
We are seeing a big increase in liver disease symptoms all over the world. This is mainly because of lifestyle diseases and substance abuse. It’s putting a big strain on healthcare systems everywhere, making us rethink how we treat these conditions.
The impact of liver damage is huge, with about 2 million deaths every year. Most of these deaths are from cirrhosis and liver cancer. Keeping our livers healthy is key. Knowing what harms our livers is the first step to fighting this big health problem.
Key Takeaways
- Lifestyle diseases and substance abuse are major contributors to the rise in liver diseases.
- Liver conditions result in approximately 2 million deaths each year globally.
- Cirrhosis and liver cancer are the leading causes of liver-related fatalities.
- Understanding liver damage is key to finding better treatments.
- Global healthcare systems are facing big challenges because of more liver diseases.
The Vital Role of the Liver in Human Health
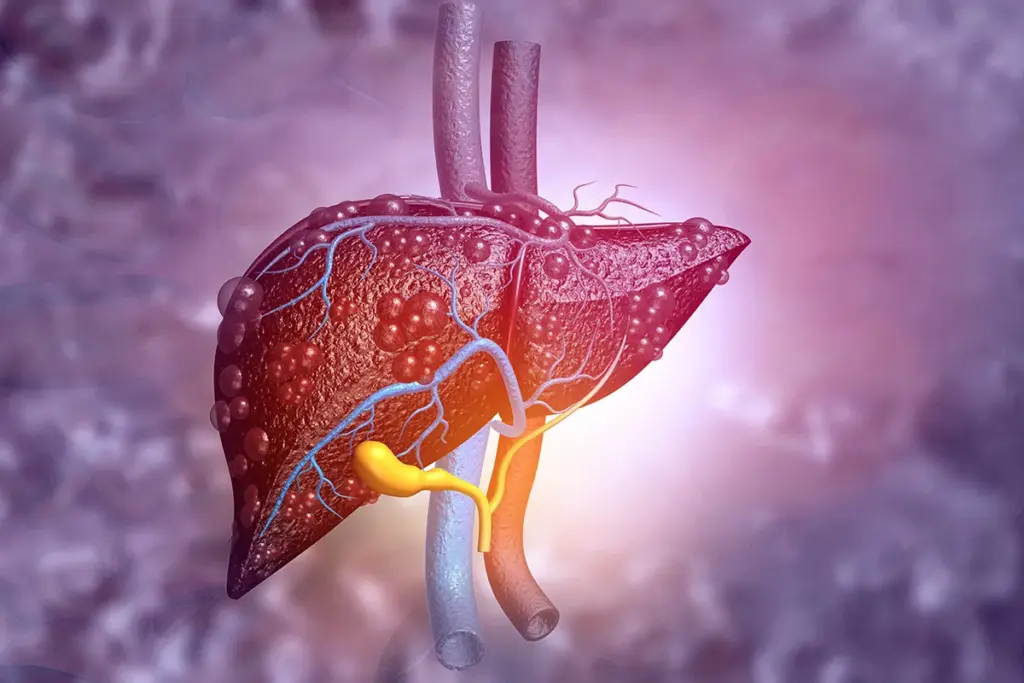
Our liver is key to our health, doing many important jobs. It helps our body work right. It’s a vital organ that does a lot for us.
Essential Functions of the Liver
The liver does many critical things for us to live. These include:
- Detoxification: It removes toxins from our body, keeping us safe.
- Protein Synthesis: It makes proteins for healthy tissues and organs.
- Production of Biochemicals Necessary for Digestion: It makes bile for digesting fats and vitamins.
- Metabolic Regulation: It helps manage how our body uses nutrients.
The liver’s role in metabolism is very important. It breaks down fats, proteins, and carbs for energy. It also stores glycogen for quick energy when needed.
Why Liver Health Matters for Overall Wellness
Keeping our liver healthy is key for feeling good. A healthy liver helps our body detox and metabolize. A sick liver can cause fatigue, weakness, and even serious problems like cirrhosis or liver failure.
So, it’s important to know how to keep our liver healthy. We can do this by living a healthy lifestyle, not drinking too much alcohol, and being careful with our medicines and supplements.
