Autoimmune hepatitis is a chronic condition where the immune system attacks the liver. Learn about its definition, types (Type 1 and Type 2), and importance.
Send us all your questions or requests, and our expert team will assist you.
Autoimmune hepatitis is a chronic liver condition in which the body’s immune system mistakenly attacks its own liver cells, causing inflammation and potential liver damage. Early recognition and proper management are essential to prevent complications such as cirrhosis and liver failure.

Autoimmune hepatitis is a chronic liver disease in which the body’s immune system mistakenly attacks its own liver cells. Normally, the immune system serves as a protective mechanism, defending the body against infections caused by viruses, bacteria, or other harmful agents. However, in autoimmune hepatitis, this system malfunctions and treats liver cells, called hepatocytes, as foreign invaders. This misguided attack leads to inflammation, cell damage, and impaired liver function.
Literally, it translates to “self-immune liver inflammation.” If left untreated, the ongoing immune attack can result in scarring of the liver (cirrhosis), which may eventually progress to liver failure.

Autoimmune hepatitis is more than just a liver condition; it is a systemic autoimmune disorder with potential impacts beyond the liver. Understanding its scope is essential for timely diagnosis and effective management.
The liver plays a vital role in the body’s overall health. Autoimmune hepatitis affects several critical liver functions:

Because autoimmune hepatitis is an autoimmune disorder, it can coexist with other autoimmune diseases, such as:

It is crucial to differentiate autoimmune hepatitis from other liver diseases to ensure accurate diagnosis and appropriate treatment.
Correct differentiation is essential because treatment strategies differ significantly between these conditions.
Doctors classify autoimmune hepatitis into two primary types based on specific antibodies found in the blood. Identifying the type helps guide treatment decisions and predict disease progression.
Type 1 is the most common form of autoimmune hepatitis. It can occur at any age but is most frequently diagnosed in adults. It is associated with Anti-Smooth Muscle Antibodies (ASMA) and may present with mild or chronic liver inflammation. In some cases, Type 1 progresses slowly and may remain asymptomatic for years, making routine liver function tests crucial.
Type 2 is less common and typically affects children and young adults. It is often more severe than Type 1 and is associated with Liver Kidney Microsomal type 1 (LKM-1) antibodies. Type 2 can progress rapidly if untreated, sometimes leading to early liver damage, cirrhosis, or liver failure.

Managing autoimmune hepatitis often requires a multidisciplinary approach due to the complexity of the disease.
Hepatologists specialize in liver diseases, including autoimmune hepatitis. They oversee diagnosis, treatment planning, and long-term monitoring to prevent disease progression.
In severe or end-stage cases, where liver function is critically impaired, transplant specialists become essential. Liver transplantation may be necessary to replace the damaged organ and restore normal liver function.
Since autoimmune hepatitis is an immune-mediated condition, immunologists can help manage immune system suppression, adjusting medications to minimize side effects while controlling inflammation.

Managing autoimmune hepatitis effectively is critical because the liver is resilient but irreplaceable. Chronic inflammation gradually replaces healthy liver tissue with scar tissue (fibrosis), ultimately leading to cirrhosis.
Early recognition allows prompt treatment, which can halt disease progression and prevent irreversible damage. Patients with subtle or no symptoms may only be diagnosed through routine liver function tests or antibody screening.
Treatment typically involves immunosuppressive medications, such as corticosteroids and azathioprine. Proper treatment can:
Symptoms vary widely and may develop slowly, sometimes making early detection challenging. Common signs include:
Because these symptoms overlap with other liver or autoimmune conditions, specialized testing is essential for accurate diagnosis.
Diagnosing autoimmune hepatitis involves multiple steps:
Early diagnosis allows timely intervention, preventing long-term liver damage.

Send us all your questions or requests, and our expert team will assist you.
Autoimmune hepatitis is a condition where the immune system attacks the liver. A specialist, usually a hepatologist or gastroenterologist, diagnoses it using blood tests and biopsies, then prescribes immunosuppressive medication to protect liver function.
Treatment addresses liver inflammation and prevents complications such as fibrosis, cirrhosis, and liver failure caused by ongoing immune attacks.
The two main types are Type 1 and Type 2. Type 1 primarily affects adults, while Type 2 is rarer, more severe, and commonly affects children.
Consult a specialist if you experience persistent fatigue, jaundice, abdominal pain, or joint pain, or if routine blood tests indicate abnormal liver enzymes.
Autoimmune hepatitis is immune-mediated and non-contagious, whereas viral hepatitis is caused by infection and can spread to others.


