The oral mucosa acts as a shield between the outside world and our body’s inner parts. It’s made up of stratified squamous epithelium. This layer is built to handle the wear and tear of daily life. Wondering “what type of epithelium makes up the oral mucosa?” This guide gives the surprising answer (stratified squamous) and explains why.
This stratified squamous epithelium has four layers. It keeps the inside of our mouth safe. At Liv Hospital, we focus on the details of oral epithelium. This helps us diagnose and treat mouth problems better.
Key Takeaways
- The oral mucosa is composed of stratified squamous epithelium.
- This epithelium is a multilayered structure that protects underlying tissues.
- It is designed to withstand mechanical stress within the oral cavity.
- Understanding oral epithelium is key to diagnosing mouth issues.
- Knowing about oral mucosa helps us find the right treatments.
The Fundamental Structure of Oral Mucosa

The oral mucosa acts as a shield against many stresses. It has several layers, with the epithelium being the outermost. This layer faces the outside environment of the mouth.
Basic Components and Layers
The oral mucosa includes the epithelium, lamina propria, and basement membrane. The epithelial layer changes in thickness and keratinization based on its location. For example, the gingiva and hard palate have thicker, keratinized epithelium for better protection.
The lamina propria is a thin layer of tissue under the epithelium. It, along with the epithelium and basement membrane, makes up the mucosa. The lamina propria supports the epithelium and helps with nutrient and waste exchange.
Protective Functions and Adaptations
The oral mucosa protects against mechanical, chemical, and microbial threats. The epithelial layer is specially adapted for the mouth’s harsh conditions. Its thickness and keratinization level affect its protective strength.
In areas like the gingiva and hard palate, the epithelium is keratinized for extra protection. But, the buccal and labial mucosa, less exposed to friction, has a non-keratinized epithelium.
Relationship to Underlying Tissues
The oral mucosa is closely linked with the tissues beneath it, like the lamina propria and bone or muscle. The basement membrane, a thin layer, connects the epithelium to the lamina propria. It’s vital for the mucosa’s integrity.
The bond between the oral mucosa and the tissues below is key for oral health. Damage to this bond can cause serious problems.
What Type of Epithelium Makes Up the Oral Mucosa: A Comprehensive Overview
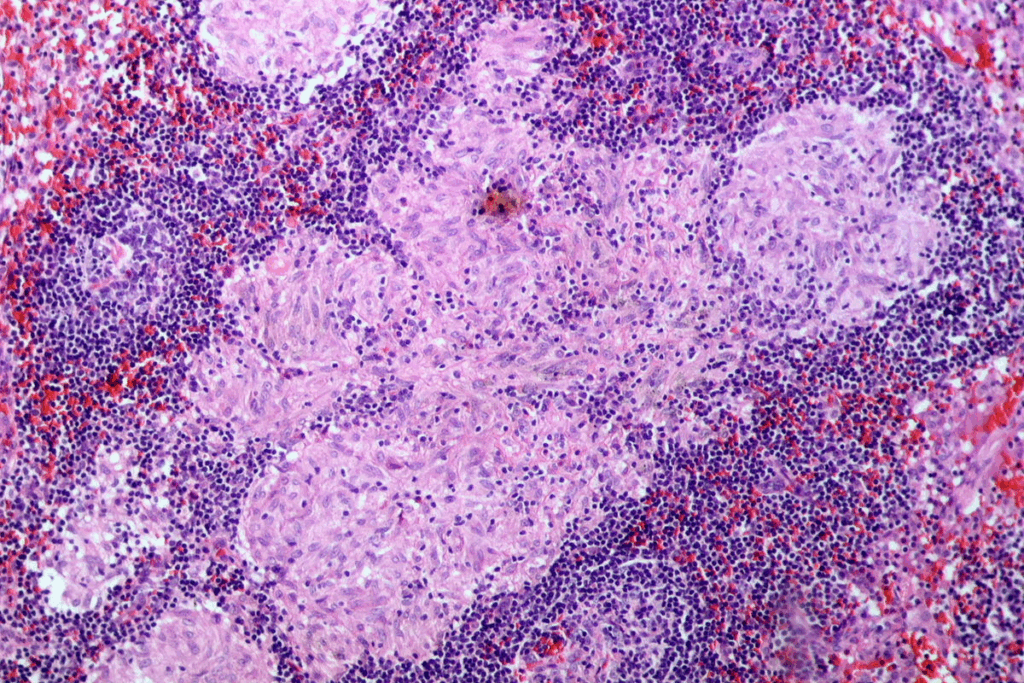
The oral mucosa is covered by stratified squamous epithelium. This tissue is perfect for the oral environment’s stresses. It’s key for the mucosa’s protection and function.
