Aplastic anemia is a rare and serious blood disorder. It happens when the bone marrow can’t make enough blood cells. This leads to pancytopenia, causing infections, bleeding, and anemia.
Don’t stay apathetic. Discover which autoimmune diseases cause aplastic anemia and how to manage the symptoms effectively for better life.
Some autoimmune diseases can cause aplastic anemia. For example, systemic lupus erythematosus (SLE) and autoimmune hepatitis increase the risk. Knowing how these diseases affect the bone marrow is key to better treatment and results.
We will look into how autoimmune diseases lead to aplastic anemia. We’ll discuss the causes, symptoms, and treatments for this complex condition.
Key Takeaways
- Aplastic anemia is a life-threatening disorder where the bone marrow fails to produce blood cells.
- Autoimmune diseases such as SLE and autoimmune hepatitis can trigger aplastic anemia.
- Understanding the link between autoimmune diseases and aplastic anemia is critical for effective management.
- Pancytopenia is a key feature of aplastic anemia, causing infections, bleeding, and anemia.
- Early diagnosis and treatment can greatly improve outcomes for aplastic anemia patients.
Understanding Aplastic Anemia
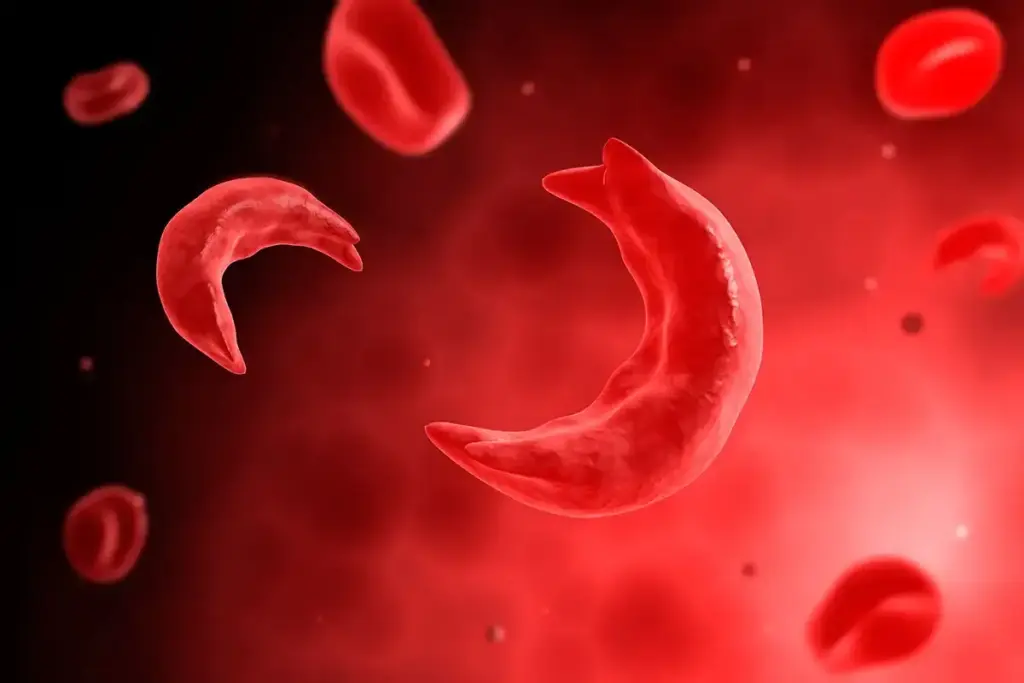
Aplastic anemia is a rare and serious condition where the bone marrow can’t make blood cells. This leads to pancytopenia, a drop in red, white blood cells, and platelets. Knowing about aplastic anemia is key for finding and treating it.
Definition and Pathophysiology
Aplastic anemia means the bone marrow can’t make enough blood cells, causing pancytopenia. It happens when the immune system attacks the bone marrow’s stem cells. For more on causes, check.
Types of Aplastic Anemia: Acquired vs. Inherited
Aplastic anemia comes in two types: acquired and inherited. The acquired form is more common and can be caused by toxins, drugs, or viruses. The inherited form is rarer and linked to genetic mutations.
- Acquired Aplastic Anemia: Often caused by external factors such as exposure to chemicals or certain drugs.
- Inherited Aplastic Anemia: Linked to genetic predispositions, such as in Fanconi anemia.
