Cardiology is the medical specialty focused on the heart and the cardiovascular system. It involves the diagnosis, treatment, and prevention of conditions affecting the heart and blood vessels. These conditions include coronary artery disease, heart failure, arrhythmias (irregular heartbeats), and valve disorders. The field covers a broad spectrum, from congenital heart defects present at birth to acquired conditions like heart attacks.
Send us all your questions or requests, and our expert team will assist you.
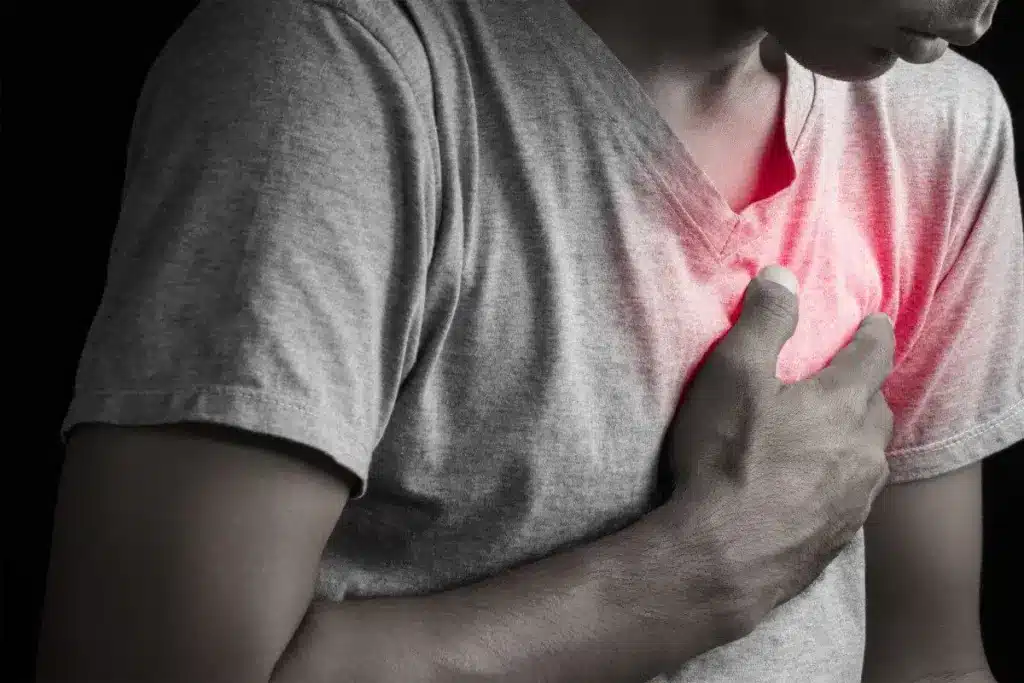

The most common symptom that leads to a recommendation for coronary angiography is chest pain, medically known as angina. Angina is not a disease itself; it is a symptom of an underlying problem, usually reduced blood flow to the heart muscle. Patients often describe it not as sharp pain, but as a pressure, squeezing, heaviness, or tightness in the center of the chest. It can feel like an elephant is sitting on your chest or like a tight band is wrapped around your lungs.
Angina typically occurs when the heart is working harder than usual and needs more oxygen, such as during exercise, emotional stress, or after a heavy meal. If the arteries are narrowed, they cannot deliver the extra blood required, and the heart muscle complains with pain. This pain can radiate, meaning it travels from the chest to the left arm, the neck, the jaw, or even the back. Recognizing the pattern of this pain is crucial for diagnosis.
Stable angina is predictable. It happens at the same level of exertion—for example, every time you walk up two flights of stairs. It usually goes away when you rest or take medication like nitroglycerin. While it needs to be evaluated, it suggests a stable blockage that is not currently changing.
Unstable angina is dangerous. This is chest pain that happens unexpectedly, even when you are resting or sleeping. It might last longer than usual or not go away with medication. This is a warning sign that a heart attack could be imminent and usually leads to an urgent angiogram.

Sometimes, the heart doesn’t hurt; it just gets worn out. Shortness of breath, or dyspnea, is a common “angina equivalent,” especially in older adults or people with diabetes. You might find yourself gasping for air after simple activities like making the bed or walking to the mailbox—activities that used to be easy for you. This occurs because the heart cannot pump efficiently when it is deprived of oxygen, which leads to fluid backing up in the lungs or failing to meet the body’s oxygen demands.
Profound fatigue is another subtle sign. This symptom isn’t just feeling sleepy; it is a deep, bone-weary exhaustion. You might feel like you are walking through mud or that your limbs are incredibly heavy. If you wake up tired or feel exhausted after mild exertion, it could be your heart signaling that its fuel supply is restricted. Because fatigue is common in many illnesses, it is often overlooked as a heart symptom until an angiogram reveals significant blockages.
