Cervical cancer starts in the cervix with abnormal cell growth. These cells can spread to other parts of the body. Cervical cancer cells themselves do not typically regress on their own. But, their early stages can.
These early stages are called cervical intraepithelial neoplasia (CIN). They can go back to normal by themselves. Recent research has highlighted the potential for CIN to regress, giving us new ways to care for patients and prevent the disease.
Knowing about CIN stages is key to managing and treating the disease. At places like Liv Hospital, we focus on top-notch care for patients from around the world.
Key Takeaways
- Cervical cancer cells do not typically go away on their own.
- Precancerous stages (CIN) can spontaneously regress.
- Understanding CIN stages is critical for effective management.
- Recent research offers new insights into patient care and prevention.
- Innovative healthcare centers provide world-class care for international patients.
Understanding Cervical Cancer Development
The journey to cervical cancer often begins with an HPV infection. This can cause various cervical abnormalities. Almost all cervical cancer cases (99%) are linked to HPV, with types 16 and 18 causing about 70% of cases worldwide.
The progression from HPV infection to cancer
HPV infection is common, but not all lead to cancer. The virus can cause changes in the cervix. If not treated, these changes can progress to cancer in several stages.
- CIN1 (Cervical Intraepithelial Neoplasia grade 1): Mild dysplasia
- CIN2 (Cervical Intraepithelial Neoplasia grade 2): Moderate dysplasia
- CIN3 (Cervical Intraepithelial Neoplasia grade 3): Severe dysplasia or carcinoma in situ
Different stages of cervical abnormalities
Cervical abnormalities range from mild to severe. Low-grade lesions (CIN1) often go away on their own. But, high-grade precancerous changes (CIN2/3) have varying regression rates. Knowing these stages is key for proper management.
Distinguishing between precancerous changes and cancer
Precancerous changes are abnormal cell growth that could turn into cancer. These are often found through Pap smear and HPV testing. Distinguishing between precancerous lesions and actual cancer is critical for determining the appropriate treatment approach. For example, an epithelial cell abnormality on a Pap smear may need further evaluation through colposcopy.
We stress the need to understand cervical abnormality stages for timely care. Recognizing the progression from HPV to cancer allows healthcare providers to offer targeted interventions.
CIN1: The Most Common Low-Grade Cervical Change
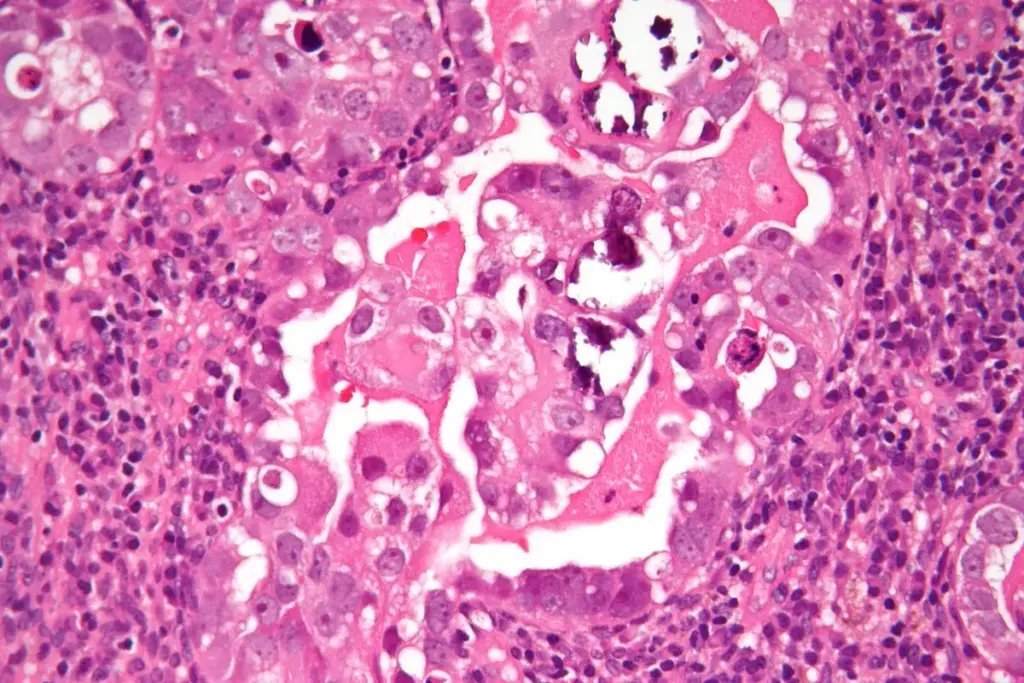
Low-grade cervical changes, known as CIN1, are often found during routine Pap smear tests. These changes are the first sign of abnormal cell growth in the cervix. They are considered precancerous.
