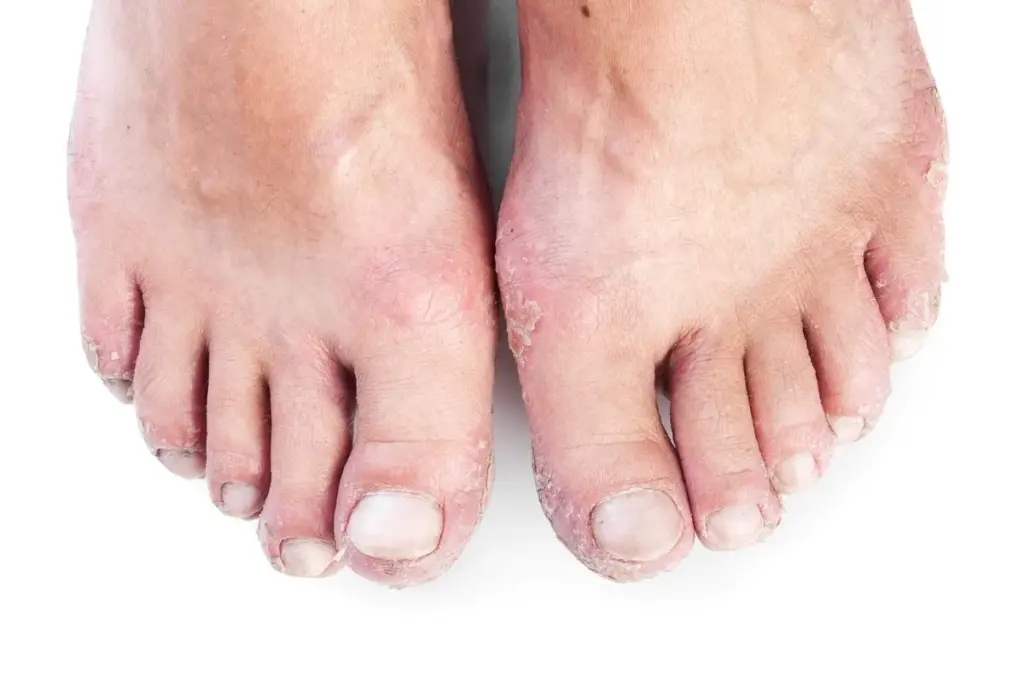
For people with diabetes, dry and itchy skin is a common problem. It affects almost 79 percent of those with diabetes mellitus. This issue can really disrupt daily life, so it’s important to know why it happens.
High blood sugar, poor blood flow, and nerve damage are the main reasons for dry, itchy skin in diabetics. Keeping blood sugar in check and using good skin care routines are key to avoiding these problems.
At Liv Hospital, we stress the need for full care for those with diabetes. Our approach is all about prevention and early action to tackle skin issues and boost overall health.
Key Takeaways
- Dry, itchy skin affects a significant majority of people with diabetes mellitus.
- High blood sugar, poor circulation, and nerve damage contribute to skin issues.
- Managing blood sugar levels is key to preventing skin problems.
- Good skin care routines can help reduce dryness and itchiness.
- Comprehensive care, like at Liv Hospital, supports overall patient well-being.
How Diabetes Affects Your Skin
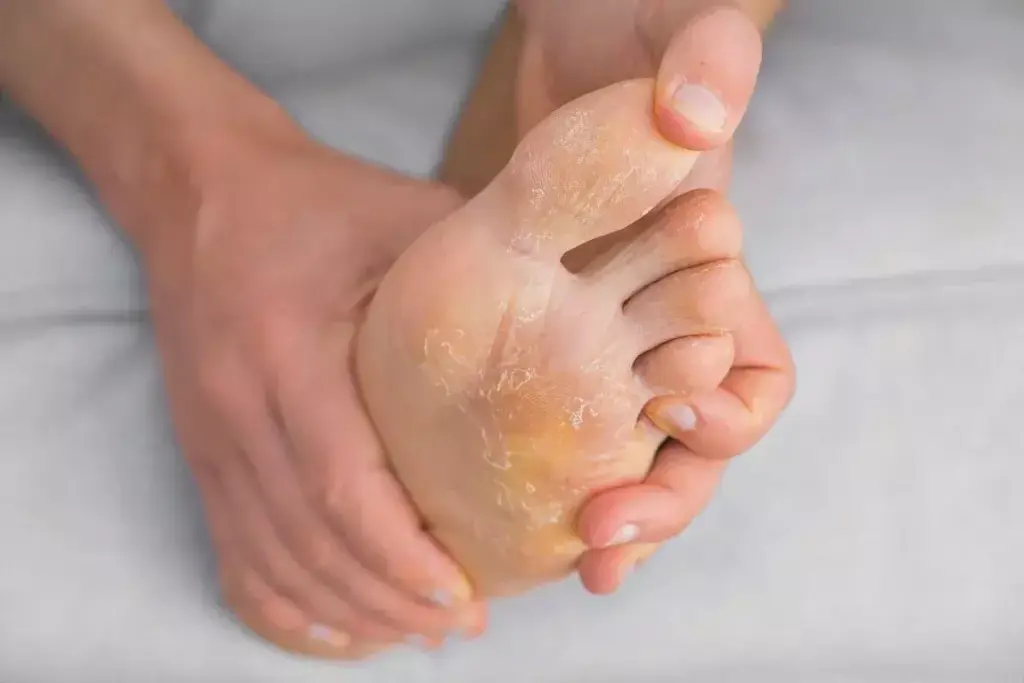
Managing diabetes means paying attention to its impact on your skin. High blood sugar, nerve damage, and poor circulation can cause skin problems. Let’s dive into how diabetes affects your skin health.
