
specific asthma attack chest pain is a critical warning. Learn why tightness occurs and when to seek emergency help for severe discomfort.
Do you feel tightness in your chest when you have asthma? You’re not alone. Many people say they feel discomfort or pain during asthma attacks.
Studies show many asthma patients in the hospital feel chest discomfort. At Liv Hospital, we understand how complex asthma can be. We offer care that focuses on you, with the right diagnosis and new treatments.
It’s important to know how asthma and chest pain are connected. We’ll help you understand how asthma can lead to chest tightness and discomfort. This way, you can better manage your symptoms and find the right treatment.
Key Takeaways
- Asthma can cause chest tightness and discomfort.
- Chest pain is a common symptom reported by asthma patients.
- Accurate diagnosis is key for managing asthma well.
- Liv Hospital offers care that focuses on the patient for asthma.
- Knowing your asthma symptoms helps you find the right treatment.
The Relationship Between Asthma and Chest Pain

Asthma and chest pain are closely linked, making it important to study their connection. Asthma causes the airways to swell and narrow, leading to symptoms like wheezing and shortness of breath. Chest tightness or pain is also common.
Prevalence Statistics in Asthma Patients
Many asthma patients feel chest pain during attacks. About 76% of those in the hospital for asthma reported chest pain. This shows how common chest pain is in severe cases.
|
Study |
Percentage Reporting Chest Pain |
Patient Group |
|---|---|---|
|
Hospitalization Study |
76% |
Acute Asthma Patients |
|
Outpatient Survey |
45% |
Chronic Asthma Patients |
|
Emergency Department Data |
60% |
Asthma Patients Requiring Emergency Care |
How Asthma Affects the Respiratory System
Asthma irritates the airways, causing them to narrow and produce more mucus. This irritation makes the airways feel tight and painful. It’s this complex process that leads to chest pain in asthma patients.
Key Mechanisms:
- Airway constriction and inflammation
- Mechanoreceptor stimulation
- Mucus production and airway obstruction
Grasping these mechanisms is key to managing asthma-related chest pain. By tackling the root causes and using the right treatments, doctors can ease symptoms. This improves the lives of those with asthma.
Recognizing Asthma Attack Chest Pain Symptoms
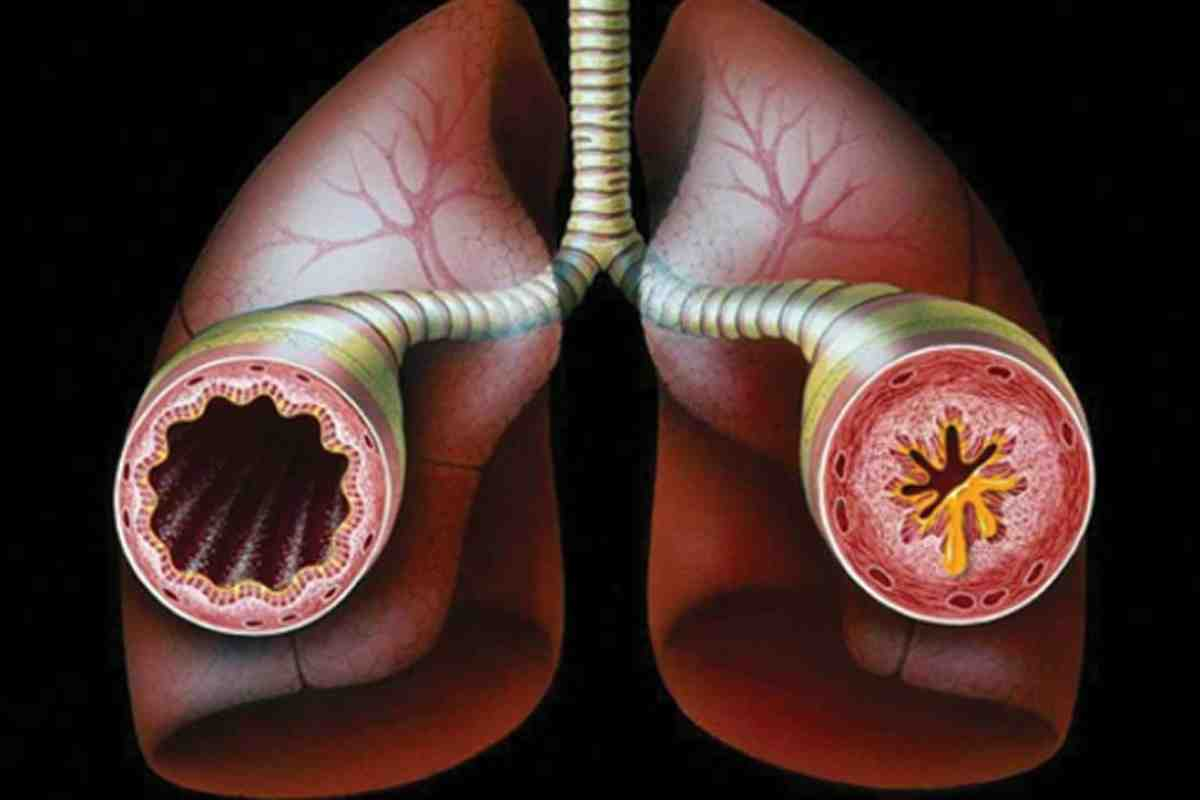
It’s important to know the signs of asthma chest pain to manage it well. Asthma can cause different kinds of chest discomfort. Knowing these signs helps in giving the right care.
Common Descriptions and Patient Experiences
