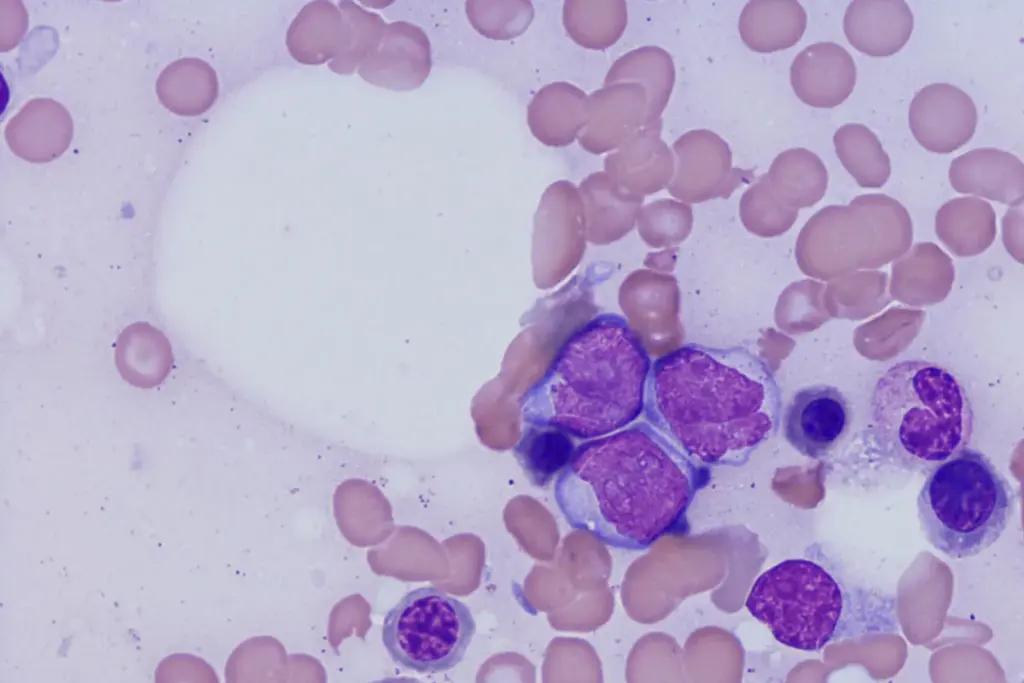
Acute Myeloid Leukemia (AML) is a tough blood cancer. It can come back even after tough treatments.
At our hospital, we focus on caring for our patients. We use the latest medical knowledge to fight AML relapse and help patients live longer.
Learning about what makes AML come back is key. Hearing from the longest AML survivors helps us find better ways to help patients. This way, we can help more people beat leukemia.
Key Takeaways
- AML is a challenging blood cancer with a high risk of recurrence.
- Understanding the factors that influence AML relapse is key to better patient care.
- We at our hospital are dedicated to caring for our patients and fighting AML relapse.
- The stories of the longest AML survivors give us insights into beating leukemia.
- With new treatments and team care, we can help more people survive AML.
Understanding Acute Myeloid Leukemia (AML)
Understanding Acute Myeloid Leukemia (AML) is key for those facing this tough diagnosis. AML is a blood cancer where abnormal white blood cells grow fast. These cells fill the bone marrow and stop it from making normal blood cells.
What is AML and How Does it Develop?
AML starts when the bone marrow makes bad myeloid cells that don’t grow right. These cells build up and take over the bone marrow. This makes it hard for it to make healthy blood cells. Knowing how AML develops helps doctors diagnose and treat it better, as the SEER Cancer Statistics Review shows.
Common Symptoms and Diagnosis
AML symptoms include feeling very tired, losing weight, and getting sick often. Doctors use blood tests and bone marrow biopsies to find abnormal cells. Finding AML early is important for good treatment.
Initial Treatment Approaches
First, AML treatment often uses chemotherapy to get the leukemia cells to die. This lets the bone marrow make healthy cells again. Doctors make treatment plans based on the patient’s health and AML type.
AML Relapse Rates: The Statistical Reality

It’s key for patients and doctors to grasp AML relapse rates. AML relapse is a big hurdle in treating Acute Myeloid Leukemia. It affects how well patients do and how long they live.
Overall Relapse Frequency
About 31% of AML patients face relapse after their first treatment. This shows why we must keep watching patients closely and have good plans for after treatment.
