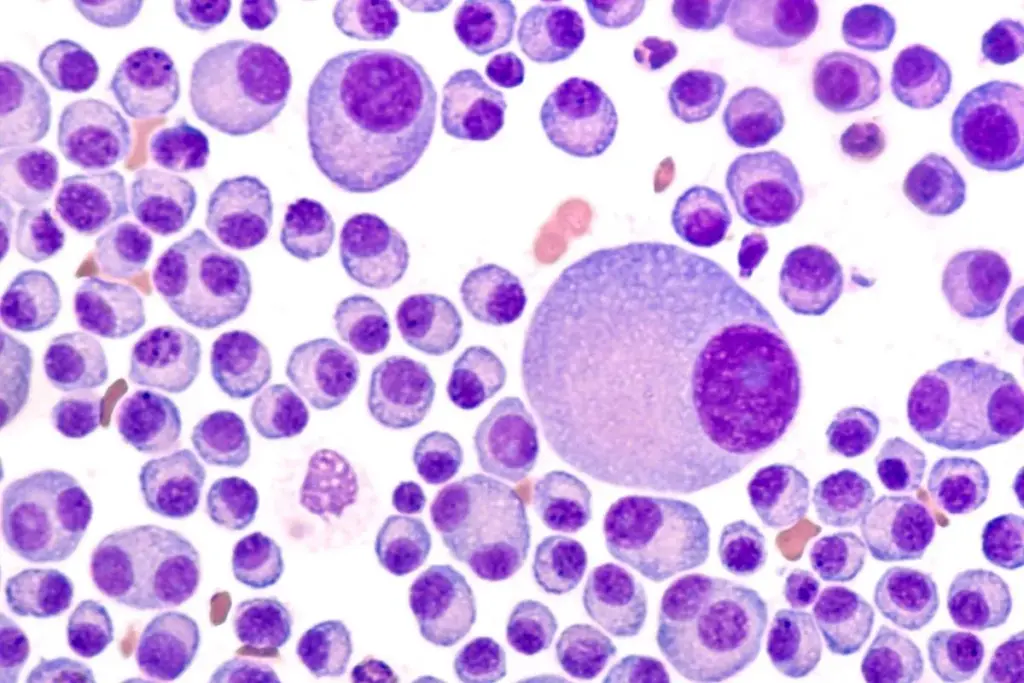
We know that myeloma often begins in the bone marrow. This is where plasma cells turn cancerous and grow too much. The bone marrow is inside some bones and makes blood cells.
In this cancer, cancerous plasma cells fill the bone marrow. They push out healthy blood cells. These cells make bad proteins instead of good antibodies, causing problems.
Understanding where myeloma starts is key for finding it early and treating it well. It’s a cancer of plasma cells and makes up about 10% of blood cancers.
Key Takeaways
- Myeloma usually starts in the bone marrow.
- Cancerous plasma cells accumulate and crowd out healthy blood cells.
- Abnormal proteins produced by cancerous cells can cause complications.
- Understanding the origin of myeloma is critical for early diagnosis.
- Good treatment plans depend on knowing where myeloma comes from.
