
Seeing unusual changes on your lips, like white patches, can worry you. These patches, called leukoplakia, can be harmless or might show signs of cancer. At Liv Hospital, we help you tell the difference between normal and lip cancer signs.
Explaining when a White patch on lip cancer (leukoplakia) should be immediately checked by a healthcare provider.
In the U.S., about 40,000 people get lip cancer each year. Getting it treated early is key. We offer top-notch care for patients from around the world. Spotting symptoms of lip cancer, like sores that won’t heal, is vital.
Key Takeaways
- White patches on lips, or leukoplakia, can be benign or precancerous.
- Lip cancer is relatively rare but requires early detection for effective treatment.
- Recognizing symptoms like persistent sores or changes in lip appearance is critical.
- Liv Hospital provides international standards of medical excellence for lip cancer diagnosis and treatment.
- Timely medical evaluation is essential for optimal prognosis.
Understanding White Patches on Lips
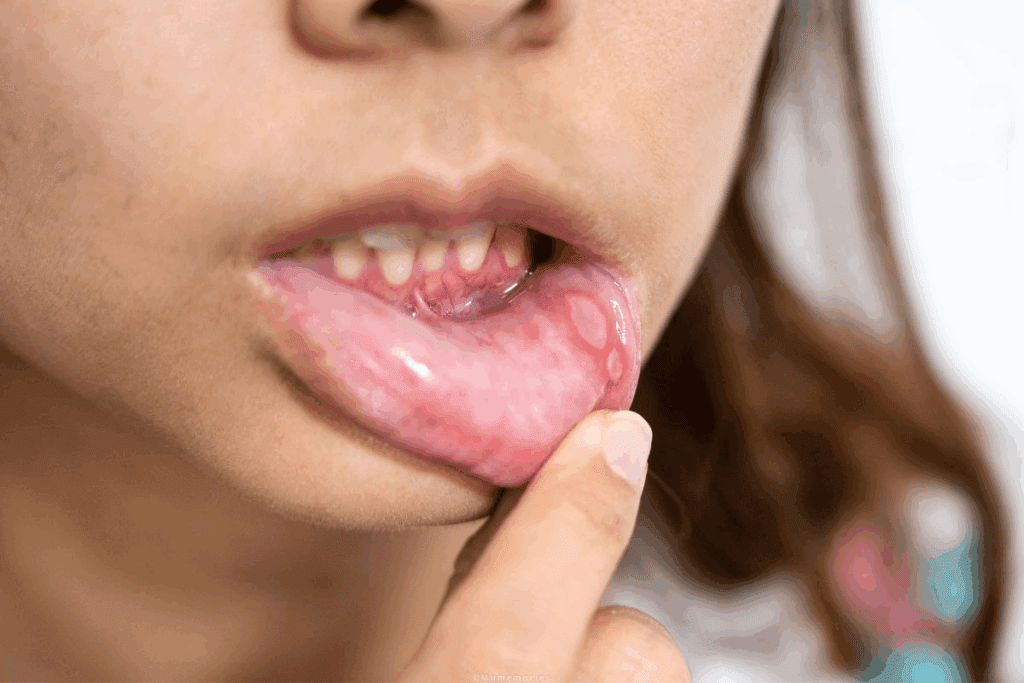
Leukoplakia is a condition that shows up as white patches on the mucous membranes, like the lips. It’s important because it can be a sign of oral health issues. These patches can be caused by many things, from harmless irritations to signs of cancer.
Knowing what these white patches look like is key. Their size, shape, and any symptoms they cause help figure out what they are and how to treat them. We’ll look at what these patches usually look like, how common they are, and their link to lip cancer.
What is Leukoplakia?
Leukoplakia is when white or gray patches show up on the mucous membranes, like the lips, tongue, and cheeks. These patches can be flat or slightly raised and come in different sizes. While often harmless, they can sometimes lead to cancer, so it’s important to watch for any changes.
The exact reason for leukoplakia isn’t always known. But it’s linked to long-term irritation, tobacco use, and other irritants. Sometimes, it’s a sign of a bigger health issue that needs doctor’s attention.
