Cardiology is the medical specialty focused on the heart and the cardiovascular system. It involves the diagnosis, treatment, and prevention of conditions affecting the heart and blood vessels. These conditions include coronary artery disease, heart failure, arrhythmias (irregular heartbeats), and valve disorders. The field covers a broad spectrum, from congenital heart defects present at birth to acquired conditions like heart attacks.
Send us all your questions or requests, and our expert team will assist you.
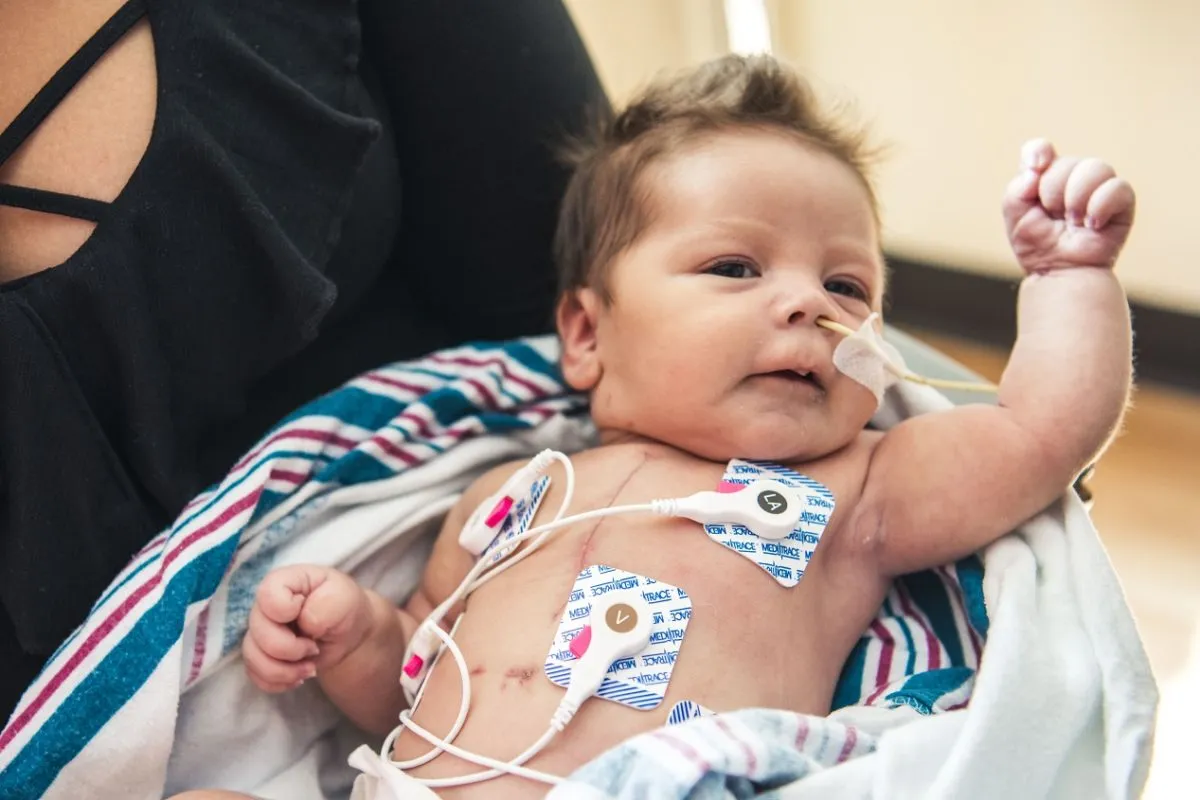
Living with congenital heart disease is a lifelong commitment to health. In the past, children with heart defects were often treated as fragile and kept on the sidelines. Today, the philosophy is radically different: the goal is for patients to live as normally and actively as possible. While we cannot always “prevent” the defect from happening in the first place (since it occurs so early in pregnancy), we can certainly prevent complications and ensure the heart remains strong for decades.
A healthy lifestyle is even more critical for someone with a congenital heart defect than for the general population. A heart that has been repaired or is structurally different has less “reserve” to handle habits. Issues like obesity, high blood pressure, and smoking, which are detrimental for anyone, can be devastating for a congenital heart patient. This section outlines how to protect that special heart through diet, exercise, and smart life choices.
Nutrition plays a vital role in protecting the heart. For infants with heart defects, the focus is often on high-calorie intake. Because they burn so much energy breathing and pumping blood, they may need special fortified formulas to gain weight and grow. Growth is a key indicator of heart health in babies.
For older children and adults, the focus shifts to preventing obesity. Excess weight puts a massive physical strain on the heart. If a heart is already working harder due to a defect, adding the burden of extra body weight can lead to premature heart failure. A heart-healthy diet includes plenty of fruits, vegetables, whole grains, and lean proteins. Sodium (salt) intake should be watched closely, as salt causes the body to hold onto fluid, which increases blood pressure and the workload on the heart.
For congenital heart patients, the statement “Exercise is medicine” holds true. Regular physical activity strengthens the heart’s muscles and the body’s ability to use oxygen. However, the type and intensity of exercise need to be tailored to the specific defect. A cardiologist will provide specific guidelines, often called “sports clearance.”
For the vast majority of patients, recreational activities—like biking, swimming, hiking, and playing tag—are encouraged. The body is good at self-regulating; children will naturally stop and rest when they are tired. Parents should generally allow this self-regulation rather than imposing strict limits unless the doctor says otherwise.
Aerobic activities that bring the heart rate up steadily are excellent. Walking, jogging, and swimming are generally safe and beneficial. They improve cardiovascular endurance without placing extreme sudden stress on the heart.