Stratified Squamous Epithelium: Definition and Characteristics
Stratified squamous epithelium is a multi-layered tissue. It has squamous-shaped cells in each layer. This tissue adapts well to wear and tear, like the oral cavity.
This tissue protects against forces, chemicals, and microbes. Its layers help in continuous renewal and adaptation.
Keratinized vs. Non-keratinized Variants
The oral mucosa has three types based on the epithelium: masticatory, lining, and specialized. Keratinized epithelium is in high-stress areas like the gingiva and hard palate.
Non-keratinized epithelium is in areas needing flexibility, like the buccal mucosa and the floor of the mouth. The table below shows the differences:
Type of Mucosa | Epithelial Characteristics | Location |
Masticatory Mucosa | Keratinized Stratified Squamous Epithelium | Gingiva, Hard Palate |
Lining Mucosa | Non-keratinized Stratified Squamous Epithelium | Buccal Mucosa, Floor of the Mouth |
Specialized Mucosa | Varied Epithelial Characteristics | Dorsum of the Tongue |
Cellular Organization and Specialization
The oral mucosa’s cells change as they move up. This change involves cell shape and protein expression.
“The oral epithelium is a dynamic tissue that undergoes continuous renewal, with cells being constantly replaced through a process of proliferation, differentiation, and desquamation.”
The tongue’s dorsum has taste buds and special structures. These are key for taste. The oral epithelium’s complexity shows its role in health and function.
Histological Features of Oral Epithelium
Understanding the oral epithelium’s histological features is key to knowing its role in the mouth. The oral mucosa epithelium is a complex layer of cells. It acts as a barrier against mechanical, chemical, and microbial threats.
Cell Layers and Their Organization
The oral epithelium has several cell layers, each with its own role. The basal layer, the deepest, is where cell growth and change happen. As cells get older, they move up, changing in structure and function.
The cells in the epithelium are very close together, with little space between them. This close packing helps block external factors. The way these layers are organized is key to keeping the oral mucosa strong.
Intercellular Junctions and Adhesion Mechanisms
Intercellular junctions are vital for the oral epithelium’s cohesion and barrier function. These junctions, like desmosomes, tight junctions, and gap junctions, help cells stick together and talk to each other.
Desmosomes help cells stick together well, even under stress. Tight junctions, by contrast, close the space between cells, stopping molecules and ions from passing through.
Epithelial Cell Differentiation Process
Epithelial cell differentiation is a complex process. It involves many molecular and cellular changes. As cells differentiate, they change shape and get special functions.
The epithelium sits on a basement membrane, which supports it. This membrane separates the epithelium from the connective tissue below, the lamina propria. The lamina propria has blood vessels, lymphatic vessels, and immune cells. These help keep the oral mucosa healthy and functioning well.
The Three Classifications of Oral Mucosa
We identify three main types of oral mucosa, each with its own role. These types are based on their functions, showing how important they are for our mouth’s health and how it works.
Lining Mucosa: Non-keratinized Epithelium
The lining mucosa has a smooth, slippery surface. It helps food and other things move easily in our mouth. You can find it on the cheeks and lips, where it needs to be flexible.
Characteristics of lining mucosa include:
- Non-keratinized stratified squamous epithelium
- High degree of flexibility
- Presence in areas like the cheeks and lips
Masticatory Mucosa: Keratinized Epithelium
The masticatory mucosa is in places that face a lot of pressure, like the gums and hard palate. It has keratinized epithelium, making it strong and able to handle chewing forces.
Characteristics | Masticatory Mucosa | Lining Mucosa |
Epithelial Type | Keratinized | Non-keratinized |
Location | Gingiva, Hard Palate | Buccal, Labial Mucosa |
Function | Withstands mastication forces | Facilitates movement |
Specialized Mucosa: Taste and Sensory Function
The specialized mucosa is mainly on the tongue’s top. It has taste buds for tasting food. This mucosa is all about sensing flavors, which is key to our taste experience.
The different types of oral mucosa show how complex and adaptable our mouths are. Knowing about these types helps us understand how our mouths work and stay healthy.
Regional Variations in Oral Epithelium
The oral epithelium changes a lot from one area to another. This is because different parts of the mouth have different jobs. Knowing about these changes helps us understand how the mouth works.
