
At Liv Hospital, we know how important dermoscopy is for better skin cancer detection. This tool helps us find cancer early and accurately. This leads to better health outcomes for our patients.
A 2023 Cochrane Review looked at 104 studies with over 42,000 lesions. It found that dermoscopy makes doctors 16% more sensitive and 20% more specific. This shows how valuable dermoscopy is in today’s dermatology.
We aim to give top-notch healthcare to everyone. We support international patients with the newest skin cancer detection methods.
Key Takeaways
- Adding dermoscopy to visual inspection improves sensitivity by 16% and specificity by 20%.
- Dermoscopy significantly enhances the accuracy of skin cancer detection.
- Liv Hospital is committed to providing world-class healthcare with complete support.
- The 2023 Cochrane Review analyzed 104 studies with over 42,000 lesions.
- Early diagnosis through dermoscopy improves patient outcomes.
What is a Dermoscopy?
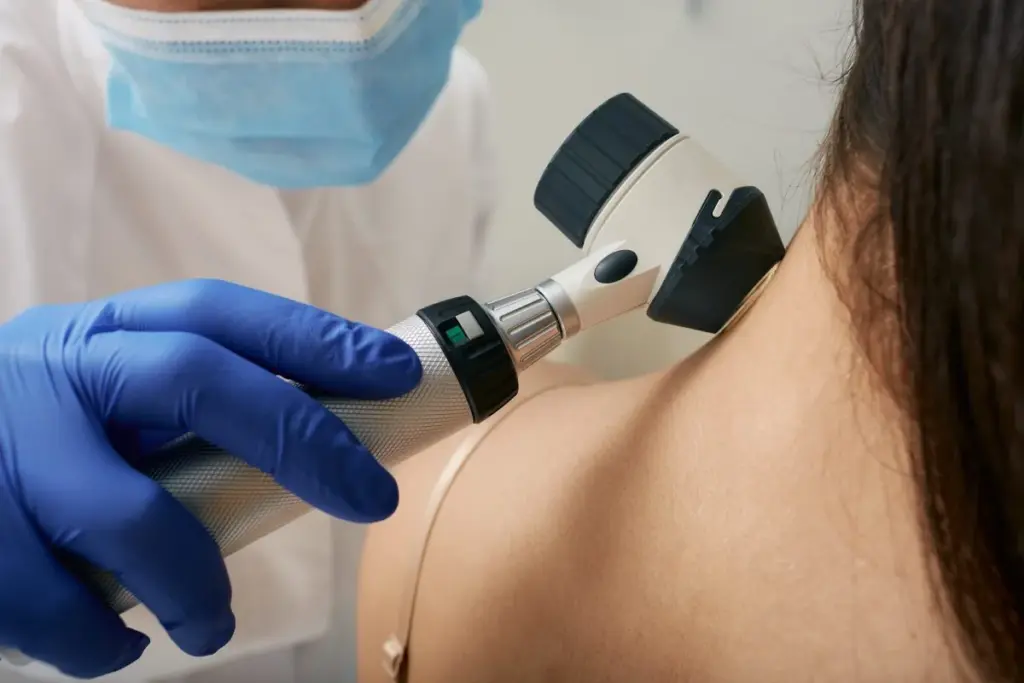
Dermoscopy is a way to see skin details that we can’t see with our eyes. It’s a non-invasive method used in dermatology. It helps doctors make more accurate diagnoses of skin problems.
Definition and Basic Principles
Dermoscopy uses a special tool called a dermatoscope to look at skin lesions. It works by lighting up the skin and making it bigger. This lets doctors see more details.
The Examination Process
The process of examining a skin lesion is done step by step. It’s designed to check the skin thoroughly.
Step-by-Step Procedure
First, a liquid like oil or gel is applied to the skin. This makes it easier to see deeper layers. Then, the dermatoscope is placed on the skin. The doctor looks at the lesion under magnification.
Patient Experience
Patients usually feel very little discomfort during the exam. It’s a painless and non-invasive process. This makes it a comfortable way to get a diagnosis.
|
Step |
Description |
|---|---|
|
1 |
Application of liquid interface |
|
2 |
Placement of dermatoscope |
|
3 |
Examination under magnification |
The Evolution of Dermoscopic Technology
Dermoscopy has grown a lot, making it better for diagnosing. New tech has made it more accurate and useful for skin exams.
Historical Development
Dermoscopy started in the early 1900s. But it really took off in the 1990s as a tool for doctors. At first, dermoscopes were just simple tools that made skin lesions look bigger.