People with asthma often say their chest feels tight or heavy, like a brick. Some feel sore or like their chest is being squeezed. These feelings usually point to discomfort or pain in the chest.
Asthma can also cause shortness of breath, tightness or pain in the chest, and wheezing. Coughing or wheezing attacks can get worse with a respiratory virus. Knowing these symptoms is key to treating asthma right.
Location and Radiation Patterns
The chest pain from asthma can be in different places for different people. It often starts in the middle of the chest but can spread to the back, shoulders, or arms. Knowing where the pain goes helps tell if it’s asthma or something else.
Duration and Intensity Variations
The length and how bad the chest pain is can change a lot. Some people might feel a little discomfort that goes away fast. Others might have really bad pain that lasts longer. Knowing these changes helps decide the best treatment.
By understanding asthma chest pain symptoms, like what it feels like, where it is, and how long it lasts, we can better manage asthma. This helps both healthcare providers and patients work together to control asthma better.
Types of Chest Discomfort in Asthma Patients
Chest pain in asthma varies a lot from person to person. It can be influenced by how severe the asthma is, what triggers it, and how well someone can handle symptoms.
Band-like Tightness and Pressure Sensations
Many asthma patients feel a band-like tightness in their chest. It’s like wearing a tight band or corset. They might also feel pressure, like something is weighing on their chest, making it hard to breathe.
Sharp vs. Dull Pain Characteristics
Asthma chest pain can be either sharp or dull. Sharp pain is stabbing and intense. Dull pain is a constant ache. Knowing the type of pain helps doctors find the right treatment.
Burning and Soreness in the Chest
Some asthma patients feel a burning sensation in their chest. It’s uncomfortable and scary. Others feel their chest is sore, like after working out. These feelings come from airway inflammation and irritation.
It’s important to understand the different chest discomforts in asthma. Recognizing the specific pain helps doctors create better treatment plans. This improves life quality for asthma patients.
The Science Behind Asthma-Related Chest Pain
Chest pain during an asthma attack comes from airway constriction and inflammation. This complex mix of physiological responses causes discomfort and pain. It’s a key part of what happens during an asthma attack.
Airway Constriction and Inflammation Mechanisms
During an asthma attack, airways narrow due to muscle constriction. This, along with inflammation and more mucus, causes chest tightness and pain. Airway constriction is a main reason for the discomfort felt by patients.
