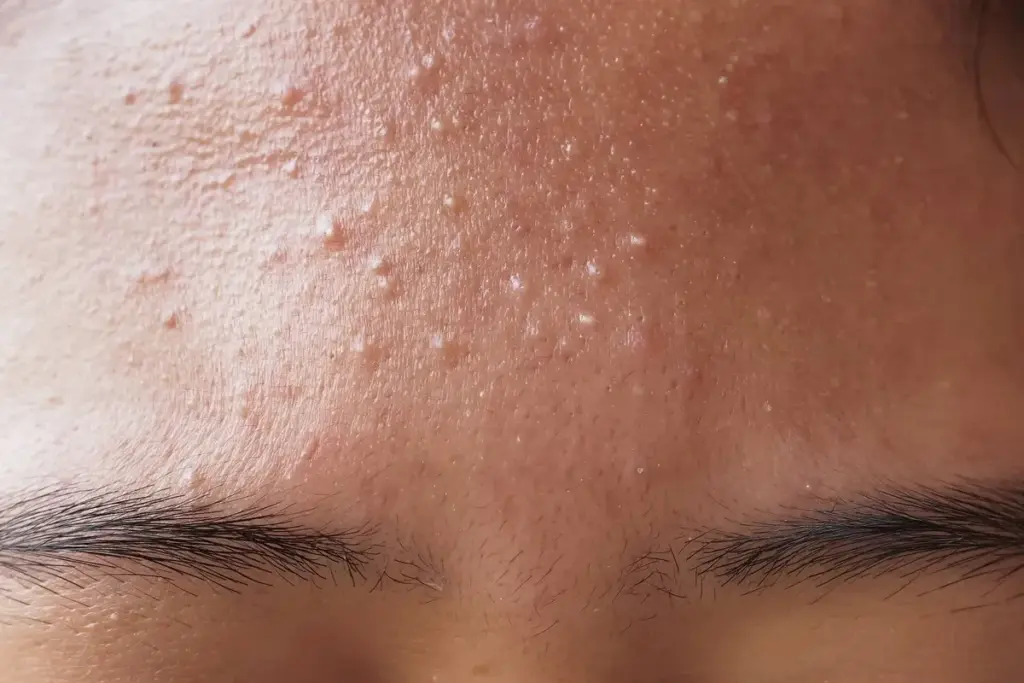
Are your current skin treatments failing despite consistent use? The culprit might not be bacterial at all. Instead, it may be a common yet misunderstood yeast overgrowth known as Malassezia.
This condition closely resembles traditional blemishes, which often leads to frequent misdiagnosis. We believe that fungal acne face treatment requires a specialized clinical approach to be truly effective.
Factors such as heat and humidity often trigger these persistent, itchy bumps. We provide evidence-based care to help you restore the natural balance of your skin flora safely.
Our team at Liv Hospital is committed to up-to-date medical protocols and compassionate, patient-centered care. We focus on modern science to ensure our international patients see lasting and healthy results.
Learning how to manage these specific bumps on the forehead is the first step toward clarity. We are here to support your journey with expert guidance and advanced therapeutic solutions.
Key Takeaways
- Identify if yeast overgrowth is the root cause of your breakouts.
- Distinguish between bacterial issues and Malassezia symptoms.
- Recognize how environmental factors like humidity worsen the condition.
- Access specialized medical protocols at Liv Hospital for recovery.
- Utilize evidence-based methods for long-term skin health.
- Receive empathetic support from our international healthcare experts.