Understanding Multiple Myeloma
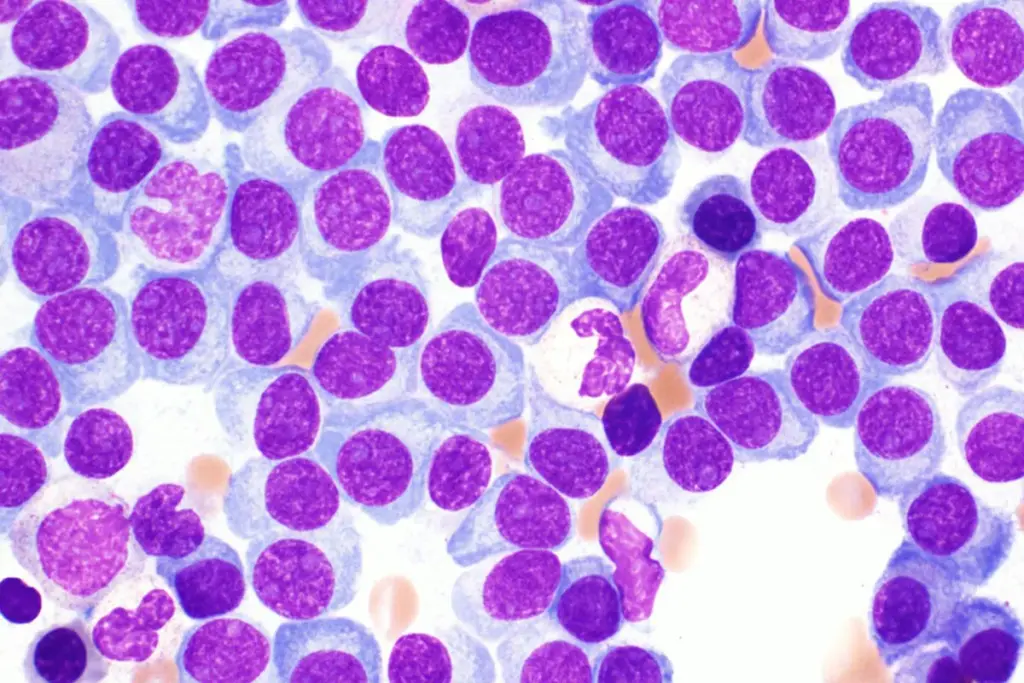
Multiple myeloma is a complex cancer that needs a deep understanding. We must know what it is and how it fits into plasma cell disorders. This helps us grasp the condition better.
Definition and Classification
Multiple myeloma is a cancer that affects plasma cells, a type of white blood cell. Plasma cells help fight infections by making antibodies. In this cancer, bad plasma cells fill the bone marrow, pushing out healthy cells.
This condition is marked by abnormal proteins in the blood and urine. These proteins are made by the cancerous plasma cells.
Understanding the various stages of multiple myeloma is crucial for effective treatment and management. It often starts with conditions like MGUS and SMM. These have monoclonal proteins but don’t have the full symptoms of active myeloma.
Types of Plasma Cell Disorders
Plasma cell disorders range from harmless to dangerous. MGUS and SMM can turn into myeloma. Other disorders include solitary plasmacytoma and plasma cell leukemia, which is more aggressive.
Knowing the different types is vital for diagnosis and treatment. Each has its own traits and care needs. This way, doctors can create the best treatment plan for each patient.
We will dive deeper into multiple myeloma and related disorders. This will give a full picture of these complex conditions.
Bone Marrow: The Primary Origin of Multiple Myeloma
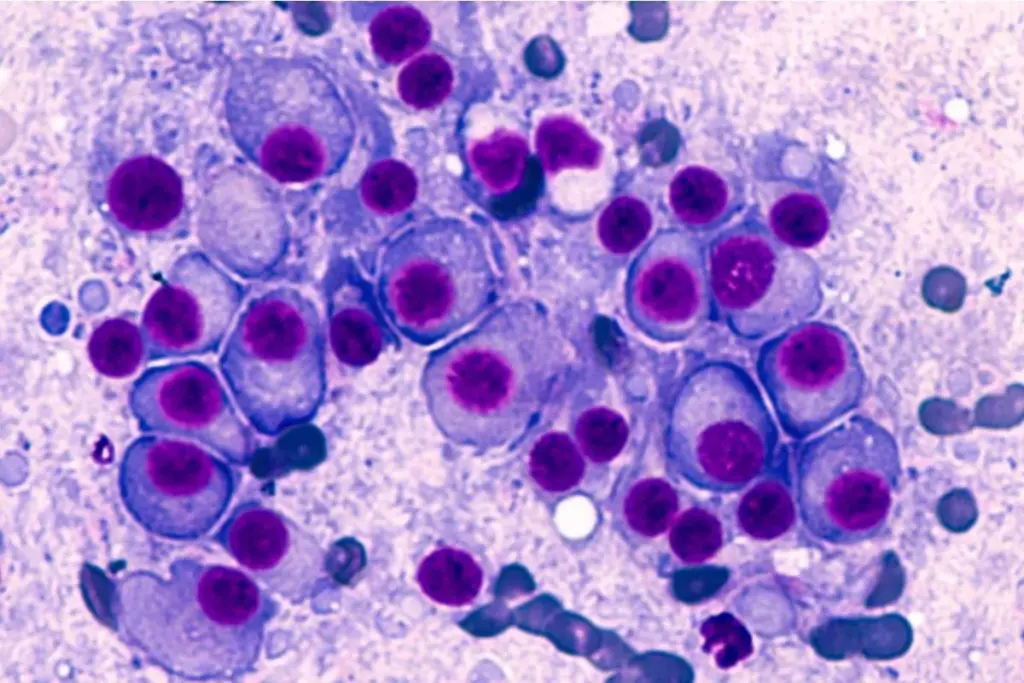
Multiple myeloma starts in the bone marrow. This cancer forms in plasma cells, a type of white blood cell. Plasma cells make antibodies. The bone marrow is inside some bones, like the hips and thighbones. It makes blood cells.