Buccal and Labial Mucosa Characteristics
The cheeks and lips are covered by a special kind of skin called the buccal and labial mucosa. This skin is thin and flexible. It moves with the mouth and face.
Key Features of Buccal and Labial Mucosa:
- Non-keratinized epithelium
- Highly vascularized lamina propria
- Presence of elastic fibers for flexibility
Palatal Epithelium: Hard vs. Soft Palate
The hard palate has a tough, keratinized skin that sticks to the bone. The soft palate has softer skin. This shows how each part of the palate does different things.
Characteristics | Hard Palate | Soft Palate |
Epithelial Type | Keratinized, Stratified Squamous | Non-keratinized, Stratified Squamous |
Attachment | Tightly bound to underlying bone | More flexible, not directly attached to bone |
Gingival Epithelium and Dentogingival Junction
The gingiva, or gums, have a tough skin that protects the teeth. The dentogingival junction is where the gums meet the teeth. It helps keep bacteria out.
The gingival epithelium’s keratinization and tight adhesion to the tooth surface are essential for maintaining periodontal health.
Lingual Epithelium: Dorsal vs. Ventral Surfaces
The tongue’s top side has special skin with papillae and taste buds. The bottom side is smooth and thin. This difference helps the tongue do its job.
Knowing about the different types of skin in the mouth is important. Each part is made for its own job. This helps keep the mouth healthy.
Supporting Structures and Microenvironment
The oral epithelium’s microenvironment has many parts working together. This complex setup is key for the epithelium to function well. It’s vital for keeping the mouth healthy.
Basement Membrane: Composition and Function
The epithelium sits on a basement membrane, a thin, fibrous layer. It’s made of two parts: the basal lamina and the reticular lamina. This membrane helps keep the epithelium strong and lets nutrients and waste pass through.
Lamina Propria: Papillary and Reticular Layers
Underneath the basement membrane is the lamina propria, a layer of connective tissue. It supports the epithelium. The lamina propria has two parts: the papillary layer near the epithelium and the reticular layer deeper down.
It’s filled with collagen fibers, capillary networks, and immune cells. These elements help protect and adapt the oral mucosa.
Vascular Networks and Nutrient Supply
The oral mucosa has many vascular networks. These networks give the epithelium the nutrients and oxygen it needs. They also help remove waste.
The blood vessels are close to the epithelium. This helps nutrients get to the cells fast and waste gets removed quickly. This supports the fast turnover of epithelial cells.
Immune Components Within Oral Mucosa
The oral mucosa has immune components like lymphocytes and macrophages. These cells are important for fighting off pathogens. They are found in the lamina propria and epithelium, ready to act fast.
Having these immune cells is essential for the oral cavity’s health.
Epithelial Turnover and Regenerative Capacity
The oral epithelium can repair itself every day. This is key to keeping the mouth healthy. It helps the oral mucosa stay strong and work well.
Cell Renewal Rates in Different Regions
Cell renewal rates change in the mouth. The gingiva and hard palate renew cells faster because they face more stress. This helps them adapt to different needs in the mouth.
Studies found that renewal rates depend on keratinization and the tissue type. For example, the buccal mucosa has a different rate than the gingiva.
Stem Cell Populations in Oral Epithelium
Stem cells are vital for the mouth’s repair. They keep the epithelium fresh and are found in certain areas. Their work is key to keeping the mouth healthy and fixing it when needed.
Scientists have been studying these stem cells a lot. Knowing how they work helps us understand how the mouth heals itself.
Healing Mechanisms Following Injury
The mouth heals quickly after injury. This healing involves many cells, growth factors, and the matrix around them. First, cells move and grow to cover the wound. Then, the epithelial layer is fully restored.
How fast the mouth heals depends on the injury, infections, and overall health. Knowing this helps us find better ways to heal wounds in the mouth.
Factors Affecting Epithelial Regeneration
Many things can affect the mouth’s ability to heal. Age, diet, and diseases like diabetes can slow healing. Diabetes, for example, can hurt blood flow and change how the body reacts to injury.
Smoking and drinking alcohol also harm the mouth’s healing. Knowing this helps us find ways to keep the mouth healthy.
Clinical Significance of Oral Epithelium Structure
Understanding the oral epithelium’s structure is key for diagnosing and treating oral health issues. This structure is vital for keeping our mouths healthy. It has big implications for how we practice medicine.