By focusing on liver health, we can greatly improve our overall well-being and life quality.
The Global Burden of Liver Disease
Liver disease is a big problem worldwide. It affects many people and costs a lot for healthcare. Every year, it leads to about 2 million deaths, making it a major cause of death globally.
Worldwide Statistics and Mortality Rates
Liver disease is a big worry for health worldwide. It’s more common in some places than others. Studies show it’s a top cause of death, with cirrhosis and liver cancer leading the list.
The numbers are scary, showing we need better ways to prevent and treat it. We must know why liver disease happens, like alcohol use, viral hepatitis, and metabolic issues. Then, we can make plans to help.
Economic and Healthcare Impact
Liver disease costs a lot for healthcare. It includes managing chronic conditions, treating problems, and doing liver transplants. It also affects families and society in many ways.
We must tackle liver disease with strong prevention and treatment efforts. We should teach people about liver disease symptoms and cirrhosis symptoms. We also need to work on policies to lower risks, like drinking less and fighting obesity.
Metabolic Dysfunction–Associated Steatotic Liver Disease (MASLD)
MASLD is a growing concern due to more people having metabolic disorders. It causes too much fat to build up in liver cells. This is linked to metabolic syndrome, obesity, and insulin resistance.
The Shift in Terminology: From NAFLD to MASLD
The term change from NAFLD to MASLD shows we now understand metabolic dysfunction better. This change highlights how metabolic factors and liver issues are connected. It moves away from just focusing on liver problems.
The new name puts more focus on metabolic issues causing liver disease. This makes diagnosis and treatment more accurate and complete.
Rising Prevalence and Risk Factors
MASLD affects up to 38% of adults worldwide. It’s linked to obesity, diabetes, and metabolic syndrome. Key risk factors include:
- Obesity and insulin resistance
- Type 2 diabetes
- Dyslipidemia
- Hypertension
These factors help MASLD develop and get worse. This shows we need a full approach to manage metabolic health.
|
Risk Factor |
Impact on MASLD |
|---|---|
|
Obesity |
Increases liver fat accumulation |
|
Insulin Resistance |
Promotes liver inflammation |
|
Type 2 Diabetes |
Exacerbates metabolic dysfunction |
Progressive Damage to Liver Tissue
MASLD can get worse, leading to more serious conditions like MASH, fibrosis, and cirrhosis. This happens because of ongoing inflammation and metabolic stress.
Liver inflammation is key in MASLD getting worse. It can lead to liver fibrosis, cirrhosis, and even liver cancer.
Knowing the causes and risk factors of MASLD is vital. It helps us act early and manage the disease better. This can stop or even reverse the disease’s progression.
Alcohol-Associated Liver Disease (ALD): A Growing Crisis
Alcohol use is on the rise, leading to more cases of Alcohol-Associated Liver Disease (ALD). ALD can range from mild fatty liver to severe cirrhosis. This growing problem affects not just health but also healthcare systems worldwide.
How Alcohol Damages Liver Cells
Drinking alcohol harms liver cells, causing inflammation and scarring. This damage can lead to the loss of liver cells and fibrosis. The liver can heal, but chronic drinking can cause permanent harm.
Alarming Trends in Alcohol Consumption and Liver Disease
Alcohol-related liver disease death rates have jumped by 34.4% in the U.S. from 2009 to 2016. This trend is seen globally, due to factors like easier access to alcohol and cultural views on drinking.
Stages from Fatty Liver to Alcoholic Hepatitis to Cirrhosis
ALD goes through stages, each with its own symptoms and treatment options.
|
Stage |
Description |
Potential for Recovery |
|---|---|---|
|
Fatty Liver |
Accumulation of fat in liver cells, often reversible with abstinence. |
High |
|
Alcoholic Hepatitis |
Inflammation of the liver, which can be acute or chronic, with a range of severity. |
Moderate |
|
Cirrhosis |
Scarring of the liver that is irreversible and can lead to liver failure. |
Low |
Knowing these stages helps in early treatment and prevention of liver disease. Early action can greatly improve outcomes for ALD patients.
Viral Hepatitis: Silent Threats to Liver Health
Viral hepatitis is a growing concern for liver health. It’s a major cause of liver disease worldwide. Hepatitis B and C are big contributors to liver problems and deaths.
