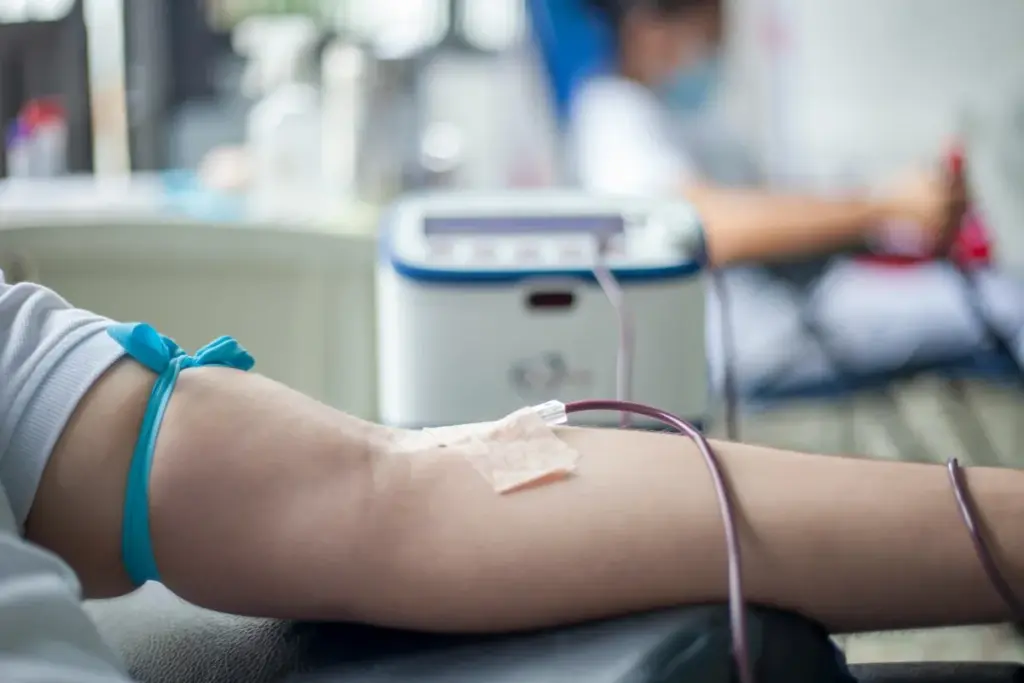
When someone’s platelet count gets very low, they face a big risk of severe bleeding. This is called thrombocytopenia and it’s very serious. At LIV Hospital, we know how urgent this is and how important platelet transfusions are to save lives.
A platelet infusion is needed when the body can’t make enough blood clots. This can happen for many reasons, like certain diseases or treatments. By giving a platelet transfusion, we can stop severe bleeding and help the patient get better.
Key Takeaways
- Platelet transfusions are critical for individuals with severely low platelet counts.
- Thrombocytopenia can be life-threatening and requires immediate medical intervention.
- Platelet infusions help support the body’s ability to form blood clots.
- Timely platelet transfusions can significantly improve patient outcomes.
- LIV Hospital specializes in providing expert care for patients requiring platelet transfusions.
Understanding Platelets and Their Function
Platelets, or thrombocytes, are tiny blood cells that play a big role in our health. They help stop bleeding by forming blood clots. These cells are made in the bone marrow and are always ready to help when needed. Knowing about platelets helps us understand bleeding disorders and when we might need a platelet transfusion.
What Are Platelets?
Platelets are small, anucleated cell fragments that are key to stopping bleeding. They come from megakaryocytes in the bone marrow and live for about 8 to 12 days. Platelet function is complex, involving adhesion, aggregation, and release of granules that contain clotting factors.
The Role of Platelets in Blood Clotting
Platelets are vital for preventing too much bleeding when a blood vessel is hurt. When injured, platelets stick to the damage, clump together, and release signals to bring more platelets. This leads to a fibrin clot that seals the injured vessel. The efficiency of platelet function is crucial for preventing both immediate and prolonged bleeding.
|
Condition |
Platelet Count |
Clinical Implication |
|---|---|---|
|
Thrombocytopenia |
< 150,000/μL |
Increased risk of bleeding |
|
Normal |
150,000 – 450,000/μL |
Normal hemostasis |
|
Thrombocytosis |
> 450,000/μL |
Increased risk of thrombosis |
Normal Platelet Count and Function
A normal platelet count is between 150,000 and 450,000 platelets per microliter (μL) of blood. Counts outside this range can signal health problems. Low platelet counts can lead to bleeding, while high counts can increase the risk of blood clots. Maintaining a normal platelet count is essential for proper blood clotting and overall cardiovascular health.