“Airway inflammation in asthma includes eosinophils, neutrophils, and lymphocytes,” medical literature says. This inflammation is a big part of the symptoms, including chest pain.
Role of Mechanoreceptors in Pain Perception
Mechanoreceptors are key in feeling chest pain during an asthma attack. These receptors feel changes in airway size and respond to stress from constriction. When airways narrow, mechanoreceptors send pain signals to the brain.
This connection between airway constriction and chest pain is important. It shows why some people feel more pain than others, even with similar airway constriction.
Rib Joint Stress and Musculoskeletal Factors
Musculoskeletal factors also play a role in chest pain in asthma patients. Breathing hard during an attack can strain the rib joints and muscles, adding to the pain.
Medical Expert, a pulmonologist, says, “The musculoskeletal part of chest pain in asthma is often missed but is very important.” This shows why looking at both respiratory and musculoskeletal factors is key in managing chest pain.
Understanding airway constriction, inflammation, mechanoreceptor activation, and musculoskeletal stress helps manage asthma-related chest pain better. This knowledge leads to more effective treatments, improving life for asthma patients.
Variant Asthma Presentations Featuring Chest Pain
Some asthma types show chest pain as a main symptom, making it hard to diagnose. We’ll look at three asthma variants with chest pain: Chest Pain Variant Asthma (CPVA), Chest Tightness Variant Asthma (CTVA), and Cough Variant Asthma with Chest Discomfort.
Chest Pain Variant Asthma (CPVA)
Chest Pain Variant Asthma is rare, with chest pain being the main symptom. People with CPVA often have chest pain that might seem like heart problems. Getting a correct diagnosis involves detailed tests and trying asthma medicines.
A study in the Journal of Asthma showed that CPVA patients usually have normal lung function between episodes. This makes diagnosing based on symptoms and history very important.
“The diagnosis of CPVA is often challenging and requires a high index of suspicion, even when lung function is normal between episodes.”- Journal of Asthma
Chest Tightness Variant Asthma (CTVA)
Chest Tightness Variant Asthma is marked by chest tightness, often with other breathing issues. It can be told apart from other chest tightness causes through careful checks and tests.
|
Characteristics |
CTVA |
Other Causes |
|---|---|---|
|
Primary Symptom |
Chest Tightness |
Varies (e.g., pain, discomfort) |
|
Respiratory Symptoms |
Often present |
May or may not be present |
|
Response to Asthma Treatment |
Positive |
Varies |
Cough Variant Asthma with Chest Discomfort
Cough Variant Asthma is known for a chronic cough, often without wheezing or shortness of breath. Chest discomfort with cough makes diagnosis harder.
Important signs include a cough that gets worse with asthma triggers and better with treatment. We should think of Cough Variant Asthma when there’s a chronic cough with chest pain.
It’s key to recognize these asthma types to give the right care. Knowing about CPVA, CTVA, and Cough Variant Asthma with Chest Discomfort helps us better diagnose and treat these tough cases.
Asthma Chest Pain in Different Age Groups
It’s important to know how asthma chest pain shows up in different ages. Asthma can start at any time, and its symptoms change with age.
Children and Adolescents
Kids and teens with asthma often feel tightness or pressure in their chest. They might also wheeze, cough, or have trouble breathing. This can worry both the child and their parents a lot.
It’s hard to figure out if a kid has asthma because they can’t always explain what they feel. Doctors usually listen to what parents say and look at the child to make a diagnosis.
Adults and Working-Age Population
Adults with asthma might feel chest pain for many reasons. This could be because of allergies, colds, or working too hard. The pain can be mild or very tight, affecting their day and job.
Adults might not get diagnosed with asthma right away. If they keep feeling tightness or pain in their chest, they should see a doctor.
Elderly Patients with Comorbidities
Older people with asthma face more challenges because of other health issues. They might have heart problems, COPD, or other lung diseases. It’s hard to tell if their chest pain is from asthma or something else.
