Explore the treatment options and recovery process for Joint Replacement. Learn about the surgical Arthroplasty procedure and what to expect during healing at Liv Hospital.
Send us all your questions or requests, and our expert team will assist you.
Treatment and Recovery
The surgical journey involves meticulous planning, precise execution, and a structured recovery pathway. Modern joint replacement is characterized by “Rapid Recovery” protocols. These are evidence based pathways designed to minimize stress on the body, manage pain effectively, and get patients moving immediately.
Treatment options vary based on the joint involved and the severity of the disease. While the surgery itself takes only an hour or two, the biological healing process takes weeks to months. The soft tissues must heal, and the bone must bond to the implant.
Recovery is a partnership. The surgeon performs the technical work, but the patient’s commitment to the post operative protocol determines the ultimate success.
Recovery starts before surgery. Pre hab involves exercises to strengthen the muscles around the joint prior to the operation. A stronger muscle recovers faster.
It also involves preparing the home environment—removing trip hazards, setting up a recovery station, and arranging for help. Education classes teach patients how to use walkers and what to expect, reducing anxiety and improving outcomes.

Most joint replacements are done under regional anesthesia (spinal or epidural) combined with sedation. This numbs the legs but keeps the patient breathing on their own, avoiding the side effects of general anesthesia like nausea and grogginess.
Peripheral nerve blocks are also used. The anesthesiologist injects numbing medicine around the nerves supplying the joint (e.g., adductor canal block for knees). This provides excellent pain relief for 18 to 24 hours after surgery without affecting muscle control significantly.
Surgeons use techniques that spare muscles. In the hip, the Direct Anterior Approach allows the joint to be replaced by separating muscles rather than cutting them. This often leads to less pain and no movement restrictions after surgery.
In the knee, subvastus or midvastus approaches avoid cutting the quadriceps tendon. These tissue sparing techniques preserve the blood supply and structural integrity of the muscles, facilitating a quicker return to walking.
During surgery, the robotic arm helps the surgeon execute the plan created from the CT scan. The robot does not act on its own; the surgeon guides it. The robot provides haptic feedback, stopping the saw or burr if it moves outside the planned safety zone.
This technology ensures that the bone cuts are accurate to within a fraction of a millimeter and a fraction of a degree. This precision balances the ligaments and aligns the limb perfectly, which is critical for the long term feel and survival of the joint.
Modern wound closure often avoids external staples. Surgeons use absorbable sutures under the skin and a zip line like closure or medical glue on the surface. This improves cosmetic results and eliminates the pain of staple removal.
Waterproof dressings containing silver (antimicrobial) are applied. These allow patients to shower immediately after surgery and are left in place for seven days, creating a sterile barrier that significantly reduces infection risk.
The era of heavy opioid use is ending. Multimodal analgesia uses a cocktail of non narcotic medications that attack pain from different angles. This typically includes anti inflammatories (NSAIDs), acetaminophen, and nerve pain medications (gabapentin).
By stacking these medications, the need for narcotics is drastically reduced. This prevents side effects like constipation, dizziness, and respiratory depression, allowing patients to be more alert and active in therapy.
Patients are typically encouraged to walk within hours of surgery. Physical therapists assist the patient in standing and taking their first steps. This early mobilization is crucial for preventing blood clots.
Getting up quickly also restores confidence and independence. Patients learn how to navigate stairs and use the bathroom safely before discharge. The goal is functional independence, not just bed rest.
TXA is a medication given during surgery to reduce bleeding. It stabilizes blood clots, preventing them from breaking down. Its routine use has almost eliminated the need for blood transfusions in standard joint replacements.
By reducing bleeding, TXA also reduces swelling and hematoma formation within the joint. Less swelling means less pain and an easier time regaining range of motion in rehabilitation.
Infection is the most feared complication. Prevention is aggressive. Patients use nasal decolonization swabs to kill bacteria in the nose before surgery. Antibiotics are given intravenously just before the incision.
Operating rooms use laminar airflow systems to keep the air sterile. Surgeons wear “space suits” (body exhaust systems) to prevent their own bacteria from reaching the patient. These redundant safety layers keep infection rates extremely low.
Most patients are discharged to their own homes, not nursing facilities. Home is a cleaner environment with familiar food and beds. Home health nurses and physical therapists visit to monitor the wound and guide exercises.
Patients are given strict instructions on wound care, medication schedules, and DVT (blood clot) prevention, which usually involves taking aspirin or a blood thinner for a few weeks.