Structure and Function of Bone Marrow
Bone marrow is key for making blood cells. It has blood vessels and cells at different stages. This helps in producing red blood cells, white blood cells, and platelets.
The bone marrow’s environment helps blood cells grow and mature. It has growth factors and signaling molecules. These help blood cells work right.
Why Myeloma Targets Bone Marrow
Myeloma cells grow well in the bone marrow. It’s because the marrow supports their growth. The interaction between myeloma cells and the marrow is complex.
Myeloma cells change the marrow to help them grow. They promote new blood vessels and weaken the immune system. They also harm bones, causing destruction.
|
Aspect |
Normal Bone Marrow Function |
Impact of Multiple Myeloma |
|---|---|---|
|
Hematopoiesis |
Produces blood cells |
Disrupts normal blood cell production |
|
Microenvironment |
Supports blood cell development |
Alters microenvironment to support myeloma cell growth |
|
Bone Metabolism |
Regulates bone health |
Leads to bone destruction and lesions |
In summary, the bone marrow is where multiple myeloma starts. Knowing how myeloma cells and the marrow interact is key. This helps in finding better treatments.
Common Anatomical Sites of Myeloma Development
Multiple myeloma often shows up in specific parts of the skeleton. It usually hits areas with lots of bone marrow activity.
Spine and Vertebral Involvement
The spine is a common place for myeloma to start. It can cause bone pain and make bones break more easily. This can really hurt a patient’s quality of life.
Research shows that the lower and middle back are most at risk. This is because these areas have a lot of bone marrow.
Pelvis and Rib Cage
The pelvis and rib cage are also often affected. The pelvis, being a big bone with lots of marrow, can hurt and break. The ribs can get involved too, leading to noticeable changes or pain when breathing or moving.
Myeloma in these spots might not show symptoms early on. So, regular check-ups are key for catching it early.
Long Bones and Other Skeletal Sites
Long bones, like those in the arms and legs, can get myeloma too, but less often. When they do, they’re at risk for breaking, which can be very limiting.
Other bones, like the skull, can also be affected. This can cause different symptoms based on where and how much the disease is present.
To wrap up, here’s a table showing where myeloma usually hits and the problems it can cause:
|
Anatomical Site |
Common Complications |
Symptoms |
|---|---|---|
|
Spine |
Vertebral fractures, bone pain |
Back pain, loss of height, kyphosis |
|
Pelvis |
Fractures, pain |
Pain in the pelvic region, difficulty walking |
|
Rib Cage |
Fractures, deformities |
Pain upon breathing or movement, visible deformities |
|
Long Bones |
Fractures |
Pain, swelling, limited mobility |
Plasma Cells: From Normal Function to Malignancy
Plasma cells are key to our immune system. Knowing how they work normally helps us understand their role in cancer. They are white blood cells that make antibodies to fight infections. In multiple myeloma, they turn cancerous due to genetic changes.
Normal Plasma Cell Role in Immunity
Plasma cells are essential for our immune system. They make antibodies to fight off infections. This is vital for our body’s defense.