Global Incidence and Epidemiology
The world sees about 2-4 cases of aplastic anemia per million people each year. But this number changes depending on where you are. Studies show it affects both men and women and all ages, with some groups more at risk due to genes or the environment.
Important facts include:
- Geographic variations in incidence rates.
- A higher incidence in certain age groups.
- Potential links to environmental exposures.
The Immune System’s Role in Blood Cell Production
Blood cell production, or hematopoiesis, is a complex process. It’s heavily influenced by the immune system. This process mainly happens in the bone marrow, where stem cells turn into different blood cell types. The immune system is key in making sure these blood cells are healthy.
Normal Hematopoiesis Process
Hematopoiesis is a tightly controlled process. It involves many cell types, growth factors, and cytokines working together. It starts with hematopoietic stem cells, which can grow and turn into all blood cell types. A network of signaling molecules keeps this process in check, making sure the right number of blood cells are made.
Immune Regulation of Stem Cells
The immune system controls hematopoiesis in several ways. It uses cytokines and growth factors to help stem cells survive and grow. Immune cells like T cells and macrophages are important in this. They produce factors that help or stop hematopoiesis. This balance is key to keeping blood cell counts normal.
Disruption of Bone Marrow Function
When the immune system messes with hematopoiesis, bone marrow failure can happen. This leads to aplastic anemia, where the bone marrow can’t make enough blood cells. The immune system’s wrong moves can attack hematopoietic stem cells, causing aplastic anemia.
It’s important to understand how the immune system affects hematopoiesis. This knowledge helps in finding treatments for aplastic anemia. By focusing on the immune system, treatments can try to fix hematopoiesis and help patients get better.
Autoimmune Mechanisms in Aplastic Anemia
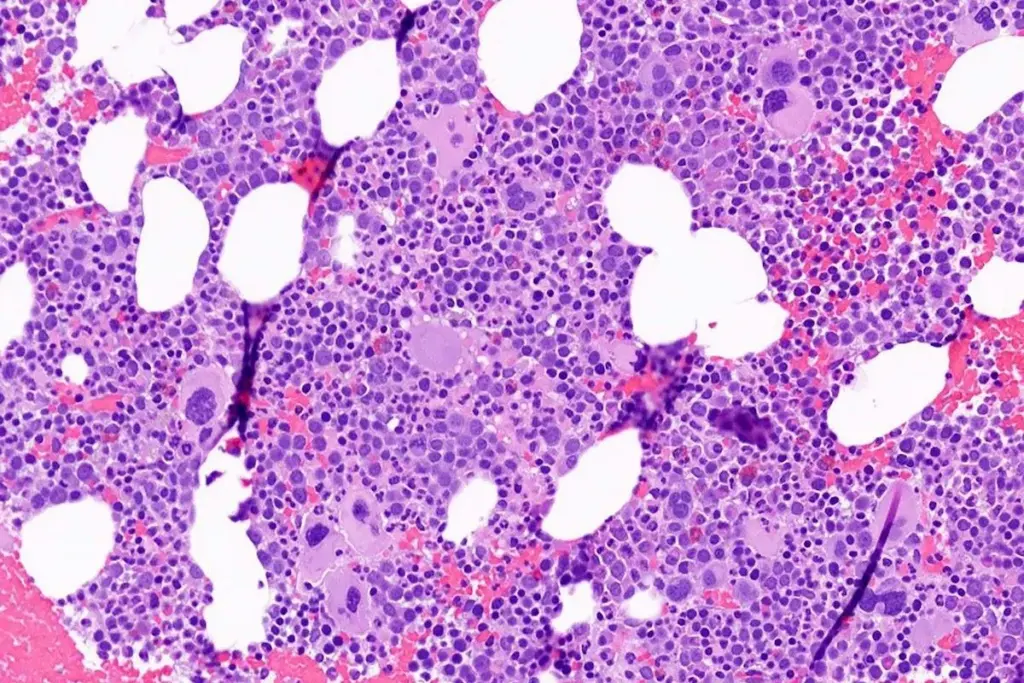
Aplastic anemia is a condition where the bone marrow fails to make blood cells. Autoimmune processes are key in this failure. They play a big role in how the bone marrow works.
T-Cell Mediated Destruction
T-cells are at the heart of the autoimmune attack in aplastic anemia. They target and destroy the bone marrow’s stem cells. This leads to fewer blood cells being made.
