Explore the primary diseases affecting your bone marrow. Learn about leukemia and anemia, and how these conditions impact your daily health.
Bone marrow diseases are a big worry for many. Bone marrow is the spongy tissue in some bones. It has stem cells that turn into red blood cells, white blood cells, and platelets.
Two major conditions that hit this vital tissue are leukemia and aplastic anemia. Leukemia is a blood cancer. Aplastic anemia makes the bone marrow fail to make blood cells.
It’s key to know about these diseases for the right diagnosis and treatment. We’ll look at how these conditions affect blood cell production in the bone marrow. This can lead to many health problems.
Key Takeaways
- Leukemia is a type of cancer affecting blood cells.
- Aplastic anemia is a condition where bone marrow fails to produce blood cells.
- Both conditions impact the production of blood cells.
- Understanding these diseases is crucial for diagnosis and treatment.
- Bone marrow diseases can lead to various health issues.
The Essential Functions of Bone Marrow in the Human Body
Bone marrow is key to making blood cells in our body. It’s a vital organ in our hematopoietic system. It makes the cells that are in our blood.
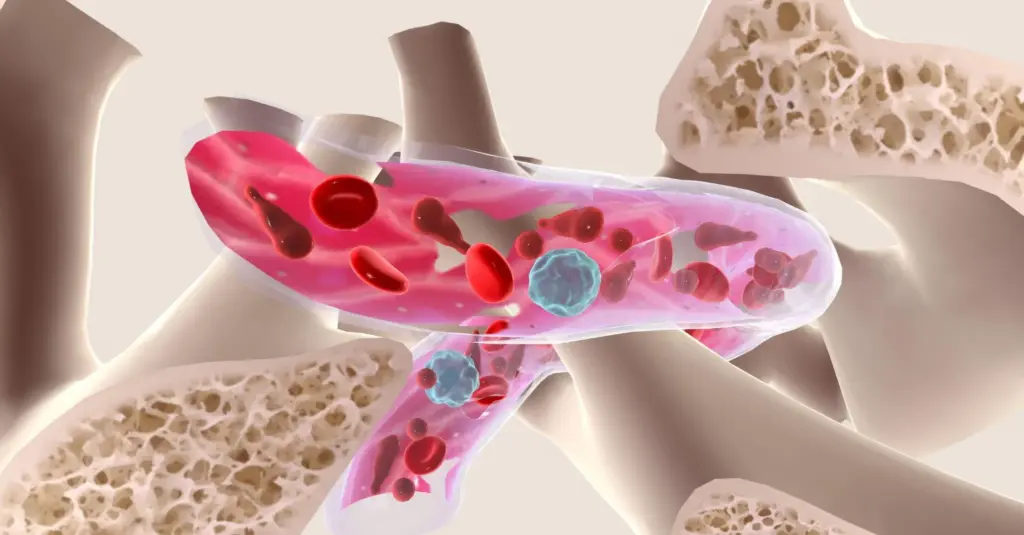
Composition and Structure of Bone Marrow
Bone marrow is spongy tissue inside bones like hips and thighbones. It has stem cells that turn into blood cells. These cells are red blood cells, white blood cells, and platelets.
The marrow has blood vessels and fibrous tissue. They help the cells grow.
There are two types of bone marrow: red and yellow. Red bone marrow makes blood cells through hematopoiesis. It’s in the spongy part of bones and has lots of blood vessels. Yellow bone marrow is mostly fat and doesn’t make blood cells.
Hematopoiesis: The Blood Cell Production Process
Hematopoiesis is how bone marrow makes blood cells. It starts with hematopoietic stem cells. These cells turn into different cell types.
Research says hematopoiesis is a complex process. It involves many cell types and growth factors .
The process has several stages. It goes from stem cell to mature blood cell. Here’s a simple overview:
|
Cell Type |
Function |
Maturation Site |
|---|---|---|
|
Red Blood Cells |
Carry oxygen throughout the body |
Bone Marrow |
|
White Blood Cells |
Part of the immune system, fighting infections |
Bone Marrow and Lymphoid Organs |
|
Platelets |
Involved in blood clotting |
Bone Marrow |
Bone marrow is crucial for making these cells. Any problem with it can cause health issues. This includes diseases like leukemia and aplastic anemia.