Doctors need to look at all the health problems an elderly person has when trying to diagnose and treat asthma. They have to think about how different medicines might work together.
|
Age Group |
Common Descriptions of Chest Pain |
Diagnostic Challenges |
|---|---|---|
|
Children and Adolescents |
Tightness, pressure |
Difficulty in describing symptoms |
|
Adults |
Discomfort, tightness |
Underdiagnosis or misdiagnosis |
|
Elderly |
Complex presentations due to comorbidities |
Managing multiple health conditions |
Differentiating Asthma Chest Pain from Other Conditions
It’s important to know the difference between asthma chest pain and other chest discomforts. This is because asthma chest pain can sometimes look like symptoms of serious conditions. Getting the right diagnosis is key.
Cardiac vs. Asthmatic Chest Pain
When you have chest pain, figuring out if it’s from your heart or asthma is a big deal. Heart pain, like from angina or a heart attack, feels different than asthma pain. Heart pain feels like a heavy pressure, while asthma pain is more about tightness and breathing trouble.
Here are some key differences:
- Trigger factors: Asthma pain can be set off by things like allergens, exercise, or cold air. Heart pain might come from hard work or stress.
- Associated symptoms: Asthma often brings wheezing, coughing, or trouble breathing. Heart problems might make you dizzy, nauseous, or feel pain in your arm or jaw.
- Response to treatment: Asthma pain usually gets better with asthma meds. Heart pain might need special heart treatments.
Gastroesophageal Reflux Disease (GERD)
GERD can also cause chest pain that might seem like asthma. GERD pain feels like a burning in your chest, worse when you lie down or eat certain foods. Unlike asthma, GERD doesn’t usually cause wheezing or trouble breathing. But it can make asthma symptoms worse in some people.
Anxiety-Related Chest Discomfort
Anxiety can make your chest feel tight or uncomfortable, which might seem like asthma. Anxiety chest pain often comes with other signs like a racing heart, sweating, or shaking. Unlike asthma, anxiety pain doesn’t usually make you wheeze or cough.
Musculoskeletal Causes
Problems like costochondritis or rib injuries can also cause chest pain that might seem like asthma. This pain is usually in one spot and gets worse with movement or pressure. Unlike asthma, this pain doesn’t usually make it hard to breathe.
In short, telling asthma chest pain apart from other conditions needs a thorough check-up. This includes looking at your medical history, doing a physical exam, and running tests. Knowing the unique signs of each condition helps doctors give the right treatment.
Diagnosing the Source of Chest Pain in Asthma Patients
When asthma patients feel chest pain, finding the cause is key. We use a detailed approach to figure out why. This includes looking at their symptoms, medical history, lung function tests, and sometimes images.
Clinical Evaluation and Medical History
First, we look at the patient’s symptoms and medical history. We check how long the pain lasts, how bad it is, and what it feels like. This helps us tell if the pain is from asthma or something else.
We also check the patient’s overall health. This includes any other health issues that might be causing the pain. Knowing the patient’s medical history helps us find what might be triggering the pain and how severe their asthma is.
Pulmonary Function Testing
Pulmonary function tests (PFTs) are important for asthma patients. Spirometry is the most common test. It measures how much air the patient can breathe in and out. This shows how well their lungs are working and if treatment is helping.
Other tests, like peak flow monitoring, might be used too. These tests help us see how well the lungs are working and how well treatment is working. They are important for managing asthma-related chest pain.
Imaging Studies and Additional Diagnostics
Sometimes, we need to use imaging studies to check for other causes of pain. Chest X-rays or CT scans can show if there’s something like pneumonia or a lung problem. These tests help us see if there’s something else going on in the lungs.