What Is Fungal Acne and How to Identify It
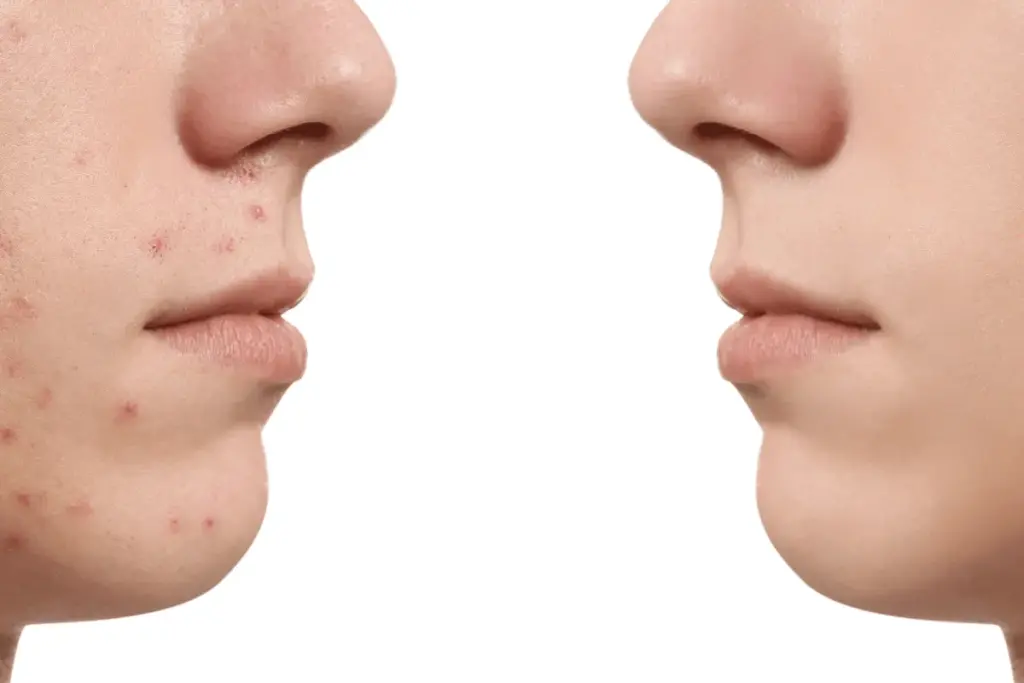
Fungal acne is different from other types of acne. It’s caused by too much yeast in the skin’s pores. This condition is also known as pityrosporum folliculitis or malassezia folliculitis.
Understanding Malassezia Yeast Overgrowth
Malassezia yeast is found on human skin. But too much of it can cause fungal acne. Things like humidity, oily skin, and certain products can lead to this.
This yeast overgrowth can make skin inflamed. It can also cause acne-like symptoms.
Key Differences Between Fungal and Bacterial Acne
Fungal acne is different from bacterial acne. Fungal acne has uniform, itchy bumps. It doesn’t have blackheads or whiteheads like bacterial acne does.
Signs and Symptoms of Fungal Acne on Your Face
Fungal acne symptoms can vary. But common signs include:
- Uniform red or flesh-colored bumps
- Intense itching, mostly in affected areas
- Lesions often show up on the upper back, chest, and face
If you notice these signs, you might have fungal acne.
Self-Assessment and Professional Diagnosis
Self-assessment can give you a starting point. But, a professional diagnosis is usually needed. A dermatologist can look at your skin, talk about your symptoms and health history, and give a proper diagnosis.
Getting professional help is key to finding the right treatment.
Best Fungal Acne Treatment Options
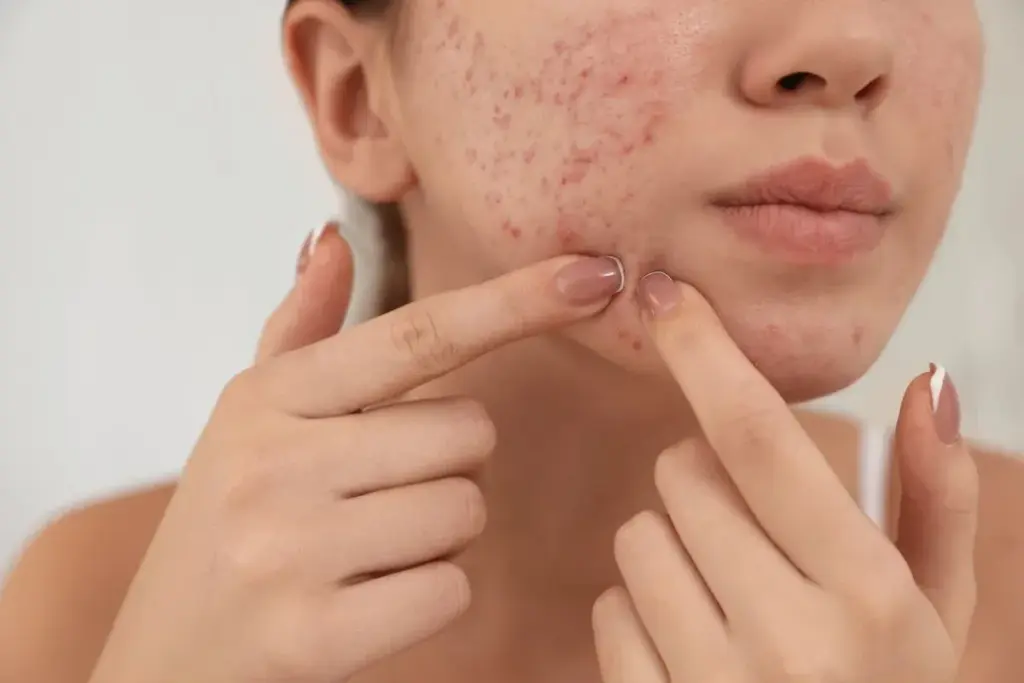
There are many ways to treat fungal acne, from products you can buy to medicines your doctor can prescribe. We’ll go over these options to help you choose the best for your skin.
