Urology treats urinary tract diseases in all genders and male reproductive issues, covering the kidneys, bladder, prostate, urethra, from infections to complex cancers.
Send us all your questions or requests, and our expert team will assist you.
The recovery phase following a circumcision is a dynamic biological process involving hemostasis, inflammation, proliferation, and maturation. At Liv Hospital, the “Recovery and Follow-Up” period is managed with clear guidance to minimize anxiety and complications. While the surgical wounds usually heal rapidly due to the excellent blood supply of the genital area, the complete adaptation of the glans to its new exposed state takes longer. Understanding the stages of healing helps patients and parents distinguish between normal physiological responses and potential complications requiring medical attention.
Recovery protocols differ slightly between infants, children, and adults, primarily regarding activity restrictions and sexual abstinence. However, the fundamental principles of wound hygiene and observation apply universally.
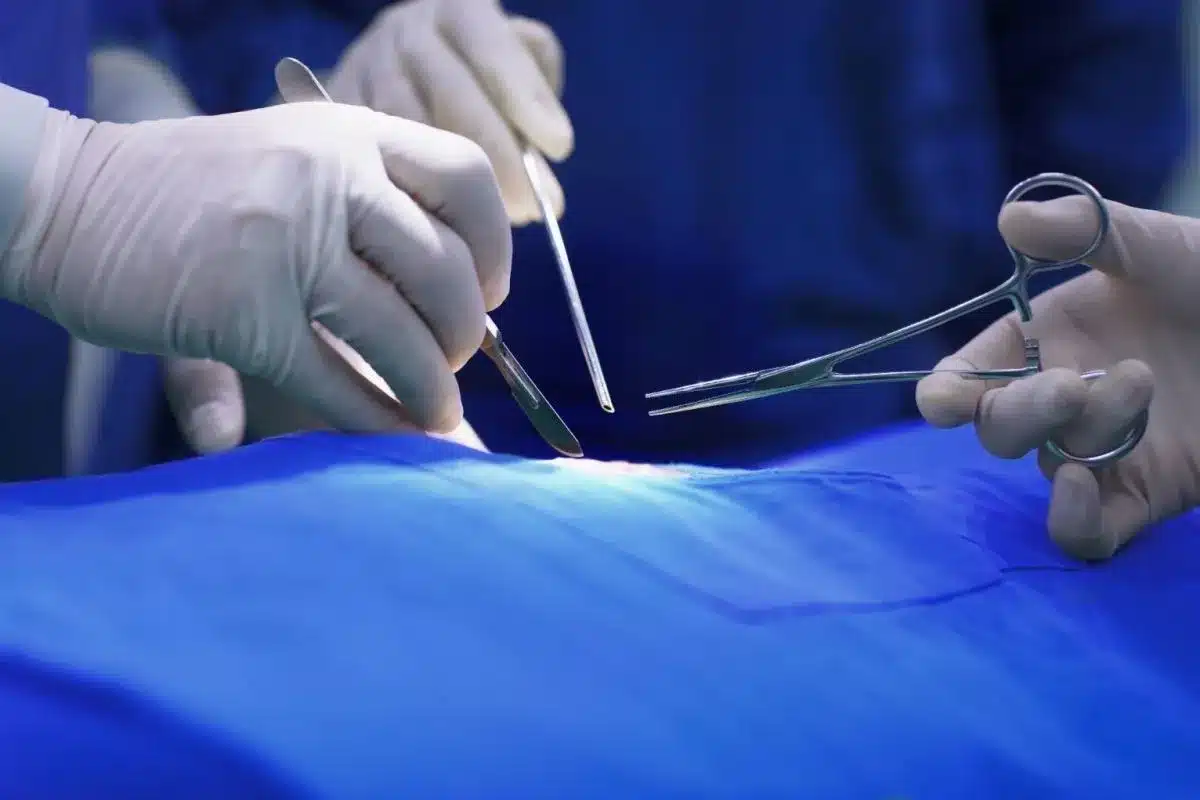
Weeks 4-6 (Final Healing): In adults, the wound strength increases sufficiently to allow for sexual activity. The scar line may remain firm (indurated) for a few months before softening.


Proper hygiene is critical to prevent infection and adhesions.
Adhesion Prevention: In children, as the swelling goes down, the shaft skin may tend to push forward over the corona. Parents are instructed to gently retract the skin daily during cleaning to ensure the raw surfaces do not stick together and form skin bridges.