We might also do tests like electrocardiograms (ECGs) to check the heart. Sometimes, we need to see specialists like pulmonologists or cardiologists to find out why the patient is having chest pain.
|
Diagnostic Tool |
Purpose |
Information Provided |
|---|---|---|
|
Clinical Evaluation and Medical History |
Assess symptoms and overall health |
Duration, intensity, and characteristics of chest pain; comorbid conditions |
|
Pulmonary Function Testing (PFT) |
Evaluate lung function |
Severity of airflow obstruction; response to treatment |
|
Imaging Studies (X-ray, CT scan) |
Identify pulmonary abnormalities |
Presence of pneumonia, pneumothorax, or other lung conditions |
Treatment Options for Asthma-Related Chest Pain
For those with chest pain from asthma, there are many ways to feel better. Treatment includes medicines, lifestyle changes, and avoiding things that make symptoms worse. This helps manage symptoms well.
Quick-Relief Medications
Quick-relief medicines are key for fast help during an asthma attack. They include:
- Short-acting beta agonists (SABAs): Like albuterol, these relax airway muscles, making breathing easier.
- Anticholinergics: Drugs such as ipratropium open airways by reducing muscle spasms.
Long-Term Control Medications
Long-term control medicines are vital for managing asthma over time. They include:
- Inhaled corticosteroids (ICS): Like fluticasone, these reduce airway inflammation.
- Combination inhalers: These mix ICS and LABAs to reduce inflammation and relax muscles.
- Leukotriene modifiers: Oral drugs that reduce inflammation and relax muscles.
Breathing Techniques and Physical Therapy
Breathing exercises and physical therapy can help too. They include:
- Pursed-lip breathing: Helps keep airways open, making breathing easier.
- Diaphragmatic breathing: Exercises that strengthen the diaphragm, improving lung capacity.
- Physical therapy: Customized exercise programs that improve lung function and fitness.
Complementary Approaches
Some people find other methods helpful for managing asthma-related chest pain. These include:
- Acupuncture: A traditional Chinese medicine technique that may reduce symptoms.
- Herbal supplements: Herbs like ginger and turmeric have anti-inflammatory properties, though effects vary.
- Stress management techniques: Yoga, meditation, and mindfulness can help reduce stress, a common asthma trigger.
Working with a healthcare provider to create a personalized treatment plan is key. Combining medical treatments with lifestyle changes and complementary therapies can help manage asthma-related chest pain. This improves overall quality of life.
When Chest Pain During an Asthma Attack Requires Emergency Care
It’s important to know when chest pain from an asthma attack needs emergency care. Severe attacks can be deadly. Quick action is key to saving lives.
Red Flag Symptoms Requiring Immediate Attention
Some symptoms during an asthma attack mean you need to see a doctor right away. These include:
- Severe difficulty breathing or shortness of breath at rest
- Chest pain or tightness that is severe or worsening
- Blue or gray lips or fingernails
- Confusion or altered mental state
- Inability to speak or walk properly due to shortness of breath
Spotting these symptoms early can make a big difference. If you or someone you know is showing them, act fast.
Emergency Response Protocol
When you have a severe asthma attack, follow a specific emergency plan. Here’s what to do:
- Give quick-relief medication as your doctor told you to.
- If you feel better, keep an eye on things and get help if symptoms come back or get worse.
- If the medicine doesn’t work, or if symptoms are bad, call emergency services right away.
- While waiting, stay calm and sit up straight to help breathe better.
“The key to managing severe asthma attacks is prompt recognition of worsening symptoms and swift action to seek medical care.”Medical Expert, Pulmonologist
What to Communicate to Healthcare Providers
When you go to the emergency room for asthma chest pain, tell the doctors everything. Be ready to share:
|
Information to Share |
Details |
|---|---|
|
Medical History |
Previous asthma attacks, allergies, and other health issues |
|
Current Symptoms |
Details about chest pain, breathing trouble, and other symptoms |
|
Medications Used |
Info on quick-relief and long-term control meds, including how much you take |
Talking clearly with doctors can help them help you better in an emergency.
Psychological Impact of Recurring Asthma Chest Pain
Recurring asthma chest pain can deeply affect a patient’s mental health. It can lead to more anxiety and fear of future episodes. Living with asthma is not just about physical symptoms. It’s also about dealing with the mental burden it brings.