Hepatitis B: Transmission, Prevention, and Management
Hepatitis B is a viral infection that causes liver inflammation. It can lead to severe liver damage. It spreads through bodily fluids like blood and semen.
Prevention is key. Vaccination is the most effective way to fight hepatitis B. The World Health Organization says all infants should get the vaccine within 24 hours of birth.
For those infected, management involves watching liver health. Sometimes, antiviral therapy is used to stop the virus and prevent damage.
Hepatitis C: Detection and Current Treatment Options
Hepatitis C is another major cause of liver disease. It spreads through blood-to-blood contact, like sharing needles. It can also spread through sexual contact, but less often.
Detection is key because hepatitis C often shows no symptoms until it’s too late. Blood tests are used to find the infection.
Treatment has improved a lot. Direct-acting antivirals (DAAs) can cure most patients. These drugs target the virus directly, leading to shorter treatments and fewer side effects.
Other Forms of Viral Hepatitis
While hepatitis B and C are major threats, other types like hepatitis A and E also exist. Hepatitis A spreads through fecal-oral contact, often through contaminated food or water.
Hepatitis E also spreads through fecal-oral contact. It can be very severe in pregnant women.
Knowing about all types of viral hepatitis is important. It helps us develop better ways to prevent and treat these diseases.
Drug-Induced Liver Injury (DILI)
Drug-induced liver injury (DILI) is a big worry in today’s healthcare. Many substances can harm the liver. It’s key to know what can cause liver damage.
Prescription Medications That Can Harm the Liver
Some prescription drugs can harm the liver. Here are a few examples:
- Antibiotics: Some, like amoxicillin-clavulanate, can cause liver injury.
- Statins: These cholesterol-lowering drugs can sometimes damage the liver.
- Anti-seizure medications: Certain ones can lead to DILI.
Over-the-Counter Drugs and Liver Toxicity
OTC drugs can also risk liver health. Acetaminophen, a common pain reliever, can harm the liver if taken too much.
Herbal Supplements and Unexpected Liver Damage
Herbal supplements, seen as safe because they’re natural, can also harm the liver. Here are a few examples:
- Kava: Used for anxiety, kava can cause liver damage.
- Green tea extract: While safe in small amounts, high doses can be toxic to the liver.
|
Substance Category |
Examples |
Liver Injury Risk |
|---|---|---|
|
Prescription Medications |
Antibiotics, Statins, Anti-seizure medications |
Variable, often dose-dependent |
|
Over-the-Counter Drugs |
Acetaminophen |
High, specially with overdose |
|
Herbal Supplements |
Kava, Green tea extract |
Variable, often idiosyncratic |
Knowing about DILI risks is vital for liver health. By understanding the dangers of different substances, we can reduce these risks. This helps protect our liver.
Metabolic Syndrome and Its Impact on the Liver
Metabolic syndrome is a growing concern worldwide. It affects liver health and increases the risk of type 2 diabetes and heart disease. The conditions include high blood pressure, high blood sugar, and excess body fat around the waist. These can harm the liver.
Insulin Resistance and Liver Disease
Insulin resistance is a key part of metabolic syndrome. It leads to liver disease. When cells resist insulin, the pancreas makes more insulin. This can cause fat to build up in the liver, leading to NAFLD and NASH.
Key factors linking insulin resistance to liver disease include:
- Increased lipogenesis: Insulin promotes the production of fatty acids in the liver.
- Impaired lipid export: Insulin resistance hinders the liver’s ability to export lipids, leading to fat accumulation.
- Inflammation: Hyperinsulinemia and insulin resistance can trigger inflammatory pathways in the liver.
Obesity and Liver Inflammation
Obesity is closely linked to liver inflammation. Abdominal fat is not just for storing fat; it’s an active endocrine organ. It releases pro-inflammatory cytokines that harm the liver.
The mechanisms by which obesity triggers liver inflammation include:
- The release of free fatty acids from adipose tissue, which can be taken up by the liver, promoting lipotoxicity.
- The production of pro-inflammatory cytokines like TNF-alpha and IL-6, which exacerbate liver inflammation.