Classification of Cervical Intraepithelial Neoplasia
Cervical Intraepithelial Neoplasia (CIN) is divided into three grades. CIN1 is the least severe and is often seen as a low-grade lesion. The World Health Organization uses a system to classify these lesions. This helps doctors decide how to treat them.
Distinguishing CIN1 from Normal Cells
CIN1 has mildly abnormal cells that differ from normal cervical cells. During a cervix biopsy, pathologists look at the cells to see if there’s CIN. It’s important to tell CIN1 apart from more serious forms or normal cells to decide if treatment is needed.
Common Symptoms and Concerns
Most women with CIN1 don’t have symptoms. The abnormal cells are usually found during a routine Pap smear or HPV testing. Women might worry about the risk of more serious CIN or cancer. But, most low-grade lesions (CIN1) go away on their own, so treatment isn’t always needed right away.
It’s important to understand CIN1 and its effects on cervical health. Regular screenings and check-ups with healthcare providers are key. They help keep an eye on any abnormal cell changes and guide the best treatment plan.
Staging
Knowing the stage of cervical cancer is key to finding the right treatment. Staging lets doctors see how far the disease has spread. This helps them plan the best treatment.
FIGO Staging System
The International Federation of Gynecology and Obstetrics (FIGO) uses a well-known staging system for cervical cancer. This system relies on clinical exams, not surgery. It gives a clear picture of the disease without needing surgery.
The FIGO system uses many ways to figure out the cancer stage. It includes imaging and looking at tissue samples. This makes it possible to accurately stage the disease, even if surgery isn’t an option.
Clinical Staging versus Pathological Staging
Clinical staging looks at the disease based on exams and tests like imaging. It’s helpful when surgery isn’t the first step.
Pathological staging, on the other hand, looks at tissue samples from surgery. It gives more detailed info about the disease. But, clinical staging is key for first assessments and treatment plans.
Accurate staging is critical for knowing the patient’s outlook and choosing the right treatment. By understanding the disease stage, doctors can create a treatment plan that meets each patient’s needs.
Spontaneous Regression of Precancerous Cells
The body can fight off CIN1 on its own. This shows how strong our natural defenses are. It also means not all precancerous cells turn into cancer.
How Often CIN1 Resolves Without Treatment
Many CIN1 cases get better by themselves without treatment. Research from the National Center for Biotechnology Information shows this. It points to the immune system’s key role in healing these lesions.
Studies show different rates of CIN1 regression. But a big part of cases get better naturally. This helps us understand CIN1 better and decide on treatment.
|
Study |
Regression Rate |
Follow-Up Period |
|---|---|---|
|
Study A |
60% |
12 months |
|
Study B |
70% |
24 months |
|
Study C |
65% |
18 months |
Timeframe for Possible Regression
How long it takes for CIN1 to get better varies. It depends on the immune system and overall health.
The Role of the Immune System in Clearance
The immune system is key in fighting off HPV and precancerous cells. A strong immune response can make CIN1 go away. This shows how important health and immune function are in stopping cervical problems.
Knowing how the immune system helps clear precancerous cells is important. It helps us find ways to manage CIN1 and lower cervical cancer risk.
High-Grade Lesions: CIN2 and CIN3 Progression Rates
It’s important to know how fast CIN2 and CIN3 lesions can turn into cervical cancer. These serious problems can lead to cancer if not treated right away.
CIN2 Regression Statistics
CIN2 lesions, or high-grade cervical dysplasia, can change in different ways. Some studies say a big part of CIN2 lesions can go away on their own. But, how many is not clear.
- Regression rates: Research shows that 20% to 50% of CIN2 lesions might go away without treatment.
- Persistence and progression: But, some CIN2 lesions stay the same or get worse, turning into CIN3 or cancer.
CIN3 Regression Possibilities
CIN3 is a more serious stage of cervical dysplasia and has a higher chance of turning into cancer. But, it’s not impossible for it to go away.
“The chance of CIN3 going away is lower than CIN2, but it’s not zero. Keeping a close eye on it and managing it right is key.”
Risk of Progression to Invasive Cancer
The worry is that CIN2 and CIN3 lesions could turn into invasive cervical cancer. This risk depends on several things like the patient’s immune system, the type of HPV, and other health issues.
- HPV type: Some high-risk HPV types are more likely to cause problems.
- Immune system function: People with weak immune systems are more likely for the lesions to get worse.
Acting fast and keeping an eye on these lesions is very important. Knowing how fast they can change and what affects this change helps doctors give better care. This can lower the chance of cervical cancer.