“The high relapse rate in AML patients shows how complex the disease is,” experts say. “We need new ways to treat it.”
Timeline of Relapse After Initial Treatment
When AML relapse happens varies from person to person. Most relapses are in the first year after treatment. Knowing this helps in planning follow-up care.
- Most relapses happen within the first 12 months.
- The risk of relapse decreases significantly after 2 years.
- Ongoing monitoring is key for catching relapse early.
Median Survival of 5.3 Months After Relapse
After AML relapse, patients usually live about 5.3 months. This shows how urgent and effective treatment at relapse is. Survival depends on how long the first remission lasted, the patient’s health, and how well they respond to treatment.
One study found, “The outlook for AML patients who relapse is not good. We need better treatments to save them.”
AML relapse is a complex issue, influenced by many factors. By understanding these rates, we can work on bettering patient outcomes and survival chances.
The 5-Year Survival Landscape for AML Patients
Understanding the 5-year survival rate for AML patients is key. This rate shows how many patients live for five years after being diagnosed. It’s a vital metric for knowing the disease’s impact.
The 5-year survival rate for AML patients is about 32.9%. This number gives a general idea of what to expect. But, each patient’s outcome can differ a lot.
Understanding the 32.9% Overall Survival Rate
The 32.9% survival rate is influenced by many things. Age, genetic makeup, and how well the first treatment works are important. Younger patients and those with certain genetic traits often do better.
This survival rate is a statistical average, not a prediction for one person. It helps give a general idea but should be seen in the context of each patient’s situation.
Factors That Influence 5-Year Survival
Many factors affect AML patients’ 5-year survival rates. These include:
- Age: Younger patients usually have better chances.
- Genetic abnormalities: Some genetic mutations can greatly impact survival.
- Response to initial treatment: Those who achieve complete remission after treatment often do better in the long run.
- Overall health: Patients with fewer health issues and better overall health tend to fare better.
AML Life Expectancy Without Treatment
AML life expectancy without treatment varies a lot. It depends on how aggressive the disease is and the patient’s health. Without treatment, AML usually progresses quickly, and life expectancy is often just months.
It’s important for patients to talk to their healthcare provider about their prognosis and treatment options. This helps understand their specific situation and the benefits of different treatments.
Genetic Factors That Influence AML Recurrence
Understanding the genetic factors that lead to AML recurrence is key to better treatments. AML is a complex disease with myeloid blasts in the bone marrow and blood. It has a diverse genetic landscape, with many mutations affecting disease progression and treatment response.
Complex Genetic Abnormalities
Older patients often have complex genetic abnormalities in AML. These include chromosomal deletions, translocations, and mutations in important genes. Complex karyotype abnormalities are linked to a poorer prognosis and higher recurrence risk.
Some common complex genetic abnormalities in AML include:
- Deletions or mutations in tumor suppressor genes
- Translocations involving transcription factors
- Mutations in genes involved in DNA repair mechanisms
|
Genetic Abnormality |
Impact on AML |
Prognostic Implication |
|---|---|---|
|
Complex Karyotype |
Increased genomic instability |
Poor prognosis |
|
TP53 Mutations |
Disrupted cell cycle regulation |
High risk of recurrence |
|
FLT3-ITD Mutations |
Constitutive activation of FLT3 signaling |
Aggressive disease course |
The Role of TP53 Mutations
TP53 mutations are common in AML, often with complex karyotype abnormalities. The TP53 gene regulates the cell cycle, apoptosis, and genomic stability. Mutations in TP53 lead to dysfunctional p53 protein, impairing cell cycle arrest and chemotherapy resistance.
Research shows that TP53 mutations increase the risk of AML recurrence and lower survival rates. These mutations can also affect treatment effectiveness, making personalized treatments necessary.
Secondary AML and Its Genetic Profile
Secondary AML (sAML) develops from previous hematologic disorders or after chemotherapy. It has a unique genetic profile, often with mutations in TP53, SRSF2, and U2AF1.
The genetic profile of sAML offers insights into its pathogenesis and treatment targets. Understanding these genetic factors is essential for developing effective treatments and improving patient outcomes.
Clinical Factors Predicting AML Relapse
Several clinical factors play a big role in predicting AML relapse. We look at these factors to better understand their impact on patient care.