- Changes in the gut microbiota, leading to increased gut permeability and the translocation of bacterial products to the liver, further fueling inflammation.
Managing Metabolic Risk Factors
Managing metabolic risk factors is key to protecting the liver. Lifestyle changes are essential, including diet, exercise, and weight loss. Sometimes, medication is needed to control specific risks.
|
Lifestyle Modification |
Benefit for Liver Health |
|---|---|
|
Weight Loss |
Reduces liver fat and inflammation |
|
Dietary Changes |
Improves insulin sensitivity and reduces liver fat |
|
Increased Physical Activity |
Enhances insulin sensitivity and overall metabolic health |
By tackling metabolic syndrome with lifestyle changes and medical treatment, we can lower liver disease risk. This improves overall health.
Autoimmune Conditions Affecting the Liver
Liver health can be harmed by autoimmune diseases. These diseases need quick diagnosis and treatment. Autoimmune conditions happen when the body’s immune system attacks its own cells and organs.
In the liver, these conditions can cause chronic inflammation and scarring. If not managed, they can lead to cirrhosis or liver failure.
Autoimmune Hepatitis: When the Body Attacks the Liver
Autoimmune hepatitis is when the body’s immune system attacks liver cells. This causes inflammation and damage. Symptoms include fatigue, jaundice, and abdominal discomfort.
If not treated, it can lead to cirrhosis and liver failure.
Diagnosis involves blood tests to find liver inflammation and autoimmune antibodies. Treatment includes immunosuppressive medications to stop the immune system’s attack.
Primary Biliary Cholangitis
Primary biliary cholangitis (PBC) is a chronic autoimmune disease. It affects the bile ducts in the liver, causing damage. Symptoms include itching, fatigue, and jaundice.
Ursodeoxycholic acid (UDCA) is often prescribed to slow disease progression. In severe cases, liver transplantation may be needed.
Primary Sclerosing Cholangitis
Primary sclerosing cholangitis (PSC) is an autoimmune condition that affects the bile ducts. It causes scarring, narrowing, and obstruction. This can lead to recurrent cholangitis, cirrhosis, or cholangiocarcinoma.
|
Disease |
Primary Characteristics |
Common Symptoms |
Treatment Options |
|---|---|---|---|
|
Autoimmune Hepatitis |
Immune system attacks liver cells |
Fatigue, jaundice, abdominal pain |
Immunosuppressive medications |
|
Primary Biliary Cholangitis |
Destruction of bile ducts within the liver |
Itching, fatigue, jaundice |
UDCA, liver transplantation |
|
Primary Sclerosing Cholangitis |
Scarring and narrowing of bile ducts |
Jaundice, pruritus, recurrent cholangitis |
Endoscopic therapy, liver transplantation |
Managing autoimmune liver diseases needs a full approach. This includes medication, lifestyle changes, and regular monitoring. It helps prevent complications and improves quality of life.
Understanding Liver Cancer Development
It’s important to know how liver cancer starts, mainly for those with long-term liver issues. Liver cancer, like hepatocellular carcinoma (HCC), is a big worry worldwide.
Hepatocellular Carcinoma (HCC): Primary Liver Cancer
Hepatocellular carcinoma (HCC) is the main type of liver cancer. It comes from the liver’s main cells, called hepatocytes. HCC often links to long-term liver disease and cirrhosis.
These can come from viral hepatitis, too much alcohol, or metabolic disease.
Key Risk Factors for HCC:
- Chronic infection with hepatitis B or C virus
- Cirrhosis from any cause
- Heavy alcohol consumption
- MASLD and metabolic syndrome
- Aflatoxin exposure
The Progression from Chronic Disease to Cancer
HCC’s growth is a complex process. It starts with chronic inflammation, liver cell regeneration, and genetic changes. Long-term liver disease can lead to cirrhosis, raising HCC risk.
|
Stage |
Description |
Risk Factors |
|---|---|---|
|
Chronic Liver Disease |
Inflammation and damage to liver cells |
Viral hepatitis, alcohol, MASLD |
|
Cirrhosis |
Scarring of the liver |
Chronic liver disease, alcohol abuse |
|
HCC |
Development of liver cancer |
Cirrhosis, chronic hepatitis B |
Screening Recommendations for High-Risk Individuals
People at high risk should get regular HCC screenings. This includes those with cirrhosis or chronic hepatitis B. Screenings use ultrasound and sometimes blood tests for alpha-fetoprotein (AFP).