Common Characteristics of White Patches
White patches from leukoplakia can look different. They might be:
- Flat or slightly raised
- White or grayish in color
- Painless or uncomfortable
- Solitary or multiple
These traits can hint at what they might be and if they could be cancerous. It’s important to see a doctor for a proper diagnosis.
Prevalence and Statistics
Research shows leukoplakia is more common in some groups, like tobacco users. The number of people with leukoplakia varies worldwide, with more cases in places where people smoke more.
| Population | Prevalence of Leukoplakia |
|---|---|
| Tobacco users | Higher prevalence |
| Non-tobacco users | Lower prevalence |
Knowing these numbers helps us understand the risks of white patches on the lips. It shows why catching them early and keeping an eye on them is so important.
Benign Causes of White Patches on Lips

White patches on lips can worry us, but often they’re not serious. Knowing what causes them can ease our minds and help us find the right treatment.
Oral Thrush and Fungal Infections
Oral thrush is a fungal infection caused by Candida species. It shows up as white patches on the lips, tongue, and in the mouth. It can happen if our immune system is weak, we’ve taken antibiotics, or we don’t clean our mouth well.
Treatment: Doctors usually give antifungal meds for oral thrush. Keeping our mouth clean and fixing health problems can stop it from coming back.
Fordyce Spots and Sebaceous Glands
Fordyce spots are small, yellowish or white bumps on the lips, cheeks, and genitals. They happen because of visible sebaceous glands, which are part of our skin.
Significance: Fordyce spots are harmless and don’t need treatment. They might bother us because of how they look, but they’re not dangerous.
| Condition | Causes | Treatment |
|---|---|---|
| Oral Thrush | Fungal infection | Antifungal medications |
| Fordyce Spots | Visible sebaceous glands | None required |
| Oral Lichen Planus | Autoimmune condition | Corticosteroids, immune modulators |
Oral Lichen Planus
Oral lichen planus is an autoimmune disease that causes white, lacy patches on the lips and inside the mouth. It can also lead to red, inflamed areas and ulcers.
“Oral lichen planus is a chronic condition that requires management to alleviate symptoms and prevent complications.”
Management: Doctors might use corticosteroids and other meds to reduce inflammation and manage symptoms.
Trauma and Irritation
White patches can also come from physical trauma or irritation to the lips. This might happen from biting ourselves, dental work, or irritation from sharp teeth or dental appliances.
Prevention: Staying away from further irritation and keeping our mouth clean can help fix white patches from trauma.
Learning about the common, non-serious reasons for white patches on lips helps us deal with them better. It reduces worry and ensures we get the right care.
When White Patch on Lip Cancer Becomes a Concern
White patches on the lips can be harmless. But, some conditions and risk factors can make them precancerous or cancerous. It’s important to know these factors to understand the situation.
Precancerous Conditions
Leukoplakia and erythroplakia are precancerous conditions that raise the risk of lip cancer. Leukoplakia shows up as white patches that can’t be scraped off. Erythroplakia is red patches. A study in the Journal of Oral Pathology found that leukoplakia can turn into oral squamous cell carcinoma.
“The presence of leukoplakia and erythroplakia should prompt further investigation to rule out malignancy.” – Oral Pathology Journal
These conditions often come from chronic irritation. They can lead to cancer if not treated early. Regular checks and early treatment are key to managing them.
Risk Factors for Malignancy
Several factors can make a white patch on the lip more likely to be cancerous. These include:
- Tobacco use: Smoking or chewing tobacco greatly increases the risk of lip cancer.
- Heavy alcohol consumption: Drinking too much alcohol can lead to oral cancer, including lip cancer.
- UV radiation exposure: Long-term exposure to UV radiation from the sun or tanning beds can damage the lips and increase cancer risk.
Knowing and reducing these risk factors can help prevent lip cancer. For example, using lip balm with SPF can protect against UV radiation.
Mixed Red and White Patches
Mixed red and white patches, known as speckled leukoplakia, are concerning. They have a higher risk of being precancerous or cancerous than white or red patches alone. It’s important to have these patches checked by a healthcare professional to find out what they are and what to do next.