Skin Xerosis from Fluid Loss
High blood sugar makes your body lose fluid, causing dehydration. This leads to dry, itchy skin, known as xerosis. Excessive urination, a diabetes symptom, adds to fluid loss, making dry skin worse.
Diabetic neuropathy also reduces sweating, making skin drier. Dry skin is more prone to cracking and irritation. This can lead to infections if not treated right.
Diabetic Polyneuropathy and Nerve Damage
Diabetic polyneuropathy damages nerves that control sweating. This results in dry skin because the skin’s moisture barrier is broken. Numbness and tingling in hands and feet, common in neuropathy, make it hard to notice skin problems.
Poor Circulation and Reduced Blood Flow
Poor circulation is a diabetes complication that harms skin health. With less blood flow, skin gets fewer nutrients and oxygen. This makes skin more prone to damage and less able to heal.
Visible Skin Changes and Warning Signs
Visible skin changes can signal diabetes complications. Skin peeling on fingers, purple fingertips, and discolorations hint at poor circulation or nerve damage. Spotting these signs early can help manage diabetes-related skin issues.
In summary, diabetes impacts skin in many ways, from dryness and itchiness to nerve damage and poor circulation. Understanding these effects is key to managing diabetes well and keeping your skin healthy.
Main Causes of Diabetes Skin Itching and Dryness

Diabetes can cause skin issues like itching and dryness. These problems come from skin xerosis and nerve damage. Itching affects 18.4 to 27.5 percent of people with diabetes, making life harder.
We will look at the main reasons for skin itching and dryness in diabetes. We’ll give detailed explanations and examples. The main causes include:
Skin Xerosis from Fluid Loss
Skin xerosis, or dry skin, is common in diabetes. It happens because of fluid loss, made worse by high blood sugar. The body tries to get rid of extra glucose, leading to dehydration and dry, itchy skin.
Key factors contributing to skin xerosis include:
- High blood sugar levels
- Dehydration
- Poor skin care
Diabetic Polyneuropathy and Nerve Damage
Diabetic polyneuropathy is nerve damage in diabetes. It causes numbness, tingling, and itching. Nerve damage messes with nerve function, causing strange skin sensations.
The symptoms of diabetic polyneuropathy can vary, but common signs include:
- Numbness or tingling in the hands and feet
- Itching or burning sensations on the skin
- Sharp pains or cramps
Poor Circulation and Reduced Blood Flow
Poor circulation can also cause skin itching and dryness in diabetes. It makes it hard for the skin to heal and stay moist, leading to dryness and itchiness.
Factors that can worsen poor circulation include:
- Smoking
- High blood pressure
- High cholesterol
Visible Skin Changes and Warning Signs
Visible skin changes can signal diabetes complications. These include skin tags, bumps on the neck, and purple fingertips. Knowing these signs can help catch and manage problems early.
Some common visible skin changes associated with diabetes include:
- Skin tags or bumps on the neck
- Purple fingertips or toes
- Dry, cracked skin on the feet
Conclusion
Diabetes can lead to skin problems like itchy lower legs and skin tags on the neck. Keeping blood sugar levels in check is key to avoiding these issues. By controlling blood sugar, people can lower their risk of dry skin and other skin problems.
Good skin care is also important for those with diabetes. It means keeping the skin clean and moisturized. Avoiding extreme temperatures and watching for early signs of skin issues is also vital.
By managing blood sugar and taking care of the skin, people with diabetes can reduce skin problems. We urge everyone to watch their skin closely and seek medical help if they notice anything unusual.
FAQ
What are the common skin problems associated with diabetes?
People with diabetes commonly experience dry skin, fungal infections, bacterial infections, diabetic dermopathy, skin tags, and slow-healing wounds.
How does diabetes cause dry skin?
High blood sugar reduces moisture in the skin, damages nerves, and impairs circulation, leading to dryness, cracking, and itchiness.
What is diabetic polyneuropathy, and how does it affect the skin?
Diabetic polyneuropathy is nerve damage caused by high blood sugar. It can reduce sensation, making the skin prone to injuries, infections, and delayed healing.
Can diabetes cause skin tags or bumps on the neck?
Yes, insulin resistance can lead to skin tags, often appearing as small, soft bumps on the neck, armpits, or groin.
How can I prevent skin complications from diabetes?
Prevent skin problems by controlling blood sugar, moisturizing daily, practicing good hygiene, inspecting skin regularly, and promptly treating cuts or infections.
What are the warning signs of diabetes-related skin problems?
Warning signs include persistent dryness, redness, itching, slow-healing wounds, rashes, dark patches (acanthosis nigricans), or recurring infections.
Can poor circulation cause skin problems in people with diabetes?
Yes, poor circulation reduces nutrient and oxygen supply to the skin, making it more vulnerable to dryness, infections, and delayed wound healing.
How can I manage itchy skin caused by diabetes?
Manage itchy skin with moisturizers, gentle cleansers, keeping blood sugar in range, avoiding hot showers, and seeking medical treatment for infections or severe irritation.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC8465972/



