Competitive sports can be different because the pressure to win might cause an athlete to push through warning signs like dizziness or chest pain. Patients with certain conditions, such as an enlarged aorta or serious rhythm issues, may need to avoid high-intensity static sports (like heavy weightlifting) or collision sports. A specific evaluation is needed before joining competitive teams.
It surprises many people to learn that brushing your teeth is a heart-protection strategy. The mouth is full of bacteria. If gums are bleeding or infected, these bacteria can enter the bloodstream. In a normal heart, they usually pass through without issue. But in a heart with a congenital defect, artificial valve, or patch material, these bacteria can stick to the rough surfaces and cause a life-threatening infection called infective endocarditis.
Because of this risk, excellent dental hygiene is non-negotiable. Regular brushing, flossing, and professional cleanings are essential. For certain high-risk patients—such as those with artificial valves or unrepaired cyanotic defects—the American Heart Association recommends taking a dose of antibiotics one hour before any dental procedures. This preventive step (prophylaxis) kills any bacteria before they can settle in the heart.
Women born with heart defects are now growing up and wanting families of their own. Most women with congenital heart disease can have successful pregnancies, but it requires careful planning. Pregnancy puts a giant stress on the circulatory system; blood volume increases by 50%, and the heart has to pump for two. A repaired heart might struggle with this extra load.
Before becoming pregnant, a woman with CHD should consult an Adult Congenital Heart Disease (ACHD) specialist. They can assess if the heart is strong enough to handle pregnancy. Some medications, such as certain blood thinners or blood pressure drugs, can harm a developing fetus and must be switched before conception. Additionally, because there is a slightly higher risk of passing the defect to the baby, fetal echocardiograms will be planned to check the baby’s heart early.
Living with a chronic condition affects more than just the body; it impacts the mind. Children may feel different from their peers because of their surgical scars (“zipper”) or physical limitations. They might experience anxiety about medical tests. Parents often suffer from significant stress and even PTSD related to their child’s surgeries and hospitalizations.
Depression and anxiety are more common in the congenital heart population than in the general public. It is vital to treat mental health as part of cardiac care. Acknowledging these feelings and seeking support is a sign of strength. Support groups, camps for kids with heart defects, and therapy can be incredibly beneficial. Connecting with others who have shared similar experiences reduces isolation and builds resilience.
One of the biggest dangers for congenital heart patients is the “gap” in care that often happens in early adulthood. When patients turn 18, they age out of the pediatric hospital. If they do not actively transfer to an adult specialist, they may go years without a check-up. They might assume that because they were “fixed” as a kid, they don’t need a doctor anymore.
This is a dangerous myth. As mentioned, congenital hearts are repaired, not cured. Issues like valve leakage, scar tissue arrhythmias, or heart muscle weakness can develop silently in the 20s, 30s, or 40s. Regular visits to an ACHD specialist—even just once every year or two—can catch these problems early when they are easy to treat. Staying in care ensures that the heart remains healthy enough to support a long, full life.

Send us all your questions or requests, and our expert team will assist you.
It depends on your specific heart condition. Guidelines have changed over the years. Currently, antibiotics are recommended for patients with artificial valves, a history of endocarditis, certain cyanotic defects, or repairs with prosthetic material done in the past 6 months. Ask your cardiologist for a wallet card with your specific instructions. a history
Yes, in most cases, a vaginal delivery is actually preferred over a C-section because it involves less blood loss and reduced risk of infection and clots. However, pain management (like an epidural) is important to reduce stress on the heart during labor.
There is a risk of infection with needles. If bacteria enter the blood, they can infect the heart (endocarditis). It is vital to use only professional, sterile shops. Some doctors advise against piercings in mucous membranes (like the tongue or nose) because these areas are teeming with bacteria.
If you take warfarin (Coumadin), you need to be consistent with foods high in vitamin K, such as green leafy vegetables (spinach, kale). You can eat them, but you must eat the same amount weekly to keep your medication dose stable.
In moderation, alcohol is usually permitted for most patients. However, excessive alcohol can weaken the heart muscle and trigger arrhythmias (irregular heartbeats). It can also interact with heart medications. It is best to discuss specific limits with your cardiologist.

 Cardiology
Cardiology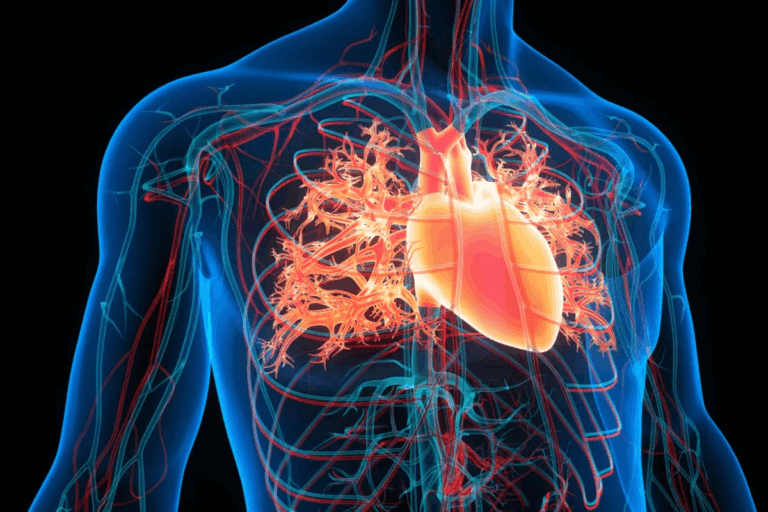 Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)