Factors Affecting Spontaneous Regression<SEP-1176_image_3>
Several factors can influence whether precancerous lesions will go away on their own. Knowing these can help in treating cervical issues more effectively.
Age and Immune System Function
A woman’s age and immune health are key in whether lesions will go away. Younger women often have a better chance because their immune system is stronger. Research shows that the immune system can fight off HPV infections better in the young, helping lesions to heal.
HPV Type and Viral Load
The type of HPV and how much virus is present are important. Some high-risk HPV types are less likely to go away. Also, a high viral load means a more serious infection, making spontaneous regression less likely.
Time Between Biopsy and Treatment
The time between getting a biopsy and treatment can affect regression. Sometimes, lesions can heal before treatment is needed. But, this time should be watched closely by doctors to catch any changes early.
Lifestyle Factors That Influence Regression
Lifestyle choices can also impact whether lesions will go away. These include:
- Dietary habits: Eating lots of fruits, vegetables, and antioxidants can boost the immune system.
- Smoking status: Quitting smoking can improve health and help with regression.
- Stress levels: High stress can weaken the immune system, making regression harder.
By changing these lifestyle factors, people may help their body heal precancerous lesions naturally.
Detection and Diagnosis of Cervical Abnormalities
Cervical abnormalities are found through tests like Pap smear, HPV testing, colposcopy, and biopsy. These tests help spot abnormal cell changes in the cervix. If not treated, these changes can turn into cancer.
Pap Smear and HPV Testing Protocols
Pap smear and HPV testing are key for finding cervical abnormalities. A Pap smear takes cells from the cervix to check for changes. HPV testing looks for high-risk HPV types that can lead to cervical cancer.
Women should get regular Pap smears and HPV tests. How often depends on age, medical history, and past test results.
|
Test |
Purpose |
Frequency |
|---|---|---|
|
Pap Smear |
Detect abnormal cell changes |
Every 3 years for women aged 21-29 |
|
HPV Testing |
Identify high-risk HPV types |
Every 5 years for women aged 30-65 |
Colposcopy and Cervical Biopsy Procedures
If a Pap smear or HPV test shows abnormal cells, a colposcopy might be done. This lets doctors closely look at the cervix for any issues. A colposcope is used to see the cells up close.
A biopsy might be taken during a colposcopy if something looks off. The sample is then checked under a microscope. This helps figure out the severity of the abnormal cell changes.
Understanding Epithelial Cell Abnormalities in Test Results
Epithelial cell abnormalities mean changes in the cells lining the cervix. These changes can be mild or severe. It’s important to understand Pap smear and biopsy results to know what to do next.
When to Seek a Second Opinion
If test results show abnormal cells, it’s key to understand what it means. Talk to your doctor about what it means and your options. Sometimes, getting a second opinion can help confirm the diagnosis and explore other treatment paths.
We suggest patients take an active role in their health. If you have questions about your diagnosis or treatment, don’t hesitate to ask for more information.
Treatment Approaches for Different CIN Grades
The grade of CIN determines the treatment plan. CIN1 is often treated conservatively, while higher grades need more aggressive methods. We will look at the different treatments for each CIN grade, ensuring a full understanding of the options.
Watchful Waiting for CIN1
Women with CIN1 usually get watchful waiting. This is because CIN1 is a low-grade lesion that often goes away on its own. Regular follow-up is key to watch for any changes to a higher grade.
Most CIN1 cases clear up without treatment. So, immediate action is not usually needed unless the lesion doesn’t go away or gets worse.
LEEP and Other Procedures for High-Grade Lesions
High-grade lesions like CIN2 and CIN3 need more action. Loop Electrosurgical Excision Procedure (LEEP) is a common treatment. It removes the abnormal tissue with a heated wire loop.
Other treatments include:
- Cold knife cone biopsy
- Laser ablation
- Cryotherapy
The right procedure depends on the lesion’s size, location, and the patient’s health and wishes.
Follow-up Protocols After Treatment
After treatment, follow-up protocols are vital to check if the abnormal cells come back. This usually means regular Pap smears and HPV tests.
|
Follow-up Protocol |
Timeframe |
|---|---|
|
Pap smear and HPV testing |
6-12 months after treatment |
|
Repeat Pap smear |
1-2 years after initial follow-up |
Modern Multidisciplinary Management Approaches
Today, CIN management is a team effort. Gynecologists, pathologists, and sometimes oncologists work together. This ensures patients get care that fits their needs.
This team approach helps improve CIN treatment outcomes. It reduces the risk of cervical cancer while avoiding unnecessary treatments.
Prevention Strategies and Risk Reduction
To lower cervical cancer risk, we need to know and use effective prevention methods. By focusing on proven ways, we can greatly reduce this disease.
