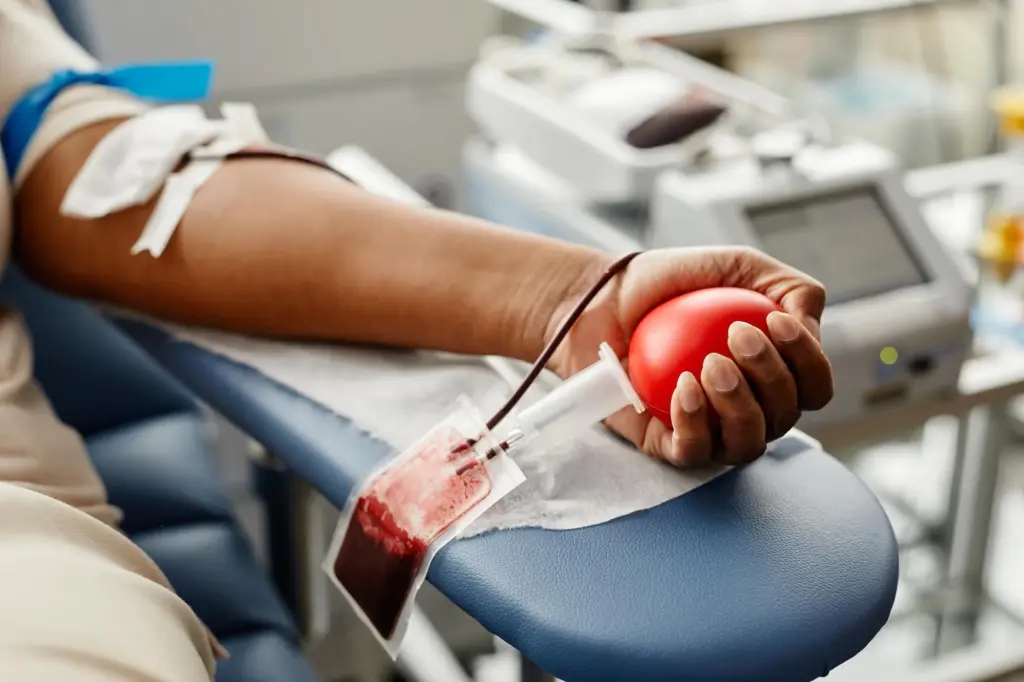
Blood donation is a key act that saves many lives. But, some medical conditions, like hemophilia, make it risky for donors and recipients. Hemophilia stops the body from making blood clots, which are essential to stop bleeding.
The CDC says the average age of diagnosis is 36 months. This shows how early hemophilia affects people.
Those with bleeding disorders, like Von Willebrand disease, face special health issues. The FDA doesn’t let them donate blood because of the risk of harm from big needles. For more on donating blood with bleeding disorders, check out.
Key Takeaways
- Hemophiliacs are not eligible to donate blood due to medical risks.
- The condition is characterized by the inability to form blood clots.
- FDA guidelines defer individuals with bleeding disorders from donating.
- Safety concerns for both donors and recipients are key.
- Bleeding disorders are diagnosed early in life, with a median diagnosis age of 36 months.
Understanding Hemophilia: A Genetic Bleeding Disorder
Hemophilia is a genetic disorder that makes it hard for the body to stop bleeding. It happens because the blood can’t form clots properly. This leads to bleeding that doesn’t stop on its own.
Definition and Types of Hemophilia
Hemophilia is mainly split into two types: Hemophilia A and Hemophilia B. Hemophilia A is caused by a lack of factor VIII. Hemophilia B is due to a lack of factor IX. Both types are genetic and affect how blood clots.
- Hemophilia A: Caused by a deficiency in clotting factor VIII.
- Hemophilia B: Resulting from a deficiency in clotting factor IX.
There are also rare types of hemophilia. Acquired hemophilia is not genetic. It can happen later in life due to diseases or cancer.
Prevalence and Demographics
About 1 in 5,000 male births worldwide have hemophilia. It’s more common in males because it’s an X-linked recessive disorder. Females can carry the gene but are less likely to have it. They can pass it to their sons, though.
It’s estimated that around 400,000 people worldwide live with hemophilia. Managing it for life often involves treatments that replace clotting factors.
Genetic Inheritance Patterns
Hemophilia follows an X-linked recessive pattern. This means males are more likely to be affected if they get the mutated gene. Females need two mutated genes to have the condition, making it rarer in them.
Carriers have a 50% chance of passing the mutated gene to each child. Sons will be affected, and daughters will likely become carriers. Knowing how it’s inherited is key for family planning and genetic counseling.