How Bone Marrow Diseases Develop and Impact Health
It’s important to understand how bone marrow diseases start. They can come from genes and the environment. This leads to problems with making blood cells.
Common Mechanisms of Bone Marrow Dysfunction
Bone marrow can go wrong in many ways. Genes can mess up blood cell making. Chemicals or radiation can also harm it. Autoimmune diseases can attack the marrow too.
These problems can be complex. For example, genes can cause myelodysplastic syndromes. This is when the marrow can’t make healthy blood cells. Exposure to things like benzene can also raise the risk of these diseases.
Systemic Effects of Compromised Bone Marrow
When bone marrow is not working right, it affects the whole body. Anemia, infections, and bleeding disorders are common. Anemia makes you tired and weak. Infections happen because of a lack of white blood cells. Bleeding disorders make it hard for blood to clot.
The effects of bad bone marrow can be big. For instance, anemia can cause shortness of breath. Bleeding disorders can make you bruise easily or bleed a lot.
|
Systemic Effect |
Cause |
Symptoms |
|---|---|---|
|
Anemia |
Lack of red blood cells |
Fatigue, weakness, shortness of breath |
|
Infections |
Deficiency in white blood cells |
Frequent infections, fever, chills |
|
Bleeding Disorders |
Low platelet count |
Bruising, prolonged bleeding, petechiae |
Leukemia: Cancer of the Bone Marrow
Leukemia starts in the bone marrow. It’s a cancer of the blood cells. It makes abnormal white blood cells grow too much, messing up blood cell production.
Definition and Pathophysiology
Leukemia is a cancer that affects the blood and bone marrow. It’s caused by abnormal white blood cells, which are key for our immune system. These cells grow out of control because of genetic mutations.
Key aspects of leukemia’s pathophysiology include:
- Genetic mutations in blood cells
- Uncontrolled cell proliferation
- Interference with normal blood cell production
How Leukemia Disrupts Normal Blood Cell Production
Leukemia messes up the bone marrow’s job to make healthy blood cells. This includes red blood cells, white blood cells, and platelets. It can cause anemia, infections, and bleeding disorders.
Leukemia’s effect on blood cell production is big. It hurts our body’s ability to carry oxygen, fight off infections, and stop bleeding.
Four Major Types of Leukemia
Leukemia is a cancer that starts in the bone marrow. It is divided into four main types, each with its own traits and treatment plans. Knowing these differences is key for the right diagnosis and treatment.
Acute Lymphoblastic Leukemia (ALL)
Acute Lymphoblastic Leukemia (ALL) is a fast-growing cancer. It affects the lymphoid cells in the bone marrow. This leads to an overproduction of immature lymphocytes, which take over and weaken the immune system.
Symptoms of ALL include feeling very tired, looking pale, and getting sick often. The usual treatment is strong chemotherapy.
Acute Myeloid Leukemia (AML)
Acute Myeloid Leukemia (AML) is a fast-moving cancer that affects the myeloid cells. It causes the bone marrow to make bad white blood cells. Symptoms include shortness of breath, easy bruising, and getting sick often.
AML treatment often includes chemotherapy and sometimes a bone marrow transplant.
Chronic Lymphocytic Leukemia (CLL)
Chronic Lymphocytic Leukemia (CLL) is a slow-growing cancer that affects the lymphoid cells. It causes mature lymphocytes to build up in the blood, bone marrow, and lymphoid tissues.
CLL might not show symptoms at first. But as it gets worse, it can cause tiredness, weight loss, and frequent sickness. Treatment for CLL depends on how far it has spread and may include special therapies.
Chronic Myeloid Leukemia (CML)
Chronic Myeloid Leukemia (CML) is a cancer that affects the myeloid cells. It leads to the production of abnormal white blood cells. CML grows slowly and can cause tiredness, weight loss, and a big spleen.
