Stay vigilant. Learn from the longest aml survivor how to recognize the subtle signs that leukemia has come back and what to do next.
Leukemia coming back is a big worry for patients, mainly those with Acute Myeloid Leukemia (AML). As the longest AML survivor, knowing the signs of recurrence is key. It helps in acting fast and managing the disease well.
To spot leukemia recurrence, doctors use a mix of checks, lab tests, and bone marrow exams. Spotting relapse signs early can really help patients. So, it’s important for patients and their families to know what to look for.
Finding AML relapse early can lead to better treatment plans and outcomes. Knowing how to spot leukemia remission and when it might come back helps patients make smart choices about their care.
Key Takeaways
- Leukemia recurrence is diagnosed through a combination of symptoms, lab tests, and bone marrow evaluations.
- Understanding the signs and symptoms of recurrence is key for early detection and effective management.
- Early detection of AML relapse can greatly improve patient outcomes and treatment strategies.
- Lab tests and bone marrow assessments are vital in diagnosing leukemia recurrence.
- Patients and caregivers should know what affects leukemia recurrence.
Understanding Leukemia Recurrence and Remission
For leukemia patients, knowing the difference between recurrence and remission is key. It’s important for managing the disease and making treatment choices.
What Defines Leukemia Recurrence vs. Remission
Leukemia recurrence happens when the disease comes back after treatment. Remission means the disease is controlled, with no leukemia cells found in the body. Remission can be partial or complete, with complete meaning no disease is detectable.
Understanding recurrence and remission helps decide the next treatment steps. If leukemia comes back, the treatment plan might change to fight it again.
Statistics on How Common Relapse Is Across Different Leukemia Types
Relapse rates differ in various leukemia types. Studies show about 15–20% of childhood Acute Lymphoblastic Leukemia (ALL) cases relapse. Acute Myeloid Leukemia (AML) relapse rates can be higher, influenced by genetics and initial treatment.
|
Leukemia Type |
Relapse Rate |
Factors Influencing Relapse |
|---|---|---|
|
Childhood ALL |
15-20% |
Genetic factors, initial treatment response |
|
AML |
Variable, often higher than ALL |
Cytogenetic factors, MRD status |
The Importance of Ongoing Monitoring
Regular checks are key to catching leukemia recurrence early. Blood tests, bone marrow biopsies, and other tests help spot the disease’s return. Early detection can greatly improve treatment results, making ongoing monitoring essential.
By grasping leukemia recurrence and remission, patients and doctors can better manage the disease. This knowledge helps patients actively participate in their care, leading to better outcomes.
Warning Signs That Leukemia May Have Returned
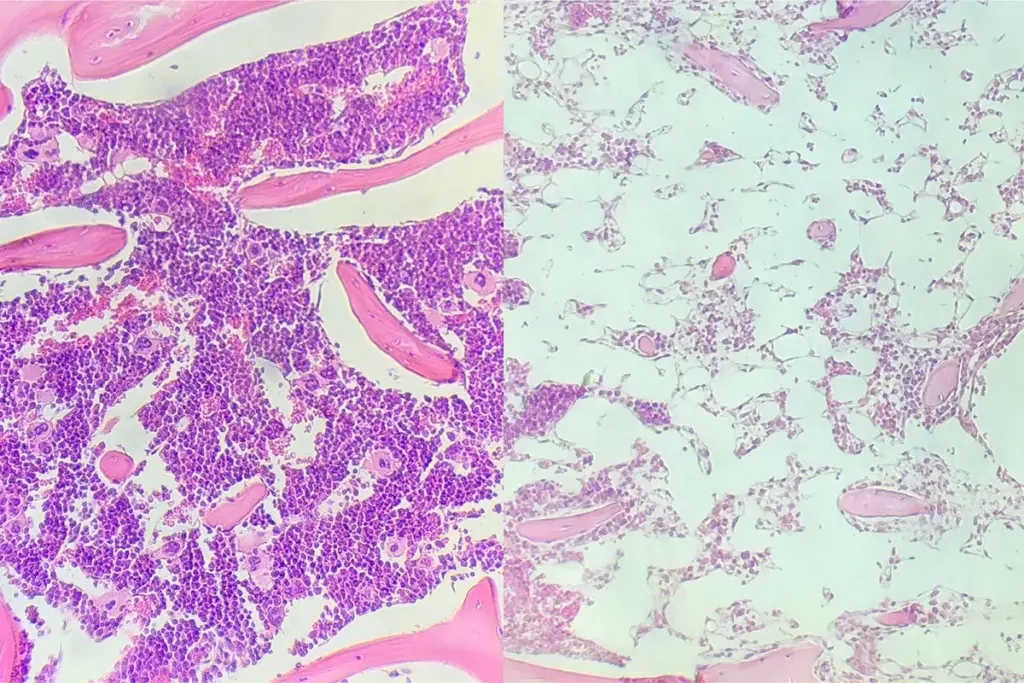
Leukemia can come back, and it’s important to know the signs. This way, you can get help quickly. We’ll talk about the main signs that leukemia might be back, and why it’s key to spot them early.