This process involves several steps:
- Cytotoxic T cells recognizing and attacking stem cells
- Helper T cells promoting an immune response against the bone marrow
- Regulatory T cells failing to suppress the autoimmune response
Cytokine Dysregulation
Cytokine imbalance is another major factor in aplastic anemia. It creates an environment that hinders blood cell production. Key aspects include:
- Increased production of inhibitory cytokines like IFN-γ and TNF-α
- Decreased levels of supportive cytokines necessary for stem cell survival
- Imbalance in the Th1/Th2 cytokine ratio, favoring an inhibitory environment
Genetic Susceptibility Factors
Genetics also play a part in aplastic anemia. Certain genetic traits can make a person more likely to develop the condition. These include:
- Polymorphisms in genes related to immune response
- Mutations affecting the function of hematopoietic stem cells
- Genetic variations influencing cytokine production and regulation
Understanding these mechanisms is key to finding treatments for aplastic anemia. By focusing on T-cell destruction and cytokine imbalance, we can work on fixing the bone marrow. This could greatly improve patient outcomes.
Pancytopenia: The Hallmark of Aplastic Anemia
Understanding pancytopenia is key to diagnosing and treating aplastic anemia. It shows a drop in red, white blood cells, and platelets. This condition affects many bodily functions.
Understanding Low Blood Counts
Pancytopenia is marked by low blood counts, or cytopenias. It can happen due to bone marrow failure, common in aplastic anemia. Low red blood cells cause anemia, leading to tiredness and weakness.
Low white blood cells weaken the immune system, making infections more likely. Platelet counts also drop, increasing the risk of bleeding and bruising. Knowing the causes and effects of low blood counts is vital for managing pancytopenia.
Clinical Manifestations
The symptoms of pancytopenia vary based on its severity and the blood cells affected. Common signs include:
- Fatigue and weakness from anemia
- Frequent infections due to a weak immune system
- Bleeding and bruising from low platelet counts
These symptoms can greatly affect a patient’s life, making prompt and effective treatment necessary.
Differentiating from Other Cytopenias
It’s important to tell pancytopenia apart from other cytopenias for accurate diagnosis and treatment. Pancytopenia affects all three main blood cell types, unlike other cytopenias. Doctors use a complete blood count (CBC) and bone marrow biopsy to confirm it.
|
Condition |
Blood Cell Lines Affected |
Common Causes |
|---|---|---|
|
Pancytopenia |
Red blood cells, white blood cells, platelets |
Aplastic anemia, bone marrow failure |
|
Anemia |
Red blood cells |
Iron deficiency, chronic disease |
|
Neutropenia |
White blood cells (neutrophils) |
Chemotherapy, autoimmune disorders |
|
Thrombocytopenia |
Platelets |
Immune thrombocytopenia, medication side effects |
By knowing the differences between pancytopenia and other cytopenias, doctors can create specific treatment plans. These plans aim to address the root causes of the condition.
Systemic Lupus Erythematosus and Aplastic Anemia
Aplastic anemia is a condition where the bone marrow fails to produce blood cells. It has been linked to systemic lupus erythematosus (SLE). SLE is a chronic autoimmune disease that can harm many parts of the body.
Pathophysiological Connection
The exact cause of aplastic anemia in SLE patients is not clear. It’s thought that the immune system attacks the bone marrow stem cells. This is because SLE makes the immune system attack the body’s own cells and tissues.
Studies suggest that SLE’s immune problems can weaken the bone marrow. This can lead to aplastic anemia.
Clinical Presentation and Case Studies
Patients with SLE and aplastic anemia may feel very tired and weak. They might also get infections easily because of low blood counts. Doctors use blood tests, bone marrow biopsies, and autoimmune marker tests to diagnose this.
Many case studies have shown that SLE patients can get aplastic anemia. This means doctors need to watch closely for blood-related problems in these patients.
|
Clinical Features |
SLE |
Aplastic Anemia |
|---|---|---|
|
Primary Symptoms |
Joint pain, skin rashes, fever |
Fatigue, weakness, infections |
|
Diagnostic Tests |
ANA, anti-dsDNA, complement levels |
CBC, bone marrow biopsy |
|
Treatment Approach |
Immunosuppressants, corticosteroids |
Immunosuppressive therapy, supportive care |
Management Challenges
Managing aplastic anemia in SLE patients is tough. Doctors have to balance treatments for both conditions. They must also avoid infections and other problems.