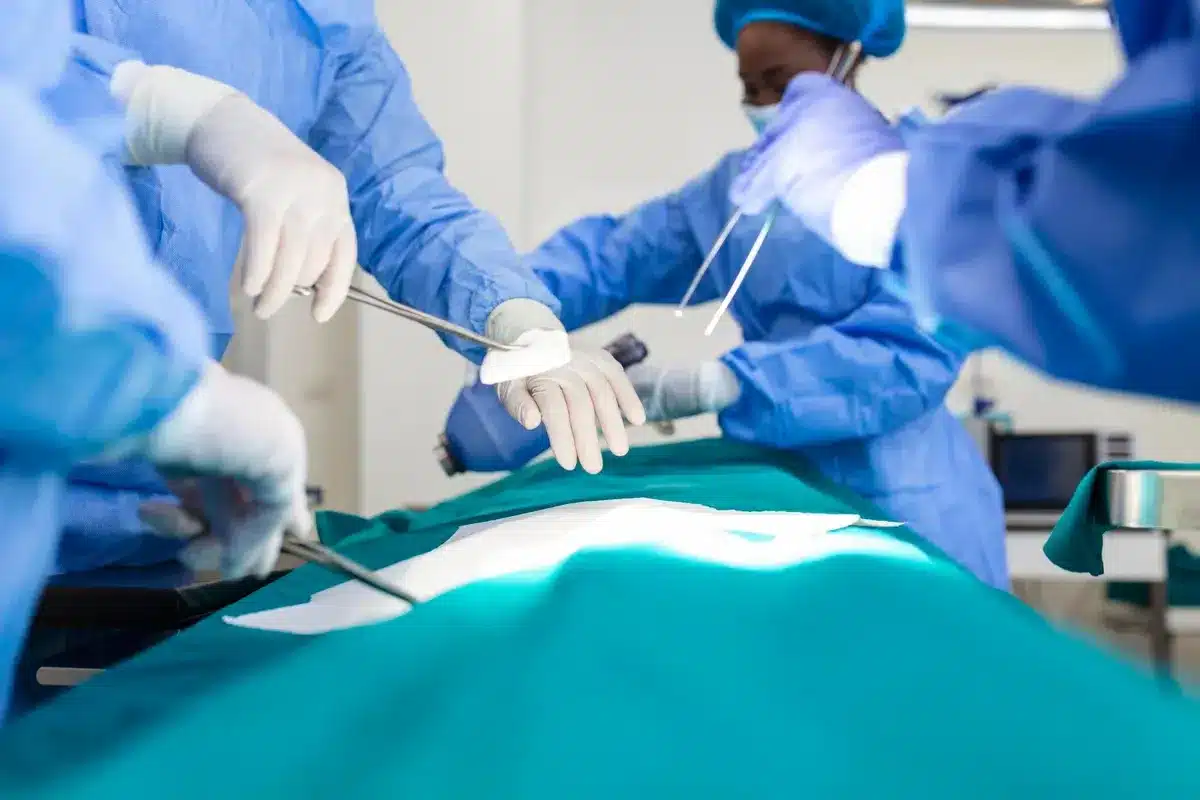
While complications are rare (occurring in 1-3% of cases), vigilance is necessary.
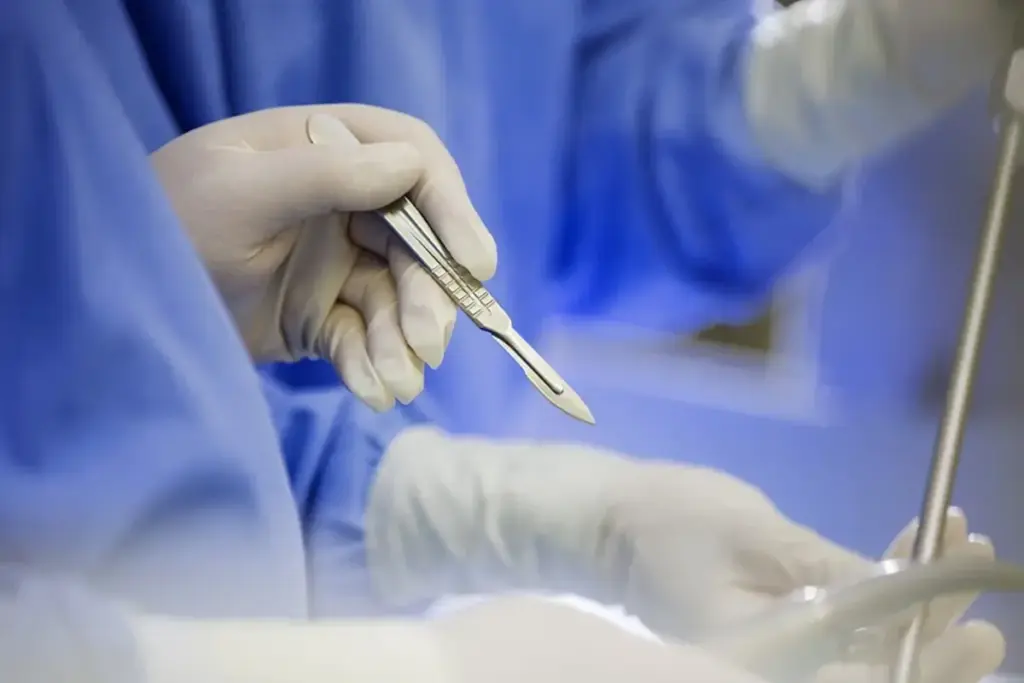
For adult patients, the return to sexual activity is a major concern. Abstinence is strictly mandated for 4 to 6 weeks to prevent wound dehiscence (splitting open). Erections during the recovery phase (nocturnal tumescence) can be painful due to the tension on the sutures. Patients are advised to empty their bladder before sleep and may be prescribed muscle relaxants or advised to use cold packs to manage this. Long-term, patients report an adjustment period where the hypersensitivity of the glans reduces, often normalizing within a few months.