What Is a Platelet Transfusion?
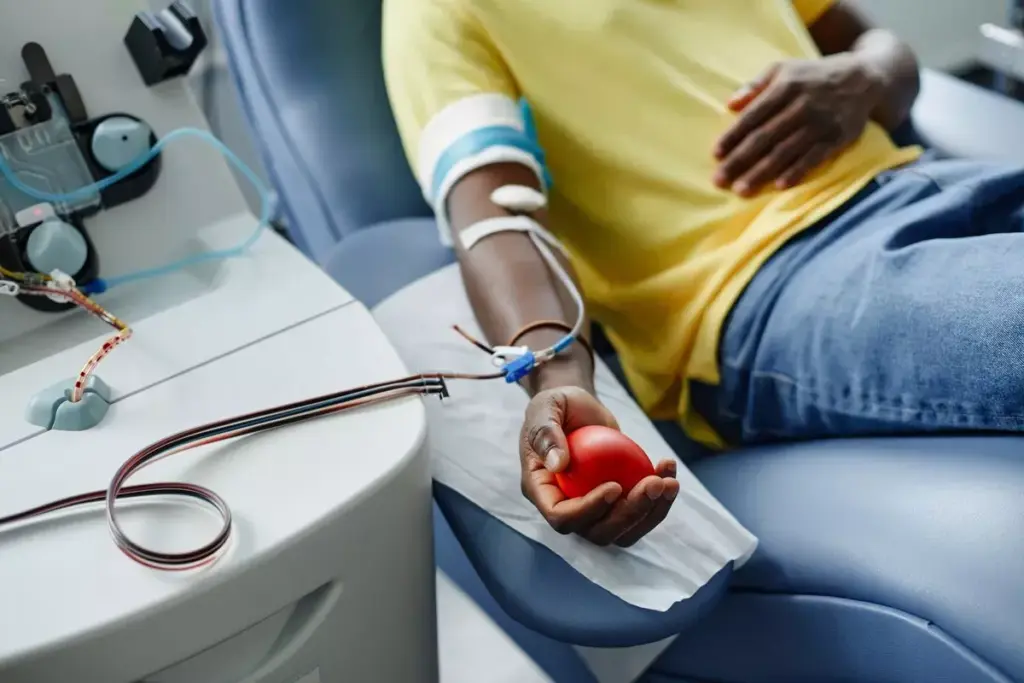
Platelet transfusions are key in modern medicine. They help patients with low platelet counts or dysfunction. These transfusions support patients during treatments that affect their platelets.
Definition and Basic Process
A platelet transfusion adds platelet products to a patient’s blood. It helps prevent or treat bleeding issues. The process starts with collecting platelets from donations or apheresis.
“Platelet transfusions are a lifeline for many patients,” say doctors. They let patients get treatments that are risky without them. The transfusions are prepared carefully, matching the product to the patient’s blood type.
Types of Platelet Products
There are different types of platelet products for transfusions:
- Random-donor platelets: These come from whole blood donations.
- Single-donor platelets (also known as apheresis platelets): These are from one donor via apheresis.
- Pooled platelets: These mix platelets from many donors.
Each type has its benefits and is chosen based on the patient’s needs.
How Platelets Are Collected and Processed
Platelets can be collected from whole blood or apheresis. Whole blood donations are processed to separate platelets. Apheresis collects platelets directly from donors.
Collected platelets are tested for diseases and compatibility. They are then prepared for transfusion.
Platelet processing is done carefully to keep them viable. They are stored under specific conditions for transfusion.
Medical technology keeps improving platelet collection and processing. This makes transfusions safer and more effective. We use the latest technology to care for our patients.
The Scope of Platelet Transfusion in Modern Medicine
Modern medicine heavily relies on platelet transfusions for many complex conditions. These transfusions are used in various clinical settings, from surgeries to treating blood disorders.