White Blood Cell Count at Diagnosis and Relapse
The white blood cell count at diagnosis is key in assessing relapse risk. High counts often mean a higher risk of relapse. Research shows that patients with high counts need closer monitoring and possibly more aggressive treatments.
Duration of First Remission
The length of the first remission is also very important. Patients with a shorter remission face a higher risk of relapse. This could mean the disease is more aggressive or not fully treated.
Age and Comorbidity Considerations
Age and comorbidities also affect relapse risk. Older patients and those with serious health issues may face a higher risk. This is because they might not tolerate intense treatments well. So, treatment plans need to be very individualized.
|
Clinical Factor |
Impact on AML Relapse |
|---|---|
|
High White Blood Cell Count at Diagnosis |
Increased risk of relapse |
|
Short Duration of First Remission |
Higher likelihood of relapse |
|
Advanced Age |
Increased risk due to decreased tolerance to therapy |
|
Presence of Comorbidities |
Higher risk due to therapy intolerance |
Understanding these clinical factors is key to creating effective treatments. By identifying high-risk patients, healthcare providers can take targeted steps. This could help reduce relapse risk and improve survival rates.
Standard Treatment Approaches for Preventing Relapse
AML treatment doesn’t stop after the first round. Consolidation therapy and maintenance are key to stopping relapse. After the first success, patients get more treatments to kill any leftover leukemia cells.
Consolidation Therapy Options
Consolidation therapy is a vital part of AML treatment. It aims to get rid of any leftover leukemia cells. High-dose chemotherapy and hematopoietic stem cell transplantation are the main choices. The right option depends on the patient’s health, AML type, and relapse risk.
- Chemotherapy: High-dose chemotherapy kills any leftover leukemia cells.
- Stem Cell Transplant: This replaces the patient’s bone marrow with healthy stem cells, from themselves or a donor.
Maintenance Strategies
Maintenance therapy is also key to preventing AML relapse. It involves giving lower doses of chemotherapy or other treatments for a long time. Targeted therapies and immunotherapies are being looked at as ways to keep remission.
- Targeted Therapy: Drugs that target specific genetic mutations or proteins in AML.
- Immunotherapy: Treatments that boost the body’s immune response against leukemia cells.
Monitoring for Early Signs of Recurrence
Regular checks are important for catching early signs of AML recurrence. This includes regular blood tests, bone marrow biopsies, and other tests as needed. Finding relapse early can lead to better treatment results.
- Regular Follow-Up: Patients get regular check-ups and tests.
- Diagnostic Tests: Blood tests and bone marrow biopsies help watch for relapse signs.
Stem Cell Transplant for AML: Impact on Recurrence
For many AML patients, a stem cell transplant is a key treatment. It can lower the chance of the disease coming back. This method replaces the patient’s sick bone marrow with healthy stem cells. These can come from the patient themselves or a donor.
Reducing Relapse Risk with BMT
Bone Marrow Transplant (BMT) helps lower the risk of AML coming back. It does this by:
- Eradicates cancerous cells: High-dose chemotherapy and/or radiation before the transplant kill off leukemia cells.
- Replaces diseased marrow: Healthy stem cells rebuild the bone marrow, aiming for a cancer-free state.
- Provides a graft-versus-leukemia effect: In allogeneic transplants, the donor’s immune cells fight any leftover cancer cells.
Factors Influencing Transplant Success
The success of a stem cell transplant for AML patients depends on several factors. These include:
- Donor compatibility: A well-matched donor greatly increases the transplant’s success.
- Patient’s overall health: Patients with fewer health issues tend to do better.
- AML status at transplant: Patients in remission at transplant time usually have better outcomes than those with active disease.
- Conditioning regimen intensity: The strength of the conditioning regimen affects the risk of relapse and transplant-related death.
Recognizing Signs of Relapse After Bone Marrow Transplant
It’s important to watch for signs of relapse after a stem cell transplant. Key signs include:
- Changes in blood counts: Unusual white blood cell counts or blasts in the blood or bone marrow.
- Symptoms recurrence: Coming back of symptoms like fatigue, weight loss, or bone pain.
- Chimerism analysis: In allogeneic transplants, a shift towards recipient cells (as opposed to donor cells) can signal relapse.
Spotting relapse early is key for quick action. Regular check-ups and monitoring are vital for managing recurrence risk.
