Bronchitis is a significant respiratory condition characterized by inflammation of the lining of the bronchial tubes, the central airways that carry air to and from the lungs. This inflammation leads to swelling of the bronchial walls and excessive mucus production, which clogs the airways and impairs normal airflow. The condition is broadly categorized into two distinct types: acute bronchitis and chronic bronchitis. Acute bronchitis is often a short-term illness that usually follows a viral respiratory infection, such as the common cold or influenza. In contrast, chronic bronchitis is a serious, long-term condition that is often part of a group of lung diseases known as chronic obstructive pulmonary disease. The defining feature of bronchitis is a persistent cough that produces thickened, discolored mucus. At Liv Hospital, we approach bronchitis by focusing on understanding the underlying inflammatory processes to distinguish between transient viral infections and potentially progressive chronic conditions.
Send us all your questions or requests, and our expert team will assist you.
The bronchial tree is an intricate network of airways that serves as the conduit for gas exchange. It begins at the trachea and divides into the right and left main bronchi, which further subdivide into smaller secondary and tertiary bronchi, eventually ending in the bronchioles. These airways are lined with a specialized mucous membrane containing goblet cells and cilia. The goblet cells produce mucus to trap dust, bacteria, and other foreign particles, while the cilia are hair-like structures that beat in a rhythmic motion to move the mucus upward toward the throat to be swallowed or coughed out. In bronchitis, this defense mechanism is compromised. Inflammation damages the cilia, paralyzing or destroying them entirely, thereby preventing adequate mucus clearance. This accumulation of mucus and cellular debris creates a breeding ground for pathogens and significantly narrows the airway lumen, increasing resistance to airflow.
When a pathogen or irritant assaults the bronchial epithelium, the body initiates an acute inflammatory response.
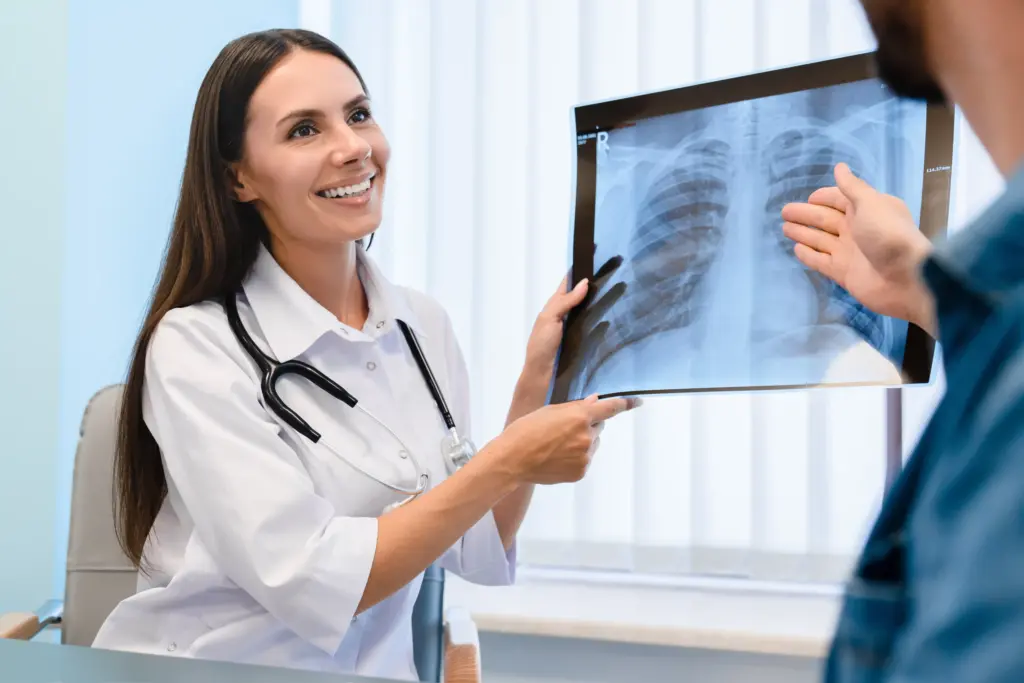
Chronic bronchitis represents a more permanent alteration of the airway structure and function. It is clinically defined as a productive cough that lasts for at least three months in two consecutive years, where other causes of cough have been excluded.