Annual Transfusion Statistics in the United States
In the United States, over two million platelet transfusions happen every year. This shows how vital platelet transfusions are in healthcare. For more info, check out the ARUP Laboratories for the latest on platelet transfusions.
Global Utilization Patterns
Platelet transfusions are used differently around the world. This depends on the healthcare system, disease rates, and product availability. Advanced healthcare systems use more platelet transfusions, showing their ability to treat complex conditions.
But, there are also healthcare access gaps globally. Some areas struggle to keep up with the demand for platelet products.
Economic Impact of Platelet Therapy
The economic side of platelet therapy is big. It includes direct costs like getting and giving platelets and indirect costs for managing side effects. The cost of platelet transfusions is high due to special handling and storage needs.
Yet, platelet transfusions are cost-effective. They help patients get better faster and stay in the hospital less time.
In summary, platelet transfusions play a huge role in modern medicine. They affect patient care, healthcare systems, and the economy. As medicine keeps changing, understanding platelet transfusions is key to better patient care worldwide.
Thrombocytopenia: The Primary Reason for Platelet Transfusions
Thrombocytopenia is a condition where you have too few platelets. Platelets are key for blood to clot. Without enough, serious bleeding can happen. We’ll look into what thrombocytopenia is, its symptoms, and when it’s a big deal.
Understanding Low Platelet Count
A normal platelet count is between 150,000 and 450,000 per microliter of blood. If it’s lower, you have thrombocytopenia. It can be caused by many things, like bone marrow problems or certain medicines. Knowing why you have it helps doctors treat you better.
Thrombocytopenia can be mild or severe. If it’s really low, you’re at high risk of bleeding. This is when you need to see a doctor fast.
Symptoms and Risks of Thrombocytopenia
People with thrombocytopenia might bruise easily or get small red spots. But severe bleeding is a big worry. Seeing a doctor early is key to avoid serious problems.
Thrombocytopenia can also mean there’s something else wrong with your body. We’ll talk about these risks and why a full check-up is important.
When Thrombocytopenia Becomes Life-Threatening
Thrombocytopenia is very serious when your platelet count is very low. Usually, this is below 10,000 per microliter. At this point, bleeding can be deadly. You need to get medical help right away.
Platelet transfusions are a big help when thrombocytopenia is severe. They raise your platelet count. This reduces bleeding risks and helps you get through tough times.
Medical Conditions That May Require Platelet Transfusion
Medical conditions can affect the bone marrow, liver, or platelet function. This may lead to the need for platelet transfusions to keep patients safe. Platelet transfusions are crucial for patients with various conditions that affect their platelet count or function. We will look at the different medical conditions that may need platelet transfusions and why these transfusions are so important.
Bone Marrow Disorders and Failure
Bone marrow disorders, like myelodysplastic syndromes or aplastic anemia, can lower platelet production. When the bone marrow can’t make enough platelets, transfusions are key to prevent bleeding. Leukemia can also harm the bone marrow, making it hard to produce platelets.
“The bone marrow is the factory of blood cells, and when it fails, patients are at risk of severe bleeding due to low platelet counts,” says a leading hematologist. “Platelet transfusions are a crucial intervention to support these patients until the underlying condition can be treated.”
Cancer and Chemotherapy Effects
Cancer and chemotherapy can greatly lower platelet counts. Chemotherapy can slow down bone marrow activity, causing thrombocytopenia. Cancer types such as leukemia directly affect the bone marrow, further complicating platelet production. In these cases, platelet transfusions are often necessary to manage the risk of bleeding.
- Chemotherapy-induced thrombocytopenia
- Leukemia and other bone marrow cancers
- Myeloproliferative neoplasms affecting platelet production
Aplastic Anemia and Other Blood Disorders
Aplastic anemia is a condition where the bone marrow fails to produce blood cells, including platelets. This condition can lead to severe thrombocytopenia, necessitating frequent platelet transfusions. Other blood disorders, such as certain types of anemia or myelodysplastic syndromes, can also require transfusion support.