Common Pathological Conditions
The oral mucosa faces many health problems, like infections and autoimmune diseases. For example, oral lichen planus is a chronic condition that causes mouth lesions and pain.
There are several types of oral mucosal disorders, including:
- Oral candidiasis
- Oral lichen planus
- Pemphigus vulgaris
- Oral squamous cell carcinoma
Diagnostic Approaches for Mucosal Disorders
Diagnosing oral mucosal disorders needs a detailed approach. This includes clinical exams, tissue analysis, and sometimes more tests. We use different tools to find the cause of oral lesions.
Diagnostic Approach | Description | Clinical Application |
Clinical Examination | Visual inspection and palpation of oral mucosa | Initial assessment of lesions and mucosal changes |
Histopathological Analysis | Microscopic examination of tissue samples | Definitive diagnosis of mucosal disorders |
Immunohistochemistry | Identification of specific proteins in tissue samples | Diagnosis of autoimmune disorders and cancer |
Therapeutic Considerations Based on Regional Variations
Treatment for oral mucosal disorders varies based on the condition, its severity, and the area affected. We tailor treatment plans to the unique features of each oral mucosal region.
For instance, the buccal mucosa epithelium is non-keratinized, making it more prone to certain issues. On the other hand, the masticatory mucosa is keratinized, providing a stronger surface for chewing.
Oral Mucosa as a Drug Delivery Route
The oral mucosa is a promising route for drug delivery because of its accessibility and rich blood supply. We are looking into using it for systemic drug delivery, which is useful for conditions needing quick absorption.
Using the oral mucosa for drug delivery has several benefits, including:
- Rapid absorption into the bloodstream
- Avoidance of first-pass metabolism
- Non-invasive delivery method
As we learn more about the oral epithelium, we see its importance in health issues and drug delivery.
Conclusion
The oral mucosa is a key part of our mouth’s health. We’ve looked at what makes it up and how it changes in different areas. The main part of the oral mucosa is a type of skin called stratified squamous epithelium.
This skin can be either keratinized or non-keratinized, depending on where it is and what it does. Knowing this helps us understand its importance in keeping our mouths healthy.
The oral mucosa can get sick in many ways. Its structure and how it works are important for finding and treating these problems. This knowledge helps doctors and dentists give better care to their patients.
The ability of the oral mucosa to heal itself is also very important. Things like how fast cells grow back and the presence of stem cells matter a lot. By understanding these things, healthcare workers can take better care of people with mouth problems.
FAQ
What type of epithelium makes up the oral mucosa?
The oral mucosa is made of stratified squamous epithelium. This is a layer that protects the tissues below. It also handles mechanical stress well.
What is the difference between keratinized and non-keratinized oral epithelium?
Keratinized epithelium is in areas that face a lot of stress, like the gingiva and hard palate. Non-keratinized epithelium is in areas that need to be flexible, like the buccal and labial mucosa.
How does the thickness of the epithelial layer vary in different regions of the oral cavity?
The thickness of the epithelial layer changes based on the area’s function. The palate and gingiva have thicker layers to handle more stress.
What is the role of the lamina propria in supporting the oral epithelium?
The lamina propria is a layer of connective tissue under the epithelium. It supports, nourishes, and defends the epithelium. It does this through its blood vessels and immune cells.
How does the oral mucosa regenerate after injury?
The oral mucosa can quickly heal because of stem cells and fast cell renewal. Nutrition and health also play a part in this process.
What are the clinical implications of understanding the structure of the oral epithelium?
Knowing how the oral epithelium is structured is key for diagnosing and treating mucosal disorders. It’s also important for finding new treatments, like using the mucosa for drug delivery.
What is the function of the basement membrane in the oral mucosa?
The basement membrane is a thin layer of extracellular matrix. It’s vital for the oral epithelium’s integrity and function. It helps cells attach and influences their behavior.
How do regional variations in oral epithelium affect its function?
The oral epithelium’s regional variations, like differences in keratinization and thickness, help it adapt to various functions. This includes mastication, speech, and sensation.
What is the significance of the oral epithelium in maintaining oral health?
The oral epithelium acts as a barrier against pathogens and mechanical stress. It’s essential for oral health. Any dysfunction or disease can lead to oral pathologies.
References
National Center for Biotechnology Information. Oral Mucosa: Stratified Squamous Epithelium Composition. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK572115/



