Diagnosis and Early Detection of Hemophilia

It’s key to catch hemophilia early to start treatment and avoid problems. Hemophilia makes it hard for the body to clot blood, which is needed to stop bleeding. Finding it early is important for managing it well.
Median Age of Diagnosis
The average age when people find out they have hemophilia is about 36 months. This shows how important it is to watch for signs in young children. Finding it early helps start the right treatment and improves life for those with hemophilia.
Diagnostic Tests and Procedures
To diagnose hemophilia, doctors use a few steps. They look at the patient’s history, family background, and run lab tests. The main tests are:
- Bleeding Time Test: Checks if the body can make a blood clot.
- Clotting Time Test: Sees how long it takes for blood to clot.
- Factor Assays: Tests the levels of clotting factors VIII and IX.
- Genetic Testing: Finds the genetic changes that cause hemophilia.
These tests help doctors confirm the diagnosis and figure out how severe it is.
Early Signs and Symptoms
Spotting the early signs of hemophilia is vital for quick medical help. Look out for:
- Frequent bruising: After small injuries.
- Prolonged bleeding: From cuts, nosebleeds, or after surgery.
- Joint pain and swelling: From bleeding into the joints.
- Bleeding into muscles: Causes pain and swelling.
Parents and caregivers should know these signs. If they think someone might have hemophilia, they should get medical help right away.
The Blood Donation Process: Basic Requirements
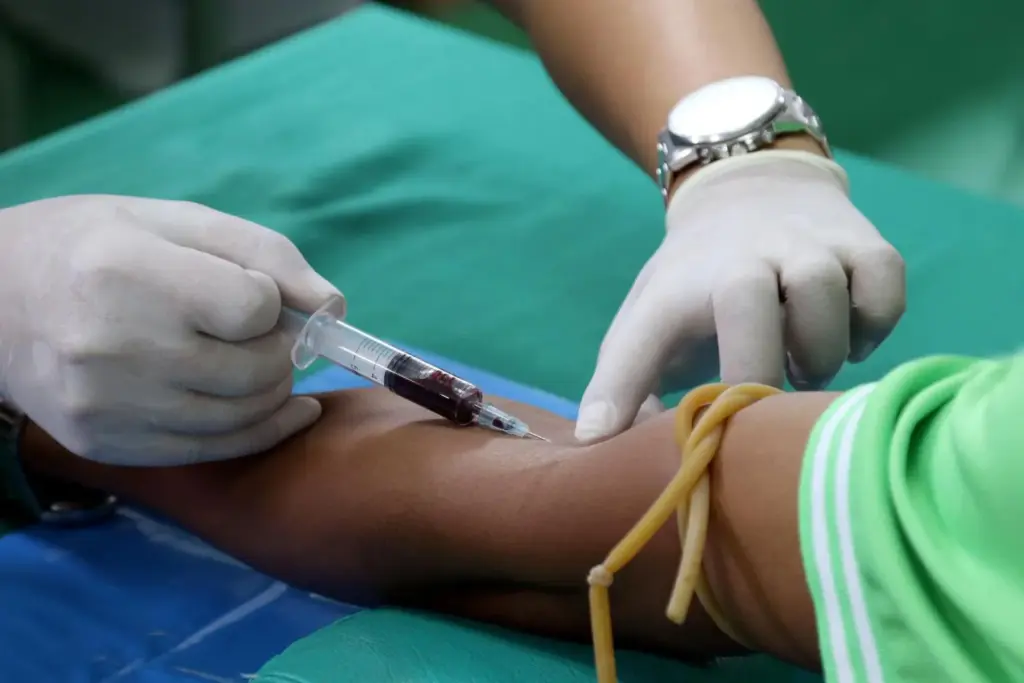
Blood donation centers have a strict process to keep donors and recipients safe. This includes checking who can donate, medical tests, and the donation itself.
Standard Eligibility Criteria
Specific eligibility criteria must be met to donate blood. You need to be at least 17 years old and weigh over 110 pounds. You must also be healthy and not have certain diseases like hemophilia.
The FDA sets these rules to protect everyone involved. Donors also have to pass a test to make sure they’re not anemic. They can’t have done things that might make them sick.
Medical Screening Procedures
Before you donate, you get a medical check-up. This includes a mini-physical, looking at your health history, and talking about risks. It’s important to make sure donating won’t hurt you.
They ask about your health, medicines, and recent activities. This helps decide if you can donate safely.
The Donation Experience
Donating blood is quick, taking about 10-15 minutes. You’ll be comfortable, and a clean needle will be used. The whole time, your safety and the blood quality are watched closely.
After, you get something to drink and advice on what to do next. This includes staying hydrated and not doing too much for a while.
