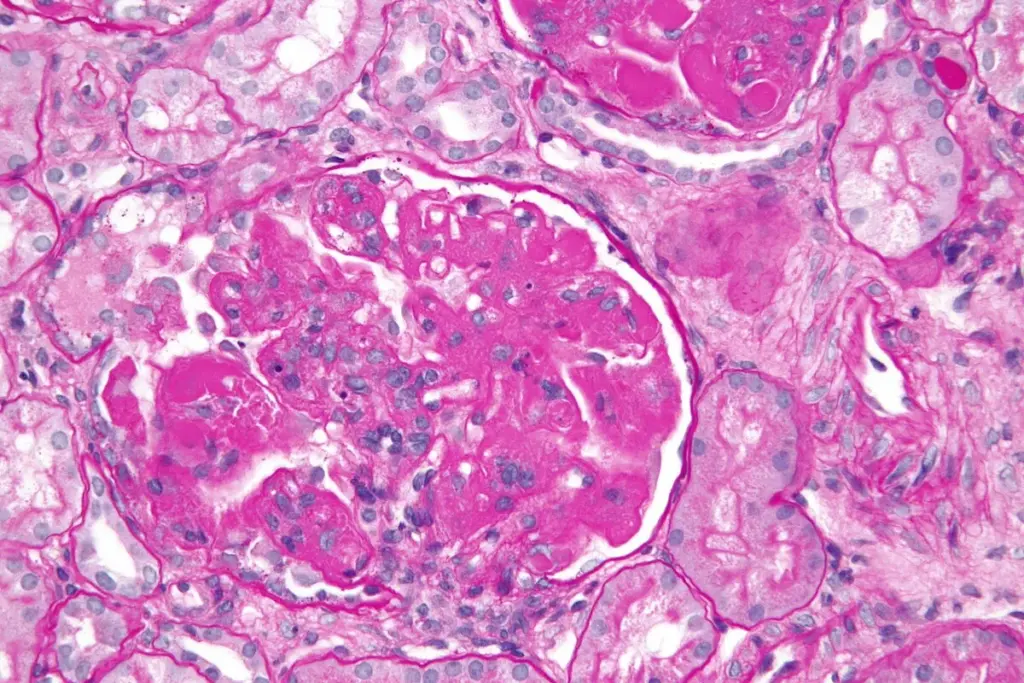
Acute interstitial nephritis (AIN) is a kidney problem. It causes inflammation in the spaces between kidney tubules. This condition can lead to long-term kidney damage if not treated early.
AIN is a common cause of kidney injury, affecting millions globally. It can be short-term or long-lasting. Often, it’s caused by certain medicines, like antibiotics and NSAIDs.
Prompt diagnosis and treatment are key to avoid lasting damage. We will look into the causes, symptoms, and why early action is vital in managing AIN.
Key Takeaways
- Acute interstitial nephritis is a kidney disorder causing inflammation between kidney tubules.
- AIN is a significant cause of acute kidney injury, often diagnosed through renal biopsy.
- The condition can be acute or chronic, resulting from medications like antibiotics and NSAIDs.
- Prompt diagnosis and treatment are essential to prevent long-term kidney damage.
- AIN affects millions worldwide, stressing the need for awareness and early intervention.
Understanding Acute Interstitial Nephritis
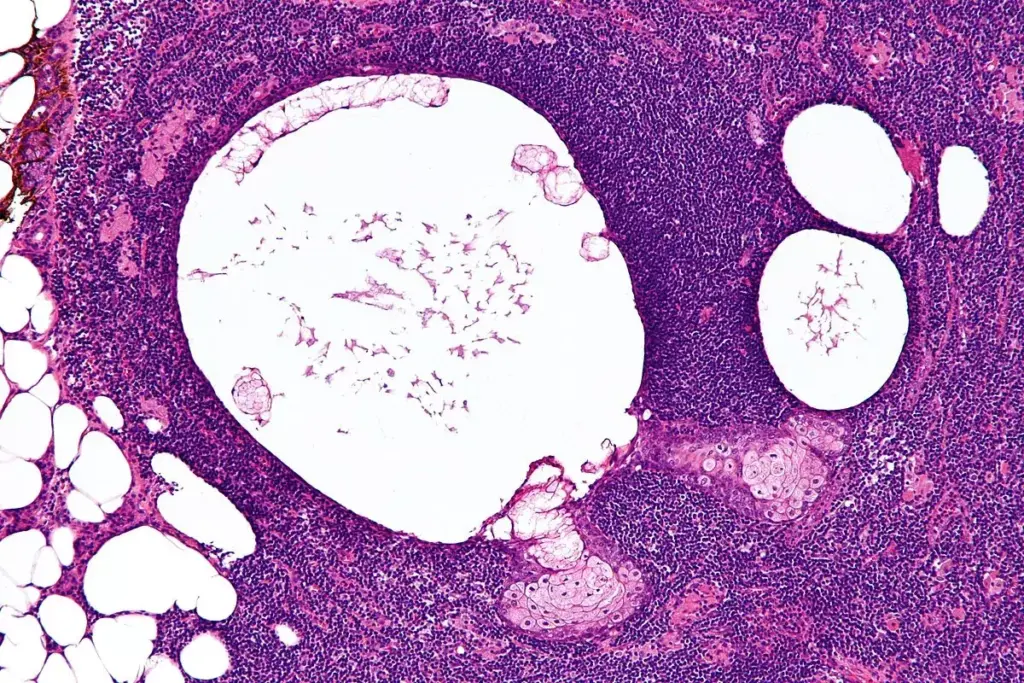
AIN, or acute interstitial nephritis, is a major cause of kidney injury. It leads to inflammation in the kidneys, damaging the tubules and the area around them.
