Cardiology is the medical specialty focused on the heart and the cardiovascular system. It involves the diagnosis, treatment, and prevention of conditions affecting the heart and blood vessels. These conditions include coronary artery disease, heart failure, arrhythmias (irregular heartbeats), and valve disorders. The field covers a broad spectrum, from congenital heart defects present at birth to acquired conditions like heart attacks.
Send us all your questions or requests, and our expert team will assist you.

The symptoms of neurocardiac conditions can be perplexing, as they often appear to originate from multiple sources simultaneously. Patients might feel a sensation in their chest one minute and dizziness in their head the next. These symptoms are rarely constant; they tend to come in episodes or attacks, leaving the person feeling perfectly fine in between. This intermittent nature can make it difficult for patients to describe what is happening to them.
Understanding the risk factors is also a bit different in this field. While diet and exercise matter, the risks here also include things like emotional trauma, brain injuries, and genetic tendencies toward fainting. The nervous system is delicate, and when it is out of balance, the body’s symptoms signal that the control center is losing its grip on the cardiovascular system. Recognizing these signs early prevents falls, accidents, and long-term damage to both the heart and the brain.
Fainting, medically known as syncope, is the hallmark symptom of neurocardiology. It is terrifying for patients and families because it happens so suddenly. One moment the person is standing or talking, and the next they are on the floor. This happens because the brain detects a sudden drop in blood flow and “shuts down” the system to force the body into a horizontal position, which makes it easier for blood to get back to the head.
This is the most common type of fainting. It is caused by an overreaction to the vagus nerve. Specific triggers like seeing blood, extreme heat, standing for too long in a line, or severe pain cause the brain to slam on the brakes. The heart slows down drastically, and blood vessels in the legs widen. Blood pools in the feet, the brain is starved of oxygen, and the person passes out.
This form of dizziness happens specifically when changing position. When you stand up from a chair or bed, gravity pulls blood down to your legs. Normally, your nervous system instantly tightens your blood vessels to push that blood back up. In this condition, that reflex fails. The blood stays in the legs, and the blood pressure drops.
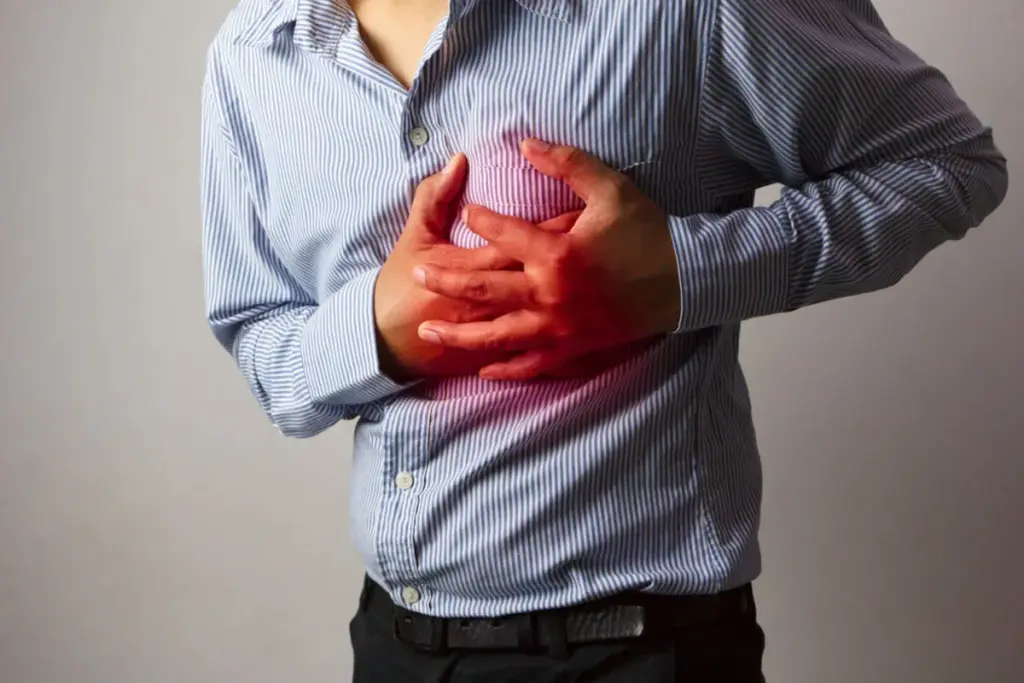
Patients frequently express sensations of their heart oscillating, skipping beats, or racing uncontrollably. In neurocardiology, the issue is often not with the heart muscle itself but rather with the nervous system. with the signals telling it when to beat. The autonomic nervous system acts like a thermostat for heart rate. If the thermostat is broken, the heart rate can fluctuate wildly without any physical exertion.
Postural Orthostatic Tachycardia Syndrome (POTS) is a prime example. In POTS, the heart races incredibly fast just because the person stands up. The nervous system fails to tighten the blood vessels, so the heart tries to compensate by beating faster and faster to maintain blood flow.