Physical Symptoms to Monitor
There are several signs that might mean leukemia is back. These include:
- Fatigue: Feeling very tired or weak, even after resting.
- Infections: Getting sick a lot or having infections that keep coming back. This is because leukemia can weaken the immune system.
- Bruising or Bleeding: Easy bruising or bleeding, like nosebleeds or bleeding gums. This is because there might not be enough platelets in the blood.
- Fever: Having a fever without a clear reason. It could mean there’s an infection or leukemia activity.
It’s important to watch these signs closely. Tell your doctor right away if you notice any changes.
Bone and Joint Pain as Possible Indicators
Pain in bones and joints can also be a sign of leukemia coming back. This pain might happen because leukemia cells are building up in these areas. Keep an eye out for:
- Persistent Pain: Pain in bones or joints that doesn’t go away and doesn’t have a clear cause.
- Swelling: Swelling in bones or joints, which can also cause pain.
If you’re feeling this kind of pain, it’s important to talk to your doctor. They can help figure out what’s causing it.
When to Seek Immediate Medical Attention
If you notice any of these, get medical help right away:
- Severe Bleeding: Bleeding that won’t stop or is very heavy.
- High Fever: Fever over 101.5°F (38.6°C) that lasts or is with other bad symptoms.
- Severe Fatigue: Feeling so tired that it stops you from doing daily things and doesn’t get better with rest.
Spotting leukemia early and treating it can make a big difference. Stay alert to your health and see a doctor if you notice anything odd.
Diagnostic Procedures for Detecting Recurrence
To find out if leukemia has come back, doctors use different tests. These tests help spot recurrence early and guide treatment.
Blood Tests and Complete Blood Counts
Blood tests are key in finding leukemia again. A complete blood count (CBC) is often the first step. It checks the levels of different blood cells.
Abnormal counts can show leukemia has returned. We look for signs like anemia or too few platelets. More tests may find specific leukemia markers.
Key Components of a CBC:
- White Blood Cell Count (WBC)
- Red Blood Cell Count (RBC)
- Platelet Count
- Hemoglobin and Hematocrit Levels
Bone Marrow Aspiration and Biopsy
Bone marrow tests are vital for diagnosing leukemia return. These tests take a sample of bone marrow for study.
A bone marrow aspiration uses a needle to take a liquid sample. A biopsy removes a small bone piece for microscope study. These tests check for leukemia cells in the bone marrow.
|
Procedure |
Description |
Purpose |
|---|---|---|
|
Bone Marrow Aspiration |
Withdrawal of liquid bone marrow sample |
Examine leukemia cells and assess marrow function |
|
Bone Marrow Biopsy |
Removal of a small piece of bone tissue |
Evaluate the extent of leukemia cell infiltration |
Advanced Imaging and Molecular Testing
Tests like PET scans or MRI can show how far leukemia has spread. They help find affected areas.
Molecular tests look at leukemia cell genes for specific mutations. This helps tailor treatments to each person’s needs.