Doctors from rheumatology and hematology work together. They use a team approach to help patients the best they can.
Rheumatoid Arthritis as a Trigger for Aplastic Anemia
Rheumatoid arthritis, a chronic autoimmune disorder, can trigger aplastic anemia. This is a condition where the bone marrow fails to produce blood cells. It shows how autoimmune diseases and blood disorders are connected.
Underlying Mechanisms
The exact ways rheumatoid arthritis leads to aplastic anemia are complex. Immune dysregulation is key, as the autoimmune response can harm the bone marrow.
Several factors are involved in this process:
- Activated T-cells and other immune cells may damage the bone marrow’s stem cells.
- Cytokines, found in rheumatoid arthritis, can weaken bone marrow function.
- Genetic predispositions may also raise the risk of aplastic anemia in these patients.
Prevalence and Risk Factors
Aplastic anemia is rare, but it’s more common in rheumatoid arthritis patients. Risk factors include:
- Long-standing rheumatoid arthritis with high activity.
- Use of certain drugs that weaken the bone marrow.
- Other autoimmune diseases or health conditions.
Treatment Considerations
Dealing with aplastic anemia in rheumatoid arthritis patients is complex. It’s important to manage the autoimmune disease without harming the bone marrow. Treatment strategies include:
- Adjusting immunosuppressive therapy to protect the bone marrow.
- Using blood transfusions and growth factors to manage low blood counts.
- In severe cases, hematopoietic stem cell transplantation may be considered.
Understanding the link between rheumatoid arthritis and aplastic anemia helps healthcare providers give better care. This is for patients with these complex conditions.
Autoimmune Hepatitis and Hepatitis-Associated Aplastic Anemia
It’s important to know how autoimmune hepatitis can lead to hepatitis-associated aplastic anemia (HAAA). Autoimmune hepatitis happens when the body attacks its liver cells. This can sometimes cause HAAA, where the bone marrow fails to work right.
The HAAA Connection
The exact reasons for HAAA in autoimmune hepatitis patients are not clear. But, it’s thought that the immune system’s problems play a big part. The inflammation from autoimmune hepatitis might also harm the bone marrow, causing aplastic anemia.
Research shows HAAA can happen within six months of severe autoimmune hepatitis starting. This is a key time for doctors to watch patients closely.
Six-Month Development Timeline
Studies suggest HAAA can appear in six months after severe autoimmune hepatitis starts. This time is very important for early detection.
It’s wise to keep a close eye on patients with autoimmune hepatitis, mainly in the first six months. This helps catch bone marrow failure early.
Diagnostic Criteria and Monitoring
To diagnose HAAA, doctors use clinical checks, lab tests, and bone marrow biopsies. The signs include low counts of blood cells and a small bone marrow.
|
Diagnostic Criteria |
Description |
|---|---|
|
Pancytopenia |
Low counts of red blood cells, white blood cells, and platelets |
|
Bone Marrow Biopsy |
Hypocellular marrow indicating bone marrow failure |
|
Autoimmune Hepatitis Diagnosis |
Confirmed through liver function tests and biopsy |
Monitoring includes regular blood tests and bone marrow checks for those with severe autoimmune hepatitis.
Knowing the link between autoimmune hepatitis and HAAA helps doctors act fast. This can greatly improve the chances of better outcomes for patients at risk.
The Apathetic Presentation: Recognizing Subtle Symptoms
Aplastic anemia can look like other diseases, making it hard to spot. It starts with symptoms that seem like other things, leading to late diagnosis and treatment.
Fatigue and Weakness Patterns
Fatigue and weakness are early signs of aplastic anemia. The bone marrow not making enough red blood cells means less oxygen for the body. This can feel like chronic fatigue or a vitamin lack.
Fatigue in aplastic anemia gets worse over time if not treated. It’s not just tiredness; it’s a sign of a serious problem.
Bleeding Tendencies and Bruising
Another sign is bleeding or bruising easily. This is because the body doesn’t make enough platelets for blood to clot. People might see easy bruising, frequent nosebleeds, or bleeding that won’t stop.
These signs are serious and need checking out. Small red or purple spots on the skin, called petechiae, also mean low platelet counts.
Infection Susceptibility and Management
Aplastic anemia makes people more likely to get infections. This is because the body doesn’t make enough white blood cells to fight off germs. People might get infections that don’t go away quickly.