Now, they have better optics and lights. This shows how much dermoscopy has improved over time.
Modern Advancements in Dermoscopy
Today, dermoscopy is way more advanced. We have digital dermoscopy and AI tools. Digital dermoscopy lets doctors save detailed images of skin. This helps them track changes in skin lesions.
AI tools help doctors spot skin problems like melanomas quickly. They make diagnosing more accurate.
|
Feature |
Traditional Dermoscopy |
Modern Dermoscopy |
|---|---|---|
|
Imaging |
Manual, non-digital |
High-resolution digital imaging |
|
Diagnostic Assistance |
Clinician-dependent |
AI-powered diagnostic tools |
|
Data Storage |
Limited, often manual recording |
Digital storage, easy comparison |
These new tools have made dermatology better. They help doctors make more accurate diagnoses. As tech keeps getting better, we’ll see even more advanced tools.
What is a Dermatoscope and How Does It Work?
A dermatoscope is a key tool in today’s dermatology. It gives a close-up look at skin lesions. This handheld device uses light and magnification to see more than the naked eye can.
Components of a Dermatoscope
A dermatoscope has a light source, usually LED, and a lens for magnification, from 3x to 10x. The light source shines on the skin lesion, and the lens lets us see it up close. Some models also have polarized light to cut down on glare from the skin.
Types of Dermoscopy Devices
Dermoscopy devices differ in what they can do. They mainly fall into contact and non-contact types, and digital dermoscopy systems.
Contact vs. Non-contact Dermatoscopes
Contact dermatoscopes need to touch the skin. They use a liquid or cross-polarized light for better views. Non-contact dermatoscopes let you examine without touching. This is good for sensitive areas or lesions.
Digital Dermoscopy Systems
Digital dermoscopy systems combine dermoscopy with digital images. This lets you save and compare images over time.
Dermoscopy Accuracy: The Statistical Evidence
Recent studies from the 2023 Cochrane Review have revealed new insights into dermoscopy’s accuracy. The review offers a detailed look at how well dermoscopy works in diagnosing skin conditions. It shows that dermoscopy has gotten better at spotting and confirming skin issues.
2023 Cochrane Review Findings
The 2023 Cochrane Review provides strong evidence about dermoscopy’s accuracy. It says dermoscopy is now a key tool in skin diagnosis, beating traditional methods. We’ll explore the review’s main points, focusing on how dermoscopy’s accuracy has improved.
Sensitivity and Specificity Improvements
Dermoscopy has made big strides in sensitivity and specificity. The review shows dermoscopy’s sensitivity went up by 16% to 92%. Specificity also rose by 20% to 95% for face-to-face checks. These numbers show how precise dermoscopy is in medical practice.
In-Person Evaluation Statistics
Face-to-face dermoscopy checks are very accurate. They have much higher sensitivity and specificity than just looking with the naked eye. This means dermoscopy helps doctors make more accurate diagnoses when they see patients in person.
Image-Based Dermoscopy Results
Image-based dermoscopy also has good results, but the numbers are a bit different. The review compares these results, showing what works well and what doesn’t in image-based assessments.
|
Evaluation Method |
Sensitivity (%) |
Specificity (%) |
|---|---|---|
|
In-Person Dermoscopy |
92 |
95 |
|
Image-Based Dermoscopy |
85 |
90 |
Which Statements Regarding the Skin Are Accurate in Dermoscopic Assessment?
Dermoscopic assessment has changed how we look at skin lesions. It lets us see details we can’t see with our eyes. This helps us make better diagnoses.
With dermoscopy, we can spot key signs that tell us if a lesion is benign or malignant. This is key for correct diagnoses and treatment plans.
Identifying Benign vs. Malignant Features
Dermoscopic assessment helps us tell benign from malignant features. Malignant lesions often have asymmetry, irregular borders, and color changes. Benign ones usually have symmetry and even color.
“The presence of specific dermoscopic features can significantly influence the diagnosis of skin lesions.” For example, seeing a pigment network, streaks, or globules can tell us if a lesion is benign or malignant. Knowing these signs is vital for accurate diagnosis.
Pattern Recognition in Skin Lesions
Pattern recognition is key in dermoscopic assessment. Recognizing patterns like the reticular, globular, or starburst patterns helps us diagnose skin lesions. “Pattern recognition is a skill that develops over time with experience and training.” It helps clinicians quickly understand a lesion’s nature and make decisions.