Liver Disease and Platelet Function
Liver disease can indirectly affect platelet count and function. Conditions like cirrhosis can lead to splenic sequestration, where platelets are sequestered in the spleen, reducing their availability in the circulation. Liver dysfunction can also impair the production of thrombopoietin, a hormone crucial for platelet production. In advanced liver disease, platelet transfusions may be required to manage bleeding risks.
In conclusion, a range of medical conditions can necessitate platelet transfusions, from bone marrow disorders to liver disease. Understanding these conditions highlights the importance of platelet transfusions in clinical practice.
Surgical and Trauma Scenarios Requiring Platelet Transfusions
Surgical procedures and traumatic injuries often cause a lot of blood loss. This makes platelet transfusions very important for patient care. In these situations, controlling bleeding is key.
Major Surgery and Blood Loss
Major surgeries, like organ transplants or cancer resections, can cause a lot of blood loss. In these cases, platelet transfusions are often needed to prevent or treat bleeding. We check the patient’s condition and platelet count to decide if a transfusion is needed.
We aim to keep the patient’s platelet levels high to support their recovery and reduce the risk of bleeding. This helps improve patient outcomes in these tough surgical situations.
Trauma and Emergency Transfusions
Traumatic injuries, like those from car accidents or penetrating wounds, can cause severe bleeding. In emergencies, quick assessment and action are vital. Platelet transfusions are often given right away to help control bleeding.
We make sure blood products, including platelets, are given quickly to trauma patients. This helps keep the patient stable and prevents complications from massive transfusions.
Cardiac Surgery Requirements
Cardiac surgery, like CABG or heart transplantation, involves complex procedures that can affect platelet function. Patients may need platelet transfusions to manage bleeding.
Our team watches the patients’ platelet counts and function closely, before and after surgery. This helps us decide if a transfusion is needed. It also helps us improve patient care and lower the risk of complications after surgery.
Platelet Dysfunction: When Count Is Normal But Function Is Not
Having a normal platelet count doesn’t mean they work right. Platelet dysfunction is when your platelets don’t function well. This can cause bleeding problems.
Congenital Platelet Function Disorders
Congenital platelet function disorders are rare and present at birth. They affect how platelets work. This can cause easy bruising, nosebleeds, and prolonged bleeding after injuries or surgeries.
Examples include:
- Glanzmann’s thrombasthenia
- Bernard-Soulier syndrome
These conditions are diagnosed through clinical evaluation, family history, and lab tests. These tests check how platelets function.
Medication-Induced Platelet Dysfunction
Some medications can make platelets less effective, increasing bleeding risk. Common offenders are:
- Aspirin
- Clopidogrel
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
These drugs are used to prevent heart problems but can also affect platelet function.
“The use of antiplatelet therapy requires a careful balance between the benefits of preventing thrombotic events and the risks of bleeding complications.”
Hematologist
Diagnosing Platelet Function Disorders
Diagnosing platelet dysfunction involves several tests, including:
- Bleeding time tests
- Platelet aggregation tests
- Flow cytometry
These tests help doctors understand the problem. They guide how to manage it.
Dealing with platelet dysfunction can be tough. Our team is here to help. We provide comprehensive care and support to manage your condition.
Current Platelet Transfusion Guidelines and Thresholds
Platelet transfusion practices are getting better, aiming for better patient care and less risk. The latest guidelines show a deeper understanding of when and how to use platelet transfusions.
Prophylactic vs. Therapeutic Transfusions
There are two main types of platelet transfusions: prophylactic and therapeutic. Prophylactic transfusions help prevent bleeding in patients with low platelet counts. Therapeutic transfusions stop active bleeding.
Choosing between these types depends on the patient’s health, diagnosis, and bleeding risk. New guidelines suggest using prophylactic transfusions more carefully, only for those at highest risk.
Threshold Counts for Different Patient Groups
The need for a platelet transfusion varies by patient group. For example, patients getting chemotherapy or with certain cancers might need transfusions at different counts than those having surgery or trauma.
|
Patient Group |
Platelet Count Threshold |
|---|---|
|
Chemotherapy Patients |
10 x 10^9/L |
|
Surgical Patients |
50 x 10^9/L |
|
Trauma Patients |
100 x 10^9/L |
These counts come from clinical trials and guidelines by experts, like the AABB.
Evolution of Transfusion Protocols
Transfusion protocols have changed a lot, thanks to medical science and research. The move to more careful transfusions aims to avoid unnecessary ones and lower risks.