The FDA has strict rules for donating. This means some people, like those with hemophilia, can’t donate. It keeps everyone safe and the blood supply good.
Blood Donation Regulatory Framework
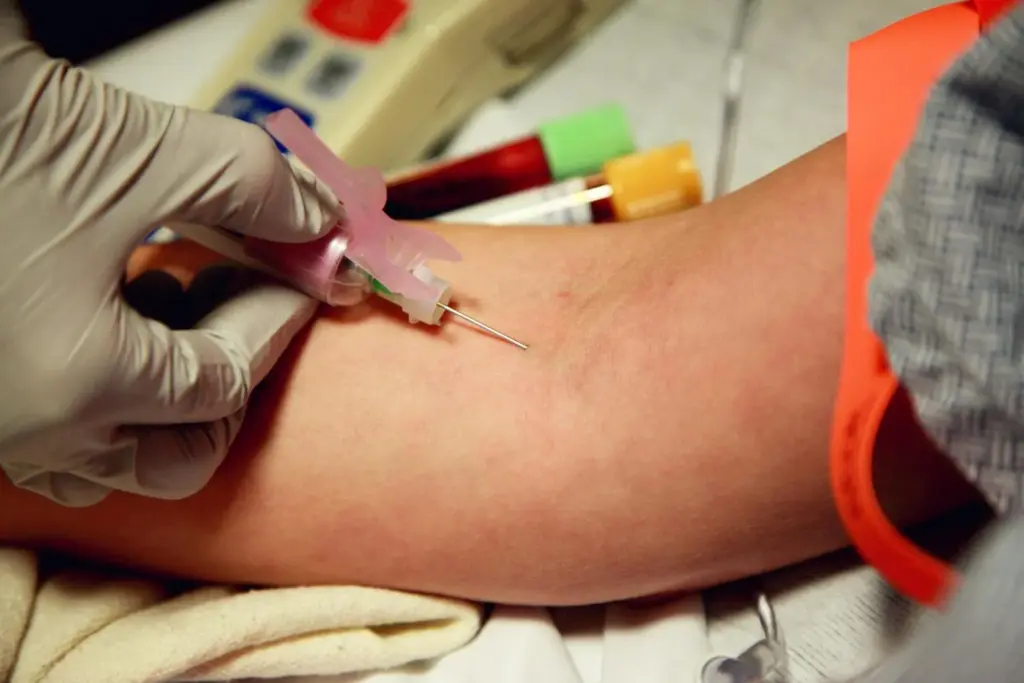
The rules for blood donation aim to keep both donors and recipients safe. They ensure a reliable blood supply. These rules come from national and international standards.
FDA Guidelines on Blood Donation
The FDA is key in the US for blood donation rules. FDA guidelines focus on safety, like who can donate and how blood is tested. They also cover good manufacturing practices for blood banks.
These rules change with new science and tech. For example, the FDA now requires nucleic acid testing (NAT) to find infectious diseases in blood.
International Standards and Practices
International standards also shape blood donation worldwide. Groups like the World Health Organization (WHO) and the International Society of Blood Transfusion (ISBT) set global standards. They help make blood donation practices the same everywhere.
These standards cover many areas, like who can donate and how blood is processed. Following these standards helps blood banks around the world keep blood safe and of high quality.
Evolution of Blood Donation Criteria
Blood donation rules have changed a lot over time. Medical science and society have both played big roles. For example, HIV screening in the 1980s made blood safer.
Now, rules are more detailed, considering things like travel and medical history. These updates help keep the blood supply safe while also making sure there’s enough blood to go around.
For people with hemophilia, donating blood is not allowed. This is to prevent too much bleeding from needles and protect their veins. It’s part of keeping everyone with bleeding disorders safe.
Regulatory agencies keep updating their rules based on new science. This keeps blood donation safe and effective. It’s important for facing new challenges and improving blood quality.
Why Hemophiliacs Cannot Donate Blood: Medical Perspective
Hemophiliacs can’t donate blood because of the risks their condition brings. We’ll look at why they can’t donate, focusing on the dangers to them, the risk of too much bleeding, and keeping veins healthy for treatment.
Risks to the Donor with Hemophilia
Donating blood is risky for people with hemophilia. The process can cause bleeding complications because their blood can’t clot well. This makes stopping the bleeding hard.
Some risks for hemophiliacs who donate include:
- Prolonged bleeding at the needle site, which can be hard to stop.
- Increased risk of hematoma formation due to bleeding into soft tissues.
- Potential for nerve damage or other problems at the venipuncture site.