Early detection and diagnosis are critical for managing potentially cancerous white patches on the lips. If you notice any unusual changes or persistent patches, it’s best to see a doctor.
Types of Lip Cancer
Lip cancer is a complex condition with several types. Each type has its own characteristics and treatment approaches. Knowing these types is key for diagnosis and treatment planning.
Squamous Cell Carcinoma
Squamous Cell Carcinoma (SCC) is the most common lip cancer. It comes from squamous cells on the lip. SCC can grow and spread if not treated quickly.
It can happen on the upper or lower lip, but the lower lip is more common. Risk factors include sun exposure, smoking, and HPV. Symptoms include a sore, lump, or growth on the lip.
Basal Cell Carcinoma
Basal Cell Carcinoma (BCC) is another skin cancer type that can appear on the lips. It’s less common here than on other face areas. BCC grows slowly and rarely spreads.
It’s more likely to appear on the upper lip. The main risk factor is UV radiation from the sun or tanning beds. It looks like a small, shiny bump or pink patch on the lip.
Melanoma of the Lip
Melanoma is a serious skin cancer that can happen on the lips. It starts from melanocytes and can be aggressive. Melanoma on the lip is rare but dangerous because it can spread fast.
Risk factors include fair skin, sunburns, and family history of melanoma. It looks like a new or changing mole on the lip.
A study in the Journal of the American Academy of Dermatology shows early detection of melanoma improves survival. “Melanoma of the lip, though rare, needs quick recognition and treatment because of its aggressive nature,” says Medical Expert, a dermatologist.
| Type of Lip Cancer | Common Location | Risk Factors |
|---|---|---|
| Squamous Cell Carcinoma | Lower lip | Sun exposure, smoking, HPV |
| Basal Cell Carcinoma | Upper lip | UV radiation |
| Melanoma | Any area of the lip | Fair skin, sunburns, family history |
Knowing the different types of lip cancer is key for effective management and treatment. Each type has its own characteristics and risk factors. This highlights the need for personalized medical care.
Recognizing Warning Signs of Lip Cancer
Knowing the early signs of lip cancer is key to managing it. Early detection makes treatment much more effective. It’s important for patients to be aware of these symptoms.
Visual Changes to Watch For
Visual signs are often the first clue to lip cancer. These include:
- White or red patches on the lips that do not heal
- Sores or ulcers that persist
- Changes in the color or texture of the lips
Physical Symptoms
There are also physical symptoms to watch for. These include:
- Numbness or tingling sensation on the lips
- Pain or difficulty swallowing
- Swelling or lumps on the lips
Early Stage Cancer White Spots on Lips
White spots on the lips can be an early sign of cancer. They are more concerning if they don’t go away or if other symptoms appear. It’s important to watch for any changes and get medical help if needed.
| Symptom | Description |
|---|---|
| White or Red Patches | Patches that do not heal and may be a sign of precancerous conditions or cancer. |
| Sores or Ulcers | Lesions that persist and do not heal normally. |
| Numbness or Tingling | Abnormal sensations that can indicate nerve involvement. |
Spotting these warning signs early and getting medical help quickly can greatly improve treatment outcomes. If you see any of these symptoms, it’s vital to see a doctor for a proper check-up.
Cancer Inside Lip vs. Outer Lip Cancer
It’s important to know the difference between cancer inside the lip and outer lip cancer. This knowledge helps in diagnosing and treating the disease effectively. Lip cancer can appear in different ways and places, with different characteristics depending on its location.
Oral Cancer Inside Lip
Oral cancer inside the lip, or inner lip cancer, happens on the inner mucous membrane. It’s often linked to tobacco use and alcohol consumption. Symptoms include sores that don’t heal, pain, and trouble swallowing.
A study in the Journal of Oral Pathology and Medicine found a link between oral cancer and tobacco and alcohol use. The risk grows with how often and long you use these substances.
“The majority of oral cancers are associated with tobacco and alcohol use, and the risk increases with the frequency and duration of use.”