As we learn more about platelet transfusions, guidelines will keep changing. This shows how crucial it is to keep up with the latest in clinical practice.
The Platelet Transfusion Procedure Explained
The platelet transfusion process has many important steps. It ensures platelets are safely given to those who need them. This detailed procedure needs careful planning, precise action, and close follow-up care.
Before the Transfusion: Testing and Preparation
Several tests and preparations are done before a transfusion. Pre-transfusion testing checks the patient’s blood type and makes sure the donor platelets match. We also look at the patient’s platelet count and health to see if a transfusion is needed.
We check the patient’s medical history for any blood transfusion reactions. We also look at their current medications to avoid any bad interactions. This careful preparation helps lower the risk of problems during the transfusion.
During the Transfusion: What to Expect
During the transfusion, the patient is watched closely for any bad reactions. The transfusion goes through an IV line, and the flow is controlled to avoid overloading the patient.
We keep an eye on the patient’s heart rate, blood pressure, and temperature. Patients might feel some discomfort or worry, which we quickly address to keep them safe and comfortable.
After the Transfusion: Monitoring and Follow-up
After the transfusion, we keep watching the patient’s vital signs and look for any bad reactions. Post-transfusion monitoring is key to make sure the patient’s body is okay with the platelets.
We check the patient’s platelet count to see if it’s gone up as hoped. We also give them care instructions and schedule check-ups to watch how they’re doing and how they’re responding to the treatment.
Risks and Side Effects of Platelet Transfusions
Platelet transfusions save many lives but come with risks and side effects. It’s important for both doctors and patients to know about these risks.
Common Adverse Reactions
Most reactions to platelet transfusions are mild and short-lived. Common issues include:
- Febrile non-hemolytic transfusion reactions (FNHTR): These cause fever and chills. They’re usually not serious but can be uncomfortable.
- Allergic reactions: These can range from mild hives to severe reactions. Doctors often treat them with antihistamines or other medications.
Rare but Serious Complications
Though rare, some complications can be serious. These include:
- Transfusion-related acute lung injury (TRALI): This is a serious condition that causes breathing problems.
- Transfusion-associated circulatory overload (TACO): This happens when the transfusion puts too much strain on the heart. It can lead to breathing problems and other issues.
- Graft-versus-host disease (GVHD): A rare but serious condition where the transfused platelets attack the recipient’s body.
Managing Transfusion Reactions
It’s crucial to manage transfusion reactions well to keep patients safe. If a reaction is suspected, the transfusion is stopped, and the patient is checked. The management depends on the reaction’s severity and type. It may include:
- Medications to help with symptoms, like antipyretics for fever or antihistamines for allergies.
- Supportive care, like oxygen therapy for breathing issues.
- In severe cases, more intensive care, like hospitalization for close monitoring and treatment.
Knowing the risks and side effects of platelet transfusions helps doctors manage these treatments better. This ensures the benefits are greater than the risks for each patient.
Special Considerations for Specific Patient Populations
When giving platelet transfusions, we must think about certain groups like kids, pregnant women, and older adults. Each group has special needs that doctors must consider. This ensures safe and effective care for everyone.
Pediatric Patients and Platelet Transfusions
Kids need special care because they are small and their bodies are still growing. Doctors use the child’s weight or body size to figure out how much platelets to give. Also, kids might face higher risks because their immune systems are still growing.
Doctors must carefully decide if kids need platelet transfusions. They weigh the benefits against risks like lung problems or immune reactions. Using special blood products can help lower these risks.
Pregnant Women and Platelet Needs
Pregnant women might need platelet transfusions for severe low platelet counts or bleeding. Pregnancy changes the body, affecting platelet counts and function.
Doctors keep a close eye on pregnant women for signs of low platelets or platelet problems. These issues can affect both the mother and the baby. Platelet transfusions might be needed to manage severe low platelets or to prepare for delivery.
Elderly Patients and Transfusion Considerations
Older adults often have complex health histories and conditions that affect platelet transfusions. Age-related changes and health problems can raise the risk of complications from transfusions.