The Longest AML Survivors: Stories of Hope and Resilience
AML, a tough form of leukemia, has amazing stories of long-term survivors. These people show us hope and resilience. They have not only survived but also thrived, often against all odds.
Remarkable Long-Term Survivor Cases
Many AML survivors have lived for years after being diagnosed. Some have stayed in remission for over a decade after treatments like chemotherapy and stem cell transplants. Their stories show us the power of medical progress and personal willpower.
One patient stayed in remission for over a decade after a bone marrow transplant. Such cases give us insights into what helps people survive long-term.
Common Factors Among Those Living with AML for Years
Studies have found common traits among long-term AML survivors. These include:
- Genetic predisposition: Some people’s genes help them respond better to treatment.
- Aggressive treatment approaches: Tough treatments like chemotherapy and stem cell transplants can greatly improve chances of survival.
- Supportive care: Care that covers physical, emotional, and mental needs is key.
|
Factor |
Description |
Impact on Survival |
|---|---|---|
|
Genetic Predisposition |
Influences response to treatment |
Positive |
|
Aggressive Treatment |
Intensive chemotherapy and transplants |
Significantly improves outcomes |
|
Supportive Care |
Comprehensive physical, emotional, and psychological support |
Enhances quality of life and survival |
Quality of Life for AML Survivors Thriving Against Odds
The quality of life for long-term AML survivors is very important. Many survivors have a new appreciation for life. They stay healthy through lifestyle changes and ongoing medical care.
Survivors say it’s important to stay positive and enjoy life. Support from family, friends, and groups helps them thrive.
Looking at the stories of the longest AML survivors, we learn a lot. We see what helps them stay strong and live well despite challenges.
Is Myeloid Leukemia Terminal? Understanding Prognosis
The outlook for AML patients changes a lot based on several things. These include the disease’s traits and how well it responds to treatment. Knowing these details is key for both patients and doctors to make the best treatment choices.
When AML Becomes Refractory
AML is tough to treat when it doesn’t get better with the first treatment. Or if it comes back after seeming to go away. This makes treatment harder, needing more intense and new ways to fight the disease.
There are many reasons why AML might not respond well. Some genetic changes make it hard for standard treatments to work. In these cases, patients might try new treatments or join clinical trials to find better options.
Does Leukemia Ever Completely Go Away?
For some, AML can seem to disappear completely. This is called complete remission. But, it doesn’t always mean the disease is gone for good. Tiny bits of the disease might stay hidden.
How likely it is to get into complete remission depends on a few things. These include the patient’s age, the disease’s genetics, and their overall health. Even if someone gets into complete remission, they often need to keep being checked and might need more treatment to stop it from coming back.
Factors That Determine Long-Term Outcomes
Many things can affect how well AML patients do in the long run. These include certain genetic changes, the patient’s age and health, and how well they do with the first treatment. Knowing these helps doctors tailor treatments to fit each patient’s needs.
|
Factor |
Influence on Prognosis |
|---|---|
|
Genetic Mutations |
Certain mutations, such as FLT3-ITD, can indicate a poorer prognosis, while others like NPM1 mutations may suggest a more favorable outcome. |
|
Age |
Older patients generally have a poorer prognosis due to decreased tolerance to intensive chemotherapy and a higher incidence of adverse genetic features. |
|
Response to Initial Treatment |
Achieving complete remission after initial treatment is a strong predictor of better long-term outcomes. |
By understanding these factors and how they affect prognosis, patients and doctors can work together. This helps create the best treatment plan for each person.
Innovative Therapies Improving AML Survival Rates
The field of AML treatment is changing fast with new therapies. Medical research has led to the creation of targeted molecular therapies, immunotherapy, and combination treatments. These advancements are boosting AML survival rates.
Targeted Molecular Therapies
Targeted molecular therapies have changed AML treatment by focusing on specific genetic mutations. These therapies aim to be more precise, harming fewer healthy cells and improving patient results. For example, studies show that targeting specific mutations can lead to better outcomes and longer life.