Malignant Transformation Process
The transformation of plasma cells into cancer involves genetic mutations. These changes lead to uncontrolled growth and abnormal proteins. In multiple myeloma, these cancerous cells fill the bone marrow, causing damage.
Clonal Evolution in Multiple Myeloma
Clonal evolution is when a single cancer cell grows and gets more mutations. This creates subclones with different traits, like treatment resistance. Knowing about clonal evolution helps in finding better treatments.
|
Characteristics |
Normal Plasma Cells |
Malignant Plasma Cells in Multiple Myeloma |
|---|---|---|
|
Antibody Production |
Produce normal antibodies to fight infections |
Produce abnormal proteins (M-protein) |
|
Cell Proliferation |
Tightly regulated, controlled proliferation |
Uncontrolled proliferation |
|
Genetic Integrity |
Maintain genetic integrity |
Accumulate genetic mutations |
Understanding how plasma cells turn cancerous is key to understanding multiple myeloma. This involves complex genetic and cellular changes. These changes lead to cancer cells building up in the bone marrow.
Precursor Conditions to Multiple Myeloma
Precursor conditions like MGUS and SMM are key in the development of multiple myeloma. These conditions show monoclonal proteins and clonal plasma cells in the bone marrow. They can lead to multiple myeloma.
Monoclonal Gammopathy of Undetermined Significance (MGUS)
MGUS is when a monoclonal protein is found in the blood or urine. It’s often found by chance during blood tests. It means you might be at risk for multiple myeloma, but the risk is low.
We keep an eye on people with MGUS for any signs of multiple myeloma. To be diagnosed with MGUS, you need a monoclonal protein level under 3 g/dL. Also, there should be less than 10% clonal plasma cells in the bone marrow, and no organ damage.
Smoldering Multiple Myeloma (SMM)
SMM is a stage between MGUS and multiple myeloma. It has more monoclonal protein and clonal plasma cells in the bone marrow than MGUS. People with SMM are at a higher risk of getting multiple myeloma.
To be diagnosed with SMM, you need a monoclonal protein level of 3 g/dL or more. Or, you need 10% or more clonal plasma cells in the bone marrow, without organ damage. We watch patients with SMM closely because early treatment can help prevent multiple myeloma.
Here’s a comparison of MGUS and SMM:
|
Characteristics |
MGUS |
SMM |
|---|---|---|
|
Monoclonal Protein Level |
Less than 3 g/dL |
3 g/dL or higher |
|
Clonal Plasma Cells in Bone Marrow |
Less than 10% |
10% or more |
|
Risk of Progression to Multiple Myeloma |
Low |
Higher |
A leading expert says, “Finding and watching precursor conditions like MGUS and SMM is key to catching multiple myeloma early.”
“Early detection is key to managing multiple myeloma effectively.”Myeloma Researcher
Extramedullary Myeloma: When Cancer Extends Beyond Bone Marrow
Extramedullary myeloma is a serious stage of multiple myeloma. In this stage, cancer cells spread beyond the bone marrow. This change often means the disease is more advanced and harder to treat.
Soft Tissue Involvement
Myeloma cells can move into soft tissues and organs outside the bone marrow. This includes places like the liver, kidneys, lungs, and even the brain. When this happens, managing the disease becomes more complex.
When myeloma spreads to soft tissues, it’s a sign of advanced disease. It makes treatment harder. We must watch patients closely for signs of this spread to act quickly.
Organ Infiltration Patterns
The way myeloma cells spread to organs can differ from person to person. Common places include the liver, spleen, and kidneys. Less often, it affects the lungs and brain. Knowing these patterns helps us diagnose and treat the disease better.
When myeloma spreads to organs, it makes the disease harder to manage. It also affects the patient’s quality of life. We must consider this when treating patients with multiple myeloma. This ensures we care for both the bone marrow and other affected areas.
In summary, extramedullary myeloma is a critical complication of multiple myeloma. Understanding its nature and impact helps us develop better treatment plans. This way, we can improve patient outcomes.
Epidemiology of Multiple Myeloma
The study of multiple myeloma shows us how common it is and who gets it. It’s a rare cancer but gets more common with age. Most people get it after they turn 65.
