Cardiology is the medical specialty focused on the heart and the cardiovascular system. It involves the diagnosis, treatment, and prevention of conditions affecting the heart and blood vessels. These conditions include coronary artery disease, heart failure, arrhythmias (irregular heartbeats), and valve disorders. The field covers a broad spectrum, from congenital heart defects present at birth to acquired conditions like heart attacks.
Send us all your questions or requests, and our expert team will assist you.
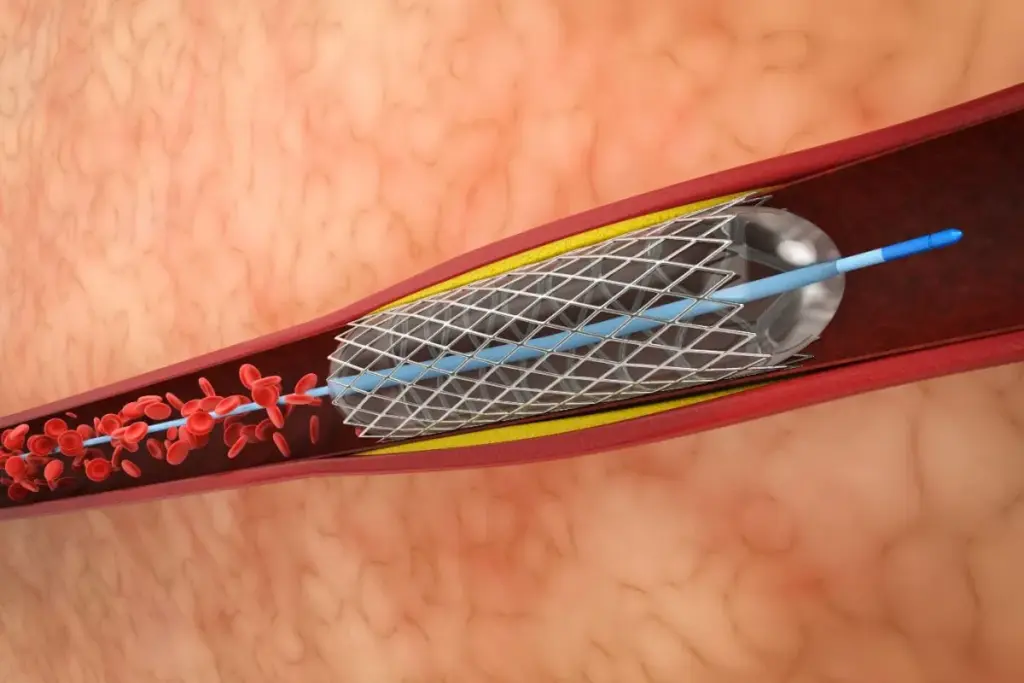
Percutaneous closure represents a significant leap forward in the field of heart medicine, specifically within the realm of structural heart repair. For decades, if a person was born with a hole in their heart or developed a leak around a heart valve, the only solution was open-heart surgery. This meant a large incision in the chest, stopping the heart, using a bypass machine, and a recovery period that could last for months. Percutaneous closure has changed this landscape entirely. It allows doctors to repair these internal defects without ever making a large cut or opening the chest. Instead, they use the body’s own blood vessels as a highway to reach the heart.
The term “percutaneous” literally translates to “through the skin.” This describes the method of entry. A small puncture, usually no bigger than the tip of a pencil, is made in a blood vessel, typically in the upper leg or groin area. Through this tiny entry point, specialized tools are guided up to the heart to seal holes or leaks. The procedure is minimally invasive, which means it causes much less trauma to the body than traditional surgery. Patients who undergo these procedures often experience dramatically shorter hospital stays, less pain, and a quicker return to their normal daily lives. It is a technique that combines precision engineering with advanced medical imaging to fix the heart from the inside out.
The history of repairing heart defects is a story of moving from major surgeries to gentle interventions. In the past, a hole in the heart was a daunting diagnosis that required a team of surgeons and a long stay in the intensive care unit. Today, thanks to percutaneous techniques, it is often an overnight procedure.
This shift began with the development of catheters, which are long, thin, flexible tubes. Doctors found that these tubes could take heart pictures and deliver treatments. Over the last thirty years, engineers and doctors have collaborated to create sophisticated devices that can be folded up to fit inside a catheter and then unfolded once they reach the heart. These devices function similarly to patches or plugs. The materials used are advanced medical-grade metals and fabrics that the body accepts readily. Once implanted, the body’s own tissue grows over the device, making it a permanent part of the heart wall.
The devices used to close these holes are marvels of medical engineering. While there are different brands and designs, most share a similar basic structure. They are typically made of a metal mesh framework. The metal used is often Nitinol, a mix of nickel and titanium. Nitinol has a unique property called “shape memory.” This means the device can be squeezed very thin to fit inside a catheter, but when it is pushed out, it instantly springs back to its original, expanded shape.
Inside the metal mesh, there is usually a fabric material, often polyester. This fabric acts as a barrier to stop blood flow immediately. More importantly, the fabric provides a scaffold for the body’s own cells. Over the weeks and months following the procedure, the heart’s lining grows over the mesh and fabric. Eventually, the device is completely covered by biological tissue.