When thinking about platelet transfusions for older adults, doctors consider their overall health, chronic diseases, and how well they can handle risks. It’s important to carefully weigh the benefits and risks in this group.
|
Patient Population |
Special Considerations |
Transfusion Strategies |
|---|---|---|
|
Pediatric Patients |
Weight-based dosing, immature immune systems |
Irradiated and leukoreduced products |
|
Pregnant Women |
Physiological changes, fetal considerations |
Monitoring for thrombocytopenia, preparation for delivery |
|
Elderly Patients |
Comorbid conditions, cardiovascular changes |
Careful risk-benefit assessment, consideration of overall health status |
Platelet Refractoriness: When Transfusions Don’t Work
Platelet refractoriness is a complex issue. It happens when patients don’t respond to platelet transfusions as expected. This condition is a big challenge, especially for those needing ongoing transfusions.
Causes of Platelet Refractoriness
The causes of platelet refractoriness can be divided into two main groups: immune and non-immune factors. Immune causes often involve antibodies against HLA or platelet-specific antigens. Non-immune causes include conditions like splenomegaly, DIC, and sepsis.
HLA-Matched Platelets and Other Solutions
Using HLA-matched platelets is a key strategy for managing platelet refractoriness. Matching the HLA types of donor and recipient reduces the risk of immune reactions. For more on platelet transfusion guidelines, including HLA-matched platelets, check out America’s Blood Centers.
Managing the Refractory Patient
Managing patients who don’t respond to platelet transfusions needs a detailed approach. It involves finding and fixing the underlying causes, choosing the right platelet products like HLA-matched platelets, and watching how the patient reacts to transfusions.
The Shift Toward Restrictive Platelet Transfusion Practices
A growing body of evidence supports the adoption of more restrictive platelet transfusion practices. This shift is driven by research indicating that more conservative transfusion strategies can reduce risks and conserve resources without compromising patient outcomes.
Evidence Supporting Restrictive Approaches
Many studies have shown that restrictive transfusion thresholds are as effective as more liberal approaches in many clinical scenarios. For instance, a landmark study published in the New England Journal of Medicine found that patients receiving restrictive transfusions had similar outcomes to those receiving more generous transfusions, with fewer complications.
The evidence supporting restrictive transfusion practices is not limited to a single patient population. Research across various clinical contexts, including surgery, critical care, and hematology/oncology, has shown that conservative transfusion strategies can be safely implemented.
Key Findings:
- Reduced risk of transfusion-related complications
- Conservation of blood products
- No significant difference in patient outcomes in many cases
Benefits of Using Fewer Transfusions
The benefits of adopting restrictive platelet transfusion practices are multifaceted. By reducing the number of transfusions, healthcare providers can minimize the risk of transfusion-related complications, such as allergic reactions, transfusion-related acute lung injury (TRALI), and transmission of infectious diseases.
|
Benefit |
Description |
|---|---|
|
Reduced Complication Risk |
Lower incidence of transfusion-related adverse events |
|
Resource Conservation |
More efficient use of blood products, reducing waste and costs |
|
Improved Patient Outcomes |
No compromise in patient care, with potential for better outcomes due to fewer complications |
Implementing Restrictive Protocols in Clinical Practice
Implementing restrictive transfusion protocols requires a multidisciplinary approach, involving clinicians, transfusion services, and hospital administrators. Education and training are crucial to ensure that healthcare staff understand the rationale behind these protocols and how to apply them effectively.
We must also consider the challenges associated with implementing restrictive transfusion practices, including the need for robust monitoring and evaluation systems to ensure that these strategies are safe and effective in real-world settings.
Implementation Strategies:
- Develop clear guidelines and protocols
- Provide education and training for healthcare staff
- Monitor and evaluate the effectiveness of restrictive transfusion practices
LIV Hospital’s Approach to Platelet Transfusion Therapy
LIV Hospital focuses on the best practices, innovation, and care for patients. We aim to provide top-notch healthcare to international patients. Our goal is to show the best in platelet transfusion therapy.
Best Practices and International Standards
At LIV Hospital, we follow strict international standards for platelet transfusions. Our methods ensure quality care from start to finish. We follow guidelines from top health organizations to give our patients the best treatment.
We are dedicated to the highest standards. Our screening and testing are thorough to ensure platelet safety and effectiveness. Our medical team also gets ongoing training to keep up with new transfusion medicine advancements.