Examples of Molecular Tests:
- PCR (Polymerase Chain Reaction) for detecting specific genetic mutations
- FISH (Fluorescence In Situ Hybridization) for identifying chromosomal abnormalities
By using these tests together, we can accurately find leukemia recurrence. Then, we can plan the best treatment.
AML Recurrence: Patterns and Detection
ML recurrence has unique traits that set it apart from other leukemias. Knowing these differences is key to managing and treating it effectively.
Characteristics of AML Relapse
AML relapse shows up when leukemia cells come back in the bone marrow or blood. It often has special genetic and molecular signs. Genetic mutations are a big part of why AML might come back.
Several factors contribute to AML relapse’s unique traits. These include:
- The presence of FLT3-ITD mutations, which raise the risk of relapse.
- Developing resistance to treatments, leading to more aggressive leukemia.
- Staying MRD after initial treatment, which can cause a full relapse.
Early Warning Signs Specific to AML
Spotting early signs of AML recurrence is critical for quick action. Common signs include:
- Persistent fatigue and weakness.
- Recurring infections because of a weak immune system.
- Unexplained bruising or bleeding.
- Bone and joint pain.
These symptoms can be vague. So, AML survivors need regular check-ups and to tell their doctors about any new or worsening symptoms.
Monitoring Protocols for AML Survivors
Good monitoring is key to catching AML recurrence early. These checks usually include:
- Regular blood tests and complete blood counts (CBCs) to watch for abnormal cell counts.
- Bone marrow aspiration and biopsy to check for leukemia cells.
- Advanced molecular testing to find minimal residual disease (MRD).
By knowing how AML recurrence works and following these monitoring steps, doctors can spot relapse early. This allows for quick action and better results.
Risk Factors That Increase Chances of Leukemia Returning
Leukemia can come back due to genetic, cytogenetic, and treatment-related factors. Knowing these risk factors helps manage the disease better. We’ll look at what increases the chance of leukemia coming back and how it affects patient care.
Genetic and Cytogenetic Factors
Genetic and cytogenetic factors are key in leukemia recurrence risk. Some genetic mutations and chromosomal changes can make the disease more aggressive. For example, changes in chromosomes 5 or 7, or mutations in FLT3 or NPM1 genes, can affect AML patients’ prognosis and relapse risk.
Initial Treatment Response as a Predictor
The first treatment response is a big indicator of leukemia coming back. Patients who quickly and fully respond to treatment usually do better. The speed and completeness of this response show how well the treatment is working and the patient’s chance of staying in remission.
Minimal Residual Disease (MRD) Significance
Minimal Residual Disease (MRD) is when a few cancer cells stay after treatment. The amount of MRD is a strong predictor of relapse risk. Tests like flow cytometry and molecular testing find and measure MRD. Patients with more MRD are at higher risk of recurrence and may need closer monitoring and extra treatment.
Timeline of Recurrence: Why Timing Matters
The timing of leukemia recurrence greatly affects treatment choices and patient results. Knowing when and why leukemia comes back is key to managing it well. We’ll look at the effects of early and late relapse and how monitoring changes over time.
Early Relapse Implications
Early relapse, within three years of first treatment, often means a more aggressive disease. This period is important because it shows how well the leukemia reacted to the first treatment.
Key factors associated with early relapse include:
- Genetic mutations that make the leukemia resistant to initial treatment
- Not responding well to the first treatment
- Having minimal residual disease (MRD)
Late Relapse Characteristics and Prognosis
Late relapse, after three years, might have different traits and a better outlook than early relapse. It can sometimes be linked to secondary leukemias or new genetic changes.
“The difference between early and late relapse is not just about timing; it shows different disease biology and how patients react to treatment.”
Hematologist
Monitoring Changes Over Time
As time goes by from the first diagnosis and treatment, how often and what to monitor might change. For example, those with a history of early relapse might need closer follow-up.
|
Time From Diagnosis |
Monitoring Frequency |
Tests Done |
|---|---|---|
|
0-3 years |
Every 3 months |
Blood counts, bone marrow biopsy |
|
3-5 years |
Every 6 months |
Blood counts, occasional bone marrow biopsy |
|
5+ years |
Annually |
Blood counts, annual check-up |
Treatment Approaches for Recurrent Leukemia
When leukemia comes back, we need to rethink how to treat it. We must adjust the treatment plan to tackle the disease’s growth and the patient’s health.