When the heart and brain are not in sync, thinking becomes difficult. Patients describe this as “brain fog.” It is akin to attempting to think through a dense fog. They might struggle to recall words, forget why they walked into a room, or have trouble concentrating on a book or a conversation. This issue is a direct result of hypoperfusion, which simply means low blood flow to the brain.
Even if the person doesn’t faint, blood flow to the brain may be slightly low. The brain survives, but the person does not thrive. It powers down non-essential functions to conserve energy. This condition can lead to chronic fatigue and mental lethargy that is often mistaken for depression or laziness.
Because the heart can throw clots to the brain, neurocardiology also covers the symptoms of stroke and transient ischemic attacks (TIAs, or mini-strokes). These are medical emergencies. If a heart rhythm disorder like atrial fibrillation allows a clot to form, that clot can travel to the brain and block a vessel.
The symptoms appear suddenly. A person might lose the ability to speak clearly, one side of their face might droop, or they might lose strength in an arm or leg. Even if these symptoms last only a few minutes and then disappear (a TIA), they are a massive warning sign. They indicate that the heart is creating clots that are reaching the brain, and a major stroke could be imminent.

The link between emotional health and heart health is a major focus of this field. We now know that chronic negative emotions are a potent risk factor for heart disease. Depression, anxiety, and chronic stress keep the body in a permanent state of “fight or flight.” This floods the system with cortisol and adrenaline.
Over time, this chemical bath damages the lining of the blood vessels and makes the heart more prone to rhythm problems. People with high levels of hostility or anger are also at greater risk. Conversely, people who have strong social support and positive coping mechanisms tend to have better outcomes. The brain’s emotional state dictates the chemical environment the heart lives in.
Pre-existing neurological conditions can put the heart at risk. Patients with epilepsy, for example, have a specific risk known as SUDEP (Sudden Unexpected Death in Epilepsy), which is believed to be caused by a heart rhythm collapse during or after a seizure. The electrical storm in the brain disrupts the heart’s electrical stability.
Similarly, patients with Parkinson’s disease or multiple system atrophy often suffer from severe autonomic failure. Their nerves degenerate, leading to dangerous drops in blood pressure and heart rate variability. Understanding these neurological roots helps doctors predict and manage heart risks in these specific populations.

Send us all your questions or requests, and our expert team will assist you.
POTS stands for Postural Orthostatic Tachycardia Syndrome. It is a condition where your heart rate spikes significantly (usually by 30 beats or more) when you stand up, causing dizziness and fatigue. It is a disorder of the autonomic nervous system.
Yes. Dehydration reduces your blood volume. This process makes it harder for your body to maintain blood pressure, leading to dizziness, fainting, and a racing heart, especially in people with sensitive nervous systems.
This is usually a temporary drop in blood pressure called orthostatic hypotension. Your blood pools in your legs, and it takes a few seconds for your nervous system to clamp down the vessels and push blood back to your brain.
Many people experience a “prodrome,” or warning phase. This can include feeling hot or clammy, nausea, yawning, tunnel vision, or sounds becoming muffled. Recognizing these signs can give you time to sit down and prevent a faint.
Usually not. If the brain fog is caused by poor blood flow or heart rhythm issues, treating the underlying heart or autonomic condition typically restores mental clarity and energy levels.

 Cardiology
Cardiology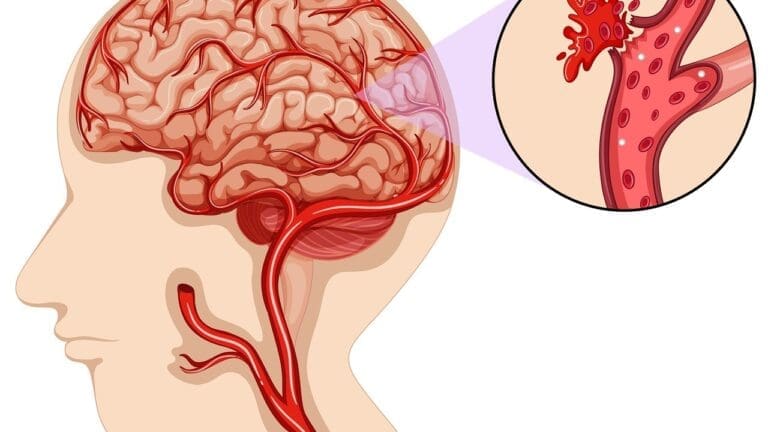 Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology Cardiology
Cardiology
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)