Definition and Pathophysiology
AIN is an inflammation of the kidney’s interstitium, the area around the tubules. It often starts as an allergic reaction or immune response to medications, infections, or autoimmune disorders. This reaction causes inflammation and damage to the kidney’s interstitium.
Prevalence and Epidemiology
AIN is not very common, making up about 1% to 3% of all kidney biopsies. But, it’s a big problem in certain groups, like the elderly and those with many health issues. It’s a key cause of sudden kidney injury, making quick diagnosis and treatment very important.
Clinical Presentation and Symptoms
AIN can show up in many ways. Symptoms include sudden kidney failure, rash, fever, and joint pain. Some people might just feel tired or unwell. Blood tests often show high creatinine levels, eosinophilia, and abnormal urine tests. This variety in symptoms highlights the need for careful testing.
| Causes of AIN | Clinical Features | Laboratory Findings |
| Medications (e.g., NSAIDs, antibiotics) | Acute kidney injury, rash, fever | Elevated serum creatinine, eosinophilia |
| Infections (e.g., pyelonephritis, sepsis) | Fever, flank pain, dysuria | Abnormal urinalysis, leukocytosis |
| Autoimmune disorders (e.g., lupus, sarcoidosis) | Systemic symptoms, renal impairment | Autoantibodies, elevated inflammatory markers |
It’s vital for doctors to understand AIN well to treat it effectively. Knowing its causes, symptoms, and test results helps us care for patients better.
Primary Causes of Interstitial Nephritis
It’s important to know what causes interstitial nephritis to manage it well. This condition affects the kidney tubules and the tissue around them. We’ll look at the main causes, which help in diagnosing and treating it.
Drug-Induced Interstitial Nephritis
Most cases of interstitial nephritis are caused by drugs, making up 67 to 90 percent of cases. Antimicrobials and NSAIDs are often to blame. The body reacts to these drugs, causing inflammation and possible damage to the kidneys.
Infection-Related Causes
About 6 to 8 percent of cases are due to infections. Different pathogens like bacteria, viruses, and fungi can cause it. These infections can either directly attack the kidney or trigger an immune response leading to inflammation.
Autoimmune and Immune-Mediated Causes
Autoimmune diseases are responsible for 20 percent of cases. Conditions like systemic lupus erythematosus and Sjögren’s syndrome can lead to AIN. Knowing these causes helps in creating effective treatment plans.
Conclusion: Progression to Chronic Interstitial Nephritis
Acute interstitial nephritis (AIN) can turn into chronic if not treated early. About 40 to 60 percent of patients face permanent kidney damage. This can lead to end-stage kidney disease.
Early diagnosis and proper care are key for AIN patients. Knowing the causes and symptoms is vital for managing the condition.
Recognizing the cause of interstitial nephritis and treating it quickly helps avoid long-term damage. Patients with AIN need regular check-ups to keep their kidney function in check.
Good care and educating patients are critical in managing AIN symptoms. This approach helps prevent chronic interstitial nephritis. With the right care, patients can keep their kidneys healthy and avoid serious complications.
FAQ
What is acute interstitial nephritis?
Acute interstitial nephritis (AIN) is inflammation of the kidney’s interstitial tissue and tubules. It can cause sudden kidney dysfunction and impaired urine output.
What are the primary causes of acute interstitial nephritis?
AIN is most commonly caused by medications, infections, or autoimmune disorders. Other triggers include toxins and systemic inflammatory conditions.
Which medications are commonly associated with drug-induced AIN?
Common culprits include antibiotics (penicillins, cephalosporins), NSAIDs, proton pump inhibitors, and certain diuretics. Reactions can occur days to weeks after exposure.
Can infections lead to acute interstitial nephritis?
Yes, bacterial, viral, or other infections can trigger AIN. Examples include streptococcal infections, viral hepatitis, and urinary tract infections.
What are the symptoms of acute interstitial nephritis?
Symptoms may include fever, rash, fatigue, nausea, decreased urine output, and sometimes flank pain. Lab tests may show elevated creatinine or eosinophils in urine.
Can acute interstitial nephritis progress to chronic interstitial nephritis?
Yes, untreated or severe AIN can lead to chronic kidney damage, fibrosis, and permanent loss of kidney function. Early intervention reduces this risk.
What is the significance of timely diagnosis and treatment of AIN?
Early diagnosis allows prompt withdrawal of offending drugs or treatment of infections. Timely management improves recovery and prevents long-term kidney damage.
How is acute interstitial nephritis diagnosed?
Diagnosis involves blood tests (creatinine, eosinophils), urinalysis, imaging, and sometimes a kidney biopsy. History of recent medication use or infection helps identify the cause.
What is the role of autoimmune diseases in causing AIN?
Autoimmune conditions like lupus or sarcoidosis can trigger AIN by causing inflammation in kidney tissues. Managing the underlying autoimmune disorder is key to treatment.
What are the consequences of untreated AIN?
Untreated AIN can lead to chronic kidney disease, irreversible kidney damage, fluid imbalance, and, in severe cases, kidney failure requiring dialysis.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/12825841/




