Chemotherapy Protocols for Relapse
Chemotherapy is often the first step for treating leukemia that comes back. It might use the same drugs as before or new ones to fight resistance. The choice depends on the leukemia type, how long it was in remission, and the patient’s health.
Key considerations for chemotherapy in relapse include:
- The risk of resistance to drugs used before
- Any health issues that might affect treatment
- The patient’s views on how intense the treatment should be
Targeted Therapies and Immunotherapies
Chemotherapy is not the only option anymore. Targeted therapies and immunotherapies are also key. Targeted therapies target specific genetic flaws in leukemia cells. Immunotherapies use the immune system to fight the disease.
Examples of targeted therapies include:
- Tyrosine kinase inhibitors for certain genetic mutations
- Monoclonal antibodies that target leukemia cell surface antigens
Immunotherapies, like CAR-T cell therapy, are showing great promise. They are most effective when other treatments have failed.
Clinical Trials for Refractory AML
Clinical trials are a lifeline for those with refractory AML. They offer access to new treatments not yet widely available. These trials are essential for finding better ways to treat leukemia.
Benefits of participating in clinical trials include:
- Access to new treatments that might improve outcomes
- Close care from a team of experts
- The chance to help develop treatments for others
Every patient’s situation is different. Treatment options depend on the leukemia type and how it has come back. Understanding these options helps patients and doctors make the best decisions.
Stem Cell Transplantation After Leukemia Relapse
In cases of AML recurrence, a stem cell transplant offers a new chance at survival. For some, this procedure is a way to achieve remission again.
When Bone Marrow Transplant Becomes Necessary for AML Recurrence
A bone marrow transplant (BMT) is considered for AML patients who relapse. This is true if their first treatment worked well or if a donor is available. The decision to undergo BMT depends on the patient’s health, AML type, and donor match. We look at each case to weigh the benefits and risks of this intense treatment.
The Transplant Process and Recovery
The stem cell transplant process has several stages. First, preparative conditioning gets rid of cancer cells and weakens the immune system. Then, healthy stem cells from a donor are infused. These cells replace the bone marrow and start making new blood cells. The recovery is key and needs careful watching for problems like GVHD or infections. We offer full care during this time to handle any side effects and help the patient recover.
Signs of Relapse After Bone Marrow Transplant
After a bone marrow transplant, patients are watched for relapse signs. These include fatigue, infections, or bruising. Regular check-ups and tests are vital for catching issues early. It’s important for patients to tell their healthcare team about any new or worrying symptoms right away. We work with our patients to spot and fix any problems quickly, improving their survival and quality of life chances.
Profiles of the Longest AML Survivors After Recurrence
Surviving AML recurrence is a big achievement. Looking at the journeys of long-term survivors gives us important insights. These people have not only beaten AML but also shown great strength in facing recurrence.
Remarkable Recovery Journeys and Survival Stories
The stories of long-term AML survivors are inspiring and varied. Some have gone through tough treatments like chemotherapy and stem cell transplants. Others have tried new therapies in clinical trials, helping them live longer.
For example, one survivor might have done well with targeted therapy. Another might have needed a mix of treatments, including immunotherapy. These stories show how complex AML is and how important personalized care is.
Common Factors Among Long-Term AML Survivors
Even though each survivor’s story is different, there are common things that help them live longer. These include:
- Timely and Effective Treatment: Getting the right treatment quickly is key.
- Strong Support Systems: Family, friends, and healthcare teams are very important.
- Positive Outlook: Keeping a positive mindset can really help.
- Participation in Clinical Trials: Trying new treatments can be beneficial.