Treatment for CML often involves special therapy. This has greatly improved how well patients do.
|
Type of Leukemia |
Characteristics |
Common Symptoms |
Typical Treatment |
|---|---|---|---|
|
ALL |
Rapidly progressing, affects lymphoid cells |
Fatigue, pale skin, infections |
Chemotherapy |
|
AML |
Aggressive, affects myeloid cells |
Shortness of breath, bruising, infections |
Chemotherapy, bone marrow transplant |
|
CLL |
Slow-progressing, affects lymphoid cells |
Fatigue, weight loss, infections |
Targeted therapies |
|
CML |
Slow-progressing, affects myeloid cells |
Fatigue, weight loss, enlarged spleen |
Targeted therapy |
Leukemia Statistics in the United States
<SEP-1555_image_2>
It’s important to know about leukemia statistics in the U.S. This disease affects thousands of Americans every year. It’s a big health issue.
Annual Incidence and Prevalence Rates
Every year, over 60,000 new cases of leukemia are found in the U.S. This makes it one of the most common cancers here. The annual incidence rate shows how many new cases happen in a year.
The number of people living with leukemia is also high. Different types of leukemia have different prevalence rates. Some are more common than others.
Key Statistics:
- Over 60,000 new leukemia cases are diagnosed each year.
- Leukemia is among the top 10 most common cancers in the U.S.
- Prevalence rates vary significantly among different leukemia types.
Demographic Patterns and Risk Factors
Demographic patterns and risk factors are key to understanding leukemia. Age, gender, and ethnicity are important. They affect the risk of getting leukemia.
Acute Lymphoblastic Leukemia (ALL) is common in kids. Acute Myeloid Leukemia (AML) and Chronic Lymphocytic Leukemia (CLL) are more common in adults. Genetic syndromes and exposure to radiation or chemicals also raise the risk.
- Age: The risk of most types of leukemia increases with age.
- Gender: Some types of leukemia are more common in men than in women.
- Ethnicity: Certain ethnic groups have a higher incidence of specific leukemia types.
Knowing these patterns and risk factors helps in creating better prevention and treatment plans.
Recognizing Leukemia: Symptoms and Warning Signs
Spotting leukemia early is key. It’s a blood and bone marrow cancer with various symptoms. Catching these signs early can help get the right treatment fast.
Common Clinical Manifestations
Leukemia symptoms can be tricky to spot. They might look like other illnesses. Common signs include fatigue, weight loss, and frequent infections.
These happen because leukemia messes with blood cell making. This leads to fewer healthy cells in the blood.
Other signs might be pale skin from anemia, easy bruising or bleeding from low platelets, and swollen lymph nodes or spleen. Some people might feel bone pain or tenderness in places like hips, ribs, or sternum. This is because leukemia cells build up in the bone marrow.
When to Seek Medical Attention
If you’re losing weight without trying, experiencing frequent illnesses, or noticing excessive bleeding, it’s crucial to seek medical attention promptly. Early treatment can really help with leukemia.
Doctors say knowing the signs of leukemia is the first step to fighting it. Seeing a doctor right away is important if you notice these symptoms.
“The key to managing leukemia lies in early detection and appropriate treatment. Being aware of the common symptoms can lead to timely intervention.”
—Hematologist
We urge everyone to watch their health closely. If you’re worried about symptoms that might be leukemia, talk to a doctor.
Diagnosing Leukemia: From Blood Tests to Bone Marrow Biopsy
Diagnosing leukemia involves several steps. First, there are initial tests and lab work. Sometimes, a bone marrow biopsy is needed. This process helps find the right treatment.
Initial Screening and Laboratory Tests
The first step is often a complete blood count (CBC). This test checks the levels of blood cells. If the white blood cell count is off, it might mean leukemia.
After a CBC shows something odd, more tests follow. These help confirm if it’s leukemia. Tests include:
- Blood smear: Looks at blood cell shapes.