Screening Guidelines:
- Those with cirrhosis should get ultrasound screenings every 6 months.
- People with chronic hepatitis B, with high viral load or family history of HCC, should also be screened.
- Decisions for other risk factors should be made individually.
Cirrhosis: The Advanced Stage of Liver Damage
Cirrhosis is the final stage of liver damage. It happens when scarring and fibrosis severely harm liver function. This damage comes from chronic liver diseases that slowly destroy liver tissue.
The Process of Liver Scarring and Fibrosis
Liver scarring, or fibrosis, happens when the liver tries to heal from injury. This leads to the buildup of scar tissue. Over time, this scar tissue can change the liver’s shape and reduce its function. Fibrosis can be reversed if caught early, but if it turns into cirrhosis, the damage is harder to fix.
Understanding fibrosis is key to fighting liver diseases. “The development of fibrosis is a complex process involving various cell types and signaling pathways,” say liver disease experts. This shows why we need a full approach to care for liver health.
Compensated vs. Decompensated Cirrhosis
Cirrhosis is divided into two stages: compensated and decompensated. In the compensated stage, the liver works fairly well despite scarring, and symptoms may not show. But, as cirrhosis moves to the decompensated stage, liver function worsens. This leads to problems like jaundice, variceal bleeding, and ascites.
|
Characteristics |
Compensated Cirrhosis |
Decompensated Cirrhosis |
|---|---|---|
|
Liver Function |
Relatively preserved |
Significantly impaired |
|
Symptoms |
Often asymptomatic |
Jaundice, variceal bleeding, ascites |
|
Prognosis |
Better prognosis with appropriate management |
Poor prognosis without liver transplantation |
Potential for Reversal in Early Stages
While cirrhosis is often seen as irreversible, early stages can be reversed. Treating the cause of liver damage can stop cirrhosis from getting worse. In some cases, the liver can even heal. Early action is critical in managing cirrhosis well.
Knowing about cirrhosis and its stages helps us manage liver health better. This can prevent liver disease from getting worse.
The Remarkable Power of Liver Regeneration
The liver exhibits a remarkable capacity for self-healing. It can fix itself after many injuries. This makes the liver a key area for medical research.
How the Liver Repairs Itself
The liver’s healing process is complex. It involves many cell types working together. When liver cells get hurt, the body starts a repair plan.
This plan includes using stem cells and growing more liver cells. This helps the liver get back to normal.
“The liver has a remarkable ability to regenerate, and understanding this process can provide insights into new therapeutic strategies for liver diseases,” says a leading researcher in the field.
Limits of Regenerative Capacity
Even though the liver can heal well, it has limits. Too much damage can cause scarring and cirrhosis. Age, health, and toxins can affect how well the liver can heal.
Supporting Natural Liver Healing
To help the liver heal, living a healthy lifestyle is key. Eating well, not drinking too much alcohol, and avoiding toxins are important. Some nutrients and supplements can also help liver health.
But, always talk to a doctor before taking new supplements. We can help our liver by making smart choices about what we eat and do. Knowing how the liver regenerates helps us protect this important organ.
Warning Signs of Liver Damage
Liver damage often goes unnoticed, making it key to spot its signs. The liver can keep working even when it’s damaged. But, this can hide the early signs of liver disease.
Early Symptoms Often Overlooked
In the early stages, liver damage may not show clear symptoms. Or, the symptoms might be mistaken for other issues. Common early signs include:
- Fatigue and general malaise
- Mild abdominal discomfort
- Loss of appetite
- Nausea
These symptoms are often mild and can be mistaken for other things. It’s important to watch for them and see a doctor if they don’t go away.
Advanced Liver Disease Manifestations
As liver damage gets worse, more obvious symptoms appear. These show advanced liver disease. These may include:
- Jaundice (yellowing of the skin and eyes)
- Dark urine and pale stools
- Severe itching
- Swelling in the legs and abdomen (edema and ascites)
These signs mean the liver is badly damaged. You need to see a doctor right away.
