Cancer involves abnormal cells growing uncontrollably, invading nearby tissues, and spreading to other parts of the body through metastasis.
Send us all your questions or requests, and our expert team will assist you.
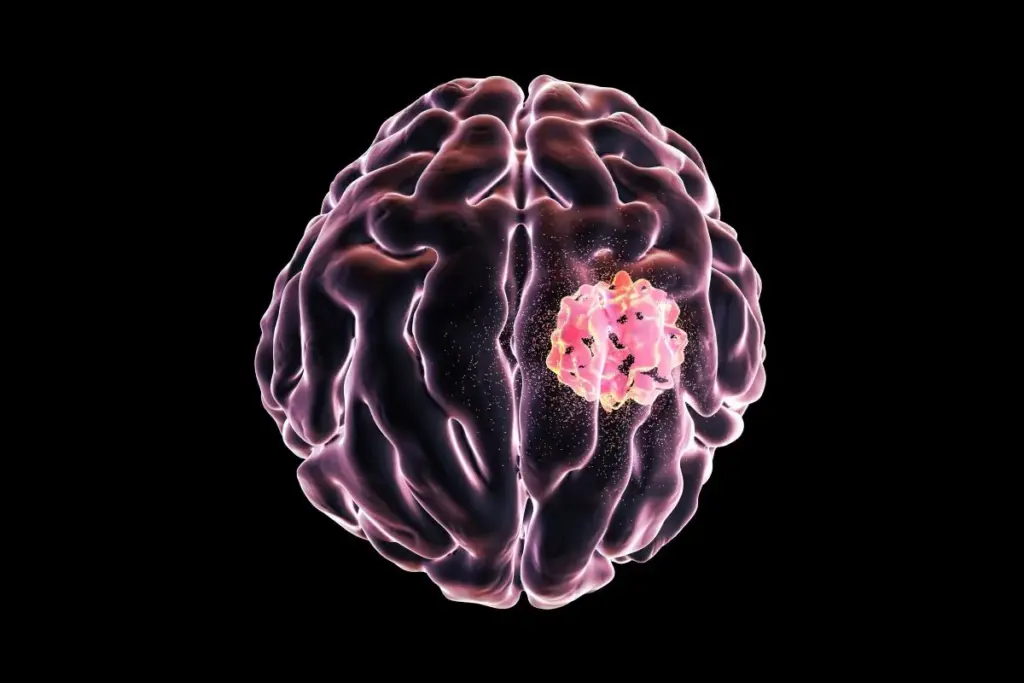
The human brain is the control center of the nervous system. It weighs about 3 pounds and contains billions of neurons and trillions of support cells. The brain sits inside the skull, which protects it from injury but also creates a problem if something goes wrong. Unlike the abdomen or chest, the space inside the skull cannot expand. According to the Monro-Kellie doctrine, the total volume of the brain, cerebrospinal fluid, and blood stays constant. So, if something extra like a tumor appears, it upsets this balance, pushes aside normal tissue, and raises pressure inside the skull.
The brain is protected from changes in blood chemistry and harmful substances by the blood-brain barrier. This barrier is made of tightly joined cells that only let certain things pass from the blood into the brain. While this protects the brain from infections and toxins, it also makes treating brain tumors harder. Most chemotherapy drugs are too large to cross the barrier, so treating brain tumors is more complicated than treating cancers in other parts of the body.
The brain is made up of different types of cells. Neurons send signals, but there are even more glial cells, which support and protect neurons. Astrocytes keep the brain’s chemical balance, oligodendrocytes make the myelin that covers nerves, and ependymal cells line the spaces where cerebrospinal fluid is made. Tumors can start from any of these cells, or from the brain’s coverings, the pituitary gland, or cranial nerves. Knowing which cell a tumor comes from helps doctors classify it and predict how it will behave.