HPV Vaccination Recommendations
HPV vaccination is key in stopping cervical cancer. Both boys and girls should get the HPV vaccine between 11 and 12. It can start as early as 9.
For those who missed it, catch-up vaccination is available. Women can get it up to age 26, and men up to 21. This vaccine protects against the most common cancer-causing HPV types, lowering cervical cancer risk.
Regular Screening Importance
Regular screening is vital for catching and treating precancerous lesions early. Women should start cervical cancer screening at 21.
Women 21 to 29 should get a Pap test every three years if results are normal. Women 30 to 65 should get co-testing (Pap test and HPV test) every five years or a Pap test alone every three years.
Lifestyle Modifications to Reduce Risk
Lifestyle choices are key in preventing cervical cancer. We stress the importance of:
- Quitting smoking, as it is a known risk factor for cervical cancer.
- Limiting sexual partners and practicing safe sex to reduce the risk of HPV infection.
- Maintaining a healthy diet rich in fruits, vegetables, and whole grains.
Addressing Common Misconceptions
There are many misconceptions about cervical cancer that can harm prevention efforts. We clear up that:
- The HPV vaccine does not protect against all types of HPV, but it covers the most common cancer-causing types.
- Cervical cancer screening is not just for sexually active women; all women in the recommended age groups should be screened.
- A healthy lifestyle can reduce the risk but does not eliminate it entirely.
Conclusion: The Importance of Monitoring and Timely Intervention
Monitoring and timely intervention are key in managing precancerous lesions like CIN1, CIN2, and CIN3. This helps prevent cervical cancer. We’ve talked about the different stages of cervical abnormalities and why awareness and timely treatment are important.
Understanding how low-grade lesions like CIN1 can heal on their own is important. But for high-grade lesions, acting fast is critical to stop cancer from developing. Regular check-ups and follow-up plans help catch and treat problems early.
A report shows that being active is good for health. It points out the need for action to tackle health issues. The same goes for cervical cancer, where watching and acting quickly can make a big difference.
By focusing on monitoring and timely action, we can better manage precancerous lesions. This reduces the chance of cervical cancer. It’s a proactive way to care for those at risk.
FAQ
Can precancerous cells on the cervix go away on their own?
Yes, some precancerous cells can go away by themselves. This is more likely for CIN1. But, CIN2 and CIN3 might need treatment because they are more serious.
What are the chances of cervical cancer after LEEP?
LEEP greatly lowers the risk of cervical cancer. It removes bad cells. But, you should keep getting checked regularly because the risk isn’t completely gone.
What does it mean to have HPV on a colposcopy?
HPV on a colposcopy means you have the virus. It’s a common cause of cervical problems. The colposcopy checks for disease, and HPV might mean you need more tests or treatment.
What are abnormal cells on a Pap smear?
Abnormal cells on a Pap smear are not normal. They can be mild or serious. They might be linked to HPV.
What is the difference between CIN1, CIN2, and CIN3?
CIN1, CIN2, and CIN3 are stages of cervical problems. CIN1 is mild, CIN2 is moderate, and CIN3 is severe. The higher the number, the bigger the risk of cancer.
What is a cervix biopsy?
A cervix biopsy takes tissue from the cervix for a microscope check. It helps find or rule out abnormal cells or cancer.
What does epithelial cell abnormality mean?
Epithelial cell abnormality means the cervix cells are not normal. It can be due to HPV and might show precancer or cancer.
Do I need a colposcopy if I have HPV?
If you have HPV, you might need a colposcopy. It depends on the HPV type, your Pap smear, and health history. A doctor will decide based on these factors.
What is the FIGO staging system for cervical cancer?
The FIGO staging system classifies cervical cancer. It shows how far the disease has spread. It helps plan treatment and predict outcomes.
How often does CIN1 resolve without treatment?
Many CIN1 cases clear up by themselves. This is often because of the immune system fighting off HPV.
What factors influence the spontaneous regression of precancerous lesions?
Several things can affect if precancerous lesions go away on their own. These include age, immune health, HPV type, and viral load. Lifestyle and time to treatment also matter.
References
- National Center for Biotechnology Information (NCBI): https://pmc.ncbi.nlm.nih.gov/articles/PMC9578209/
- Karger Publishers: https://karger.com/goi/article/84/6/562/153964/Spontaneous-Regression-of-Cervical-Intraepithelial
- National Center for Biotechnology Information (NCBI): https://pmc.ncbi.nlm.nih.gov/articles/PMC3132609/
- National Center for Biotechnology Information (NCBI): https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6323170/
- National Center for Biotechnology Information (NCBI): https://www.ncbi.nlm.nih.gov/books/NBK223216/
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC4082862/



