Dealing with infections in aplastic anemia is tricky. Doctors have to treat infections but also worry about hurting the bone marrow more.
Spotting the early signs of aplastic anemia is key to treating it right. Knowing about fatigue, bleeding, and infections helps doctors catch it early and start treatment.
Less Common Autoimmune Triggers of Aplastic Anemia
Aplastic anemia can be caused by many autoimmune diseases, some of which are not as well-known. While we often talk about common causes, there are other autoimmune disorders that can also trigger this condition.
Sjögren’s Syndrome
Sjögren’s syndrome is a chronic autoimmune disease. It mainly affects the exocrine glands, like the salivary and lacrimal glands. This leads to dry mouth and dry eyes, but it can also affect other parts of the body.
There is evidence that Sjögren’s syndrome can lead to aplastic anemia, though it’s rare. The immune system’s attack on bone marrow cells is thought to be the link between the two conditions.
Key Features of Sjögren’s Syndrome:
- Autoimmune exocrinopathy
- Systemic manifestations beyond glandular symptoms
- Potential for hematologic complications
Antiphospholipid Syndrome
Antiphospholipid syndrome (APS) is an autoimmune disorder. It’s known for causing thrombosis and pregnancy problems. APS is also linked to aplastic anemia, though it’s not as common.
The exact way APS causes aplastic anemia is not fully understood. But, it’s believed to involve the immune system suppressing the bone marrow.
|
Condition |
Primary Manifestations |
Hematologic Implications |
|---|---|---|
|
Sjögren’s Syndrome |
Dry eyes, dry mouth |
Aplastic anemia, other cytopenias |
|
Antiphospholipid Syndrome |
Thrombosis, pregnancy complications |
Aplastic anemia, thrombocytopenia |
|
Mixed Connective Tissue Disease |
Features of lupus, scleroderma, and myositis |
Aplastic anemia, other hematologic abnormalities |
Mixed Connective Tissue Disease
Mixed connective tissue disease (MCTD) is an autoimmune disorder. It combines symptoms of lupus, scleroderma, and myositis. MCTD is characterized by anti-U1 RNP antibodies. It can affect many parts of the body, but aplastic anemia is rare.
It’s important to watch for hematologic problems in patients with MCTD. This can help prevent aplastic anemia.
In conclusion, while aplastic anemia is often linked to common autoimmune diseases, it’s important to know about less common ones. Sjögren’s syndrome, antiphospholipid syndrome, and mixed connective tissue disease can also cause it. Early detection and treatment can help prevent aplastic anemia.
Diagnostic Approach to Autoimmune-Related Aplastic Anemia
Diagnosing autoimmune-related aplastic anemia is complex. We use a detailed strategy to find this condition.
Blood Tests and Complete Blood Count Analysis
First, we do blood tests and a complete blood count (CBC) analysis. A CBC shows the levels of red, white blood cells, and platelets. In aplastic anemia, all counts are low.
Bone Marrow Biopsy Procedures
A bone marrow biopsy is vital for diagnosing aplastic anemia. We take a sample from the hipbone. This test checks the bone marrow’s health.
We do bone marrow biopsies under local anesthesia to reduce pain. This test shows the bone marrow’s structure and cells, helping diagnose aplastic anemia.
Autoimmune Markers and Specialized Testing
We also test for autoimmune markers. These tests find underlying autoimmune disorders that may cause aplastic anemia. We look for antinuclear antibodies (ANA), rheumatoid factor, and other autoantibodies.
says, “Testing for autoimmune markers is key. It helps us treat both the bone marrow failure and the autoimmune condition.”
By using blood tests, bone marrow biopsies, and autoimmune marker tests, we can accurately diagnose autoimmune-related aplastic anemia. Then, we create a treatment plan.
Immunosuppressive Therapy: The Cornerstone of Treatment
Immunosuppressive therapy is key in treating aplastic anemia. It works by calming down the immune system’s attack on bone marrow cells. This helps to start making blood cells again.
First-Line Treatment Protocols
The first treatment often includes antithymocyte globulin (ATG) and cyclosporine. ATG gets rid of T-cells, which harm bone marrow. Cyclosporine stops T-cells from getting active, making the treatment more effective.
“Immunosuppressive therapy has changed how we treat aplastic anemia,” say top hematologists. This method has greatly helped patients, giving them a good alternative to bone marrow transplants.