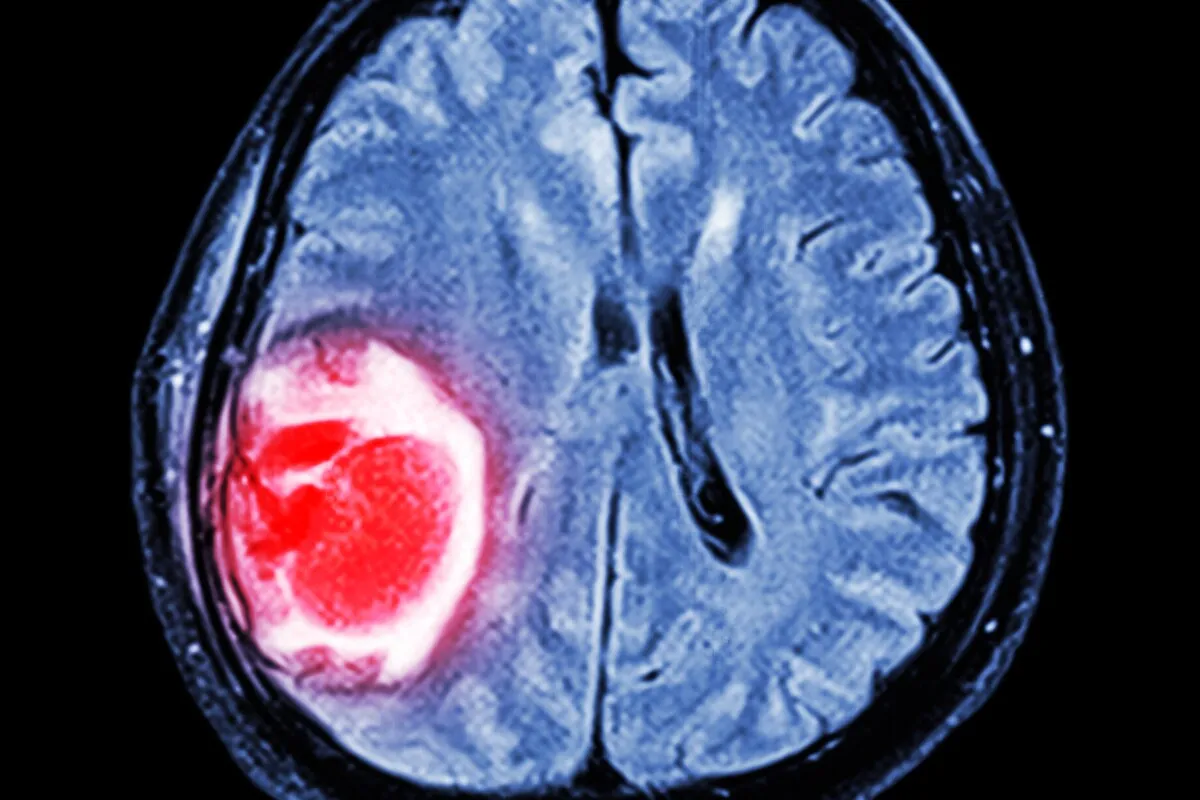
A key difference in brain tumors is whether they are primary or secondary. Secondary, or metastatic, brain tumors are much more common. These cancers start in other parts of the body like the lung, breast, skin (melanoma), kidney, or colon and travel to the brain through the bloodstream. The brain’s high blood flow and special environment make it a common place for these tumors to settle. Metastatic tumors usually form round masses at the border between the brain’s grey and white matter, where cancer cells often get stuck in small blood vessels.
Primary brain tumors start in the brain or its coverings. Unlike most other cancers, they almost never spread to other parts of the body. Instead, they are dangerous because they grow into nearby brain tissue and put pressure on areas that control breathing and heart rate. Primary brain tumors can be slow-growing and benign or very aggressive and fast-growing.