Concerns About Excessive Bleeding
Excessive bleeding is a big worry for hemophiliacs. They face a high risk of bleeding not just during but also after donating. This can lead to delayed bleeding or re-bleeding, which is hard to manage without medical help.
The risks of too much bleeding are many:
- The immediate risk of bleeding during and after donation.
- The chance of long-term problems like chronic anemia or iron deficiency.
- The need for close medical watch to handle any bleeding episodes.
Vein Preservation for Treatment Access
Keeping veins healthy is key for hemophiliacs. They often need frequent treatments, like clotting factor replacement. Donating blood can harm their veins, making future treatments harder.
Vein preservation is important for several reasons:
- To keep reliable vascular access for treatments.
- To avoid venous complications that could limit treatment options.
- To ensure hemophiliacs can keep getting life-saving treatments.
In summary, the medical reasons for not letting hemophiliacs donate blood are clear. They face risks, concerns about too much bleeding, and need to keep their veins healthy for treatments. Understanding these points helps us see the challenges of managing hemophilia and why careful thought is needed in blood donation rules.
Safety Concerns for Blood Recipients
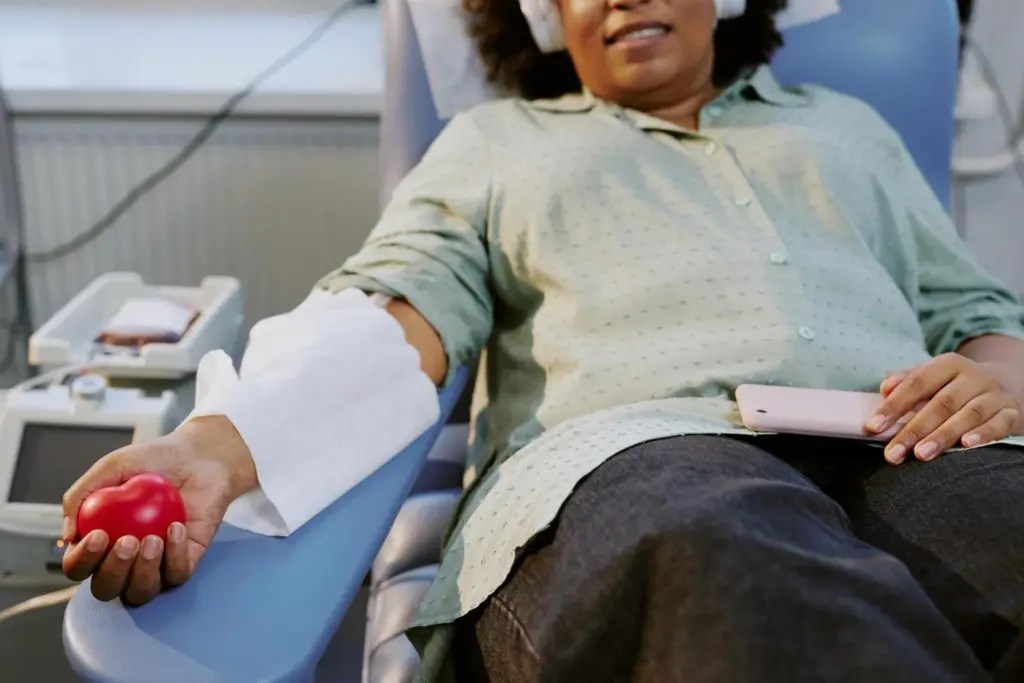
Blood transfusion safety is a top priority. We have many safeguards in place to protect recipients. The main goal is to keep the blood supply free from harmful substances. We do this through strict screening and testing.
Blood Quality Considerations
The quality of donated blood is key for recipient safety. Stringent donor screening helps identify and exclude risky donors. We look at their medical and travel history, and lifestyle factors.
Donated blood also gets tested for many pathogens, like viruses and bacteria. Nucleic acid testing (NAT) has improved virus detection, lowering transmission risks.
Transmission Risk Assessment
Even with these precautions, there’s a small chance of transmitting infectious agents. We keep working to lower this risk with better testing and surveillance. We look at disease rates in donors and how well our tests work.
Regulatory Safeguards
Regulatory agencies, like the FDA, are vital for blood safety. They set and enforce strict rules for blood donation and transfusion. These rules cover who can donate, how blood is tested, and quality control for blood banks.
Regulations also evolve to tackle new threats and use the latest safety technologies. This keeps the blood supply trustworthy and safe for recipients.
We keep improving our safety standards to protect blood recipients’ health. This way, we can reduce risks and ensure safe blood products.
VWD vs Hemophilia: Understanding the Differences
VWD and hemophilia are not just similar names; they have big differences in diagnosis and treatment. Both are bleeding disorders, but they need different ways to manage them.