Response Rates and Long-term Efficacy
Research shows that this therapy works for 60-80% of patients. Many patients keep responding for years. Survival rates have jumped to 80-85% thanks to this treatment.
“Immunosuppressive therapy is now the main treatment for aplastic anemia, except for those needing bone marrow transplants,” say recent guidelines.
Monitoring Parameters and Therapy Adjustments
Keeping an eye on patients on this therapy is vital. We check blood counts, liver function, and cyclosporine levels often. Adjusting the treatment for each patient is key to success.
Understanding immunosuppressive therapy helps us manage aplastic anemia better. This improves our patients’ lives.
Stem Cell Transplantation for Severe Cases
For those with severe aplastic anemia, stem cell transplantation is a hopeful cure. This method replaces damaged bone marrow with healthy stem cells. These can come from the patient (autologous transplant) or a donor (allogenic transplant).
Patient Selection Criteria
Choosing stem cell transplantation depends on several factors. These include the aplastic anemia’s severity, the patient’s age, health, and donor availability. Patients with very severe aplastic anemia who didn’t respond to other treatments are often considered for this option.
We look at each patient’s medical history, current health, and how likely they are to benefit. We also consider any existing health issues and their ability to handle the treatment.
Procedure Details and Process
The process starts with a conditioning regimen. This uses chemotherapy and/or radiation to clear out the damaged bone marrow. Then, the patient gets the stem cell graft through an IV, like a blood transfusion.
Post-transplant care is key. We watch for signs of the new marrow working, manage risks like graft-versus-host disease (GVHD), and support the patient to avoid infections and other problems.
Outcomes and Survival Rates
The success of stem cell transplantation for severe aplastic anemia depends on many factors. These include the patient’s age, the donor match, and the treatment used. Survival rates have gotten better thanks to better techniques, care, and managing GVHD.
We keep a close eye on patients after the transplant to see how they’re doing and handle any issues quickly. The goal is to get rid of the bad marrow without causing too much harm from the treatment.
Managing Concurrent Autoimmune Disease and Aplastic Anemia
When a patient has both autoimmune disease and aplastic anemia, managing their care is key. Coordinating treatment is essential to handle their health issues well.
These two conditions can affect each other, making treatment harder. Autoimmune diseases can make aplastic anemia worse, and vice versa.
Treatment Prioritization Strategies
Choosing which condition to treat first is critical. Clinical judgment helps decide based on symptoms and health.
If the autoimmune disease is severe, starting immunosuppressive therapy might be needed. This helps control the autoimmune response before treating aplastic anemia.
- Assess the severity of both conditions.
- Determine the most critical condition to treat first.
- Develop a detailed treatment plan.
Medication Interactions and Considerations
Choosing the right medications for both conditions is important. Some drugs used for autoimmune diseases can make aplastic anemia worse.
So, we must pick medications carefully and watch their effects. Drug interactions can be avoided by adjusting doses or using different drugs.
Multidisciplinary Team Approach
A multidisciplinary team is essential for patients with both conditions. This team includes hematologists, rheumatologists, and immunologists.
Together, healthcare providers can create a treatment plan that works for both conditions. This improves patient outcomes and quality of life.
In conclusion, managing both conditions requires a detailed and multifaceted approach. It involves prioritizing treatment, managing medications, and using a team of specialists for the best care.
Innovative Approaches at Specialized Centers
Centers like LIV Hospital are changing how we treat aplastic anemia. They use new treatment methods. LIV Hospital aims to give top-notch care by using the latest in medical science.
Treatment Protocols at LIV Hospital
LIV Hospital’s treatment for aplastic anemia covers all aspects of care. It includes immunosuppressive therapy tailored for each patient. This approach helps both the body and mind of patients.
Studies show that immunosuppressive therapy works well for aplastic anemia. Some patients see big improvements. A study on highlights the need for ongoing research in this area.
International Best Practices
LIV Hospital follows global standards for treating aplastic anemia. We use multidisciplinary care models. This means teams of experts work together to create detailed treatment plans.
We keep our treatment plans up-to-date with the latest research. Experts say that teamwork is key in treating complex diseases like aplastic anemia.
“The future of aplastic anemia treatment lies in the continued innovation and collaboration among healthcare professionals, researchers, and patients.”