The nomenclature for primary tumors is derived from the cell type they resemble. Gliomas are tumors arising from glial cells and include astrocytomas, oligodendrogliomas, and ependymomas. Meningiomas arise from the arachnoid cap cells of the meninges. Pituitary adenomas arise from the hormone-producing cells of the pituitary gland. Nerve sheath tumors, such as vestibular schwannomas, arise from the Schwann cells covering the cranial nerves. Each of these entities has distinct biological behavior, genetic profiles, and responses to therapy.
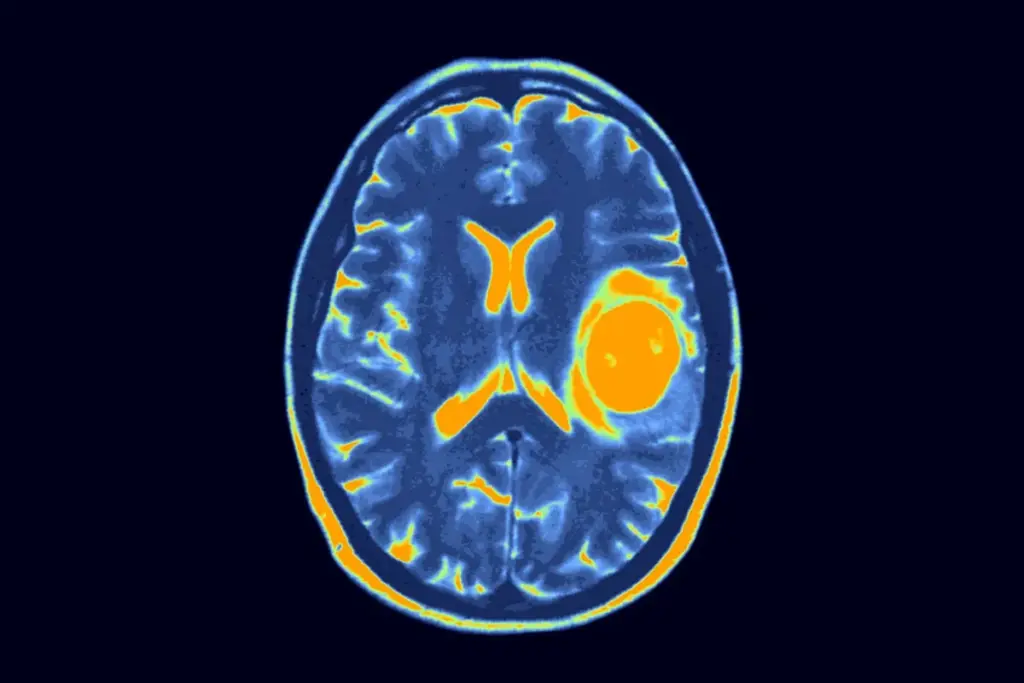
Gliomas are the most common malignant primary brain tumors in adults. In the past, doctors classified them by how they looked under a microscope. But in 2021, the World Health Organization (WHO) changed the system to include genetic information. Now, doctors look at both the tumor’s appearance and its genetic mutations, such as changes in the IDH gene and the loss of parts of chromosomes 1p and 19q.
Astrocytomas are the most frequent gliomas. They are graded on a scale of 1 to 4. Grade 1 (Pilocytic Astrocytoma) is a circumscribed, slow-growing tumor common in children, often curable with surgery alone. Grade 2 (Diffuse Astrocytoma) is infiltrative and slow-growing, but it tends to progress. Grade 3 (Anaplastic Astrocytoma) is a malignant and aggressive tumor. Grade 4, known as Glioblastoma (GBM), is the most common and lethal primary brain tumor in adults. Glioblastomas are characterized by necrosis (dead tissue) and microvascular proliferation (abnormal blood vessel growth) and are now defined by the absence of an IDH mutation (IDH-wildtype).
Oligodendrogliomas are differentiated from astrocytomas by the presence of both an IDH mutation and the 1p/19q codeletion. This molecular signature is prognostic gold: these tumors respond much better to chemotherapy and radiation than astrocytomas, and they carry a significantly longer survival time. Ependymomas, arising from the ventricle lining, are stratified by anatomical location (supratentorial, posterior fossa, or spinal) and specific gene fusions (such as RELA), which more accurately predict aggressiveness than histology alone.