Incidence and Prevalence Statistics
Multiple myeloma makes up about 1% of all cancers and 10% of blood cancers. The (SEER) says most people get it when they’re 69 years old. It’s more common in men than women and varies by race and ethnicity.
Some important facts about multiple myeloma include:
- The number of new cases has stayed about the same in recent years.
- African Americans get it more often than Caucasians or Asians.
- It’s rare in people under 40.
Demographic and Age Distribution
Who gets multiple myeloma shows a clear pattern. It’s more common in older adults, with a big jump after 60. Men are a bit more likely to get it than women. There’s also a racial gap, with African Americans getting it more often.
Knowing these patterns helps us make better health plans and improve care for patients.
Risk Factors for Developing Multiple Myeloma
Multiple myeloma develops due to a mix of genetic, environmental, and demographic factors. Knowing these risk factors helps us understand the disease better. It also guides us on how to prevent it.
Age and Gender Considerations
Age is a big risk factor for multiple myeloma, with most cases found in people over 65. The risk goes up with age, hinting at age-related changes. Also, men are a bit more likely to get it than women.
Genetic Predisposition
Genetics play a key role in getting multiple myeloma. People with a family history of the disease are at higher risk. Genetic changes like translocations and mutations also raise the risk.
Environmental and Occupational Factors
Some environmental and job-related exposures increase the risk of multiple myeloma. These include radiation, certain chemicals, and pesticides. Knowing these risks helps in preventing and detecting the disease early.
In summary, multiple myeloma’s risk factors include age, gender, genetics, and environmental or job exposures. Recognizing these factors helps in early detection and management of the disease.
Early Signs and Symptoms of Multiple Myeloma
Knowing the early signs of multiple myeloma is key to managing it well. This disease affects the bone marrow and other organs, causing various symptoms.
Bone Pain and Skeletal Manifestations
Bone pain is a common symptom of multiple myeloma. It happens when cancer cells grow in the bone marrow. This can cause bones to weaken and hurt, often in the back, ribs, and hips.
This pain can last a long time and get worse. It might even cause bones to break easily, even without a big injury.
Fatigue, Anemia, and Blood Abnormalities
Fatigue is another common symptom, often due to anemia. Anemia happens when cancer cells replace healthy bone marrow cells. This makes it hard for the body to get enough oxygen.
People with multiple myeloma might also have low platelet and white blood cell counts. This makes them more likely to get infections and bleed easily.
|
Symptom |
Description |
Underlying Cause |
|---|---|---|
|
Bone Pain |
Persistent pain in the back, ribs, or hips |
Lytic lesions caused by myeloma cells |
|
Fatigue |
Feeling weak and tired |
Anemia due to replacement of normal bone marrow |
|
Kidney Problems |
Impaired kidney function |
Excess light chains produced by myeloma cells |
Kidney Problems and Other Systemic Symptoms
Kidney issues are common in those with multiple myeloma. This is because cancer cells produce too many light chains. These can harm kidney tubules and reduce kidney function.
Other symptoms include weight loss, frequent infections, and high calcium levels. These can cause confusion, weakness, and constipation.
Diagnosing Multiple Myeloma
Diagnosing multiple myeloma requires a detailed approach. It involves several tests to understand the disease’s extent and genetic traits.
Blood Tests and Biomarkers
Blood tests are key in diagnosing multiple myeloma. They help spot abnormal proteins from myeloma cells. Important tests include:
- Serum protein electrophoresis (SPEP) to detect monoclonal proteins
- Urine protein electrophoresis (UPEP) to identify abnormal proteins in urine
- Free light chain assays to measure kappa and lambda light chains
These tests are vital for diagnosing and tracking the disease.
Imaging Studies and Their Importance
Imaging studies are vital for seeing how much bone disease is present. They use:
- X-rays to spot bone lesions
- Magnetic Resonance Imaging (MRI) for detailed bone marrow checks
- Positron Emission Tomography-Computed Tomography (PET-CT) scans to find active myeloma cells
These methods help figure out how far the disease has spread. They also guide treatment and check how well it’s working.