- Flow cytometry: Analyzes cell characteristics.
- Cytogenetic analysis: Checks chromosomes for genetic issues.
|
Test |
Purpose |
|---|---|
|
Complete Blood Count (CBC) |
Measures levels of different blood cells. |
|
Blood Smear |
Examines the morphology of blood cells. |
|
Flow Cytometry |
Analyzes the characteristics of cells. |
The Bone Marrow Biopsy Procedure
A bone marrow biopsy is key for diagnosing leukemia. It takes a small bone marrow sample, usually from the hipbone. This helps find out if leukemia is present and what type it is.
Doctors say, “A bone marrow biopsy is vital for diagnosing and classifying leukemia. It gives important info on the disease’s progress and helps decide treatment.”
Advanced Diagnostic Techniques
Modern tests like molecular testing and genetic analysis are also important. They help understand leukemia’s specific traits. These tests can find genetic changes that affect treatment options.
“The use of advanced diagnostic techniques has greatly improved our ability to accurately diagnose leukemia. It helps us tailor treatment plans to each patient’s needs.”
— Expert in Hematology
By using initial tests, lab work, and modern techniques, doctors can accurately diagnose leukemia. This leads to effective treatment plans for patients.
Treatment Approaches for Leukemia
Leukemia treatment involves many steps. We’ll look at chemotherapy, targeted therapies, and immunotherapies.
Chemotherapy and Radiation: Cornerstones of Leukemia Treatment
Chemotherapy is a main treatment for leukemia. It uses drugs to kill cancer cells. We choose the right chemotherapy for each patient based on their leukemia type and health.
Radiation therapy is used in some cases. It targets leukemia cells in specific body areas.
Advancements in Targeted and Immunotherapies
Targeted therapies have changed leukemia treatment. They focus on specific disease targets. This makes them more effective and have fewer side effects than traditional chemotherapy.
Immunotherapies, like CAR-T cell therapy, use the immune system to fight leukemia. They offer hope for patients with certain types of leukemia.
Monitoring and Managing Treatment Outcomes
It’s important to check how well treatment is working. We use blood tests and bone marrow biopsies to monitor this.
Managing side effects is also key. We help patients deal with treatment’s effects on their quality of life.
|
Treatment Approach |
Description |
Application |
|---|---|---|
|
Chemotherapy |
Uses drugs to kill leukemia cells |
Primary treatment for most leukemia types |
|
Targeted Therapies |
Targets specific molecular mechanisms |
Used for specific genetic mutations or markers |
|
Immunotherapies |
Harnesses the immune system to fight leukemia |
Emerging treatment for certain leukemia types |
|
Radiation Therapy |
Uses radiation to kill leukemia cells |
Used in specific cases, such as localized disease |
Aplastic Anemia: When Bone Marrow Fails to Produce Blood Cells
Aplastic anemia is a rare and serious condition. It happens when the bone marrow can’t make enough blood cells. This can cause fatigue, infections, and bleeding problems.
Definition and Disease Mechanism
Aplastic anemia means the bone marrow can’t make enough blood cells. This includes red blood cells, white blood cells, and platelets. It happens when the bone marrow’s stem cells get damaged.
The immune system attacks the bone marrow’s stem cells. But what starts this attack isn’t always clear. Sometimes, chemicals, radiation, or infections can trigger it.
Key factors contributing to aplastic anemia include:
- Immune system disorders
- Exposure to toxins or radiation
- Infections
- Genetic predisposition
Distinguishing Aplastic Anemia from Other Cytopenias
Aplastic anemia is different from other cytopenias. The main difference is the bone marrow’s failure to make blood cells. It’s not a problem with the cells themselves.
To diagnose aplastic anemia, doctors do several tests. These include:
- Blood tests to check blood cell counts
- Bone marrow biopsy to look at the marrow’s cells and structure
- Genetic testing to find possible causes
It’s important to understand aplastic anemia well. This helps doctors create better treatment plans and improve patient care.