Meningiomas are the most common primary brain tumors, and many are found by accident. They do not start in brain tissue but in the arachnoid mater, a layer covering the brain. Since they are outside the brain itself, they cause problems by pressing on the brain, not by growing into it. Most meningiomas (WHO Grade 1) grow slowly and are benign, and surgery can often cure them. Grade 2 (Atypical) and Grade 3 (Anaplastic) meningiomas are more aggressive, come back more often, and can invade the skull or skin.
Pituitary adenomas are another major category. Located in the sella turcica at the base of the skull, these tumors can disrupt hormonal balance. Functional adenomas secrete excess hormones (such as prolactin or growth hormone), causing systemic syndromes, while nonfunctional adenomas grow silently until they compress the optic chiasm, causing visual field loss. Though rarely malignant in the traditional sense, their proximity to the carotid arteries and optic nerves makes management delicate.
Other non-glial tumors include Vestibular Schwannomas (Acoustic Neuromas), which grow on the nerve connecting the ear to the brain, causing hearing loss and balance issues. CNS Lymphomas are rare aggressive tumors of the immune cells within the brain, often associated with immunocompromised states but increasingly seen in immunocompetent elderly adults. These are unique because they are usually treated primarily with chemotherapy (Methotrexate) rather than surgical resection.

Brain tumors are the most common solid tumors in children, but they are very different from those in adults. In adults, most brain tumors are found in the cerebral hemispheres (supratentorial), while in children, they are often in the back of the brain (posterior fossa), affecting the cerebellum and brainstem. Tumors in this area are especially serious because they can quickly block the flow of cerebrospinal fluid and cause hydrocephalus.
Common brain tumors in children include medulloblastomas, which are highly malignant tumors in the cerebellum that can spread through the cerebrospinal fluid. Pilocytic astrocytomas are benign, cyst-like tumors often found in the cerebellum. Diffuse midline gliomas (previously called DIPG) are very serious tumors in the brainstem that affect areas controlling breathing and heart rate, so they cannot be removed with surgery.
The molecular drivers also differ. Adult gliomas are driven by accumulated mutations associated with aging (such as EGFR amplification or PTEN loss). In contrast, pediatric tumors are often driven by dysregulation of developmental pathways or by histone mutations (such as H3K27M). This divergence means that treatments successful in adults usually fail in children, and vice versa, necessitating distinct research pipelines and clinical trial protocols.

Send us all your questions or requests, and our expert team will assist you.
While “benign” usually implies harmless, in the brain, a benign tumor can still be life-threatening. A benign tumor (like a Grade 1 meningioma) grows slowly and does not invade brain tissue, but it can grow large enough to press on vital structures or increase pressure inside the skull. Malignant tumors grow rapidly and invade the surrounding healthy brain tissue, making complete removal difficult.
The blood-brain barrier is a network of tightly joined cells lining the blood vessels in the brain. It acts as a security checkpoint, preventing toxins and bacteria in the blood from entering the brain. However, it also prevents many chemotherapy drugs from reaching brain tumors, which is a significant challenge in treating these cancers.
The World Health Organization (WHO) grades brain tumors from 1 to 4 based on how abnormal the cells look and how fast they grow. Grade 1 tumors are slow-growing and often curable. Grade 2 is slow-growing but can recur as a higher-grade tumor. Grade 3 is malignant and aggressive. Grade 4 tumors are the most aggressive and fast-growing tumors.
Cancer cells from other parts of the body, like the lungs or breast, often travel through the bloodstream. The brain receives a large amount of blood flow (about 20 percent of the body’s output), making it a common site for circulating cells to become trapped and begin growing.
Primary brain tumors very rarely spread (metastasize) to organs outside the central nervous system. The brain has a unique environment and lacks a lymphatic drainage system connected to the rest of the body in the traditional sense, which keeps these tumor cells contained within the brain and spinal cord.


