
Gestational diabetes mellitus (GDM) is a condition where high blood glucose levels occur during pregnancy. It affects over 7% of pregnancies in the United States. Understanding GDM is key for both the mother and the baby’s health.
Understanding GDM is critical for expectant mothers. It helps them make informed choices about their pregnancy and childbirth. The American College of Obstetricians and Gynecologists sees GDM as a major concern.
The debate on when to start labor for GDM patients is ongoing. Some suggest early labor induction. But, the decision should be based on each woman’s health and how the baby is growing.
Key Takeaways
- Gestational diabetes mellitus (GDM) affects over 7% of pregnancies in the United States.
- GDM is a significant concern due to its complications for both mother and baby.
- The decision to induce labor should be individualized based on factors like glycemic control and fetal growth patterns.
- Understanding GDM is critical for expectant mothers to make informed decisions about their pregnancy and childbirth.
- The clinical debate surrounding labor timing for GDM patients is ongoing.
Understanding Gestational Diabetes: Definition and Prevalence
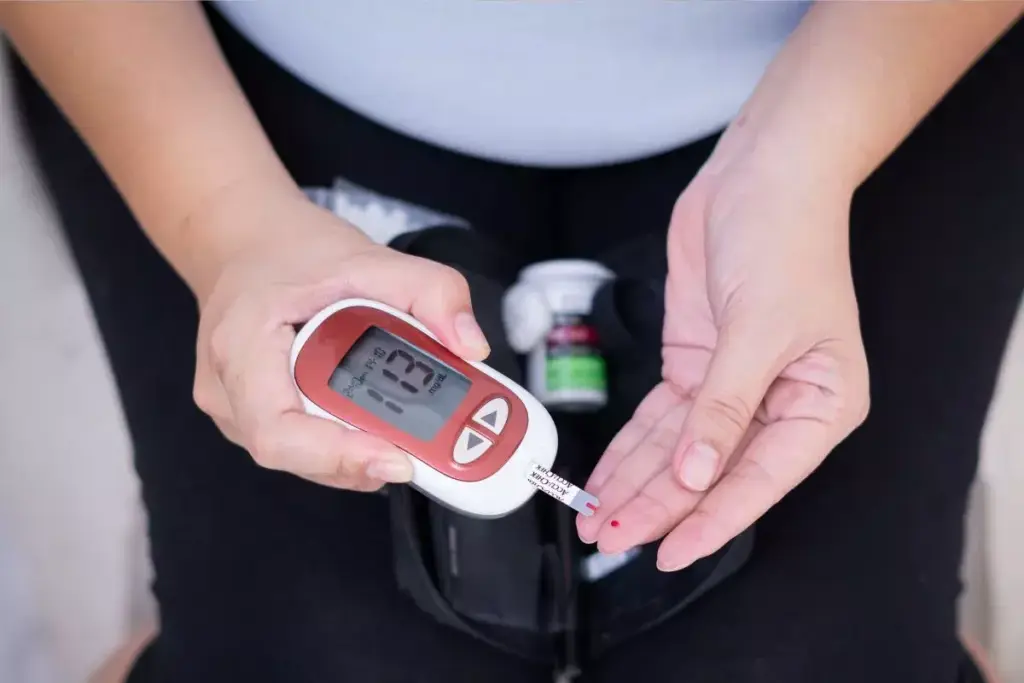
Gestational diabetes mellitus (GDM) is a big health issue during pregnancy. It’s when blood sugar levels get too high during pregnancy. It’s different from other diabetes because it starts during pregnancy in women who didn’t have it before.
What Does GDM Mean?
GDM is short for Gestational Diabetes Mellitus. It means diabetes that starts during pregnancy. Knowing what GDM is helps manage it better.
How Common Is Gestational Diabetes in the United States?
The CDC says about 7% of pregnancies in the U.S. have GDM. This shows GDM is quite common in pregnant women. The exact number can change based on who is studied and how diabetes is diagnosed.
Risk Factors and Diagnosis
Some risk factors make getting GDM more likely. These include:
- Obesity
- A family history of diabetes
- A previous history of GDM in a prior pregnancy
- Age over 35 years
- A history of delivering a macrosomic (large birth weight) baby
To find GDM, a test is done between 24 and 28 weeks of pregnancy. The glucose challenge test (GCT) is often used first. If that shows high sugar levels, a glucose tolerance test (GTT) is done next.
Spotting and treating GDM early is key to avoid problems for mom and baby. Knowing the risks and how to diagnose helps doctors take action early.
Gestational Diabetes Induced Labor: Evaluating the Evidence

Looking into induced labor for gestational diabetes needs a deep dive into current studies. Managing gestational diabetes mellitus (GDM) affects both mom and baby. Healthcare providers must decide between inducing labor or waiting it out.
The Clinical Debate: Induction vs Expectant Management
The debate on labor induction for GDM patients is complex. It weighs the risks against the benefits. Inducing labor is considered when the pregnancy risks are too high.
