need more time. We provide personalized care and instructions.
Will my insurance cover interventional radiology procedures?
Coverage varies by insurance plan and procedure. Check with your provider for details on coverage and costs.
References
National Center for Biotechnology Information. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11288872/