Causes and Types of Aplastic Anemia
It’s important to know the causes and types of aplastic anemia. This knowledge helps in finding better treatments and improving patient care. Aplastic anemia can be either acquired or inherited.
Acquired Aplastic Anemia: Environmental and Immune Factors
Acquired aplastic anemia happens when external factors harm the bone marrow. This makes it unable to make blood cells. Key factors include:
- Exposure to Toxins: Pesticides, benzene, and some industrial chemicals can harm the bone marrow.
- Radiation Exposure: High radiation, like from nuclear accidents, can badly affect bone marrow.
- Medications: Some drugs, like antibiotics and chemotherapy, can cause aplastic anemia as a side effect.
- Viral Infections: Viruses like hepatitis and HIV can harm bone marrow, leading to aplastic anemia.
- Immune System Disorders: When the immune system attacks the bone marrow, it can cause acquired aplastic anemia.
Inherited Bone Marrow Failure Syndromes
Inherited bone marrow failure syndromes are genetic disorders. They affect the bone marrow’s ability to make blood cells. These conditions are present from birth and can start at different ages. Some notable syndromes include:
- Fanconi Anemia: A rare genetic disorder with bone marrow failure, increased cancer risk, and birth defects.
- Dyskeratosis Congenita: A condition with premature aging of the skin, mucous membranes, and bone marrow failure.
- Shwachman-Diamond Syndrome: Characterized by pancreatic insufficiency, bone marrow problems, and skeletal issues.
These syndromes show the complex genetic causes of some aplastic anemia cases. They highlight the need for detailed genetic testing and counseling.
Recognizing and Diagnosing Aplastic Anemia
Diagnosing aplastic anemia requires a detailed clinical check-up and advanced lab tests. We’ll look at the key steps to diagnose this condition. This includes the first signs and the final tests used.
Clinical Presentations and Physical Findings
Aplastic anemia can be tricky to spot because its symptoms are not specific. Common signs include feeling very tired, weak, and short of breath. These are due to low red blood cells. Also, people might get infections and bleed easily because of low white and platelet cells.
Key clinical findings may include:
- Pallor and fatigue due to anemia
- Petechiae or ecchymosis due to thrombocytopenia
- Fever and infections due to neutropenia
During a physical check-up, doctors might see signs of bone marrow failure. These can be pale skin, spots, or bruises. It’s also important to take a detailed medical history to find out what might have caused it.
Diagnostic Criteria and Testing Protocols
To diagnose aplastic anemia, we use lab tests to check blood cell counts and bone marrow function. The criteria include:
- Peripheral blood counts showing pancytopenia
- Bone marrow biopsy revealing hypocellularity
- Ruling out other causes of bone marrow failure
Bone marrow biopsy is a key test. It shows how many cells are in the marrow and their shape. We also use flow cytometry and cytogenetic analysis to rule out other bone marrow problems.
Ruling Out Other Bone Marrow Disorders
It’s important to tell aplastic anemia apart from other bone marrow issues. These can look similar, like myelodysplastic syndromes or acute leukemia. We use advanced tests, like molecular testing and imaging, to make sure we have the right diagnosis.
By combining what we find in the clinic with lab results, we can accurately diagnose aplastic anemia. Then, we can start the right treatment plan.
Treatment Options for Aplastic Anemia
Managing aplastic anemia needs a treatment plan made just for you. Every patient is different, so the treatment must fit their unique needs and health.
Immunosuppressive Therapy Approaches
Immunosuppressive therapy is a key treatment for aplastic anemia. It aims to stop the immune system from attacking the bone marrow. This therapy often includes anti-thymocyte globulin (ATG) and cyclosporine.
These drugs help the bone marrow recover. They let it start making blood cells again.
Supportive Care: Transfusions and Growth Factors
Supportive care is vital in managing aplastic anemia. It helps ease symptoms and prevents problems. Blood transfusions are used to boost red and white blood cell counts. This reduces the risk of infections and bleeding.