It is a frightening reality that for some people, the first symptom of heart disease is a massive heart attack. This is known as “silent ischemia.” In these cases, the arteries are narrowing, but the patient feels no pain. This type of condition is particularly common in people with diabetes because high blood sugar can damage the nerves that transmit pain signals from the heart. They literally cannot feel the warning signs.
Women also frequently present with “atypical” symptoms that don’t fit the classic Hollywood image of a heart attack (clutching the chest). Women might experience nausea, indigestion, extreme anxiety, or pain between the shoulder blades. Because these symptoms are vague, they are often dismissed as the flu or stress. Doctors rely on risk factors and non-invasive tests to catch silent heart disease before it causes permanent damage, leading to a preventative angiogram.
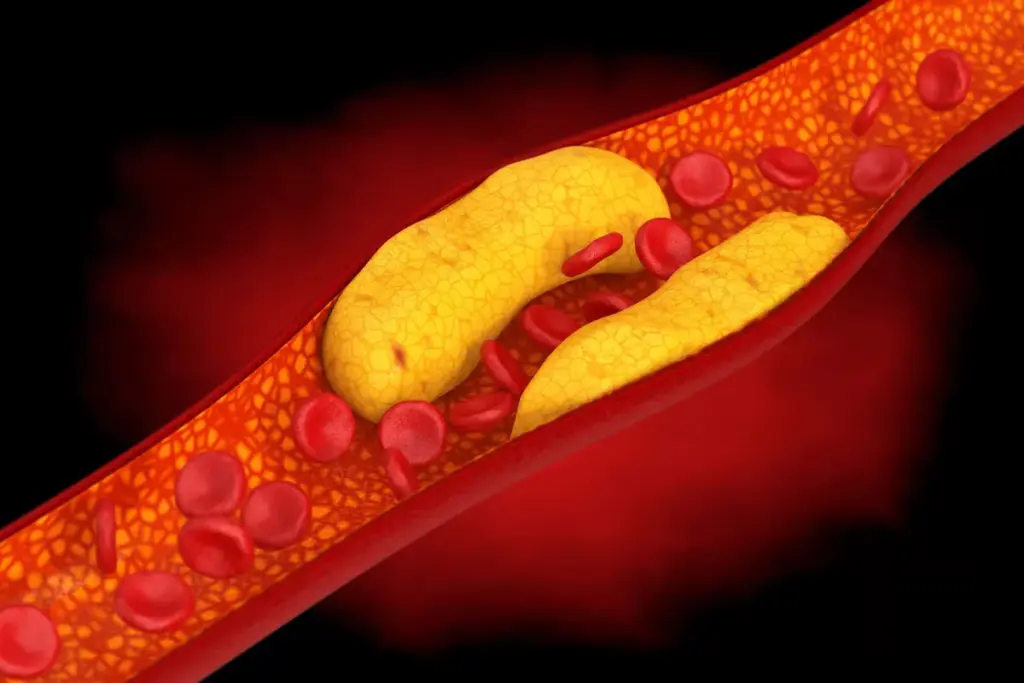
Why do arteries get blocked in the first place? The primary culprit is atherosclerosis, a process where deposits of fat, cholesterol, calcium, and other substances build up in the inner lining of an artery. This buildup is called plaque. High levels of “bad” cholesterol (LDL) in the blood are the raw material for this plaque. High blood pressure is the force that damages the artery walls, creating rough spots where plaque can stick and grow.
Smoking is perhaps the single most preventable risk factor. Chemicals in tobacco smoke damage the blood cells and the structure of the blood vessels, making them prone to collecting plaque. Diabetes is another major accelerant of heart disease; high blood sugar acts like slow-acting poison to the blood vessels, making them stiff and narrow. Being overweight and physically inactive also contributes significantly to the risk profile by raising blood pressure and cholesterol levels.
Occasionally, you can do everything right—eat well, exercise, not smoke—and still develop heart disease. This is where genetics comes into play. If your parents or siblings developed heart disease at a young age, your risk is significantly higher. This situation is not necessarily because you share the same habits, but because you share the same genes that control how your body processes cholesterol and inflammation.
Genetic factors can determine the shape of your arteries, the strength of your vessel walls, and your liver’s ability to clear fats from your blood. While you cannot change your DNA, knowing your family history is a powerful tool. It alerts your doctor to watch you more closely. For someone with a strong family history, an angiogram might be recommended at the first sign of trouble, rather than waiting for symptoms to become severe.
Conditions like familial hypercholesterolemia cause dangerously high cholesterol levels from birth, regardless of diet. These patients often need angiograms in their 30s or 40s.