Pathophysiology Comparison
Hemophilia A and B happen when there’s not enough clotting factors VIII and IX. VWD, on the other hand, is caused by a problem with von Willebrand factor (VWF). This key difference changes how we treat each condition.
Hemophilia mainly affects males because it’s on the X chromosome. VWD, though, can affect both males and females and is passed down in a different way. Knowing this helps with family planning and genetic counseling.
Symptom Variations
Both VWD and hemophilia can cause easy bruising and long bleeding times. But, VWD often leads to heavy menstrual bleeding in women, which is rare in hemophilia.
Hemophilia tends to cause more severe joint and muscle bleeds than VWD. The severity of bleeding can vary a lot among people with either condition.
Diagnostic Approaches
Diagnosing VWD and hemophilia involves clinical checks, lab tests, and sometimes genetic tests. For hemophilia, it’s about checking the levels of factor VIII or IX. VWD diagnosis looks at VWF levels and activity, and sometimes genetic tests.
Lab tests are key in telling these conditions apart, as their treatments are quite different.
Treatment Distinctions
Hemophilia treatment often means replacing the missing clotting factor. This can be for immediate bleeding or to prevent it. VWD treatment might include desmopressin, VWF concentrates, or other measures like antifibrinolytics.
The right treatment depends on the condition’s severity, the specific problem, and how the patient responds. Customizing treatment is vital for good care.
In summary, while VWD and hemophilia are both bleeding disorders, their differences in cause, symptoms, diagnosis, and treatment highlight the need for accurate diagnosis and personalized care.
Blood Donation Eligibility for Other Clotting Disorders
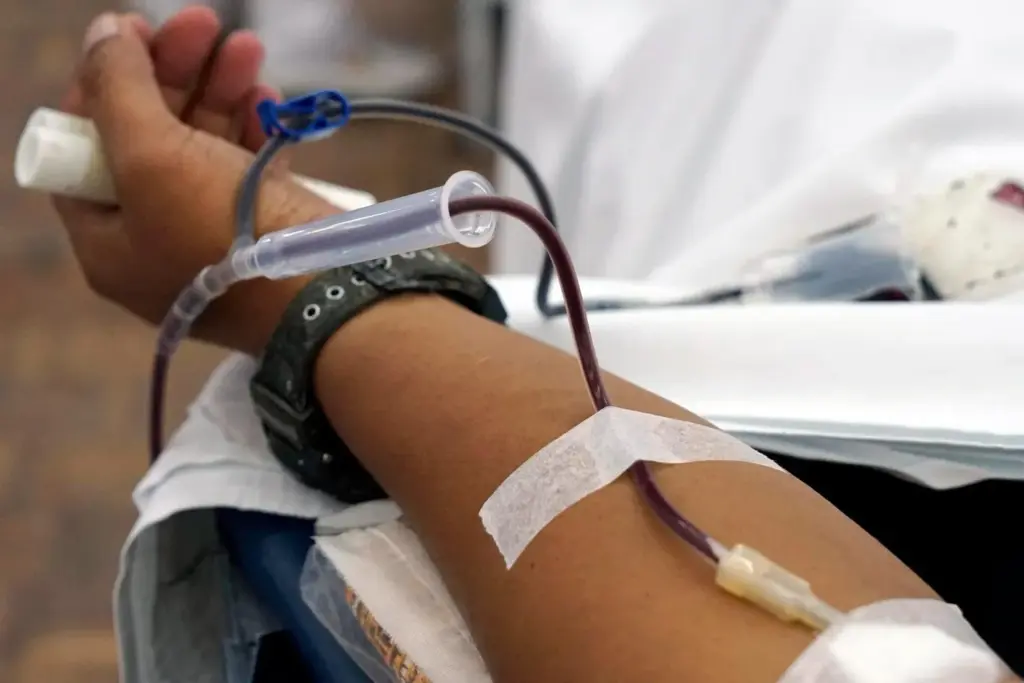
It’s important to know about different clotting disorders to understand blood donation rules. Hemophiliacs can’t donate blood, but others might have different rules.
Factor V Leiden and Blood Donation
Factor V Leiden raises the risk of blood clots. People with this condition usually can’t donate blood because of the risks. Studies say it’s a big worry for blood donation.
But, rules can change based on where you are. Some places might let people with Factor V Leiden donate plasma. This plasma is frozen and safe before use.
Von Willebrand Disease Considerations
Von Willebrand disease (VWD) affects how blood clots. It’s different from hemophilia because it’s about a missing protein. Who can donate blood with VWD depends on how bad it is and how well it’s treated.