Growth factors like granulocyte-colony stimulating factor (G-CSF) also help. They encourage the bone marrow to make more white blood cells. These cells are key in fighting off infections.
Monitoring Treatment Response and Complications
It’s important to regularly check how well the treatment is working. We watch for signs of bone marrow recovery and any side effects. This careful watching lets us make changes to the treatment if needed.
Stem Cell Transplantation for Bone Marrow Diseases
Bone marrow diseases like leukemia and aplastic anemia can be treated with stem cell transplantation. This method replaces damaged stem cells with healthy ones. It has greatly improved treatment options for these diseases, giving patients a chance for long-term recovery.
The Transplantation Process and Preparation
The stem cell transplantation process is complex. First, patients go through pre-transplant conditioning. This includes chemotherapy and sometimes radiation to remove the diseased bone marrow and weaken the immune system. This step is key for the transplant’s success, allowing the new stem cells to take hold.
We check the patient’s health and medical history to choose the best conditioning regimen. This careful planning helps reduce risks and complications.
Finding Suitable Donors: Family Members vs. Registries
Finding a suitable donor is crucial. Donors can be family members or unrelated individuals from registries. Human leukocyte antigen (HLA) matching is essential for compatibility. Ideally, a sibling or relative is a match, but if not, we look for an unrelated donor through registries like the National Marrow Donor Program (NMDP).
Searching for a donor involves testing for HLA compatibility to avoid graft-versus-host disease (GVHD). We also consider the donor’s age, health, and willingness to donate.
Post-Transplant Care and Recovery Timeline
After the transplant, patients need close monitoring and supportive care. We provide post-transplant care to prevent GVHD, infections, and other issues. Patients are watched for signs of engraftment, which usually happens in 2-4 weeks.
The recovery can take months to a year or more for the immune system to fully recover. We teach patients how to stay safe and manage their health. This includes tips on preventing infections, taking medications, and attending follow-up appointments.
Bone Marrow Donation: Process and Impact
The process of bone marrow donation is complex. It involves many procedures and strict donor requirements. This process has changed the way we treat blood-related disorders, saving lives.
Types of Donation Procedures
Bone marrow donation has two main procedures: bone marrow harvest and peripheral blood stem cell (PBSC) donation. The bone marrow harvest is a surgery that takes marrow from the hipbone. PBSC donation collects stem cells from the bloodstream.
PBSC donation is more common. It’s less invasive and has quicker recovery times for donors.
Donor Requirements and Registry Participation
To donate bone marrow, you must be 18 to 44 years old and in good health. You also need to pass a detailed screening.
Joining the bone marrow registry is key. It boosts the chances of finding a match for patients. Becoming a donor can give patients with blood disorders a second chance at life.
The Critical Need for Diverse Donors
There’s a big need for diverse donors. Patients from different ethnic backgrounds need donors with similar genetic profiles. We’re working to increase diversity in the registry to help more patients.
By becoming a bone marrow donor, you can greatly help patients with blood disorders.
Living with Bone Marrow Diseases: Patient Perspectives
<SEP-1555_image_3>
Living with a bone marrow disease is more than just treatment. It changes a patient’s life in many ways. Patients face many challenges, from managing symptoms to dealing with the emotional side of their illness.
Managing Day-to-Day Challenges
Every day, patients with bone marrow diseases live with uncertainty. Symptom management is key. They need to watch their health closely and make lifestyle changes.
- Maintaining a balanced diet to support overall health
- Avoiding crowded areas and people who are sick to reduce the risk of infection
- Engaging in gentle exercise to combat fatigue
The emotional side of living with a bone marrow disease is also tough. Patients often feel anxious, depressed, and worried about the future. Getting help from mental health professionals is very important.
Support Resources and Patient Communities
There are many support resources for patients with bone marrow diseases. These include patient communities, support groups, and online forums. Organizations also offer information, counseling, and help.
Meeting others who know what it’s like can be very helpful. It makes patients feel less alone and more supported.