Some key targeted therapies include:
- FLT3 inhibitors for patients with FLT3 mutations
- IDH1 and IDH2 inhibitors for patients with IDH1/2 mutations
- Other emerging targets such as TP53 and NPM1 mutations
|
Targeted Therapy |
Mutation Targeted |
Clinical Benefit |
|---|---|---|
|
FLT3 inhibitors |
FLT3 |
Improved response rates and survival |
|
IDH1/2 inhibitors |
IDH1/2 |
Better outcomes in patients with IDH1/2 mutations |
Immunotherapy Approaches
Immunotherapy is a promising area in AML treatment, using the body’s immune system to fight cancer. Various immunotherapy methods are being explored, including:
- CAR-T cell therapy
- Checkpoint inhibitors
- Cancer vaccines
These therapies have shown promise in clinical trials, giving new hope to AML patients. Immunotherapy enhances the immune system’s ability to fight cancer cells, leading to a more durable response and potentially better long-term survival.
Combination Treatment Strategies for AML Recurrence
Combination treatment strategies are being used more to tackle AML recurrence. By combining different therapies, doctors can attack the disease from multiple sides. This can help overcome resistance and improve patient outcomes.
Some combination strategies include:
- Pairing targeted therapies with chemotherapy
- Combining immunotherapies with targeted therapies
- Using multiple targeted therapies together
These combination strategies are showing promise in clinical trials. They offer new ways to treat AML recurrence and improve survival rates.
Life After AML Relapse: Treatment Options
AML relapse is tough, but there’s hope. New treatments and clinical trials offer a chance for recovery. It’s important to reassess and plan a new treatment when AML comes back.
Second-Line Treatment Approaches
There are many options for AML relapse. These include different chemotherapies, targeted therapies, and stem cell transplants. These treatments aim to cure or control the disease.
Doctors choose treatments based on how long the first remission lasted, the patient’s health, and genetic tests.
Clinical Trial Opportunities
Clinical trials offer new, cutting-edge treatments. They include immunotherapy, targeted therapies, and combinations of treatments. These trials can lead to better outcomes.
Joining a clinical trial can be a good choice for those who have relapsed. It offers a chance for better results.
When Leukemia Remission Is Achieved Again
Getting remission again is a big win. It means careful management and regular checks to keep the patient healthy. This helps prevent another relapse.
- Regular follow-up appointments are key to watch for relapse signs.
- The treatment plan might need changes based on how the patient responds.
- Supportive care, like mental health support, is important for overall health.
End-of-Life Considerations with Advanced AML
End-of-life care for AML patients is more than just symptom management. It’s about giving emotional and psychological support too. As AML gets worse, patients and their families face many challenges. They need care that is both compassionate and all-encompassing.
Managing Symptoms in Advanced AML
Managing symptoms is a big concern for advanced AML patients. Symptoms can include pain, fatigue, bleeding, or infection. It’s key to manage these symptoms well to improve their quality of life.
We use different strategies to manage symptoms. These include:
- Pharmacological interventions to control pain and other symptoms
- Palliative care services to address the physical, emotional, and social needs of patients
- Supportive care measures to prevent and treat complications
|
Symptom |
Management Strategy |
|---|---|
|
Pain |
Pharmacological interventions, palliative care |
|
Fatigue |
Rest, nutritional support, gentle exercise |
|
Bleeding/Infection |
Transfusions, antibiotics, supportive care |
Palliative Care Approaches
Palliative care is a key part of end-of-life care for AML patients. It aims to ease symptoms and stress from serious illness. Our palliative care team works with patients and families to create care plans that fit their needs.
Palliative care includes:
- Symptom management
- Emotional and psychological support
- Spiritual care
- Support for patients and their families
Supporting Patients and Families
Supporting patients and their families is vital in end-of-life care. We offer counseling, emotional support, and practical help.
Our support services are:
- Counseling for patients and their families
- Emotional support groups
- Practical assistance with daily needs
We aim to enhance the quality of life for patients with advanced AML. We also support their loved ones during this tough time.
Psychological Impact of Living with Relapse Risk
The psychological impact of AML is deep, affecting patients and their families in many ways. Living with AML means always worrying about relapse. This worry can cause a lot of stress and anxiety.
Managing Fear of Recurrence
It’s key for AML survivors to manage their fear of recurrence. This fear can take over daily life and harm mental health. Strategies to manage this fear include:
- Regular follow-up appointments to monitor health
- Mindfulness and relaxation techniques to reduce stress
- Support groups where patients can share their experiences
By using these strategies, patients can deal with their fear better. This helps improve their quality of life.