Anxiety and Fear of Future Episodes
Chest pain can be very distressing, causing high anxiety levels. Patients worry a lot about when the next asthma attack will happen. This worry can make everyday tasks hard and affect their overall well-being. Healthcare providers must address these worries as part of treating asthma.
Quality of Life Considerations
The psychological effects of asthma chest pain go beyond anxiety. It can make simple tasks seem scary because of the fear of an asthma attack. This fear can also lead to feeling isolated, as patients might avoid places that could make their condition worse. We aim to improve our patients’ quality of life and reduce the mental burden of asthma.
Coping Strategies and Support Resources
There are ways to manage the mental side of asthma. Cognitive-behavioral therapy (CBT) can help reduce asthma-related anxiety. Support groups also offer a place for patients to share and learn from others. Using these resources can help patients deal with the mental side of their condition.
We believe in a holistic approach to managing asthma. This means caring for both the physical and mental health of our patients. By doing this, we can help our patients live better lives despite their condition.
Conclusion: Managing Asthma and Chest Discomfort for Better Quality of Life
Managing asthma and chest discomfort is key for a good life. Knowing about asthma, its symptoms, and treatments helps a lot. This way, people with asthma can live more fully.
Handling asthma means using medicines, changing your lifestyle, and watching your symptoms. Quick and long-term medicines are vital for easing chest tightness and other symptoms.
For a better life with asthma, you need more than just medicine. Breathing exercises, physical therapy, and other methods help a lot. These steps can make daily life easier and improve overall health.
With the right care, people with asthma can have a better life. They can enjoy their days without the worry of chest tightness and discomfort. We aim to provide top-notch healthcare and support for those with asthma.
FAQ
Does asthma cause chest pain?
Yes, asthma can cause chest pain and tightness. These are common symptoms for asthma patients during attacks.
What are the common descriptions of chest pain in asthma patients?
Asthma patients often feel a band-like tightness in their chest. They might also describe the pain as sharp or dull, or feel burning or soreness.
How does asthma affect the respiratory system?
Asthma causes the airways to constrict and become inflamed. This can lead to chest pain and discomfort.
What is the difference between cardiac and asthmatic chest pain?
Cardiac chest pain is linked to heart conditions. Asthmatic chest pain is due to airway constriction and inflammation. It’s important to get a proper diagnosis to know the cause.
Can asthma chest pain vary in different age groups?
Yes, chest pain from asthma can differ across age groups. It’s important to understand these differences for proper management.
What are the treatment options for asthma-related chest pain?
Treatment options include quick-relief medications and long-term control medications. Breathing techniques, physical therapy, and complementary approaches are also available.
When should I seek emergency care for chest pain during an asthma attack?
Seek emergency care if you have severe chest pain, trouble breathing, or severe wheezing. These are red flag symptoms.
How can I manage anxiety and fear related to recurring asthma chest pain?
There are coping strategies and support resources to help manage anxiety and fear. Counseling and support groups are available.
Can GERD cause chest pain similar to asthma?
Yes, GERD can cause chest pain similar to asthma. It’s important to get a proper diagnosis to determine the cause.
What is the role of mechanoreceptors in asthma-related chest pain?
Mechanoreceptors play a role in pain perception. They can contribute to the sensation of chest pain in asthma patients.
How is asthma-related chest pain diagnosed?
Diagnosing asthma-related chest pain involves a clinical evaluation and pulmonary function testing. Imaging studies may also be used.
Can musculoskeletal factors contribute to chest pain in asthma patients?
Yes, musculoskeletal factors like rib joint stress can contribute to chest pain in asthma patients.
What is the psychological impact of recurring asthma chest pain?
Recurring chest pain can lead to anxiety and fear of future episodes. It can also reduce quality of life, highlighting the need for effective management.
References
https://pmc.ncbi.nlm.nih.gov/articles/PMC4965212




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























