Plastic surgery restores form and function through reconstructive procedures, cosmetic enhancements, and body contouring.
Send us all your questions or requests, and our expert team will assist you.
The consultation is a comprehensive evaluation process. The surgeon assesses the patient’s facial balance, focusing on the relationship between the nose, lips, and chin. Physical palpation assesses the quality of the bone and the thickness of the soft-tissue pad.
The surgeon evaluates the dental bite. If a significant malocclusion (bad bite) is present, the chin issue may be secondary to a jaw issue. In these cases, the surgeon may recommend a consultation with an orthodontist or discuss orthognathic surgery.
Standardized photography is performed. The surgeon takes photos from frontal, profile, and oblique angles. These photos are critical for analysis and surgical planning.
Advanced clinics utilize 3D imaging technology (such as Vectra) to create a digital model of the patient’s face. This allows the surgeon to morph the image and simulate the potential surgical outcomes.
Patients can visualize how different amounts of projection will look on their faces. This tool is invaluable for communication, ensuring the patient and surgeon share the same aesthetic vision and managing realistic expectations.
A thorough medical history is taken to identify any contraindications. The surgeon asks about bleeding disorders, wound healing problems, and previous facial surgeries or trauma.
Smoking status is a critical factor. Nicotine constricts blood vessels and impairs bone healing. Patients are informed that smoking increases the risk of infection and implant rejection significantly.
The surgeon assesses the patient’s risk profile for anesthesia and surgery. Age, BMI, and chronic conditions like diabetes or hypertension are evaluated.
Patients with gum disease or active dental infections are identified. Because the surgery often involves intraoral incisions, oral health must be optimized before surgery to prevent infection of the bone or implant.
A review of all current medications and supplements is conducted. Blood-thinning medications (aspirin, ibuprofen, warfarin) and herbal supplements (fish oil, vitamin E, ginkgo) must be stopped before surgery to minimize bleeding.
The surgeon provides a specific schedule for stopping and restarting medications. Essential medications for chronic conditions are usually continued with particular instructions.
The surgeon evaluates the patient’s motivation and psychological readiness. Patients should seek surgery for themselves, not to satisfy a partner or career pressure.
Body dysmorphic disorder (BDD) is screened for. Patients with unrealistic expectations or an obsession with minor flaws may not be good candidates for surgery. The goal is a healthy, positive outlook on the enhancement.
If an implant is chosen, the specific size and shape are selected. The surgeon may use “sizers” during the consultation to give the patient a rough idea of the volume change, though 3D imaging is more accurate.
The surgeon explains the different materials available and helps the patient choose the best option for their anatomy and lifestyle.
Patients receive detailed written instructions for the days leading up to surgery. This includes fasting protocols (NPO after midnight) and skin cleaning regimens.
Instructions for postoperative care are also provided, so the patient can purchase supplies (soft foods, mouthwash, ice packs) and arrange their home environment for recovery.
Patients must arrange for a responsible adult to drive them home after surgery and stay with them for the first 24 hours. Driving is prohibited while on narcotic pain medication.
Planning for time off work and social activities is discussed. Understanding the downtime helps reduce stress during the recovery period.
Standard preoperative blood work is ordered to assess anemia and coagulation. For older patients or those with medical conditions, an EKG or medical clearance from a primary care doctor may be required.
This ensures the patient is physiologically fit to undergo the stress of surgery and anesthesia.
In some cases, specifically for osseous genioplasty, a panoramic X-ray of the teeth (Panorex) or a formal dental clearance may be requested. This ensures that the tooth roots are healthy and located safely away from the planned bone cuts.

Send us all your questions or requests, and our expert team will assist you.
Men should shave their faces on the morning of surgery to keep the field clean. However, be gentle to avoid nicks or razor burn that could harbor bacteria.
Yes, you should brush your teeth thoroughly to reduce bacteria in your mouth. Do not swallow any water. Rinse and spit completely.
If you develop a fever, cough, or significant illness, you must notify your surgeon. Elective surgery involving general anesthesia is usually rescheduled if the patient is sick to avoid airway complications.
You don’t have to guess. Trust your surgeon’s analysis. They use cephalometric norms (ideal angles and measurements) to recommend a projection that balances your nose and forehead. It is a mathematical and artistic decision.
Yes, most patients are required to wear a compressive chin strap or tape for the first week. This helps reduce swelling and supports the chin tissues in their new position. The surgeon will provide this.

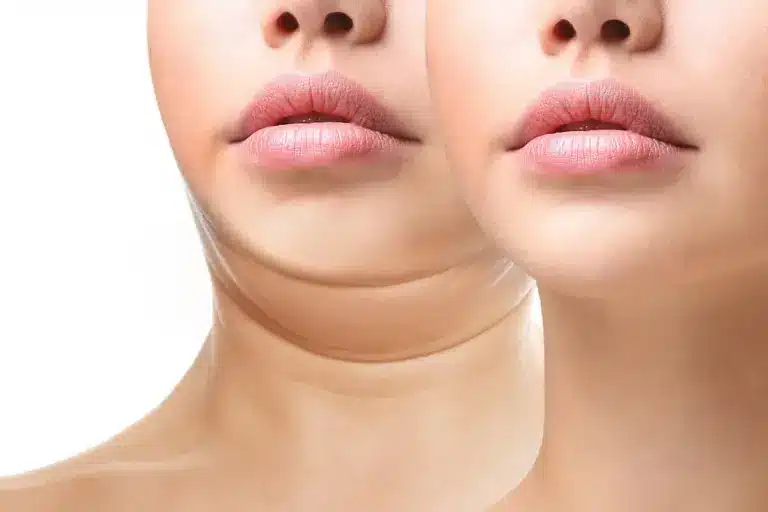 Chin Aesthetic
Chin Aesthetic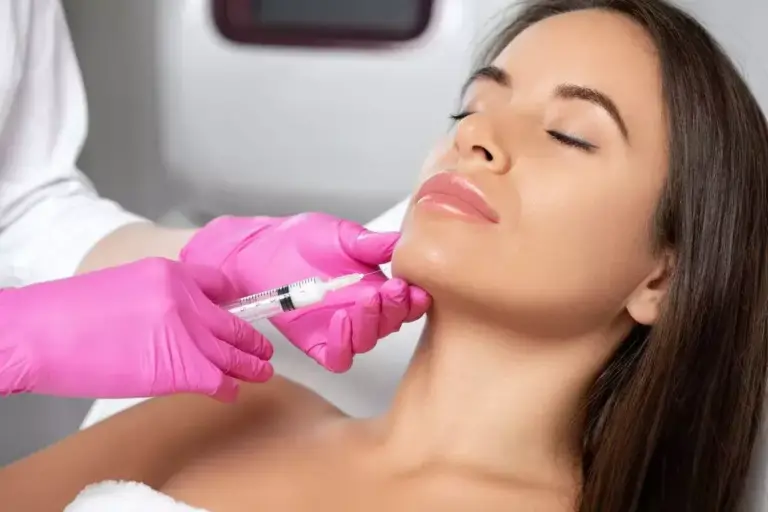 Chin Aesthetic
Chin Aesthetic
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)