People with mild VWD might donate blood if they meet certain criteria. But, those with severe VWD usually can’t because of bleeding risks.
Other Coagulation Disorders
Other clotting issues, like missing clotting factors or platelet problems, also affect blood donation. For example, some with mild clotting factor issues might donate under certain conditions. But, those with severe issues or platelet problems usually can’t.
The safety of both the donor and the person getting the blood is key. Rules from places like the FDA help decide who can donate based on their condition and how severe it is.
In short, donating blood with clotting disorders other than hemophilia depends on many things. These include the specific condition, how severe it is, and the rules in place. We need to look at these carefully to keep everyone safe.
Treatment Approaches for Hemophilia

Managing hemophilia well needs a full treatment plan. Hemophilia is a genetic disorder that makes blood clotting hard. Thanks to medical progress, treatments have improved a lot. This has made life better for those with hemophilia.
Clotting Factor Replacement Therapies
Clotting factor replacement therapy is key in treating hemophilia. It adds the missing clotting factor to the blood. This can be done with plasma-derived or recombinant clotting factor concentrates. Recombinant clotting factors are safer because they have a lower risk of infectious agents.
Choosing between plasma-derived and recombinant products depends on several things. These include what the patient prefers, the cost, and what’s available.
- Plasma-derived clotting factors come from human plasma and have been used for years.
- Recombinant clotting factors are made through genetic engineering, making them safer.
Prophylactic vs On-Demand Treatment
Hemophilia treatment can be either prophylactic or on-demand. Prophylactic treatment involves regular infusions to prevent bleeding. This is important for joints, as bleeding can cause chronic disease. On-demand treatment is given when bleeding happens to stop it.
- Prophylactic treatment is the best way to manage severe hemophilia. It helps prevent joint damage.
- On-demand treatment is used for acute bleeding. It can be life-saving in severe cases.
Emerging Treatment Options
New treatments for hemophilia are being developed. Gene therapy aims to fix the genetic defect causing hemophilia. Non-factor replacement therapies work differently to help blood clot.
- Gene therapy could be a cure for hemophilia by letting the body make the missing clotting factor.
- Non-factor replacement therapies offer new ways to treat hemophilia. They might mean fewer infusions and better results.
As research goes on, more treatment options for hemophilia will come. This could lead to better management and maybe even a cure.
The Role of Blood Transfusions in Hemophilia Treatment
Blood transfusions are key in treating hemophilia, a disorder that makes it hard for blood to clot. Treatment has changed, using new ways to handle bleeding and improve life for those with hemophilia.
When Transfusions Are Necessary
Transfusions are needed when there’s a big risk of bleeding or during an active bleed. Clotting factor replacement therapy helps prevent or treat bleeding. They are used in surgeries, severe injuries, or when there’s a high risk of bleeding due to clotting factor VIII or IX deficiency.
” This highlights the importance of having a comprehensive treatment plan that includes guidelines for blood transfusions.
Risks and Benefits
Choosing to use blood transfusions in hemophilia treatment means looking at the good and bad sides. Transfusions can stop or prevent bleeding, which is good. But, there are risks like getting infectious diseases or making antibodies against clotting factors.
- Benefits: Less bleeding, preventing joint damage, and better quality of life.
- Risks: Getting infectious diseases, making antibodies, and allergic reactions.
Modern Alternatives to Whole Blood Transfusion
New blood therapy has made whole blood transfusions less needed. Now, recombinant clotting factors or plasma-derived clotting factor concentrates are used. These are safer, reducing the chance of getting bloodborne diseases.
Prophylactic treatment regimens are becoming more common. They aim to prevent bleeding before it happens. This method has shown to cut down on bleeding episodes and better manage hemophilia.
“The evolution of hemophilia treatment has been remarkable, with significant advancements in clotting factor therapies and transfusion practices,” “These developments have transformed the management of hemophilia, providing patients with more effective and safer treatment options.”
Nucleic Acid Testing (NAT) and Blood Safety
The safety of the blood supply is a big deal in healthcare. Nucleic acid testing (NAT) is key to this. It has led to big steps forward in blood screening.
NAT is a detailed test that finds viruses and other pathogens in blood donations. It spots these pathogens early. This stops diseases from spreading through blood transfusions.
How NAT Works
NAT uses special methods to find and amplify genetic material. It can spot tiny amounts of virus genetic material. This makes it very good at checking blood donations.
The NAT process includes steps like taking a sample, extracting DNA, amplifying it, and detecting it. New tech has made these steps faster and more accurate.
Impact on Bloodborne Infection Rates
NAT has greatly lowered the risk of bloodborne infections. It finds pathogens in blood donations. This has cut down on diseases like HIV, hepatitis B, and C.