Bone Marrow Biopsy and Genetic Testing
A bone marrow biopsy is a key test. It looks at bone marrow cells for myeloma. Genetic tests on these cells find specific traits, like:
|
Genetic Abnormality |
Clinical Significance |
|---|---|
|
Translocation t(11;14) |
Associated with standard risk |
|
Deletion 17p |
Indicates high-risk disease |
|
Translocation t(4;14) |
Associated with high-risk disease |
These tests give important clues about the disease’s risk. They help doctors plan the best treatment for each patient.
Challenges in Early Detection of Multiple Myeloma
Finding multiple myeloma early is hard because its symptoms are not clear.
Many times, multiple myeloma is found late. This is because its early signs are vague or missing. This late start can make treatment harder and affect how well patients do.
Why Localized Diagnosis Is Rare
Finding multiple myeloma in one place is rare. This is because it spreads through the bone marrow before symptoms show. By the time someone goes to the doctor, the cancer has usually spread.
Reasons for delayed diagnosis include:
- Lack of specific early symptoms
- Misattribution of symptoms to other conditions
- Limited awareness of multiple myeloma among the general public
Improving Early Detection Strategies
It’s important to find ways to detect multiple myeloma sooner. This can be done by raising awareness of risk factors and using screening tests for those at high risk.
Awareness and education are key to spotting multiple myeloma early. Doctors should watch for signs of the disease, mainly in older people and those with a family history.
Also, new diagnostic technologies and biomarkers will help find multiple myeloma sooner. Research on better tests is ongoing. It offers hope for earlier diagnosis and better care for patients.
Disease Progression and Spread Patterns
It’s important to know how multiple myeloma grows to manage it well. This disease can start in one place but spread to many bones and organs.
From Localized to Systemic Disease
At first, multiple myeloma might seem to be in just one spot, called solitary plasmacytoma. But it often turns into a bigger problem, called multiple myeloma. In this stage, cancer cells build up in the bone marrow.
This change happens because of how myeloma cells and the bone marrow work together. It leads to bone damage, anemia, and other big problems.
Common Pathways of Myeloma Spread
There are two main ways myeloma can spread: direct invasion and hematogenous spread. Direct invasion means myeloma cells move into nearby tissues and bones. Hematogenous spread happens when cancer cells travel through the blood to other places.
The table below shows where myeloma often goes and what it means for patients:
|
Skeletal Site |
Frequency of Involvement |
Clinical Implications |
|---|---|---|
|
Spine |
High |
Risk of vertebral fractures and spinal cord compression |
|
Pelvis |
High |
Bone pain, risk of fractures |
|
Ribs |
Moderate |
Pain, risk of fractures |
|
Long Bones |
Moderate |
Risk of fractures, bone pain |
Knowing how myeloma spreads helps doctors diagnose and treat it better.
In summary, myeloma’s growth from one spot to many involves complex biology. Understanding how it spreads and its effects is key to finding good treatments.
Current Treatment Approaches for Multiple Myeloma
The treatment for multiple myeloma has changed a lot, giving patients new hope. Now, we have many effective treatments that can be customized for each patient.
Initial Therapy Options
At first, treatment for multiple myeloma often includes induction chemotherapy to shrink tumors. We mix drugs like proteasome inhibitors, immunomodulatory agents, and corticosteroids for a quick response. The right treatment depends on the patient’s age, health, and if they can get a stem cell transplant.
Induction chemotherapy is key at the start, aiming for a deep response to better long-term results. We watch patients closely to see how they’re doing and adjust treatment if needed.
Stem Cell Transplantation
For some patients, stem cell transplantation is a big part of treatment. It involves taking stem cells from the blood or bone marrow, then using high-dose chemotherapy to kill myeloma cells. The stem cells are then given back to rebuild the bone marrow.
Stem cell transplantation can greatly improve how well patients do and how long they live. We check if a patient is a good candidate, looking at their age, health, and how far the disease has spread.