Strategies That Contributed to Beating the Odds
Long-term AML survivors use different strategies to manage their condition and improve their life. These strategies include:
|
Strategy |
Description |
Benefit |
|---|---|---|
|
Healthy Lifestyle Choices |
Making smart choices about diet, exercise, and stress. |
Boosts overall health and resilience. |
|
Regular Monitoring |
Keeping up with health check-ups and screenings. |
Helps catch problems early. |
|
Mental Health Support |
Getting help for emotional and psychological challenges. |
Improves mental health and coping skills. |
By learning from the longest AML survivors after recurrence, we gain insights into what helps them survive long-term. Their stories inspire hope and guide patients and healthcare providers on how to manage AML recurrence effectively.
Life Expectancy and Survival Statistics After Relapse
Life expectancy after leukemia relapse varies a lot. It depends on many factors. Knowing these can help patients and their families.
Five-year Survival Rates by Leukemia Type
Survival rates after relapse differ by leukemia type. For example, Acute Lymphoblastic Leukemia (ALL) patients have different rates than those with Acute Myeloid Leukemia (AML). Studies show B-ALL patients might live 30-40% of the next five years. T-ALL patients might live 20-30% of the next five years. AML patients face a tough road, with a 10-20% chance of survival in the next five years.
Researchers found key factors for better survival. Their work shows the need for more research and tailored treatments.
Factors Influencing Long-term Survival
Many things affect survival after leukemia relapse. These include:
- Genetic and cytogenetic factors: The leukemia’s genetic makeup greatly affects survival.
- Initial treatment response: How well the leukemia responds to first treatment is a big survival predictor.
- Minimal residual disease (MRD): MRD levels after treatment can greatly influence long-term survival.
A study found MRD levels are a strong survival predictor. This highlights the need to monitor MRD levels closely.
Recent Improvements in Post-relapse Outcomes
Recently, post-relapse outcomes for leukemia patients have improved a lot. New treatments like targeted therapies and immunotherapies have helped. For example, CAR-T cell therapy has changed ALL treatment, giving patients new hope.
Recent advancements in leukemia treatment have greatly improved care. They offer better survival rates and quality of life for patients.
We keep seeing better treatments for leukemia. This means better survival rates and quality of life for patients. Understanding survival factors and staying updated on treatments helps patients and families face leukemia relapse challenges.
Emotional and Psychological Aspects of Facing Recurrence
Leukemia recurrence is more than a medical issue; it’s a journey of emotions and psychology. It requires resilience and support. Patients and their families face many emotions, like fear and frustration with treatment.
Coping with the Emotional Impact of Relapse
Dealing with leukemia recurrence is complex emotionally. It’s important for patients to acknowledge their feelings and seek help. Key strategies include:
- Talking openly with healthcare providers about emotional health
- Joining support groups to share and learn
- Doing stress-reducing activities like meditation or yoga
These steps can help manage the emotional toll of relapse. They make it easier for patients to cope.
Building Resilience and Maintaining Hope
Building resilience is key for patients facing leukemia recurrence. Resilience is about learning to handle challenges, not avoiding them. Patients can build resilience by:
- Focusing on the present and taking things one step at a time
- Celebrating small wins
- Setting and working towards realistic goals
Keeping hope alive is also important. It gives the motivation to keep going and improve life quality.
Support Resources for Patients and Families
Support resources are vital for patients and families facing leukemia recurrence. Available resources include:
- Professional counseling for emotional and psychological needs
- Online forums and support groups for connection
- Educational materials and workshops on managing leukemia
Using these resources, patients and families can better handle recurrence. This improves their well-being and resilience.
Managing Long-Term Health After Multiple Treatments
The journey doesn’t end with the completion of leukemia treatment. In fact, managing long-term health becomes a new priority. Leukemia survivors must be aware of the late effects of repeated treatments. They need to take proactive steps to maintain their overall health.