Studies show NAT has been a game-changer. It has made blood safer. Now, patients and healthcare workers can feel more confident.
|
Pathogen |
Pre-NAT Infection Rate |
Post-NAT Infection Rate |
|---|---|---|
|
HIV |
1 in 200,000 |
1 in 1,000,000 |
|
Hepatitis B |
1 in 50,000 |
1 in 300,000 |
|
Hepatitis C |
1 in 100,000 |
1 in 500,000 |
Future Developments in Blood Screening
New tech is coming, and it will change blood screening. Next-generation sequencing and multiplex NAT will make detection even better.
These new tools will keep the blood supply safe. As we learn more about diseases, our screening methods must keep up.
Living with Hemophilia: Daily Challenges
Living with hemophilia comes with daily challenges that need careful management. People with hemophilia face a complex mix of medical treatment, lifestyle changes, and psychological support. These are all important for their well-being.
Physical Limitations and Adaptations
Hemophilia can limit physical activities and mobility. To cope, people with hemophilia often make big lifestyle changes. For example, they might avoid sports that could cause injuries.
Regular exercise, like swimming or cycling, helps keep joints mobile and healthy. Making their living space safer is also key. Simple changes, like removing tripping hazards or installing handrails, can help prevent falls and injuries.
Wearing protective gear, like knee pads or elbow guards, can also offer extra protection during daily tasks.
Medical Management Strategies
Effective medical management is key for those with hemophilia. This includes prophylactic treatment with clotting factor concentrates to prevent bleeding. Regular infusions keep clotting factor levels up, reducing bleeding risks.
Having a plan for managing bleeding episodes is also important. Understanding when to use clotting factors and how to access emergency care is crucial for effective management. Regular check-ups with a hematologist or a hemophilia treatment center are essential to monitor the condition and adjust treatment plans.
Patient education on self-infusion techniques and bleed management empowers individuals to manage their condition. This improves their quality of life.
Psychological and Social Impacts
Hemophilia can deeply affect a person’s mental health and social life. The ongoing need for medical care can lead to anxiety or depression. Support from family, friends, and support groups is vital for coping with these emotional challenges.
Connecting with others who understand hemophilia can offer a sense of community and reduce feelings of loneliness. Psychological support from mental health professionals can also help. It aids in developing coping strategies and improving mental well-being.
Encouraging open talks about the emotional side of living with hemophilia can help reduce stigma. It promotes a more supportive environment.
Famous People with Hemophilia: Historical Perspective
Hemophilia has touched the lives of many famous people throughout history. This genetic disorder makes it hard for blood to clot. It has affected many families, including royal ones, leaving a big mark on their stories.
The Royal Connection: Queen Victoria’s Legacy
Queen Victoria was a key figure who carried hemophilia. She passed it to several of her kids. This spread the disorder to European royal families through marriages and inheritances.
- Prince Leopold, Duke of Albany, Queen Victoria’s son, who suffered from hemophilia.
- Tsarevich Alexei Nikolaevich of Russia, grandson of Queen Victoria through her daughter Alice, who had hemophilia.
- Infante Alfonso, Duke of Calabria, and Infante Gonzalo of Spain, descendants of Queen Victoria, who also had the condition.
Hemophilia was called the “Royal Disease” because of its presence in royal families. This shows how the disorder is genetic and affects many generations and places.
Notable Figures with Bleeding Disorders
Many famous people have lived with hemophilia or other bleeding disorders. They have brought attention to these conditions. Some examples include:
- Richard Burton, the renowned actor, who was known to have a mild form of hemophilia.
- The “Bleeder” Baseball Players, a group of baseball players in the early 20th century who suffered from various bleeding disorders, though not necessarily hemophilia.
These individuals have helped raise awareness about bleeding disorders through their lives and struggles.
Advocacy and Awareness Through Celebrity
Celebrities with hemophilia or affected by it have been key in advocacy. They share their experiences to:
- Educate the public about hemophilia and its implications.
- Reduce stigma associated with the condition.
- Support research and development of new treatments.
Through their efforts, they stress the need for more research, better treatments, and care for those with hemophilia.
We see how famous people with hemophilia have changed how we view the condition. Their stories show the challenges but also inspire hope and strength.
Specialized Healthcare for Hemophilia: Liv Hospital Approach
Liv Hospital focuses on treating hemophilia with a team effort and new healthcare methods. We know that treating hemophilia is more than just medicine. It’s about taking care of the whole person, including their feelings and mind.
Multidisciplinary Treatment Teams
Our teams are key to our hemophilia care. They include doctors, nurses, and physiotherapists. Together, they create plans that fit each patient’s needs.