When to Seek Immediate Medical Attention
Some symptoms need urgent doctor visits. These include:
- Severe abdominal pain
- Vomiting blood or black tarry stools
- Confusion or altered mental state
- Severe jaundice
If you or someone you know has these symptoms, get medical help fast. Quick action can help a lot in treating liver disease.
Diagnostic Approaches for Liver Assessment
Checking the liver is key to finding out if it’s damaged or diseased. We use different tools to see how well the liver is working. Each tool gives us special information about the liver’s state.
Blood Tests and Liver Function Panels
Blood tests are a big part of checking the liver. They look at enzymes and proteins in the blood linked to liver health. Important tests include:
- Liver function tests (LFTs) that measure levels of alanine aminotransferase (ALT) and aspartate aminotransferase (AST)
- Tests for bilirubin levels
- Measurements of albumin and prothrombin time
These tests show if the liver is damaged, inflamed, or not working right. For example, high ALT and AST levels mean liver cells are hurt.
|
Blood Test |
Normal Range |
Significance |
|---|---|---|
|
ALT |
0-40 U/L |
Elevated levels indicate liver cell damage |
|
AST |
0-40 U/L |
Elevated levels can indicate liver damage or other conditions |
|
Bilirubin |
0.1-1.2 mg/dL |
High levels can cause jaundice and indicate liver dysfunction |
Imaging Studies: Ultrasound, CT, and MRI
Imaging studies give us pictures of the liver’s shape and help find different liver problems. Common ones are:
- Ultrasound: Good for spotting fatty liver, cysts, and tumors
- CT scans: Show detailed pictures, useful for finding liver masses and damage
- MRI: Gives clear images of the liver, great for diagnosing conditions like cirrhosis and tumors
These methods are safe and give important info for treating liver diseases.
FibroScan and Other Non-invasive Alternatives to Biopsy
New tools have come up as safer choices instead of liver biopsy. FibroScan is one that checks liver stiffness, which shows how fibrotic the liver is.
Other non-invasive options include:
- Transient Elastography (FibroScan)
- Magnetic Resonance Elastography (MRE)
- Blood-based biomarkers and scoring systems
These methods are less invasive and give useful info about liver health.
Nutrition’s Impact on Liver Health
The liver is key to our health, and what we eat matters a lot. Eating right helps the liver work well. But, bad food choices can hurt it.
Harmful Foods for the Liver
Some foods are bad for the liver. These include foods high in saturated fats, refined sugars, and processed stuff. Too much alcohol is also bad. It’s important to avoid or cut down on these foods to keep the liver healthy.
Beneficial Dietary Patterns
Eating lots of fruits, veggies, whole grains, and lean proteins is good for the liver. Foods packed with antioxidants, like berries and leafy greens, are extra helpful. Adding these to our diet can help protect the liver.
The Role of Added Sugars and Processed Foods
Added sugars and processed foods can cause problems like insulin resistance and fatty liver disease. It’s key to eat less of these to keep the liver safe. Staying away from added sugars and processed foods can help avoid liver damage.
|
Food Group |
Recommended Foods |
Foods to Limit |
|---|---|---|
|
Fruits |
Apples, Berries, Citrus Fruits |
Fruits High in Sugar |
|
Vegetables |
Leafy Greens, Cruciferous Vegetables |
Starchy Vegetables |
|
Proteins |
Lean Meats, Fish, Legumes |
Processed Meats |
|
Grains |
Whole Grains |
Refined Grains |
To show how important a healthy diet is for the liver, look at this image:
By eating right and watching what we eat, we can help our liver stay healthy. This is good for our overall health too.
Treatment Options for Liver Diseases
The treatment for liver diseases is changing fast, giving hope to patients everywhere. As we learn more about liver conditions, new ways to treat them have been found. These treatments meet the different needs of patients.
Disease-Specific Medications
Medicines are key in treating liver diseases. For viral hepatitis, antiviral drugs are used. Corticosteroids and immunosuppressants help with autoimmune hepatitis. Ursodeoxycholic acid is given for primary biliary cholangitis to help bile flow and lessen liver harm.