Innovation in Transfusion Medicine
Innovation is key in our transfusion medicine program at LIV Hospital. We use the newest technologies and methods to improve transfusion safety and success. Our team works with international partners to bring in the latest research and techniques.
We focus on creating personalized transfusion plans for each patient. This approach makes treatment more effective and safer for our patients.
Patient-Centered Transfusion Protocols
At LIV Hospital, we put patients first in our transfusion protocols. We understand that every patient is different. Our protocols are designed to make the transfusion process as comfortable as possible.
We also make sure patients and their families are well-informed. We teach them about the transfusion process, its risks, and benefits. This helps them make informed decisions about their care.
|
Key Aspect |
Description |
Benefit |
|---|---|---|
|
Best Practices |
Adherence to international standards and guidelines |
Ensures high-quality care and safety |
|
Innovation |
Investment in latest technologies and techniques |
Improves efficacy and safety of transfusions |
|
Patient-Centered Care |
Tailored protocols and patient education |
Enhances patient comfort and informed decision-making |
Conclusion: The Future of Platelet Transfusion Medicine
Looking ahead, platelet transfusion medicine is set for big changes. Medical science and technology will keep pushing the boundaries of transfusion therapy. We’re seeing major steps forward, thanks to new ideas in transfusion medicine and a better grasp of platelet biology.
The future looks bright for platelet transfusions. We might see personalized transfusion plans, better ways to store platelets, and new substitutes for platelets. These advancements could mean better care for patients, fewer risks, and more efficient use of platelet products.
At LIV Hospital, we’re all about keeping up with these advances. We use the latest research and tech to give our patients the best care. As the field grows, we’re committed to top-notch healthcare and support for international patients.
FAQ
What is a platelet transfusion, and when is it necessary?
A platelet transfusion is when platelets are given to a patient to stop bleeding. This happens when a patient has too few platelets or when platelets don’t work right. It’s needed when a patient’s platelet count is very low or when platelets don’t function well.
What are the risks associated with platelet transfusions?
Platelet transfusions are usually safe but can have risks. These include allergic reactions, lung problems, and infections. It’s important to manage these risks to keep patients safe.
How are platelets collected and processed for transfusion?
Platelets are collected from donors through apheresis. This is when whole blood is drawn, and platelets are separated and collected. The rest of the blood is returned to the donor. Then, the platelets are tested and stored for use.
What is thrombocytopenia, and how is it treated?
Thrombocytopenia is when a person has too few platelets, leading to bleeding. Treatment depends on the cause. In severe cases, platelet transfusions may be needed to stop bleeding.
Can platelet transfusions be used in surgical and trauma scenarios?
Yes, platelet transfusions are crucial in surgeries and trauma. They help prevent or control bleeding. They are often lifesaving.
What is platelet dysfunction, and how is it diagnosed?
Platelet dysfunction is when platelets don’t work right, even with a normal count. It can be caused by genetic issues or certain medicines. Tests like aggregometry or flow cytometry are used to diagnose it.
What are the guidelines for platelet transfusions?
Guidelines for platelet transfusions vary based on the patient’s condition. They cover when to use transfusions and the counts needed. The goal is to use transfusions wisely while keeping patients safe.
How does LIV Hospital approach platelet transfusion therapy?
LIV Hospital follows best practices in platelet transfusion therapy. They focus on innovation and patient care. Their goal is to improve patient outcomes and safety.
What is platelet refractoriness, and how is it managed?
Platelet refractoriness is when patients don’t respond to transfusions. It’s often due to immune issues. Managing it involves using HLA-matched platelets and other strategies to improve transfusion success.
Are there special considerations for specific patient populations receiving platelet transfusions?
Yes, certain groups like kids, pregnant women, and the elderly need special care. Their unique needs require tailored transfusion therapy for the best care.
What is the future of platelet transfusion medicine?
The future of platelet transfusion medicine looks promising. It will include new technologies, better guidelines, and more patient-focused care. This will lead to better patient outcomes.
References
The Lancet. Evidence-Based Medical Insight. Retrieved from
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(12)61264-1/fulltext


