To understand percutaneous closure, it is helpful to understand what is being closed. The human heart has four chambers: two upper chambers called atria and two lower chambers called ventricles. In a perfectly formed heart, walls separate the left side from the right side, ensuring that oxygen-rich blood does not mix with oxygen-poor blood. However, sometimes these walls do not form correctly, or they do not close after birth as they should.
An atrial septal defect, or ASD, is a hole in the wall between the two upper chambers of the heart. You can think of it as a missing piece of the wall. Because the pressure is higher on the left side of the heart, blood flows through this hole into the right side. This opening causes the right side of the heart and the lungs to work harder than they should. Over many years, this extra blood flow can damage the blood vessels in the lungs and cause the right side of the heart to enlarge. Percutaneous closure uses a device that looks like a double-sided umbrella to sandwich the hole shut.
A patent foramen ovale, or PFO, is slightly different from an ASD. Every baby has a PFO before they are born; it is a small flap-like opening that allows blood to bypass the lungs while the baby is in the womb. Normally, this flap fuses shut shortly after birth. However, in about one out of every four people, this flap stays open. It is not a missing piece of tissue but rather a door that failed to lock. Usually, it stays closed, but sometimes it can pop open when you cough or strain. Percutaneous closure is used to seal this flap permanently, usually to prevent blood clots from crossing over and causing a stroke.
The devices used to close these holes are marvels of medical engineering. While there are different brands and designs, most share a similar basic structure. They are typically made of a metal mesh framework. The metal used is often Nitinol, a mix of nickel and titanium. Nitinol has a unique property called “shape memory.” This means the device can be squeezed very thin to fit inside a catheter, but when it is pushed out, it instantly springs back to its original, expanded shape.
Inside the metal mesh, there is usually a fabric material, often polyester. This fabric acts as a barrier to stop blood flow immediately. More importantly, the fabric provides a scaffold for the body’s own cells. Over the weeks and months following the procedure, the heart’s lining grows over the mesh and fabric. Eventually, the device is completely covered by biological tissue.
The doctor who performs percutaneous closure is called an interventional cardiologist. This is a heart specialist who has undergone extra years of training specifically in catheter-based procedures. They are heart specialists who use wires and catheters instead of scalpels or saws. Instead, their skills lie in manipulating wires and catheters from outside the body, guiding them deep inside the heart using X-ray screens and ultrasound monitors.
These doctors must have incredible hand-eye coordination. They watch a screen while their hands move the tools at the patient’s hip. They must also be experts in interpreting medical imaging. During the procedure, they rely on echocardiograms (ultrasounds of the heart) to see the exact edges of the defect. They work in a specialized room called a cardiac catheterization lab, or “cath lab,” which is filled with high-tech imaging equipment. Their goal is to navigate the device to the perfect spot, deploy it safely, and ensure there are no leaks before finishing the procedure.
Patients often ask why anyone would choose open surgery if percutaneous closure is an option. The reality is that percutaneous closure is the preferred choice whenever possible, but it is not always suitable for every patient. The anatomy of the defect plays a significant role. For example, if a hole is huge or located very close to other important structures like valves or veins, a catheter device might not fit safely. In those cases, a surgeon’s ability to sew a patch directly onto the heart is necessary.
However, for the majority of standard defects like PFOs and central ASDs, percutaneous closure offers distinct advantages. There is no large scar on the chest. There is no need for the heart-lung bypass machine, which can sometimes cause temporary fogginess or memory issues. The pain is minimal, usually just some soreness at the top of the leg. Most significantly, the recovery time is measured in days rather than months. A patient might be back to desk work in a week, whereas surgery might require six to eight weeks of rest.
One of the most reassuring aspects of percutaneous closure is its safety record. These procedures have been performed for decades, and the data shows they are highly effective and carry low risk. Complications are rare but can include bleeding at the leg insertion site or the device moving out of position before it However, specialized steps are taken to minimize these risks.
Once the device is in place and the tissue has healed over it, the repair is considered permanent. The device does not need to be replaced. It does not wear out like a battery. It simply becomes a part of the heart’s dividing wall. Long-term studies indicate that patients who undergo these closures see a resolution of their symptoms and a significantly reduced risk of complications like stroke. For parents of children with defects, or adults discovering them later in life, a closure offers a lifelong cure without the lifelong reminder of a surgical scar.

Send us all your questions or requests, and our expert team will assist you.
An ASD is a hole where heart tissue is missing, allowing blood to flow freely between chambers. A PFO is a flap that failed to seal shut after birth, acting like a trapdoor that usually stays closed but can open under pressure.
Yes, the device is typically made of Nitinol, a medical-grade alloy of nickel and titanium. It is non-corrosive and safe. If you have a severe nickel allergy, you should discuss the matter with your doctor, as alternative options may be considered.
No, you will not feel the device. The heart has no nerve endings that sense touch inside the chambers. Once it is placed, you will not be aware of its presence.
It is generally not classified as major surgery because there is no large incision and the heart is not stopped. It is considered a minimally invasive interventional procedure.
Device dislodgement is extremely rare. Doctors measure the defect precisely to choose the correct size, and the device is designed to clamp securely onto the tissue. Once tissue grows over it, it is permanently locked in place.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)