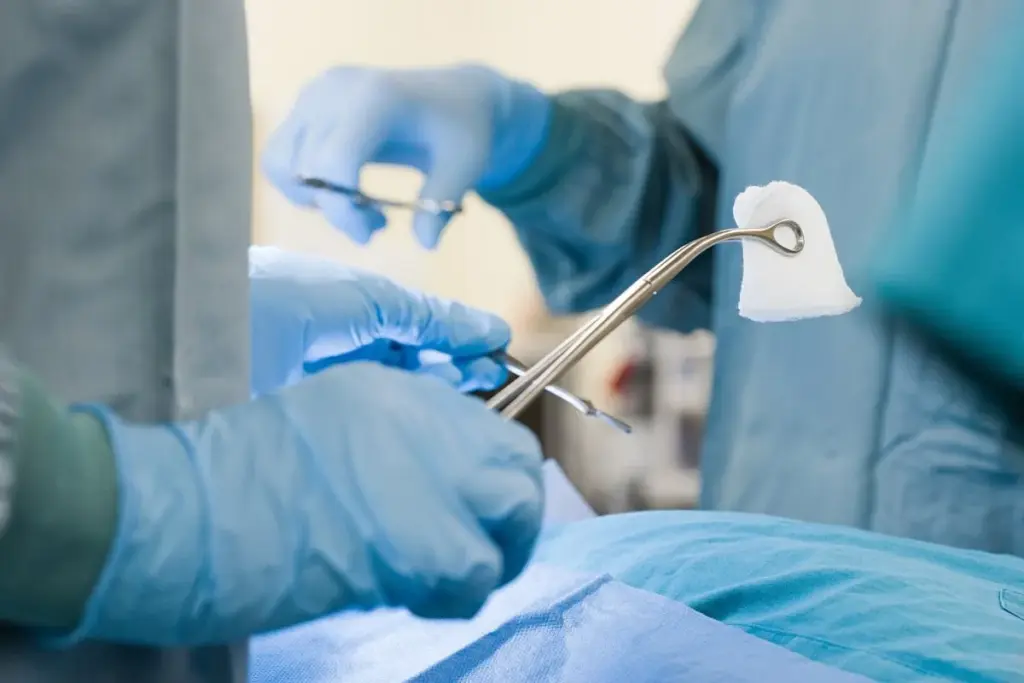
Routine follow-up is typically scheduled 1-2 weeks post-surgery to check wound healing. Long-term issues such as keloid formation, asymmetrical skin removal, or dissatisfaction with the cosmetic result are addressed in subsequent visits. The final result is a permanent anatomical change that requires standard hygiene practices, specifically washing the glans to prevent the accumulation of debris, now that the self-cleaning mechanism of the foreskin is absent.

Send us all your questions or requests, and our expert team will assist you.
The yellow or whitish film that appears on the glans a few days after surgery is called a fibrinous exudate. It is a biological dressing produced by the body to protect the healing raw surface. It is a sign of normal healing, not infection (pus). It should not be wiped or scrubbed off; it will resolve naturally as the skin matures and keratinizes.
Nocturnal erections are involuntary and can stretch the healing wound, causing pain. To manage this, empty your bladder before bed to reduce pressure. Sleeping in a fetal position (knees drawn up) can reduce tension on the skin. If you wake up with an erection, applying an ice pack to the groin or walking on a cold floor can help it subside quickly. Avoid sexual stimuli.
You must wait until the wound is completely healed and the stitches have fully dissolved or fallen out. This typically takes 4 to 6 weeks. Engaging in sexual activity too early can cause the wound to tear open (dehiscence), leading to bleeding, infection, and potential scarring that could require corrective surgery. Always get clearance from your surgeon first.
To prevent the raw glans from sticking to the diaper, you should apply a generous amount of petroleum jelly (Vaseline) or a prescribed antibiotic ointment to the front of the diaper or directly on the penis with every diaper change for the first week. This creates a non-stick barrier that protects the healing tissue from friction and urine irritation.
While minor redness and swelling are normal, signs of infection include redness that spreads up the shaft of the penis or onto the abdomen, a fever (temperature over 38°C/100.4°F), thick green or creamy discharge (pus) that smells bad, or the baby being excessively fussy and refusing to eat. If any of these occur, contact your healthcare provider immediately.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)