Send us all your questions or requests, and our expert team will assist you.
With modern nerve blocks and multimodal pain medicine, pain is manageable. Most patients report the surgical pain is different—and often less severe—than the deep, grinding arthritis pain they lived with before. It is usually described as soreness and stiffness rather than sharp pain.
You can drive when you are off narcotic pain medication and have regained enough reaction time to safely move your foot from gas to brake. This is typically 2 to 4 weeks for a left leg surgery (automatic car) and 4 to 6 weeks for a right leg surgery.
Yes, most modern joint implants contain enough metal to trigger airport security scanners. You should tell the TSA agent you have an artificial joint. They will likely scan you with the wand. You do not need a doctor’s note, as they generally don’t accept them anyway.
With modern waterproof dressings, you can usually shower the day after surgery. You should not soak the incision in a bathtub, pool, or hot tub until it is fully healed, usually about 3 to 4 weeks.
Guidelines have changed. For most healthy patients with fully healed joints, routine antibiotics before dental cleaning are no longer recommended. However, if you have a compromised immune system or a history of infection, your surgeon may still advise it. Always check with your specific surgeon.

 Joint Replacement
Joint Replacement Joint Replacement
Joint Replacement Joint Replacement
Joint Replacement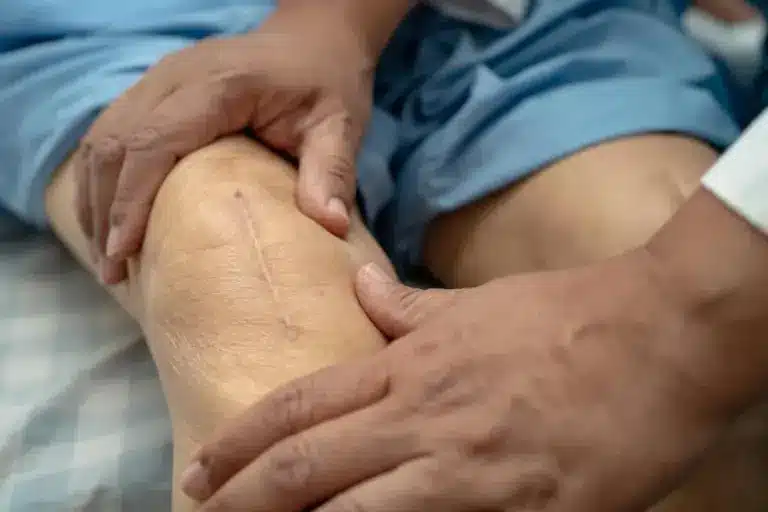 Joint Replacement
Joint Replacement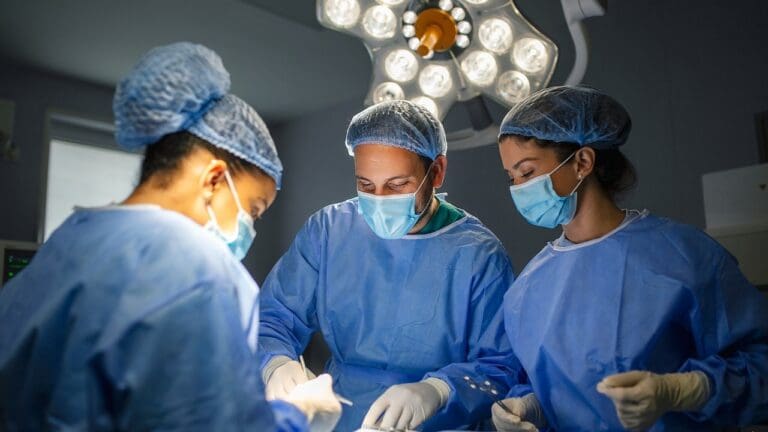 Joint Replacement
Joint Replacement Joint Replacement
Joint Replacement
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)