Seeing white patches or spots on your tongue can worry you. These changes can be from simple issues or serious health problems. The Medical organization

Every second matters when it comes to aheart attack. At Liv Hospital, we’re dedicated to top-notch healthcare. We offer full support and guidance for international
Heart disease is a major killer worldwide, causing millions of deaths each year. Early detection is key to prevent and manage heart conditions. A cardiac
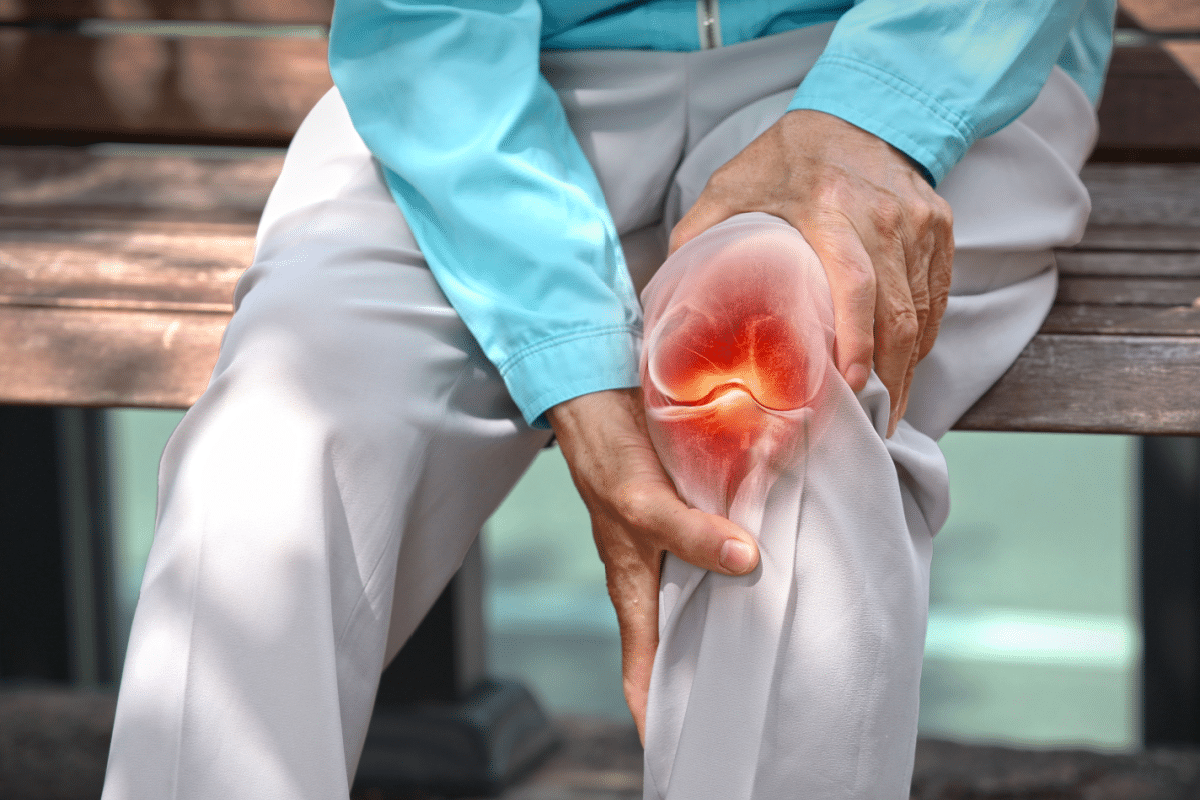
Osteoarthritis affects about 528 million people worldwide. It causes joint pain, stiffness, and swelling. But, effective management is possible with the right care and personalized
Posterior oropharyngeal erythema is a common condition. It causes redness and inflammation in the back of the throat. This affects millions of people worldwide, making
Autoimmune Polyendocrinopathy-Candidiasis-Ectodermal Dystrophy (APECED) is a rare genetic disorder. It is caused by mutations in the AIRE gene. APECED syndrome is known for its three main symptoms:

Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)