This forward-thinking approach is what drives us at LIV Hospital to push the boundaries of what’s possible in patient care.
Multidisciplinary Care Models
Multidisciplinary care is vital for treating aplastic anemia. It brings together hematologists, immunologists, and more. This way, we can tackle the complex needs of our patients.
Our team works with patients to offer support and education. We want patients to be able to make informed decisions about their care. This teamwork is at the core of our mission to provide top healthcare.
Conclusion
It’s key to understand how autoimmune diseases and aplastic anemia are connected. We’ve looked into how autoimmune attacks can cause aplastic anemia. This includes the damage done by T-cells and the imbalance of cytokines.
Aplastic anemia is a complex issue that needs special care. People with autoimmune diseases are more likely to get it. It’s important to spot the early signs and diagnose it quickly.
Managing aplastic anemia linked to autoimmune diseases needs a team effort. This includes using immunosuppressive drugs and sometimes stem cell transplants. We stress the need for a full care plan, including how to handle treatments and medications.
Knowing the connection between autoimmune diseases and aplastic anemia helps doctors give top-notch care. This is true for patients from around the world who need advanced medical help and support.
FAQ
What is aplastic anemia, and how is it related to autoimmune diseases?
Aplastic anemia is when the bone marrow can’t make blood cells. Autoimmune diseases can cause this by attacking the bone marrow.
What are the symptoms of aplastic anemia, and how do they differ from other blood disorders?
Symptoms include feeling very tired, weak, and getting sick easily. Aplastic anemia is special because it affects all blood cell types.
How is aplastic anemia diagnosed, and what tests are used to confirm the condition?
Doctors use blood tests and a bone marrow biopsy to diagnose it. They also check for autoimmune markers.
What is the role of immunosuppressive therapy in treating aplastic anemia?
Immunosuppressive therapy helps by stopping the immune system from attacking the bone marrow. It’s a key part of treatment.
Can stem cell transplantation be used to treat severe aplastic anemia, and what are the criteria for patient selection?
Yes, stem cell transplantation is an option for severe cases. The choice depends on how severe the disease is, the patient’s age, and health.
How do autoimmune diseases like systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) contribute to the development of aplastic anemia?
Autoimmune diseases like SLE and RA can cause aplastic anemia. They do this by destroying bone marrow cells and disrupting cytokine balance.
What are the challenges in managing patients with concurrent autoimmune disease and aplastic anemia?
Managing these patients is tough. It needs a team effort, careful planning, and watching for drug interactions.
Are there any rare autoimmune diseases that can lead to aplastic anemia?
Yes, diseases like Sjögren’s Syndrome, antiphospholipid syndrome, and mixed connective tissue disease can also cause aplastic anemia.
What is the significance of understanding the link between autoimmune diseases and aplastic anemia?
Knowing this link is key for better care. It helps in creating targeted treatments and improving patient results.
What is pernicious anemia, and how does it differ from aplastic anemia?
Pernicious anemia is caused by a lack of vitamin B12, leading to anemia. Aplastic anemia is when the bone marrow can’t make blood cells.
How does being apathetic relate to the experience of having aplastic anemia?
Patients with aplastic anemia might seem apathetic due to constant fatigue and weakness. This affects their quality of life.
What is the difference between microcytic anemia and aplastic anemia?
Microcytic anemia is about small red blood cells. Aplastic anemia is when the bone marrow can’t make any blood cells, leading to pancytopenia.
Can you define platonic in the context of medical care?
In medicine, platonic means a caring, non-romantic relationship between healthcare providers and patients. It’s about compassion and care.
References:
• StatPearls. (n.d.). Aplastic anemia. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK534212/
• NORD. (n.d.). Acquired aplastic anemia – symptoms, causes, treatment. Retrieved from https://rarediseases.org/rare-diseases/acquired-aplastic-anemia/
• Aplastic Anemia and MDS International Foundation (AAMDSIF). (n.d.). Aplastic anemia. Retrieved from https://www.aamds.org/aplastic-anemia
• Nature. (2019). A rare complication of allogeneic hematopoietic stem cell transplantation. Retrieved from https://www.nature.com/articles/s41409-019-0680-4
• ScienceDirect. (2017). An overview of an article on Bone Marrow Transplant. Retrieved from https://www.sciencedirect.com/science/article/pii/S1040842817317708
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/19020928/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