Maintenance Therapy Strategies
After the first treatment and stem cell transplant (if done), maintenance therapy helps keep the disease under control. We use drugs like lenalidomide to keep the disease from coming back.
The main goal of maintenance therapy is to keep the disease from getting worse and to make the treatment last longer. We choose the right maintenance treatment for each patient, balancing how well it works and its side effects.
By using initial therapy, stem cell transplant, and maintenance therapy together, we can really help patients. Our treatment plans are made just for each patient, considering their disease and health.
Advances in Multiple Myeloma Therapy
Medical research has led to new treatments for multiple myeloma, improving patient care. The treatment options for multiple myeloma have grown, giving patients and doctors more choices.
Immunotherapy Breakthroughs
Immunotherapy is a promising new approach for treating multiple myeloma. Monoclonal antibodies have shown great promise in targeting cancer cells. These therapies use the body’s immune system to fight cancer, making them a less toxic option than traditional treatments.
Some key immunotherapies include:
- Daratumumab, which targets CD38 on myeloma cells
- Elotuzumab, which targets SLAMF7
- Isatuximab, another CD38-targeting antibody
These treatments have shown success in clinical trials, both alone and with other treatments.
Targeted Treatments and Precision Medicine
Targeted treatments are another big step forward in treating multiple myeloma. Researchers have found ways to target specific genetic flaws in myeloma cells.
Proteasome inhibitors, like bortezomib and carfilzomib, are examples of targeted therapies that have helped patients. Also, immunomodulatory drugs like lenalidomide and pomalidomide have shown to be effective.
There’s also work on precision medicine, aiming to tailor treatments to each patient’s genetic profile.
The benefits of targeted treatments include:
- They work better because they target specific cells
- They cause fewer side effects than traditional chemotherapy
- Combining them with other treatments can lead to even better results
As research keeps moving forward, we can look forward to even more new treatments for multiple myeloma. This brings hope to patients and their families.
Conclusion: Understanding the Journey of Multiple Myeloma
Our look into multiple myeloma shows how complex it is. It starts in the bone marrow and can spread to other parts. Knowing how it works is key to finding it early and treating it well.
The path of multiple myeloma includes different stages. These include MGUS and smoldering multiple myeloma. Spotting these early is important for better care and results.
Research and clinical trials are changing how we fight multiple myeloma. New treatments like immunotherapy and targeted therapies give patients new hope.
By keeping up with the latest in treating multiple myeloma, we can help those fighting this disease. Together, we can make a difference in their lives.
FAQ
What is multiple myeloma?
Multiple myeloma is a cancer that affects plasma cells in the bone marrow. These cells are a type of white blood cell. It causes cancerous plasma cells to build up in the bone marrow, leading to problems.
Where does multiple myeloma usually start?
It usually starts in the bone marrow. This is the spongy tissue inside some bones, like the hips and thighbones.
What are the precursor conditions to multiple myeloma?
Before multiple myeloma, there are MGUS and Smoldering Multiple Myeloma (SMM). Both can turn into multiple myeloma.
What are the common symptoms of multiple myeloma?
Symptoms include bone pain, fatigue, anemia, and kidney issues. These happen because of the disease’s impact on the bone marrow and other organs.
How is multiple myeloma diagnosed?
Doctors use blood tests, imaging studies, bone marrow biopsy, and genetic testing. This helps diagnose the disease.
What are the risk factors for developing multiple myeloma?
Risk factors include age, genetics, family history, and certain exposures. These can increase the chance of getting the disease.
What are the current treatment approaches for multiple myeloma?
Treatments include initial therapy like chemotherapy and stem cell transplants. There are also maintenance therapies to keep the disease under control.
What is extramedullary myeloma?
It’s when myeloma cells spread to organs or soft tissues outside the bone marrow. This is often a sign of a worse prognosis.
How does multiple myeloma progress and spread?
It can start in one bone and spread to many. This happens through the bloodstream and direct invasion.
What are the advances in multiple myeloma therapy?
New therapies include immunotherapy and targeted treatments. These use specific genetic changes to fight the disease.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/35657121/

