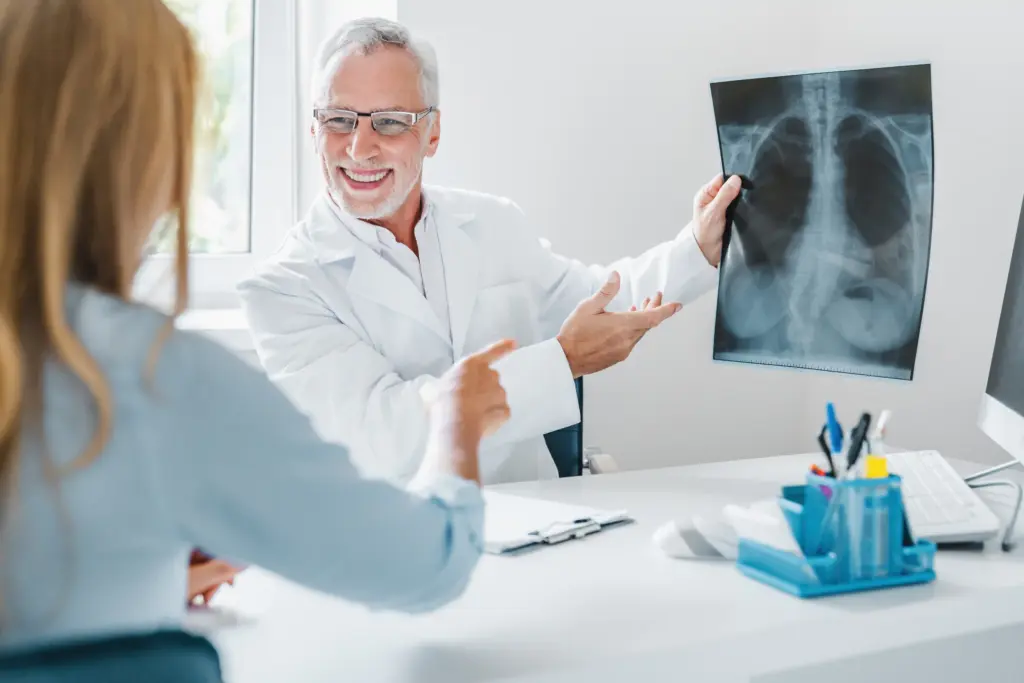
The mucociliary apparatus is the lung’s primary innate defense system. In a healthy lung, this system functions like a continuous escalator, keeping the sterile lower airways free from contamination. In bronchitis, this system fails. Viral or bacterial toxins can directly shear off cilia, leaving patches of the airway unprotected. The mucus changes in consistency, becoming more viscous and difficult to transport. This failure leads to mucostasis, where stagnant mucus allows bacteria to proliferate, potentially leading to secondary bacterial pneumonia. Understanding this mechanism is central to the therapeutic approach at Liv Hospital, which often focuses on restoring mucociliary clearance.
The vast majority of acute bronchitis cases are viral. The same viruses that cause the common cold and the flu are often the culprits that descend into the chest.
Respiratory symptoms are often a direct indication of a problem with the lungs or airways. Recognizing these signs and their underlying causes is crucial for early diagnosis and treatment.
While bacteria are rarely the primary cause of acute bronchitis in healthy individuals, they can complicate the course of the illness. Bacterial superinfection occurs when bacteria invade the airways that a virus has already damaged.
Bronchitis is not solely infectious; it can also be triggered or exacerbated by environmental factors. Inhalation of irritants triggers the same inflammatory cascade as a viral infection.
In chronic cases, the persistent inflammation leads to structural changes known as airway remodeling. This involves the hypertrophy of smooth muscle cells and the deposition of collagen in the airway walls. The result is a stiffer, thicker airway that is less compliant and more prone to collapse during exhalation. This gas trapping contributes to the sensation of breathlessness and hyperinflation of the lungs seen in long-term sufferers. Recognizing these changes early is crucial for preventing irreversible damage.
Bronchitis is not just a localized event; it triggers a systemic immune response. Cytokines released from the inflamed bronchial cells enter the bloodstream, causing fever, fatigue, and malaise. This systemic activation is why patients often feel thoroughly exhausted even if the infection is limited to the chest. In elderly patients or those with underlying conditions, this systemic stress can decompensate other organs, leading to heart failure or metabolic disturbances.

Send us all your questions or requests, and our expert team will assist you.
Acute bronchitis is a temporary infection that usually resolves in a few weeks, while chronic bronchitis is a long-term condition characterized by a persistent cough that lasts for months or years.
Acute bronchitis, whether viral or bacterial, is contagious and spreads through droplets, whereas chronic bronchitis caused by smoking or irritants is generally not contagious.
Yes, if the infection spreads from the bronchial tubes into the air sacs of the lungs, it can develop into pneumonia, which is a more serious condition.
Smoking damages the cilia that clean the lungs and causes the mucus glands to enlarge, leading to chronic inflammation and a higher risk of infection.
The mucus turns yellow or green due to the presence of white blood cells and cellular debris that the body sends to fight the inflammation, not necessarily indicating a bacterial infection.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)