Late Effects of Repeated Leukemia Treatments
Repeated leukemia treatments can have significant long-term effects on the body. A study on the National Center for Biotechnology Information shows understanding these effects is key. Common late effects include:
- Cardiac issues due to certain chemotherapy drugs
- Increased risk of secondary cancers
- Cognitive difficulties
- Emotional and psychological challenges
Monitoring for Secondary Cancers
Leukemia survivors face a high risk of secondary cancers. Regular monitoring and follow-up care are essential. We recommend survivors work closely with their healthcare providers to develop a personalized follow-up care plan.
|
Secondary Cancer Type |
Risk Factors |
Monitoring Recommendations |
|---|---|---|
|
Myelodysplastic Syndromes (MDS) |
Previous chemotherapy, radiation exposure |
Regular blood counts, bone marrow biopsies as needed |
|
Solid Tumors |
Radiation therapy, certain chemotherapy agents |
Annual screening tests (e.g., mammograms, colonoscopies) |
Quality of Life Considerations for Survivors
Managing long-term health is not just about medical issues. It’s also about maintaining a good quality of life. Survivors should be aware of the resources available to them. This includes support groups and counseling services to help with emotional and psychological challenges.
By being proactive and informed, leukemia survivors can improve their long-term health outcomes. They can enjoy a better quality of life. We encourage survivors to stay connected with their healthcare team and to seek support when needed.
Conclusion
Understanding leukemia recurrence is key for both patients and healthcare providers. This article has covered the signs, symptoms, and how to diagnose it. We also talked about treatment options and the importance of ongoing monitoring.
Managing Acute Myeloid Leukemia (AML) needs a full plan. This includes standard treatments, targeted therapies, and immunotherapies. For some, stem cell transplantation is needed. Knowing the patterns of AML recurrence helps patients get early treatment, which can lead to better survival rates.
As we learn more about leukemia and its treatment, it’s vital for patients to stay informed. Working closely with healthcare providers helps patients manage their disease well. This teamwork can lead to the best possible outcomes.
FAQ
What are the signs that leukemia has come back?
Signs include fatigue, frequent infections, and bruising. Fever and bone and joint pain are also common. If you notice these symptoms, get medical help right away.
How is leukemia recurrence diagnosed?
Doctors use blood tests and bone marrow biopsies to diagnose. They also use advanced imaging and molecular testing. These tools help find recurrence early and plan treatment.
What are the risk factors for leukemia recurrence?
Genetic factors and how well you responded to treatment are risks. So is the presence of minimal residual disease (MRD). Knowing these helps manage the disease better.
How does the timing of leukemia recurrence impact prognosis?
Early relapse (within 3 years) has a different outlook than late relapse. Treatment plans may change over time based on your history and risk factors.
What treatment options are available for recurrent leukemia?
Treatments include standard chemotherapy and targeted therapies. Immunotherapies and clinical trials are also options, like for refractory AML. Sometimes, a bone marrow transplant is considered.
When is a bone marrow transplant necessary for AML recurrence?
A bone marrow transplant is needed when other treatments fail. It replaces diseased bone marrow with healthy stem cells. Recovery is key and needs careful monitoring.
What are the signs of relapse after a bone marrow transplant?
Signs include fatigue, infections, and bone pain. Changes in blood tests also indicate relapse. Regular checks are vital to catch relapse early.
How can patients cope with the emotional impact of leukemia recurrence?
Building resilience and hope helps. Seeking support from resources for patients and families is also key. Emotional support is essential for dealing with recurrence.
What are the long-term effects of multiple leukemia treatments?
Late effects include secondary cancers and organ damage. Monitoring for these and maintaining quality of life are important for survivors.
Is it possible to survive leukemia relapse?
Yes, survival after relapse is possible. Advances in treatment have improved outcomes. Survival depends on the type of leukemia, treatment response, and overall health.
What is the life expectancy after leukemia relapse?
Life expectancy varies. It depends on the type of leukemia, treatment response, and other factors. Five-year survival rates give a general idea, but individual outcomes can vary.
Can leukemia go away permanently after treatment?
Leukemia can go into remission. Some patients stay in long-term remission. But, the risk of recurrence remains, and ongoing monitoring is necessary.
What is the significance of minimal residual disease (MRD) in leukemia?
MRD is the presence of small leukemia cells after treatment. It indicates a higher risk of recurrence. Monitoring MRD helps guide treatment decisions.
Are there support resources available for leukemia patients and their families?
Yes, many resources are available. These include counseling, support groups, and educational materials. They help with the emotional and practical challenges of leukemia.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11966364/




