New medicines for liver diseases are being developed. Researchers are looking for better ways to treat these conditions.
Surgical and Minimally Invasive Interventions
Sometimes, surgery or small procedures are needed for liver disease complications or liver cancer. Liver transplantation is a lifesaving choice for those with severe liver disease.
- Liver resection for hepatocellular carcinoma
- Transarterial chemoembolization (TACE) for liver cancer
- Radiofrequency ablation for small liver tumors
These treatments need careful thought and planning. A team of doctors and healthcare workers usually helps decide the best course of action.
Emerging Therapies and Clinical Trials
New treatments like gene therapy, stem cell therapy, and targeted molecular therapies are being explored. Clinical trials are important for checking if these treatments are safe and work well.
We suggest patients talk to their doctors about joining clinical trials. This can give them access to new treatments and help improve liver disease care.
Conclusion: Protecting Your Liver Through Prevention and Early Intervention
Keeping your liver healthy is key to feeling good overall. We’ve talked about how different things can harm the liver, leading to serious problems. To keep your liver in top shape, focus on prevention and catching issues early.
Liver disease can sneak up on you, so it’s important to get regular check-ups. Knowing the risks and acting early can lower your chance of liver problems.
Living a healthy lifestyle is a big part of keeping your liver safe. Eating right and drinking alcohol in moderation are important. Also, be careful with medications and supplements to avoid liver damage.
We stress the need for a complete approach to liver health. This includes prevention, early action, and making smart choices. By focusing on your liver, you can keep yourself healthy and avoid liver disease.
FAQ
What are the primary functions of the liver?
The liver is key to our health. It cleanses toxins, makes proteins, and helps digest food. It also stores glycogen and regulates metabolism.
What are the common symptoms of liver disease?
Liver disease symptoms include fatigue and jaundice. You might also see dark urine and pale stools. Abdominal swelling is another sign.
As the disease gets worse, symptoms can get more severe. This includes confusion and difficulty concentrating. In the worst cases, it can lead to coma.
How does alcohol consumption affect the liver?
Drinking too much alcohol harms the liver. It causes damage and inflammation. This can lead to fatty liver, hepatitis, and cirrhosis.
What is the difference between compensated and decompensated cirrhosis?
Compensated cirrhosis means the liver is scarred but works well. You might not even notice symptoms. Decompensated cirrhosis is when the liver fails, causing jaundice and other serious problems.
How can I protect my liver from damage?
To keep your liver healthy, eat well and avoid too much alcohol. Stay away from toxins. Regular health checks and vaccinations against hepatitis are also important.
What dietary patterns are beneficial for liver health?
Eating foods high in antioxidants and fiber is good for your liver. Include fruits, vegetables, whole grains, and lean proteins. Avoid processed foods and added sugars.
Can the liver regenerate itself?
Yes, the liver can heal itself by replacing damaged cells. But it can only do this for so long. Chronic damage can lead to cirrhosis and liver failure.
What are the risk factors for developing liver cancer?
Liver cancer risks include hepatitis B or C, cirrhosis, and too much alcohol. Certain metabolic disorders also increase risk. People at high risk should get regular screenings.
How is liver disease diagnosed?
Doctors use blood tests and imaging like ultrasound and CT scans to diagnose liver disease. Liver biopsy and FibroScan are also used to check liver health.
What are the treatment options for liver diseases?
Treatment depends on the disease. It can include medications, lifestyle changes, surgery, or liver transplant. New treatments and clinical trials offer hope for managing liver diseases.
How does metabolic syndrome impact liver health?
Metabolic syndrome can cause liver inflammation and disease. It includes insulin resistance, obesity, and high cholesterol. Managing these risks is key to liver health.
What is the role of nutrition in liver health?
Nutrition is vital for liver health. A balanced diet protects the liver. But a diet full of processed foods and unhealthy fats can harm it.
References
Liver Injury and Regeneration: Current Understanding, New Approaches, and Future Perspectives
https://pmc.ncbi.nlm.nih.gov/articles/PMC10486351/























