Combining the ability to spot benign vs. malignant features and recognizing patterns in skin lesions makes dermoscopic assessment more accurate. This leads to better patient care by catching skin cancers early.
Dermoscopy for Melanoma: Enhancing Early Detection
Early detection of melanoma is key, and dermoscopy is a big help. It lets doctors see more details in skin lesions. This way, they can spot things not seen by the naked eye.
Early Stage Melanoma Dermoscopy
Dermoscopy is great for catching melanoma early. It looks at the shape, color, and texture of lesions. This helps doctors find melanoma when it’s easier to treat.
Characteristic Dermoscopic Features of Melanoma
Melanoma has special signs that set it apart from harmless spots. Look for odd pigment patterns, different colors, and strange blood vessel shapes. Knowing these signs is key to spotting melanoma right.
ABCD Rule in Dermoscopy
The ABCD rule helps doctors check if a spot might be melanoma. It checks for Asymmetry, Border irregularity, Color variation, and Diameter. If a spot shows these signs, it’s likely to be checked further.
Seven-Point Checklist
The seven-point checklist is another tool for spotting melanoma. It looks for odd pigment patterns, a blue-white veil, and strange blood vessels. A score is given based on these signs, helping doctors decide what to do next.
|
Dermoscopic Feature |
Description |
Significance |
|---|---|---|
|
Asymmetry |
Lack of symmetry in the lesion |
High risk of melanoma |
|
Border Irregularity |
Notched, ragged, or irregular borders |
Suggests malignancy |
|
Color Variation |
Presence of multiple colors within the lesion |
Indicative of melanoma |
|
Diameter |
Lesion diameter greater than 6mm |
Potential indicator of melanoma |
Using these dermoscopic rules helps us find melanoma early. This leads to better treatment and outcomes for patients.
Visual Inspection vs. Dermoscopy: A Comparative Analysis
Dermoscopy is a key tool in skin exams, giving more detail than just looking. We’ll look at how these two methods compare, focusing on spotting skin cancer.
Limitations of Naked Eye Examination
Looking at skin with the naked eye is a basic method. It depends on the doctor’s skill to spot odd skin spots without tools. But, it’s not perfect.
Many skin cancers are hard to find early without better tools. The naked eye can miss small details, leading to late diagnosis. Research shows it’s not enough for skin cancer diagnosis.
Quantifiable Advantages of Dermoscopic Assessment
Dermoscopy gives a clearer view of skin spots. It uses a magnifying glass and light, helping doctors see more. This makes finding skin cancer easier.
Comparing visual checks to dermoscopy shows big differences. Here’s a quick look at what studies found:
|
Diagnostic Method |
Sensitivity |
Specificity |
|---|---|---|
|
Visual Inspection |
60-70% |
80-90% |
|
Dermoscopy |
85-95% |
90-95% |
Using dermoscopy helps doctors spot skin cancer better. It makes them less reliant on just looking.
Factors Influencing Dermoscopy Accuracy
The success of dermoscopy depends on many things. These include the skill of the healthcare provider and the technical details of the process. Knowing these factors helps make dermoscopy more accurate.
Clinician Experience and Training Impact
The skill of the clinician greatly affects dermoscopy’s success. Research shows that well-trained dermatologists make more accurate diagnoses. It’s important for clinicians to get thorough training in dermoscopy.
Technical and Procedural Considerations
Technical details also play a big role in dermoscopy’s accuracy. Things like the quality of the dermoscope, the lighting, and the use of contact mediums matter a lot.
Lighting and Contact Medium Factors
Good lighting and the right contact mediums are key for clear images. Bad lighting or wrong contact mediums can ruin the image quality. This can make it harder to make accurate diagnoses.
Documentation Quality
Keeping detailed records of dermoscopy findings is vital. Good documentation helps track changes in skin lesions. This is important for catching cancer early.
Reducing Unnecessary Biopsies: The Specificity Advantage
Dermoscopy is key in cutting down on unnecessary biopsies. It helps a lot in managing skin lesions. Getting the right diagnosis is very important.
From 70.6% to 84.6%: Understanding the Improvement
The accuracy of dermoscopy has gone up a lot. It’s now 84.6%, up from 70.6%. This means fewer people have to go through the stress of biopsies.
- Improved diagnostic accuracy
- Reduction in unnecessary procedures
- Enhanced patient care
Economic and Psychological Benefits
Dermoscopy’s role in reducing biopsies has big benefits. It saves money by cutting down on biopsies. It also makes patients feel less stressed and anxious.