2cm is how big? Discover scary facts about tumor size and why early detection of a small lump is powerful for your breast cancer recovery

Breast cancer spreading to lymph nodes is a complex process. It depends on the tumor’s biology, size, and molecular subtype. Knowing this timeline is key
Squamous cell lung cancer, a type of non-small cell lung cancer, can spread to the brain. This happens, but not as often as in other
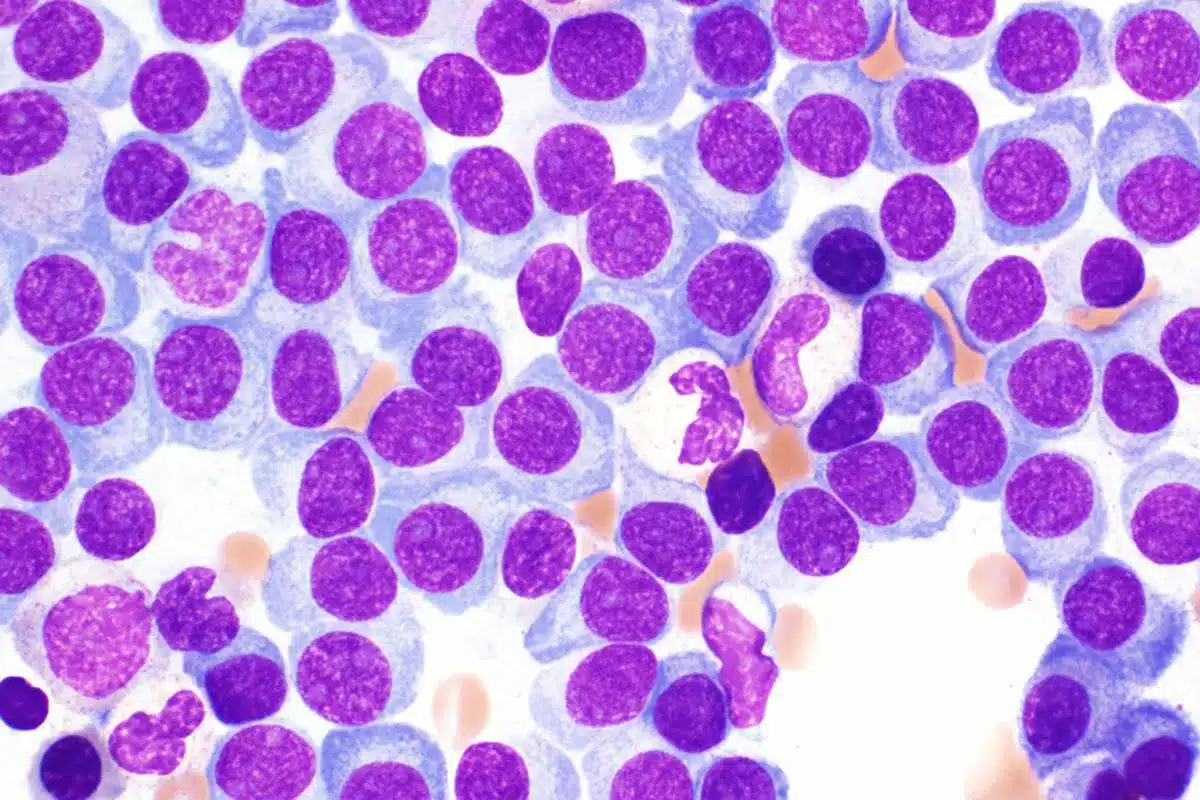