Journal of Oral Pathology and Medicine
Skin Cancer on Lips
Skin cancer on the lips happens on the outside and is linked to prolonged sun exposure. The most common types are squamous cell carcinoma and basal cell carcinoma. Look out for changes in the skin, like new or changing moles, or sores that don’t heal.
- Squamous cell carcinoma is a common type of skin cancer that can occur on the lips.
- Basal cell carcinoma is another type that is often found on sun-exposed areas.
Differences in Symptoms and Treatment
The symptoms and treatments for cancer inside the lip and outer lip cancer are different. Oral cancer inside the lip might need surgery, radiation, or chemotherapy, based on the stage and severity. On the other hand, skin cancer on the lips is usually treated with surgery. Sometimes, topical treatments or photodynamic therapy are used.
| Cancer Type | Common Symptoms | Typical Treatments |
|---|---|---|
| Oral Cancer Inside Lip | Sores, pain, difficulty swallowing | Surgery, radiation, chemotherapy |
| Skin Cancer on Lips | Changes in skin appearance, new moles | Surgical excision, topical treatments |
In conclusion, knowing the differences between cancer inside the lip and outer lip cancer is key for the right diagnosis and treatment. If you notice any unusual changes or symptoms, see a healthcare professional for the right evaluation and care.
When to Seek Medical Attention
Don’t ignore signs on your lips; knowing when to seek help is key. If you notice unusual or lasting changes, see a healthcare professional.
Concerning Symptoms That Shouldn’t Be Ignored
Some lip health symptoms need immediate medical care. These include:
- Persistent sores or lesions that don’t heal in a few weeks.
- Numbness or pain in or around the lip area.
- Swelling or thickening of the lip.
- Changes in appearance, such as white or red patches, or unusual bleeding.
If you see any of these concerning symptoms, make an appointment with your healthcare provider.
What to Expect at Your Appointment
Your healthcare provider will examine your lips and mouth closely. They’ll also ask about your health history, like smoking or too much sun.
Your doctor might look at your lips and possibly take a biopsy if they find something odd. A biopsy is when they take a small tissue sample for tests.
Knowing what to expect can make you feel less anxious and more ready for your visit.
Diagnosing White Patches and Lip Tumors
Diagnosing lip tumors and white patches involves several steps. We aim for accurate identification and the right treatment. When a patient shows white patches or lip tumors, we start a detailed diagnostic process.
Initial Examination
The first step is a thorough initial examination. We look closely at the lip and mouth for any oddities. This includes white patches, redness, or swelling. We also check the patient’s medical history and risk factors, like smoking or sun exposure.
“A thorough initial examination is key to figuring out the next steps in diagnosis and treatment.”
Biopsy Procedures
If we find suspicious lesions or white patches, we might do a biopsy. A biopsy takes a small tissue sample for a microscope check. There are a few biopsy types, like incisional and excisional biopsies.
Biopsy results tell us if the growths are cancerous. This helps us decide on the next steps in treatment.
Imaging and Staging
After confirming lip cancer or tumor, we use imaging to see how far it has spread. CT scans, MRI, or PET scans help us understand the tumor’s size and if it has spread. Knowing the cancer’s stage is vital for planning treatment.
“Accurate diagnosis and staging are key to choosing the best treatment for lip cancer and improving patient outcomes.”
We combine findings from the initial check, biopsy, and imaging to give a full diagnosis. This helps us create a treatment plan that fits the patient’s needs.
Treatment Options for Lip Cancer
The treatment for lip cancer depends on several things. These include the cancer’s stage and the patient’s health. Knowing about these options helps patients make better choices about their care.
Surgery for Upper and Lower Lip Cancer
Surgery is often the first step in treating lip cancer. The goal is to remove the tumor and affected tissue while keeping the lip’s function and look as much as possible. The type of surgery depends on the tumor’s size and where it is.
Radiation Therapy
Radiation therapy is also a key treatment for lip cancer, mainly for early-stage cancers. This treatment uses high-energy rays to kill cancer cells. It can be used alone or with surgery. It’s great for cancers that are sensitive to radiation.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells. For lip cancer, it might be used with other treatments like surgery or radiation. The choice of chemotherapy depends on the cancer type and stage, and the patient’s health.