This teamwork brings many benefits:
- Comprehensive Care: We cover all parts of hemophilia treatment, from medicine to physical therapy.
- Personalized Treatment Plans: We make plans that work best for each patient.
- Supportive Environment: Our teams make sure patients feel cared for and understood.
Innovative Healthcare Protocols
Liv Hospital always looks for new ways to treat hemophilia. Our methods aim to improve treatment results and quality of life for our patients.
Some of our new approaches include:
- Prophylactic Treatment: We use regular clotting factor infusions to prevent bleeding.
- Gene Therapy: We explore treatments that fix the genetic cause of hemophilia.
- Personalized Medicine: We tailor treatments to each patient’s unique needs.
Preventive and Curative Services
At Liv Hospital, we offer many services to manage hemophilia. Our preventive care includes regular checks and treatments. Our curative services include the latest in hemophilia treatment, like gene therapy.
|
Service |
Description |
Benefits |
|---|---|---|
|
Prophylactic Treatments |
Regular infusion of clotting factors |
Reduces frequency of bleeding episodes |
|
Gene Therapy |
Treatment aimed at correcting the genetic cause of hemophilia |
Potential for long-term or permanent cure |
|
Personalized Medicine |
Tailored treatment based on individual patient characteristics |
Optimizes treatment outcomes |
By combining these services, Liv Hospital aims to improve the lives of those with hemophilia. Our dedication to top-notch healthcare and support for international patients is strong.
Conclusion: Understanding Blood Donation Restrictions for Hemophiliacs
We’ve looked into hemophilia, a genetic disorder that causes bleeding issues. It affects millions globally. Knowing the rules about blood donation for those with hemophilia is key.
People with hemophilia can’t give blood because of health risks. The main concerns are too much bleeding and keeping veins for treatment. Rules from the FDA help keep everyone safe.
Even though hemophiliacs can’t donate blood, there are other ways to help. By learning about these rules, we support those with bleeding disorders better. This makes the blood donation process safer for everyone.
Our talk about hemophilia and blood donation shows the need for special healthcare. Places like Liv Hospital offer great support for those with bleeding disorders.
FAQ
What is hemophilia, and how does it affect blood donation?
Hemophilia is a genetic disorder that makes it hard for blood to clot. People with hemophilia can’t donate blood because it’s risky. They might bleed too much and could pass on their condition.
Can individuals with Von Willebrand disease donate blood?
No, people with Von Willebrand disease usually can’t donate blood. It’s because of the risk of passing on their condition and the chance of bleeding problems during donation.
What are the main differences between hemophilia and Von Willebrand disease?
Hemophilia affects the clotting factors VIII or IX. Von Willebrand disease deals with Von Willebrand factor, a key clotting protein. Both cause bleeding but are treated differently.
Are there any clotting disorders that allow blood donation?
Some clotting disorders, like Factor V Leiden, might not stop you from donating. But, it depends on the specific condition and how severe it is.
How does nucleic acid testing (NAT) impact blood safety?
NAT is a key part of blood screening. It finds genetic material of pathogens. This makes blood transfusions much safer by reducing infection risks.
What treatment options are available for hemophilia?
Treatments for hemophilia include clotting factor replacement. This can be given regularly to prevent bleeding or as needed for acute episodes. Gene therapy is also being researched.
Can people with hemophilia lead normal lives with proper management?
Yes, with the right treatment and care, people with hemophilia can live active lives. They can do most things without the condition getting in the way.
How does Liv Hospital approach the treatment of hemophilia?
Liv Hospital uses a team approach for hemophilia treatment. They offer both preventive and curative care. It’s all tailored to meet each patient’s needs.
Why are hemophiliacs unable to donate blood?
Hemophiliacs can’t donate blood because of the risks. They might bleed too much during donation. Also, they need to keep their veins healthy for treatment.
What are the daily challenges faced by individuals with hemophilia?
People with hemophilia face many daily challenges. They have to manage their physical limits, follow treatment plans, and deal with the emotional and social effects of their condition.
References
National Bleeding Disorders Foundation (NBDF) – HemAware. Can People with Bleeding Disorders Donate Blood? https://hemaware.org/fighting-you/can-people-bleeding-disorders-donate-blood
National Institutes of Health (NIH) – PMC. Safety of blood donation for people with inherited bleeding disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC6214824/
National Bleeding Disorders Foundation (NBDF). Blood & Blood Product Safety. https://www.bleeding.org/advocacy/federal-priorities/blood-and-blood-product-safety




