Support Systems for AML Survivors
A strong support system is essential for AML survivors. This includes family, friends, healthcare providers, and support groups. These networks offer emotional support, practical help, and a sense of community. They are key to facing AML’s challenges.
Support groups are special. They let survivors share their stories and learn from others facing similar issues. This shared understanding is comforting and empowering.
Overcoming AML Against the Odds: Mental Resilience
Mental resilience is vital in overcoming AML. It’s about bouncing back from tough times, adapting to challenges, and staying positive. Building mental resilience can be done through:
- Setting realistic goals and celebrating achievements
- Practicing self-care and prioritizing well-being
- Seeking professional help when needed, such as counseling or therapy
By building mental resilience, AML survivors can handle the psychological challenges. This improves their overall well-being.
Conclusion: Hope and Progress in AML Treatment
Advances in AML treatment have greatly improved patient outcomes. This brings new hope for long-term survival. We’ve looked at the complexities of Acute Myeloid Leukemia, from diagnosis to treatment and survivorship.
The stories of the longest AML survivors show the progress made in fighting this disease. They are a testament to our growing understanding and management of AML.
As research goes on, new therapies are being found. These offer more options for patients at risk of relapse. By understanding what causes AML to come back, we can improve survival rates and quality of life for AML patients.
The journey with AML is tough, but there’s growing hope. With the progress in AML treatment, patients and their families have something to look forward to. We’re dedicated to providing top-notch healthcare and support to those dealing with this complex disease.
FAQ
What is Acute Myeloid Leukemia (AML)?
Acute Myeloid Leukemia (AML) is a blood cancer. It affects the bone marrow. This leads to abnormal white blood cells, causing anemia, infections, and bleeding.
Is AML always terminal?
No, AML is not always fatal. It’s a serious disease, but some patients can live for years with the right treatment.
What are the common symptoms of AML?
Symptoms include fatigue, weight loss, fever, night sweats, and easy bleeding or bruising.
How is AML diagnosed?
Doctors use blood tests, bone marrow biopsies, and genetic tests. These help find cancer cells and genetic issues.
What are the treatment options for AML?
Treatments include chemotherapy, targeted therapy, stem cell transplant, and clinical trials.
Can AML relapse after treatment?
Yes, AML can come back after treatment. This can happen due to genetic issues and how well the first treatment worked.
How does a stem cell transplant reduce the risk of AML relapse?
A stem cell transplant replaces the bone marrow with healthy cells. This can help get rid of cancer cells and lead to long-term remission.
What are the factors that influence the 5-year survival rate for AML patients?
Survival rates depend on age, genetic issues, treatment response, and health conditions.
Is dying from AML painful?
Dying from AML can be painful without proper care. Palliative care helps manage pain and symptoms, improving life quality.
Can AML go away completely?
Sometimes, AML goes into remission. With the right treatment, some patients can live long-term. But, they must stay under watch for relapse.
What are the innovative therapies improving AML survival rates?
New therapies like targeted treatments, immunotherapy, and combination strategies aim to boost survival and lower relapse risk.
How can AML survivors manage the fear of recurrence?
Survivors can stay connected with their doctors, use stress-reducing methods, and seek support from family and groups.
What is secondary AML?
Secondary AML develops after chemotherapy, radiation, or toxins. It often has a worse outlook than primary AML.
Can AML relapse after a bone marrow transplant?
Yes, AML can relapse after a transplant. The risk depends on remaining disease and transplant success.
References
• American Cancer Society. Key Statistics for Acute Myeloid Leukemia. https://www.cancer.org/cancer/types/acute-myeloid-leukemia/about/key-statistics.html
• SEER. Key statistics for acute myeloid leukemia. https://seer.cancer.gov/statfacts/html/amyl.html
• Haematologica. Outcomes and genetic dynamics of acute myeloid leukemia at first relapse. https://haematologica.org/article/view/11576
• PMC. Acute myeloid leukemia and acute lymphoblastic leukemia classification and metabolic characteristics for informing and advancing treatment. https://pmc.ncbi.nlm.nih.gov/articles/PMC11675077/
• Cancer.Net. Acute Myeloid Leukemia (AML) Statistics. https://www.cancer.net/cancer-types/leukemia-acute-myeloid-aml/statistics
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11966364/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