Over-the-Counter Antifungal Products
For a start, you can try over-the-counter (OTC) antifungal products. These include shampoos for dandruff and creams for athlete’s foot. They have ingredients like ketoconazole and clotrimazole that fight fungal infections.
Some good OTC options for fungal acne are:
- Antifungal creams with clotrimazole or miconazole
- Anti-dandruff shampoos with ketoconazole or zinc pyrithione
- Products called “antifungal” or “anti-yeast”
Prescription Antifungal Medications
If your fungal acne is severe, you might need prescription medicines. These include oral drugs like fluconazole or stronger creams. Always talk to a dermatologist to find the best treatment for you.
Prescription treatments are often stronger and can be customized for your needs.
Fungal Acne-Safe Skincare Products
Choosing the right skincare is key to fighting fungal acne. Look for non-comedogenic and oil-free products to avoid making things worse.
When picking skincare, look for:
- Products labeled “non-comedogenic” or “oil-free”
- Products without fragrances to avoid irritation
- Products with soothing ingredients like aloe vera or green tea
By using the right treatments and skincare, you can manage and lessen fungal acne.
Step-by-Step Guide to Treating Fungal Acne on Your Face
To treat fungal acne, knowing the steps is key. It’s not just about treating the symptoms. You need to tackle the root cause for healthier skin.
Step 1: Eliminate Yeast-Feeding Ingredients from Your Routine
Start by checking your skincare products. Look for oils, fatty acids, and sugars. These can make yeast grow, leading to fungal acne. Switch to “non-comedogenic” or “oil-free” products to avoid clogged pores and yeast feeding.
Step 2: Cleanse with Antifungal Ingredients
Use a cleanser with antifungal properties. Ingredients like ketoconazole, tea tree oil, or sulfur work well. Massage the cleanser on your face for 30 seconds before rinsing with lukewarm water.
Step 3: Apply Targeted Antifungal Treatment
After cleansing, apply an antifungal treatment to the affected areas. Clotrimazole or selenium sulfide can help. Use a thin layer as directed by the product.
Step 4: Use Only Fungal Acne-Safe Moisturizers
Moisturizing is important, but choose wisely for fungal acne. Look for moisturizers labeled as “fungal acne-friendly” or without oils and fatty acids. This keeps your skin’s barrier strong without worsening the condition.
Stick to these steps and your treatment plan. This way, you can manage fungal acne and get healthier skin.
Conclusion
Managing fungal acne well starts with knowing what it is. Understanding its causes and symptoms helps find the right treatment. This leads to better skin health.
We’ve shown how to treat fungal acne on the face. This includes avoiding foods that feed yeast and using antifungal products. With the right care, you can beat this tough condition.
At Liv Hospital, we offer top-notch healthcare for fungal acne. We use professional diagnosis and proven treatments. Our goal is to help you get healthier, clearer skin.
If you’re fighting fungal acne, get professional help. They can create a treatment plan just for you.
FAQ
What treats fungal acne most effectively at home? Fungal acne is best managed at home with antifungal products like ketoconazole or selenium sulfide washes, keeping the skin dry, avoiding oily/heavy skincare, and wearing breathable fabrics.
How to treat fungal acne on forehead? Use an antifungal shampoo (like ketoconazole) as a short-contact face wash a few times per week, apply lightweight non-comedogenic moisturizers, and avoid sweat buildup or occlusive products on the forehead.
Are there specific fungal acne treatments for sensitive skin? Yes, opt for gentle antifungal cleansers, fragrance-free products, and soothing ingredients like aloe vera or niacinamide while avoiding harsh exfoliants that can irritate sensitive skin.
How long does it take for fungal acne treatments to show results? Improvement is often seen within 1–2 weeks, but consistent treatment for several weeks is usually needed for full clearing.
Can I use regular acne creams for fungal face acne? Most regular acne treatments (like benzoyl peroxide or antibiotics) are not effective because fungal acne is caused by yeast, not bacteria, and some products may even worsen it.
What to use for fungal acne if it keeps coming back? Continue maintenance with antifungal washes weekly, avoid triggers like sweat and heavy oils, and consider consulting a doctor for prescription antifungal creams or oral treatment if recurrence is frequent.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC3970831/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