If a male relative had a heart attack before age 55 or a female relative before age 65, this is considered a red flag for “premature” heart disease. It suggests a more aggressive genetic form of atherosclerosis.
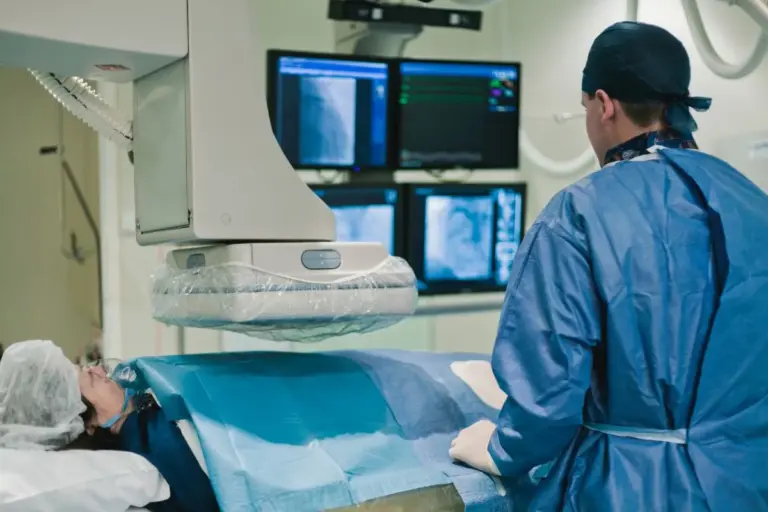
It is critical to know when to stop waiting for an appointment and call 911. An angiogram is often performed as an emergency procedure during a heart attack. The signs of an emergency include chest pain that feels like a crushing weight, lasts more than a few minutes, or goes away and comes back. Pain that spreads to the arm, neck, or jaw is a classic emergency signal.
Other emergency signs include breaking out in a cold sweat, sudden severe nausea, or lightheadedness accompanying the chest pain. If you experience these, do not drive yourself to the hospital. Call an ambulance. Emergency medical teams can start treatment on the way and alert the hospital to have the catheterization lab (where angiograms are done) ready the moment you arrive. Time is muscle; the faster the artery is opened, the less permanent damage occurs.

Send us all your questions or requests, and our expert team will assist you.
Yes, absolutely. This is called silent ischemia. You might experience shortness of breath, fatigue, or nausea instead of pain. This type of condition type of condition is especially common in people with diabetes and in women.
High blood pressure damages the inner lining of the arteries. This damage creates a rough surface where cholesterol plaque can stick and build up, eventually leading to a blockage. It is a major contributor to coronary artery disease.
This is called “referred pain.” The nerves that serve the heart and the nerves that serve the arm and jaw travel along similar pathways to the brain. The brain sometimes gets confused and interprets the heart’s distress signal as coming from the arm or jaw.
Yes, panic attacks can mimic heart symptoms, causing chest tightness, racing heart, and sweating. Physical exertion often triggers heart symptoms, whereas emotional stress frequently triggers panic attacks. An angiogram or other tests can definitively tell the difference.
If you have new or worsening chest pain, shortness of breath, or fatigue, you should stop exercising and see a doctor immediately. Exercising with a severe blockage can be dangerous. Once treated, exercise will likely be part of your recovery plan.

 Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology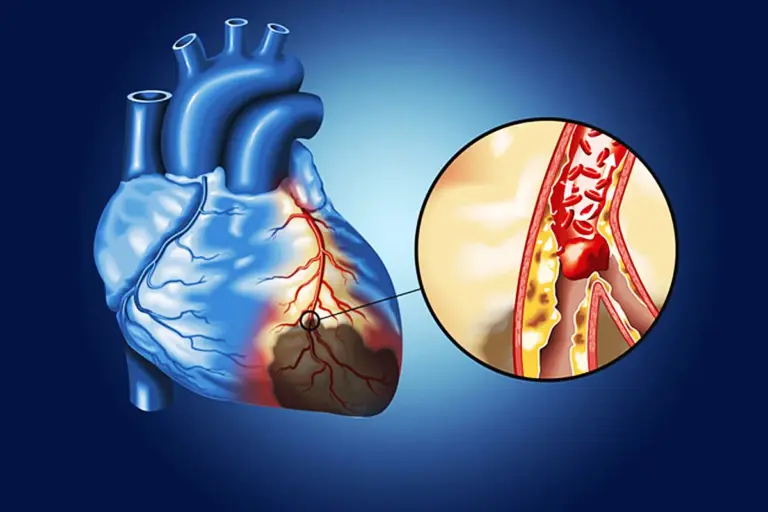 Cardiology
Cardiology
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)