Targeted and Immunotherapies
Targeted therapy and immunotherapy are newer ways to treat lip cancer. Targeted therapy uses drugs that target cancer cells, harming normal cells less. Immunotherapy boosts the body’s immune system to fight cancer better. These treatments are promising for advanced or recurrent lip cancer.
It’s important for patients to understand the different treatments for lip cancer. This helps them make informed decisions about their care. We work closely with patients to find the best treatment plan for their needs and health.
Survival Rates and Prognosis
Lip cancer has a good chance of recovery if caught early. This shows how vital it is to seek medical help quickly. Knowing about survival rates and what affects them helps both patients and doctors make better choices.
Early vs. Advanced Stage Outcomes
The outlook for lip cancer patients changes a lot based on when they get diagnosed. Early-stage lip cancer has a much better chance of recovery than cancer that’s further along. Recent studies show that the five-year survival rate for Stage I and II lip cancers is over 90 percent.
Here’s a table that shows how survival rates change with the stage of cancer:
| Cancer Stage | Five-Year Survival Rate |
|---|---|
| Stage I | 95% |
| Stage II | 90% |
| Stage III | 60% |
| Stage IV | 40% |
Factors Affecting Prognosis
Many things can change how likely a person is to recover from lip cancer. These include the cancer’s stage, where the tumor is, and the patient’s overall health. Early detection is key because it greatly improves treatment results.
Other important factors include the patient’s age, any other health issues they might have, and how well they do with treatment.
Conclusion
White patches on the lips, known as leukoplakia, can signal different conditions. These range from harmless to serious, like cancer. We’ve looked into how these patches might link to lip cancer, including oral cancer inside the lip and signs of skin cancer on the lips.
It’s key to know the causes, risk factors, and warning signs of lip cancer. Spotting symptoms like cancer white spots on lips early is vital. Getting medical help quickly can greatly improve treatment chances.
Spotting lip cancer early, like white patches, can lead to better treatment results. We stress the need for awareness and quick medical checks to tackle lip cancer concerns.
FAQ
What are white patches on lips, and are they a sign of cancer?
White patches on lips, known as leukoplakia, can be signs of many things. They can be harmless or might be cancerous. It’s important to get them checked to know for sure.
What causes white patches on the lips?
Several things can cause white patches on lips. These include oral thrush, Fordyce spots, and oral lichen planus. They can also be from trauma or irritation. Sometimes, they might even be a sign of cancer.
What are the risk factors for lip cancer?
Lip cancer risks include smoking, drinking a lot of alcohol, and UV radiation. Knowing these risks helps figure out if white patches are serious.
What are the symptoms of lip cancer?
Lip cancer symptoms include sores or lesions that don’t go away, numbness or pain, swelling, and changes in lip appearance. Spotting these signs early is key to treating it well.
How is lip cancer diagnosed?
Diagnosing lip cancer starts with a detailed check-up. Sometimes, more tests like biopsies are needed. Imaging studies help see how far the cancer has spread.
What are the treatment options for lip cancer?
Treatment for lip cancer depends on the cancer’s stage and location, and the patient’s health. Options include surgery, radiation, chemotherapy, and targeted or immunotherapies. These can be used alone or together.
What is the prognosis for lip cancer patients?
Lip cancer prognosis varies with the stage at diagnosis. Catching it early greatly improves chances of survival. Early detection leads to better outcomes.
Can oral cancer occur inside the lip?
Yes, oral cancer can happen inside the lip. It may show as sores, pain, or trouble swallowing. Knowing the difference between oral cancer inside the lip and skin cancer is key for treatment.
When should I seek medical attention for white patches on my lips?
See a doctor if you have sores or lesions that won’t heal, numbness or pain, swelling, or changes in lip color. Quick medical check-ups are vital for early treatment.
References
National Health Service (NHS). White Patches on Lips: Leukoplakia and Cancer Differentiation. Retrieved from https://www.nhs.uk/conditions/leukoplakia/



