For women with GDM, risks like big babies, preeclampsia, and cesarean deliveries are big concerns.
Key considerations include:
- The gestational age at diagnosis
- The level of glycemic control achieved
- The presence of other pregnancy complications
Studies show that inducing labor at 38-39 weeks can lower cesarean rates for some GDM patients. But, the choice to induce must be made on a case-by-case basis.
Research Findings for First-Time Mothers
For first-time moms with GDM, research on labor induction is mixed. Some studies suggest inducing at 39 weeks can lower cesarean rates without increasing other risks.
Research Findings for Women with Previous Births
Women with GDM who have had babies before might have different outcomes with labor induction. Research shows that those who have had a vaginal birth before might have a lower cesarean risk.
What Systematic Reviews Show About Routine Induction
A Cochrane Database systematic review found no solid evidence for routine induction in GDM. It stressed the importance of personalized care plans.
The main point is that while there’s evidence for considering labor induction in GDM, it should be based on each patient’s unique situation and preferences.
Timing Considerations: Risks and Benefits of Different Approaches
Women with gestational diabetes need to know the risks and benefits of different labor timing approaches. Managing gestational diabetes means controlling blood sugar and deciding when to deliver. These decisions are critical for their care.
Risks of Inducing Labor Before 39 Weeks
Inducing labor before 39 weeks can harm the baby. Studies show it leads to more NICU admissions and neonatal jaundice. These risks are key when deciding on labor timing for women with gestational diabetes.
NICU Admission Rates: Babies born before 39 weeks often need NICU care. This is because their lungs and other organs are not fully developed.
Average Week of Delivery with Gestational Diabetes
The delivery week for women with gestational diabetes varies. It depends on diabetes severity, other pregnancy issues, and doctor advice. Women with well-controlled diabetes might go to term. Those with complex cases might need labor induced between 38 and 39 weeks.
Can You Give Birth Naturally with Gestational Diabetes?
Yes, many women with gestational diabetes can have a natural birth. It depends on blood sugar control, pregnancy complications, and mother and baby health. Well-managed pregnancies increase the chance of a vaginal delivery.
Does Gestational Diabetes Cause Early Labor?
Gestational diabetes itself doesn’t cause early labor. But, it increases the risk of pregnancy complications. These might include preeclampsia and fetal macrosomia, leading to early delivery.
| Gestational Age | Risks Associated with Induction | Benefits of Waiting to Term |
| Before 39 Weeks | Increased NICU admissions, neonatal jaundice | Reduced risk of stilbirth, more spontaneous labor |
| 39-40 Weeks | Lower NICU admission rates, fewer neonatal complications | Optimal fetal development, lower risk of complications |
Conclusion
Our study on gestational diabetes and induced labor shows how complex it is. The choice to induce labor depends on many factors. It’s about what’s best for each woman, based on her health and what she wants.
Research shows that not all women with gestational diabetes need to be induced. But, for some, it might help. The American College of Obstetricians and Gynecologists suggests inducing labor at 40 weeks for these women.
Studying gestational diabetes and labor timing is key. It’s about weighing the risks and benefits. This helps women make smart choices about their care.
In the end, we want the best for both mom and baby. By looking at all the evidence and each woman’s situation, doctors can create good plans. This helps manage gestational diabetes well.
FAQ
What is gestational diabetes mellitus (GDM)?
Gestational diabetes mellitus (GDM) is a condition in which blood sugar levels become high during pregnancy. It usually develops in the second or third trimester and typically goes away after delivery.
How common is gestational diabetes in the United States?
Gestational diabetes affects about 6% to 9% of pregnancies in the United States. The risk may increase due to factors such as obesity, family history, or older maternal age.
Does gestational diabetes require induced labor?
Gestational diabetes does not always require induced labor. Induction may be recommended if blood sugar levels are not well controlled or if there are concerns about the baby’s health.
What are the risks of inducing labor before 39 weeks in women with gestational diabetes?
Inducing labor before 39 weeks may increase the risk of breathing problems, feeding difficulties, and other complications in newborns. Doctors usually recommend waiting unless there is a medical reason.
What is the average week of delivery for women with gestational diabetes?
Many women with gestational diabetes deliver between 38 and 40 weeks. The exact timing depends on blood sugar control and the overall health of the mother and baby.
Can you give birth naturally with gestational diabetes?
Yes, many women with gestational diabetes can have a natural vaginal birth. Proper blood sugar management and regular monitoring during pregnancy are important.
Does gestational diabetes cause early labor?
Gestational diabetes does not always cause early labor, but poorly controlled blood sugar can increase the risk of complications that may lead to earlier delivery.
What does DMA1 mean in the context of gestational diabetes?
DMA1 refers to gestational diabetes that is managed through diet and lifestyle changes without medication. It indicates that blood sugar levels can be controlled through non-medication methods.
REFERENCE
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK545196/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