Long-term Survivorship Considerations
For those who have been treated for bone marrow diseases, long-term survivorship is key. They need to watch for late effects of treatment and manage chronic health issues. Staying healthy is also important to prevent problems.
- Regular follow-up appointments with healthcare providers
- Surveillance for secondary cancers or other late effects
- Maintaining a healthy lifestyle, including diet and exercise
By knowing the challenges and resources, patients with bone marrow diseases can live better lives.
Conclusion
We’ve looked into bone marrow diseases like leukemia and aplastic anemia. We’ve also talked about the different ways to treat them. It’s key to understand these conditions well to manage them better.
Treating bone marrow diseases is a big job. Doctors use many methods, from chemotherapy to stem cell transplants. Each treatment is chosen based on the patient’s needs, showing how important personalized care is.
Stem cell transplants are a big hope for some patients. They might even cure some diseases. Our work in treating these diseases is always getting better, giving patients new hope.
We want to help patients and doctors understand bone marrow diseases better. Our goal is to make it easier to deal with these complex conditions.
FAQ
What is bone marrow, and what is its function in the human body?
Bone marrow is the spongy tissue inside bones like the hips and thighbones. It makes blood cells, including red and white blood cells, and platelets. This process is called hematopoiesis.
What are the main types of bone marrow diseases?
Main bone marrow diseases include leukemia, aplastic anemia, and other failure syndromes. These affect blood cell production and can cause health problems.
What is leukemia, and how does it affect the body?
Leukemia is cancer in the bone marrow. It makes abnormal white blood cells. This can stop normal blood cell production and cause health issues.
What are the symptoms of leukemia, and when should I seek medical attention?
Symptoms of leukemia include fatigue, weight loss, and frequent infections. If you have these symptoms, see a doctor for diagnosis and treatment.
How is leukemia diagnosed, and what are the diagnostic tests involved?
Diagnosing leukemia involves blood tests, bone marrow biopsies, and other tests. These help find and type the leukemia.
What are the treatment options for leukemia, and how are they determined?
Leukemia treatments include chemotherapy, targeted therapies, and stem cell transplants. The choice depends on the disease type and the patient’s health.
What is aplastic anemia, and how does it differ from other bone marrow disorders?
Aplastic anemia is when the bone marrow can’t make blood cells. It leads to anemia, infections, and bleeding. It’s different from leukemia and needs specific treatment.
What are the causes and risk factors for developing aplastic anemia?
Aplastic anemia can be caused by environmental factors, immune disorders, and genetic mutations. These affect the bone marrow’s blood cell production.
How is aplastic anemia treated, and what are the treatment goals?
Aplastic anemia treatment includes immunosuppressive therapy and transfusions. Stem cell transplantation may also be used. The goal is to restore bone marrow function.
What is the process of bone marrow donation, and how can I become a donor?
To donate bone marrow, register with a donor registry and undergo testing. Then, donate bone marrow or stem cells through surgery. You can register with organizations that manage donor registries.
What are the challenges faced by patients with bone marrow diseases, and how can they be supported?
Patients face challenges like managing symptoms and treatment side effects. Support resources, like patient communities and counseling, help them cope.
What is the importance of diverse bone marrow donors, and how can we increase diversity in the donor pool?
A diverse donor pool is key for patients to find compatible donors. To increase diversity, recruit donors from underrepresented groups and raise awareness about bone marrow donation.
What is red bone marrow, and what is its role in the body?
Red bone marrow produces blood cells through hematopoiesis. It’s in the spongy tissue of bones and is crucial for healthy blood cell production.
What are bone marrow disorders, and how do they affect the body?
Bone marrow disorders, like leukemia and aplastic anemia, affect blood cell production. This can lead to anemia, infections, and bleeding disorders.
References
National Institutes of Health. Evidence-Based Medical Insight. Retrieved from https://www.niddk.nih.gov/health-information/blood-diseases/aplastic-anemia-myelodysplastic-syndromes/symptoms-causes




