Here’s a quick look at the benefits:
|
Benefits |
Description |
|---|---|
|
Economic Benefits |
Reduction in healthcare costs due to fewer biopsies |
|
Psychological Benefits |
Reduced stress and anxiety for patients |
Limitations and Challenges in Dermoscopic Diagnosis
Dermoscopy is very useful but faces challenges in some cases. It’s key to know its limits to better diagnose skin cancers.
When Dermoscopy May Be Less Effective
In some cases, dermoscopy might not work as well. This is true for nonspecific or atypical lesions. Early melanomas or those with regression structures can be hard to spot.
“Diagnosing melanoma can be tough, like when the lesion looks plain or doesn’t fit the usual pattern,” experts say.
Overcoming Common Diagnostic Pitfalls
To tackle these issues, doctors need to know the common mistakes in dermoscopy. They should watch out for false negatives and false positives. These can cause delays or wrong treatments.
By using dermoscopy with clinical wisdom and sometimes histopathology, we can get better at diagnosing. Training and experience are also vital for doctors to keep up with new techniques and improve their skills.
As we move forward in dermoscopy, it’s important to recognize its limits and work to overcome them. This will help us give the best care to our patients.
Advanced Applications and Future Directions
Dermoscopy is on the verge of a big change. This is thanks to new tech like artificial intelligence and teledermoscopy. These tools are going to change how we diagnose skin problems a lot.
Teledermoscopy and Remote Diagnosis
Teledermoscopy is another big step forward. It lets doctors check skin problems from far away. This means patients don’t always have to come in for a visit.
Accessibility Improvements
Teledermoscopy makes it easier for people in far-off places to get skin care. They don’t have to travel far to see a doctor.
Accuracy of Remote Assessment
Research shows teledermoscopy works well when AI is used too. This mix of tech makes remote checks very reliable. It’s a big step for the future of skin diagnosis.
As we go on, using AI and teledermoscopy will be key. They will help make diagnosis more accurate, accessible, and better for patients.
Conclusion
Dermoscopy has changed the game in dermatology. It lets doctors look closely at skin lesions. This helps find skin cancer early, making treatments more effective.
It’s great for reducing unneeded biopsies and making diagnoses more accurate. At Liv Hospital, we use the latest dermoscopic tech. This ensures our patients get top-notch care.
In short, dermoscopy is key in the battle against skin cancer. It combines doctor skills with new tech for better patient care. We’re all in at Liv Hospital, working hard to give our patients the best care possible.
FAQ
What is dermoscopy and how does it aid in skin cancer detection?
Dermoscopy is a non-invasive way to look at skin lesions. It uses a special microscope. This helps find skin cancer, like melanoma, more accurately.
How accurate is dermoscopy in detecting melanoma?
A 2023 Cochrane Review found dermoscopy is very good at spotting melanoma. It’s better than just looking with the naked eye.
What are the characteristic dermoscopic features of melanoma?
Melanoma shows certain signs under the microscope. These include irregular pigment patterns and atypical blood vessels. Doctors use rules like the ABCD rule to check these.
How does dermoscopy reduce unnecessary biopsies?
Dermoscopy is better at telling if a spot is cancerous. This means fewer unnecessary biopsies. It also saves money and reduces stress.
What factors influence the accuracy of dermoscopy?
Many things affect how well dermoscopy works. These include the doctor’s skill, the equipment used, and how well the skin is lit. Good pictures are also important.
What are the advancements in dermoscopic technology?
New tech includes digital dermoscopy and AI tools. These make diagnosis better and let doctors check patients remotely.
How does Liv Hospital utilize dermoscopy in patient care?
Liv Hospital uses dermoscopy to find skin cancer. We aim to give top-notch care to our patients from around the world.
What is the difference between contact and non-contact dermatoscopes?
Contact dermatoscopes need gel or oil and touch the skin. Non-contact ones use polarized light for a look without touching.
Can dermoscopy be used for remote diagnosis?
Yes, new tech lets doctors diagnose remotely. This makes getting expert skin care easier for more people.
What are the limitations of dermoscopy?
Dermoscopy might not work as well for very small spots or those that look the same everywhere. Its success also depends on the doctor’s skill and the equipment used.
References
National Center for Biotechnology Information (NCBI): https://pmc.ncbi.nlm.nih.gov/articles/PMC11460753/


