Multiple myeloma, a blood cancer, can harm memory and thinking skills. Studies show that cognitive impairment is common, often seen after treatment. We will look
Lung cancer spreading to the brain presents a significant challenge for doctors. At LIV Hospital, we focus on finding cancer early and using the latest
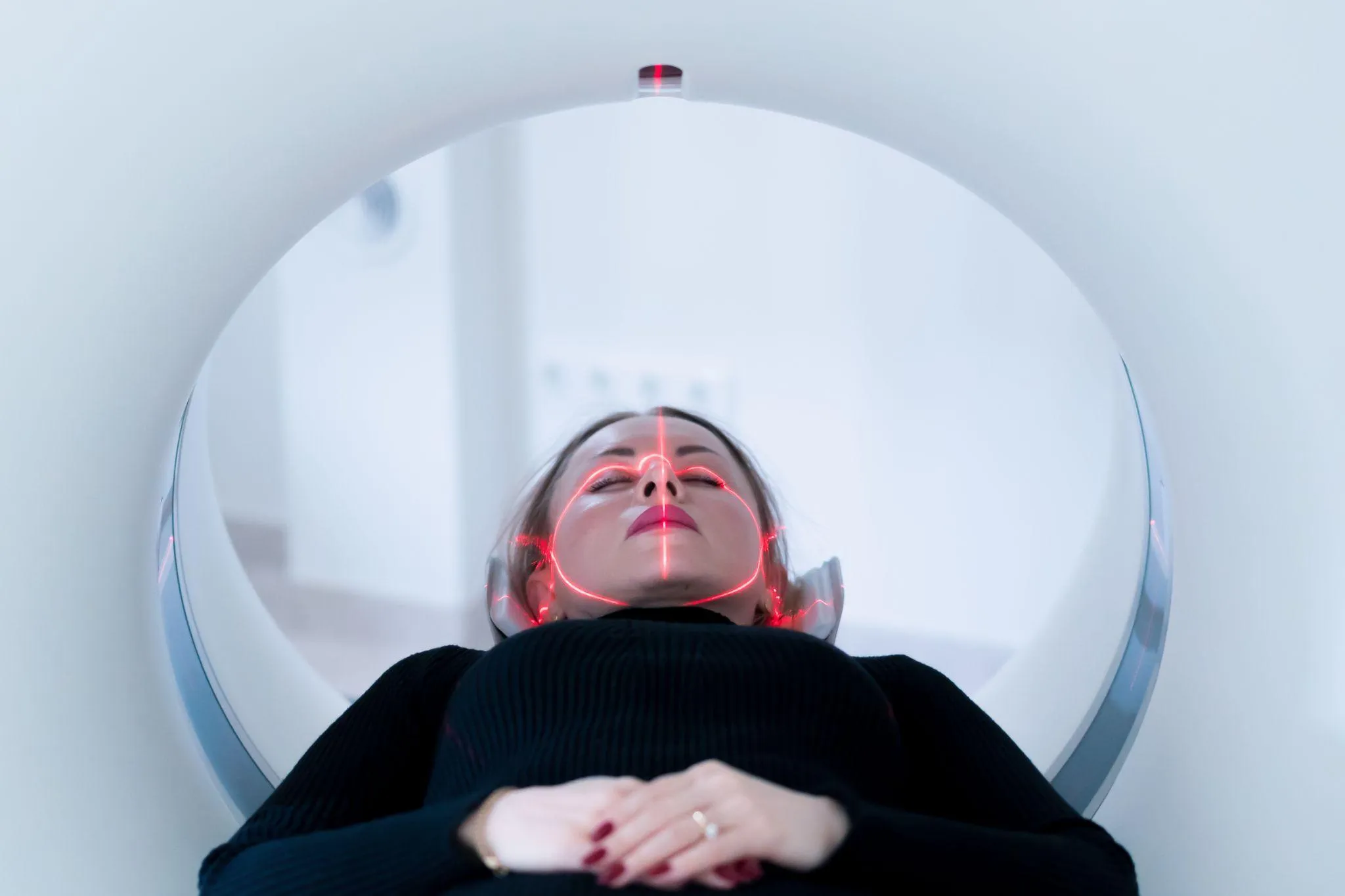
At Liv Hospital, we use advanced tools like PET scans to find brain damage and metabolic issues. A PET scan shows how the brain works

Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)